A Rare Case of Tumor-to-Tumor Metastasis of Thyroid Papillary Carcinoma within a Pulmonary Adenocarcinoma
Article information
Tumor-to-tumor metastasis (TTM) is a rare phenomenon first reported several decades ago in Fried’s description of a bronchogenic carcinoma that metastasized to a meningioma [1]. According to previous studies, renal cell carcinoma and meningioma are common recipients, whereas lung and breast cancer are common donors [2]. Thus far, four cases of lung carcinoma harboring papillary thyroid carcinoma (PTC) metastasis have been reported in the English literature [3-6]. Here we present another case of PTC that metastasized to pulmonary adenocarcinoma.
CASE REPORT
A 56-year-old non-smoking male presented with a 3-month history of cough and sputum. On chest computed tomography, a 53-mm-sized ground-glass opacity in the left upper lobe (LUL) of the lung was identified (Fig. 1A left). On positron emission tomography, F-18 fluorodeoxyglucose uptake was detected in the left thyroid accompanied by lymphadenopathy (Fig. 1A right). Histological confirmation was performed for each lesion. Fine needle aspiration of thyroid and bronchoscopic biopsy of the lung lesion revealed PTC with cervical lymph node metastasis and pulmonary adenocarcinoma, respectively. Lobectomy of the LUL was performed prior to thyroid cancer treatment.
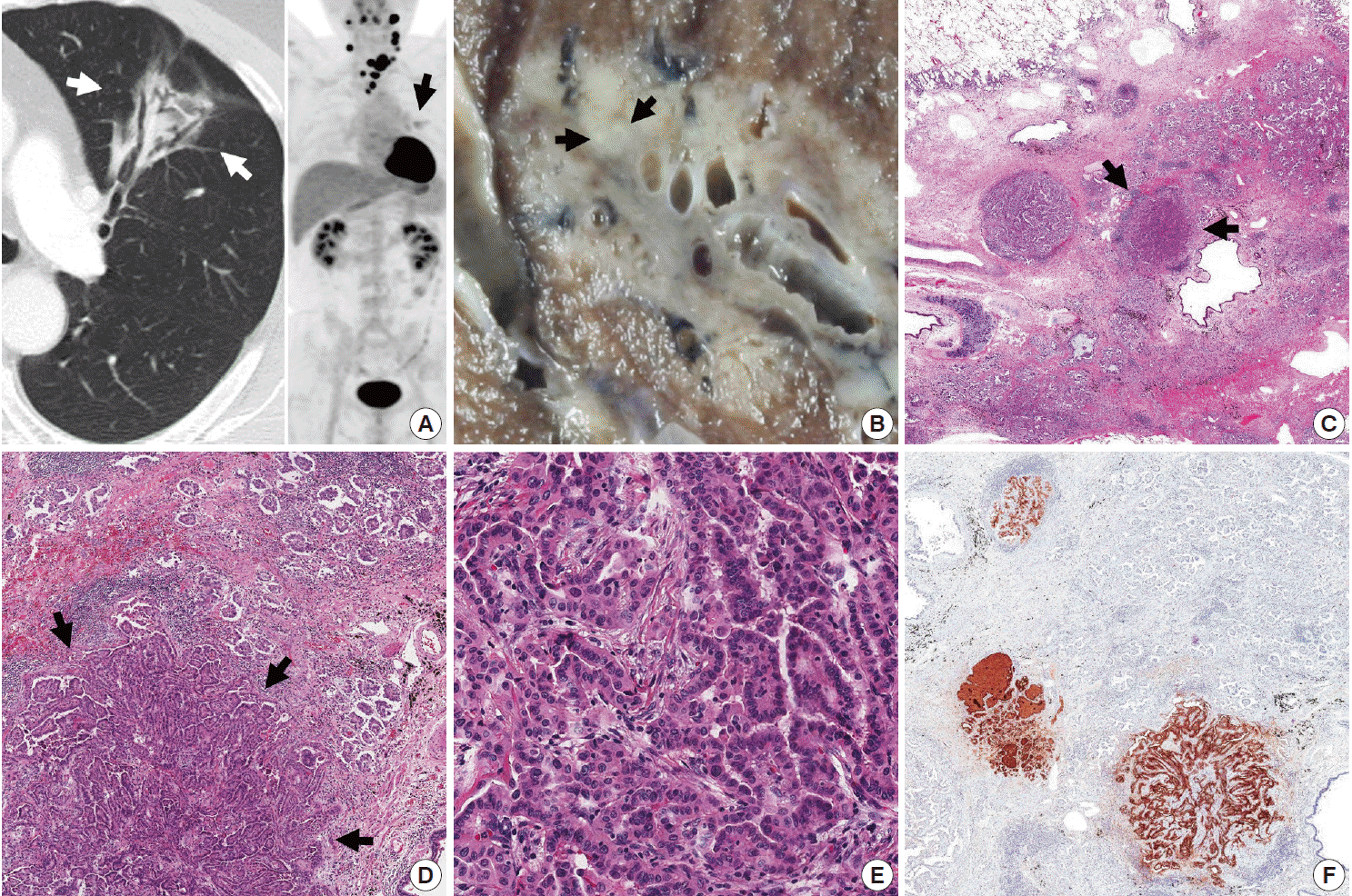
Metastasis of thyroid papillary carcinoma within a pulmonary adenocarcinoma. (A) Chest computed tomography shows ground-glass opacity (white arrows) in the left upper lobe. Positron emission tomography reveals F-18 fluorodeoxyglucose uptake in the left lobe of the thyroid, multiple cervical lymph nodes and the left upper lung (black arrow). (B) Grossly, metastatic papillary thyroid carcinoma (PTC) is a small, round, firm, white-tan nodule (arrows) located within an irregular, soft, grey lung mass. (C) Under low-power magnification, metastatic PTC (arrows) is distinguished from background pulmonary adenocarcinoma by its localized and compact arrangement of tumor cells. (D) Metastatic PTC (arrows) exhibits a papillary growth pattern and less fibrosis compared to the predominant acinar pattern and large-scale fibrosis of pulmonary adenocarcinoma. (E) Together with well-formed papillae, tumor cells of metastatic PTC have typical nuclear features including nuclear clearing and grooves. (F) Three metastatic PTCs are strongly positive for thyroglobulin on immunohistochemistry.
A single, well-defined, 0.6×0.6-cm-sized, round, firm, whitetan nodule was found in the peribronchial area within a 3.9×3.1-cm-sized, irregular, soft, grey mass in the anterior segment of the LUL, on gross examination (Fig. 1B) and low-power magnification (Fig. 1C). No other suspicious lesions were detected in the given specimen. The main lung lesion was diagnosed as conventional pulmonary adenocarcinoma and was composed of moderately differentiated