Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 51(3); 2017 > Article
-
Brief Case Report
A Rare Case of Nodular Mucinosis of the Breast - Hyun Min Koh, Young Hee Maeng1, Bo Geun Jang1, Jae Hyuk Choi2, Chang lim Hyun,1
-
Journal of Pathology and Translational Medicine 2017;51(3):332-334.
DOI: https://doi.org/10.4132/jptm.2016.07.26
Published online: December 5, 2016
Department of Pathology, Jeju National University Hospital, Jeju, Korea
1Department of Pathology, Jeju National University Hospital, Jeju National University College of Medicine and Graduate School of Medicine, Jeju, Korea
2Department of Surgery, Jeju National University Hospital, Jeju National University College of Medicine and Graduate School of Medicine, Jeju, Korea
- Corresponding Author Chang lim Hyun, MD, PhD Department of Pathology, Jeju National University School of Medicine, 15 Aran 13-gil, Jeju 63241, Korea Tel: +82-64-754-8818, Fax: +82-64-717-1131, E-mail: venisua@jejunu.ac.kr
© 2017 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- A 22-year-old previously healthy woman visited our hospital complaining of a soft mass on her right breast that had been present for a year. Recently, the lesion had gradually increased in size. She had no other complaints, such as pain or nipple discharge. There was no relevant family or personal medical history. She had never been pregnant and had never taken exogenous hormones or any drugs. The patient showed no evidence of Carney complex. Upon physical examination, a well-demarcated, protruding and movable cystic nodule was present at 10 o’clock on the areola of her right breast. The skin surface covering the nodule exhibited no specific changes and the nipple was unremarkable. Ultrasonography of the breast revealed a 1-cm ovoid cystic nodule located in the dermal layer, which was presumed to be a benign lesion. Surgical resection was carried out without other diagnostic tests, such as fine needle aspiration or mammography.
