Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 49(1); 2015 > Article
-
Letter to the editor
TdT+ T-Lymphoblastic Proliferation in Castleman Disease - Chang Gok Woo, Jooryung Huh
-
Journal of Pathology and Translational Medicine 2015;49(1):1-4.
DOI: https://doi.org/10.4132/jptm.2014.11.17
Published online: January 15, 2015
Department of Pathology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
- Corresponding Author: Jooryung Huh, M.D. Department of Pathology, Asan Medical Center, University of Ulsan College of Medicine, 88 Olympic-ro 43-gil, Songpa-gu, Seoul 138-736, Korea Tel: +82-3010-4553, Fax: +82-472-7898, E-mail: jrhuh@amc.seoul.kr
• Received: September 5, 2014 • Revised: October 24, 2014 • Accepted: November 17, 2014
© 2015 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
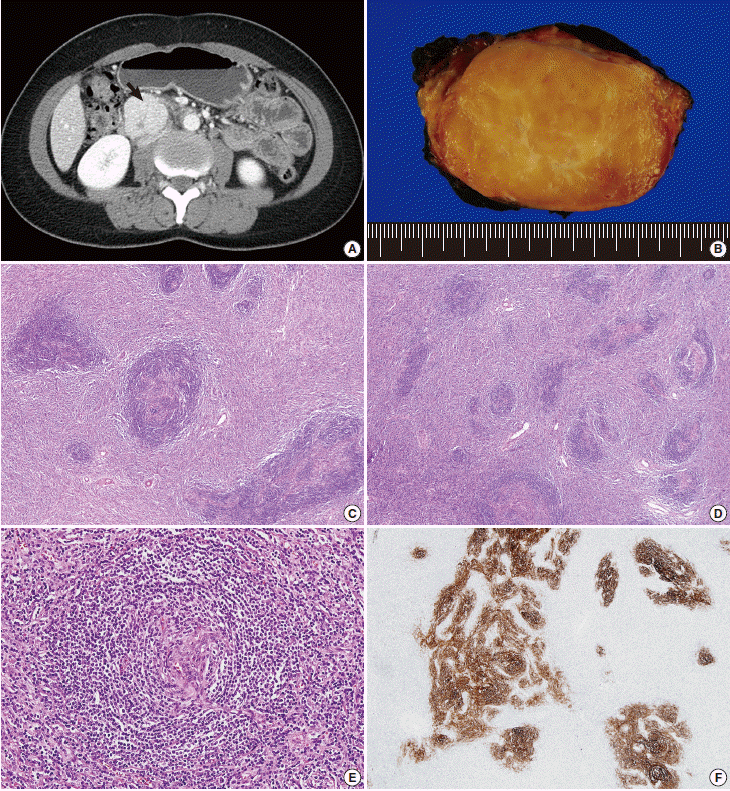
Fig. 1.Hyaline vascular-type Castleman disease. (A) Abdominal computed tomography demonstrates a well-defined homogeneous enhancing mass (arrow) in the retroperitoneum. (B) The mass exhibits a fleshy cut surface with central fibrosis. (C) Variably-sized follicles with multiple germinal centers are present. The interfollicular compartment is expanded with vascular proliferation. (D) Follicular structures appear smaller due to the regression of germinal centers. (E) Mantle zone lymphocytes have a laminated appearance, similar to onion skin. The vessel penetrating the atrophic follicle has a lollipop-like appearance. (F) Hyperplastic follicular dendritic cells are stained with CD21.