adenocarcinoma with an acinar and papillary pattern accompanied by a focal micropapillary pattern (Fig. 1D). The small nodule within the adenocarcinoma (Fig. 1D) was comprised of papillae lined by cuboidal cells with nuclear clearing and grooves suggestive of PTC (Fig. 1E). Additional thyroglobulin immunohistochemical staining (1:1,000, Dako, Glostrup, Denmark) highlighted metastatic PTCs in a total of three foci (Fig. 1F). A metastatic papillary carcinoma was also identified in a separately submitted mediastinal lymph node.
Subsequent total thyroidectomy with central neck node dissection was performed one month after lobectomy. Bilateral PTCs (3.3×3 cm and 0.3×0.3 cm) and metastasis to 17 of 36 regional lymph nodes were identified on histologic examination.
DISCUSSION
Synchronous primary cancers are occasionally observed, but TTM is extremely rare; only about 100 cases have been reported in the English literature. Campbell et al. [7] proposed the concept of TTM, which can be distinguished from collision tumor based on following criteria: 1) more than one primary tumor; 2) the recipient tumor may be a true benign or malignant neoplasm; 3) the metastatic neoplasm is a true metastasis with established growth within the host tumor, not the result of contiguous growth (collision tumor) or tumor emboli; 4) primary tumors spreading into the lymphatic system in the setting of generalized lymphoreticular malignancy are excluded.
According to the ‘seed and soil hypothesis’ [8] of cancer metastasis, interactions between cancer cells (seed) and specific organ microenvironments (soil) determine the outcome of metastasis. Renal cell carcinoma and meningioma are both highly vascularized tumors, and have high lipid and glycogen content, which can provide a fertile environment for growth. However, pulmonary adenocarcinoma is a less likely candidate recipient tumor because it is often accompanied by fibrosis, rather than the “nutritious components” described above, and is less vascularized than normal lung tissue [3].
TTM is rare, but with the advent of new diagnostic tools and treatment strategies, reports of such cases are becoming more common. In the current study, despite the challenge of radiologic detection on account of its small size and location, metastatic PTC within pulmonary adenocarcinoma was observed both macroscopically and microscopically. The typical nuclear features and immunohistochemistry along with the patient’s history of PTC were helpful in establishing an accurate diagnosis. Regular radiologic follow-up is scheduled for this patient based on the potential for multiple metastases. Pathologists should consider the possibility of TTM when they encounter a histologically unusual component within a typical tumor of the primary organ because appropriate treatment will vary in cases of TTM.
Notes
Conflicts of Interest
No potential conflict of interest relevant to this article was reported.