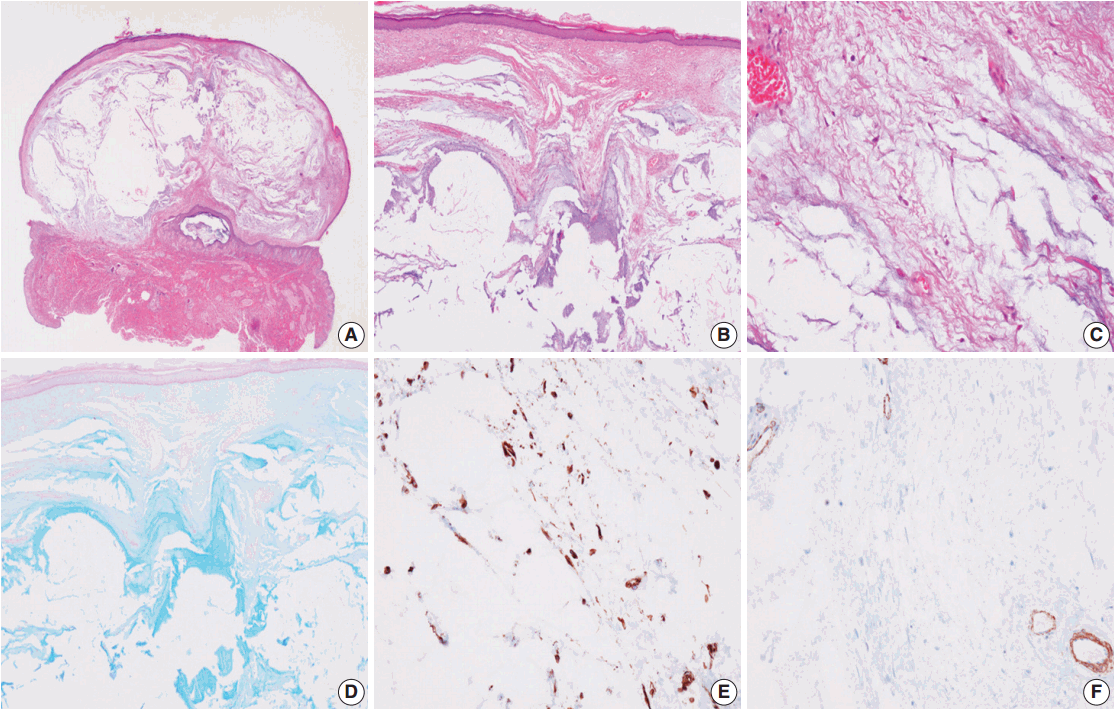
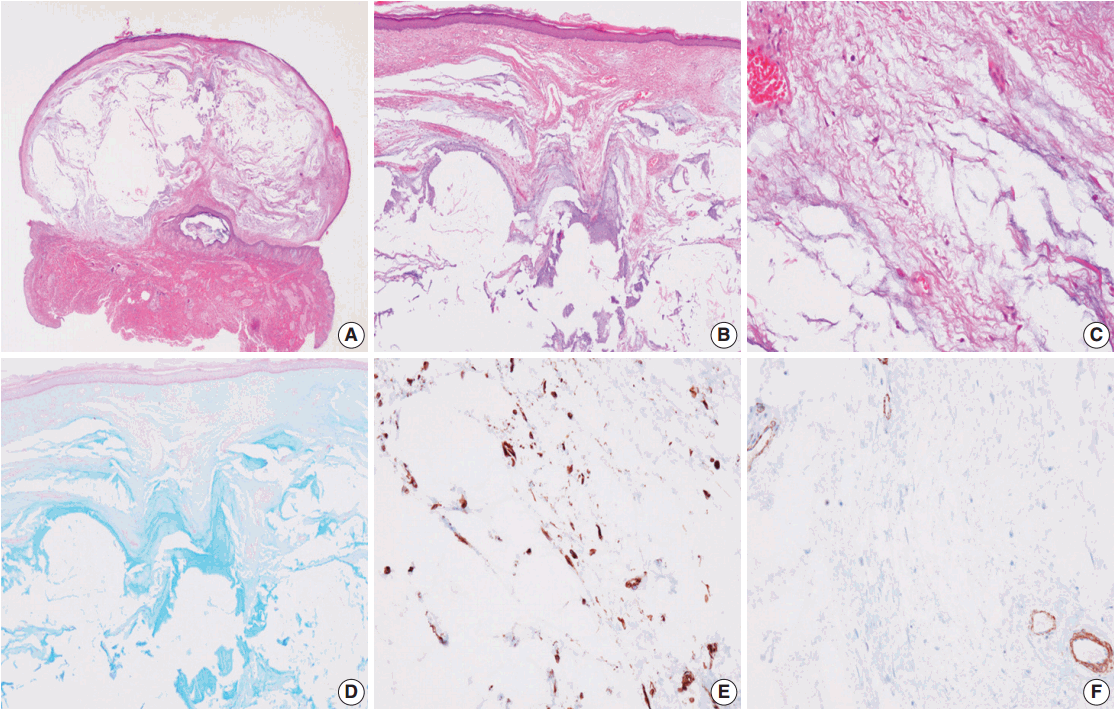
- Grossly, the specimen was an ovoid cystic nodule measuring 1.1 × 0.6 × 0.6 cm and was covered by an ellipse of normal skin. The outer surface of the nodule was smooth and glistening. Upon sectioning, the cyst was well circumscribed, but not encapsulated (Fig. 1A) and was filled with pale tan, gelatinous material surrounded by grayish white fibrous tissue (Fig. 1B). Histologically, the lesion consisted of abundant myxoid tissue with a few scattered spindle cells and had a slightly multilobular appearance with fibrocollagenous stroma. Capillaries and thin-walled vessels were noted within the nodule (Fig. 1C). Rare histiocytes, lymphocytes, and plasma cells were seen in the nodule. Neither mammary ducts nor epithelial elements were observed. Spindle cells showed bland-looking nuclei and elongated amphophilic cytoplasm with no atypia or mitosis. The myxoid tissue was analyzed via Alcian blue staining (pH 2.5) and periodic acid-Schiff (PAS) testing. Alcian blue stained the myxoid stroma bright blue (Fig. 1D) and PAS was negative, indicating the existence of acidic mucopolysaccharides. The spindle cells showed reactivity to vimentin (Fig. 1E) but were nonreactive to smooth muscle actin (Fig. 1F). Based on these findings, we confirmed nodular mucinosis of the breast. Postoperative status was good, and the patient has been in remission for 3 years since the surgery.