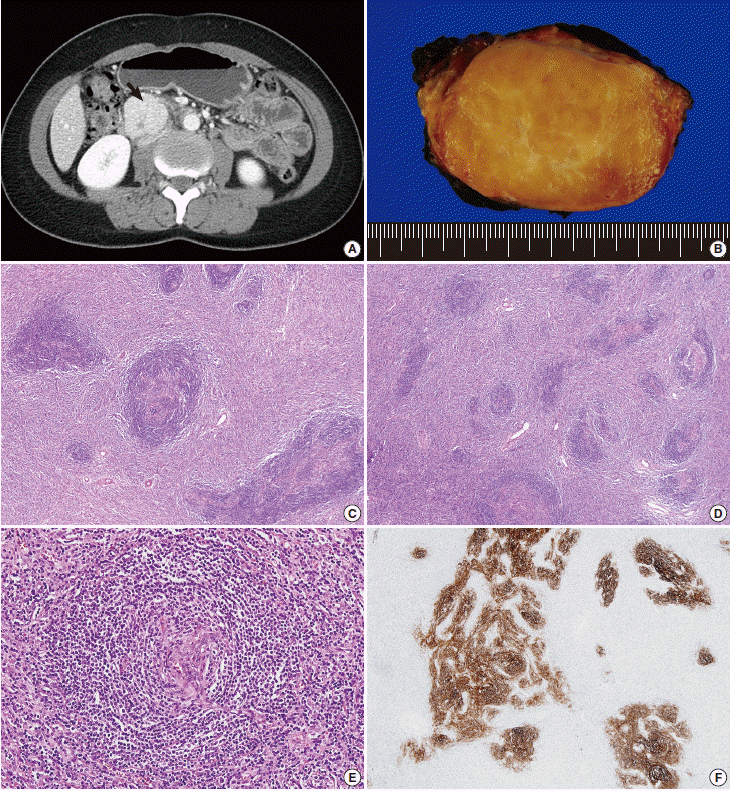

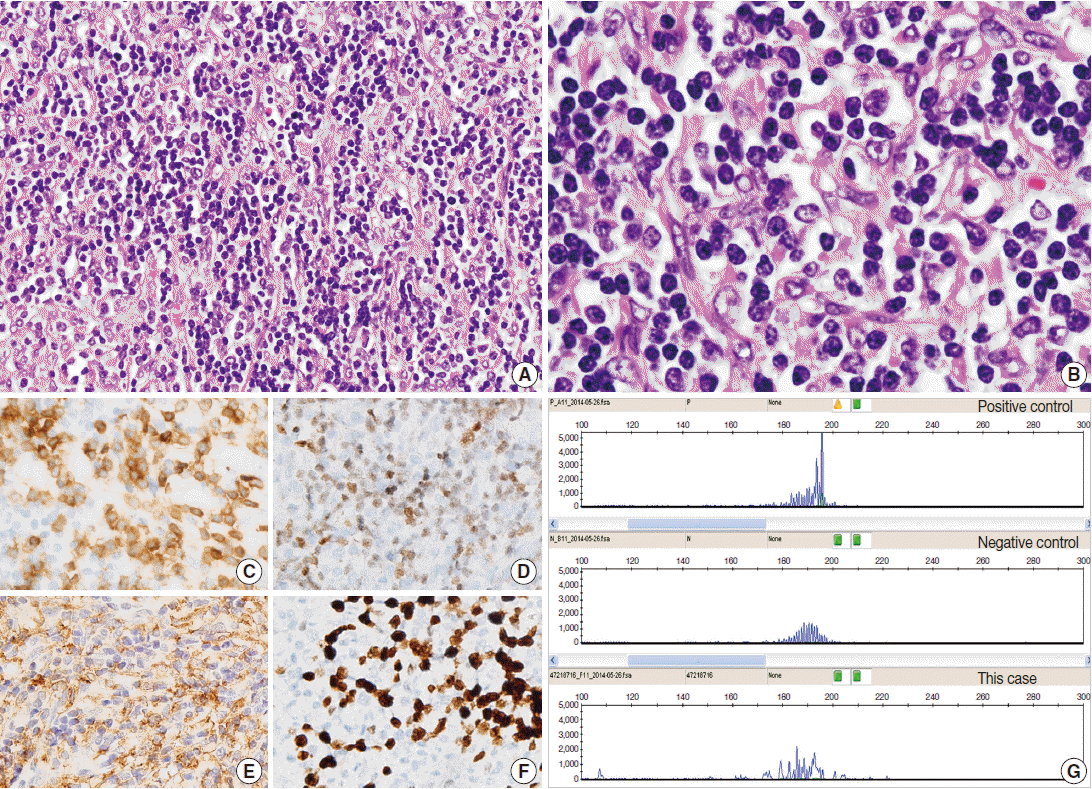
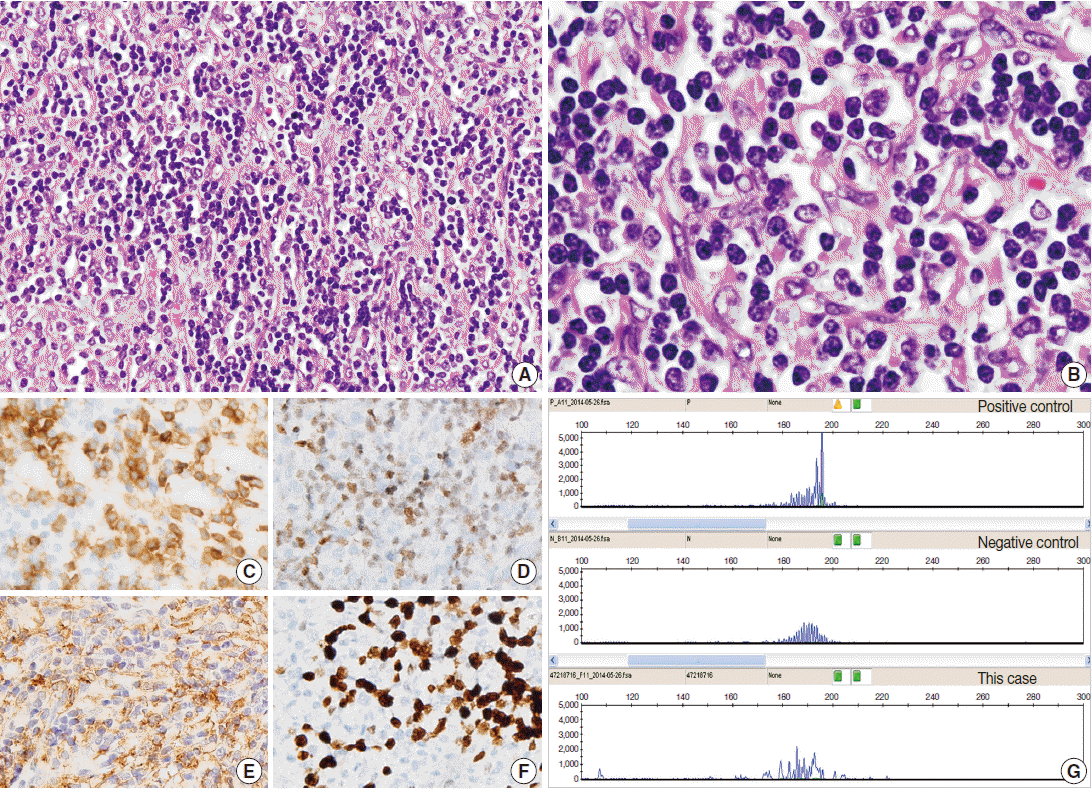
Fig. 2.Indolent T-lymphoblastic proliferation (iTLBP). (A) Nodular and diffuse areas of monotonous lymphoid cell infiltration in the interfollicular and perifollicular regions. (B) The cells show blastic nuclei with open chromatin and inconspicuous nuclei. (C–F) Cells are immunopositive for CD3 (C), terminal deoxynucleotidyl transferase (D), and CD33 (E), and have an increased Ki-67 labeling index (F). (G) Polymerase chain reaction study of the T-cell receptor gamma genes using BIOMED-2 primers shows no evidence of monoclonality.

- 1. Velankar MM, Nathwani BN, Schlutz MJ, et al. Indolent T-lymphoblastic proliferation: report of a case with a 16-year course without cytotoxic therapy. Am J Surg Pathol 1999; 23: 977-81. PubMed
- 2. Ohgami RS, Arber DA, Zehnder JL, Natkunam Y, Warnke RA. Indolent T-lymphoblastic proliferation (iT-LBP): a review of clinical and pathologic features and distinction from malignant T-lymphoblastic lymphoma. Adv Anat Pathol 2013; 20: 137-40. PubMed
- 3. Ohgami RS, Zhao S, Ohgami JK, et al. TdT+ T-lymphoblastic populations are increased in Castleman disease, in Castleman disease in association with follicular dendritic cell tumors, and in angioimmunoblastic T-cell lymphoma. Am J Surg Pathol 2012; 36: 1619-28. PubMed
- 4. Qian YW, Weissmann D, Goodell L, August D, Strair R. Indolent T-lymphoblastic proliferation in Castleman lymphadenopathy. Leuk Lymphoma 2009; 50: 306-8. PubMed
- 5. Ohgami RS, Sendamarai AK, Atwater SK, et al. Indolent T-lymphoblastic proliferation with disseminated multinodal involvement and partial CD33 expression. Am J Surg Pathol 2014; 38: 1298-304. PubMed
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 

- Unicentric Castleman Disease: Updates and Novel Insights Into Spindle Cell Proliferations and Aggressive Forms of a Localized Disease
FNU Alnoor, Alexandra Rangel, Matthew Luo, Oscar Silva, Karen M. Chisholm, Dennis O'Malley, Roger Warnke, Jyoti Kumar, Robert S. Ohgami
International Journal of Laboratory Hematology.2025; 47(1): 26. CrossRef - Indolent T-lymphoblastic proliferation with fibrolamellar hepatocellular carcinoma developed after colorectal adenocarcinoma: a case report
Wen Han, Bei Wang, Xiang Yong, Yi Zhang, Mingyu Shao, Chun Wang
Pathology and Oncology Research.2023;[Epub] CrossRef - Indolent T-lymphoblastic proliferation involving hepatocellular carcinoma—presentation in novel settings and comprehensive review of literature
Alireza Ghezavati, Christine A. Liang, Daniel Mais, Alia Nazarullah
Journal of Hematopathology.2023; 16(3): 167. CrossRef - Indolent T-lymphoblastic proliferation: a report of three cases
Zheng Yuanyuan, Xie Jianlan, Zhang Yanlin, Zhou Xiaoge
Virchows Archiv.2022; 480(5): 1121. CrossRef - Indolent T-Lymphoblastic Proliferation in Idiopathic Multicentric Castleman Disease
Nabin Raj Karki, Ahmed Samire Arfa, Natasha Savage, Abdullah Kutlar
Acta Haematologica.2022; 145(2): 214. CrossRef - Indolent T‐lymphoblastic proliferation: A systematic review of the literature analyzing the epidemiologic, clinical, and pathologic features of 45 cases
Arzu Saglam, Kunwar Singh, Sumanth Gollapudi, Jyoti Kumar, Nivaz Brar, Alexandra Butzmann, Roger Warnke, Robert S. Ohgami
International Journal of Laboratory Hematology.2022; 44(4): 700. CrossRef - The 5th edition of the World Health Organization Classification of Haematolymphoid Tumours: Lymphoid Neoplasms
Rita Alaggio, Catalina Amador, Ioannis Anagnostopoulos, Ayoma D. Attygalle, Iguaracyra Barreto de Oliveira Araujo, Emilio Berti, Govind Bhagat, Anita Maria Borges, Daniel Boyer, Mariarita Calaminici, Amy Chadburn, John K. C. Chan, Wah Cheuk, Wee-Joo Chng,
Leukemia.2022; 36(7): 1720. CrossRef - T-lymphoblastic leukemia/lymphoma with interfollicular growth pattern and Castleman-like morphologic features
Weijie Li, Alexander Kats, Linda D. Cooley, Midhat S. Farooqi, Keith August
Journal of Hematopathology.2021; 14(2): 163. CrossRef - Maladie de Castleman localisée avec prolifération lymphoblastique T indolente
Bertrand Chauveau, François Le Loarer, Julia Bacci, François Baylac, Pierre Dubus, Catherine Ling, Marie Parrens
Annales de Pathologie.2019; 39(1): 29. CrossRef - Sirolimus for the Treatment of Airway Obstruction due to Indolent T-Lymphoblastic Proliferation
Eric Moughames, Ana P. Kiess, Lee M. Akst, Antoine Azar
Case Reports in Immunology.2019; 2019: 1. CrossRef - Indolent T‐lymphoblastic proliferation concomitant with acinic cell carcinoma mimicking T‐lymphoblastic lymphoma: case report and literature review
Hajime Yasuda, Miyuki Tsutsui, Yasunori Ota, Masaru Tanaka, Norio Komatsu
Histopathology.2018; 72(5): 862. CrossRef - Indolent T-lymphoblastic proliferation: a name with specific meaning—reply
Bharat N. Nathwani, Rina Kansal, Xanthi Yiakoumis, Gerassimos A. Pangalis
Human Pathology.2015; 46(11): 1786. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure
TdT+ T-Lymphoblastic Proliferation in Castleman Disease


Fig. 1. Hyaline vascular-type Castleman disease. (A) Abdominal computed tomography demonstrates a well-defined homogeneous enhancing mass (arrow) in the retroperitoneum. (B) The mass exhibits a fleshy cut surface with central fibrosis. (C) Variably-sized follicles with multiple germinal centers are present. The interfollicular compartment is expanded with vascular proliferation. (D) Follicular structures appear smaller due to the regression of germinal centers. (E) Mantle zone lymphocytes have a laminated appearance, similar to onion skin. The vessel penetrating the atrophic follicle has a lollipop-like appearance. (F) Hyperplastic follicular dendritic cells are stained with CD21.
Fig. 2. Indolent T-lymphoblastic proliferation (iTLBP). (A) Nodular and diffuse areas of monotonous lymphoid cell infiltration in the interfollicular and perifollicular regions. (B) The cells show blastic nuclei with open chromatin and inconspicuous nuclei. (C–F) Cells are immunopositive for CD3 (C), terminal deoxynucleotidyl transferase (D), and CD33 (E), and have an increased Ki-67 labeling index (F). (G) Polymerase chain reaction study of the T-cell receptor gamma genes using BIOMED-2 primers shows no evidence of monoclonality.
Fig. 1.
Fig. 2.
TdT+ T-Lymphoblastic Proliferation in Castleman Disease

 E-submission
E-submission