CASE REPORT
- Nodular mucinosis of the breast is an extraordinary entity that has been reported fewer than 10 times in the English literature since the first case was described in 1989 (Table 1) [1-7]. Several common clinical and pathologic features were observed in previous reports. Nodular mucinosis of the breast is predominantly found in young women ranging from 15 to 72 years [2-6]. The typical clinical manifestation is a soft mass under the nipple or in the subareolar region that gradually increases in size, and occasionally presents with nipple discharge or pain [2-6]. Ultrasonography usually reveals a well-circumscribed, lobulated, homogenous, hypoechoic mass and mammography shows a roundlobular, radiopaque mass without microcalcifications or spicula formation [2-5]. Fine needle aspiration typically reveals mucin without epithelial elements or malignant evidence [2,4,5]. The treatment of choice is surgical excision, which usually leads to a successful outcome without residual disease. Nodular mucinosis of the breast does not have an established link with Carney complex [5], which is an autosomal dominant syndrome characterized by multiple neoplasias, including myxomas at various sites, endocrine tumors, and lentigenosis related to genetic defects [8].
- Grossly, the lesion is usually a small, ovoid protruding nodule, ranging from 0.9 to 3.2 cm in diameter [2-6]. The cut surface demonstrates a well-circumscribed but not encapsulated, multinodular lesion that is grayish-white, grayish-pink, or yellow-to-tan in color [2-6] and has a myxoid, mucinous or gelatinous consistency [3-6]. The histological features of nodular mucinosis of the breast include a multinodular myxoid or mucinous lesion separated by fibrocollagenous stroma [2-6]. The lesion consists of sparse spindle cells, which have bland and elongated nuclei, scant and/or pale cytoplasm, and indistinct cell boarders [2,4,5]. Rarely histiocytes, lymphocytes, plasma cells, and/or mast cells can be seen within and around the nodules [2-6], and some capillaries or small vessels are seen within the lesions [3,5,6]. The lesion neither contains nor invades the breast parenchyma [2-4,6]. Also, no epithelial components can be identified [2-6]. Myxoid or mucinous areas are stained intensely with Alcian blue and Hale colloidal iron, but are negative on PAS, proving the existence of acid mucopolysaccharide [2-6]. The spindle cells are positive for calponin, vimentin, and smooth muscle actin and negative for cytokeratin, smooth muscle myosin, and S-100, probably arising from myofibroblasts [2-5].
- Clinicians need to be able to differentiate nodular mucinosis of the breast from other myxoid and mucinous lesions such as mucinous carcinoma, micropapillary carcinoma in situ with excessive mucin, fibroadenoma with myxomatous stroma and mucocele-like lesions [2-5]. Nodular mucinosis exhibits mucin with no epithelial elements or malignant evidence on fine needle aspiration [2,4,5]. The presence of an epithelial cell component in the mucin suggests other myxoid and mucinous lesions [4,7]. In addition, cytologically mucocele-like lesions are characterized by abundant mucin and monolayer clusters or sheets of epithelial cells without nuclear atypia and is usually associated with microcalcifications, which is a feature not typical of nodular mucinosis [4]. Mucin in mucocele-like lesions is usually stained with PAS but appears negative on Alcian blue and Hale colloidal iron staining [4,7].
- Considering that nodular mucinosis has no epithelial components in acidic mucin pools, differentiation is not a major challenge, so long as spindle cells are not mistaken for epithelial cells.
- We have discussed a very rare case of nodular mucinosis of the breast. Although this entity is benign, it is imperative that it be distinguished from other lesions that occur near the nipple, especially mucinous carcinoma, via pathologic examination after surgical excision.
DISCUSSION
| Reference | Age (yr) | M/F | Location | Size (cm) | Follow-up | Prognosis |
|---|---|---|---|---|---|---|
| Michal et al. [6] (1998) | 40 | M | Left nipple | 2 × 1.5 × 1.5 | 6 yr | No recurrence |
| 28 | F | Right nipple | 1.5 × 1.5 × 1 | 3 yr | No recurrence | |
| 29 | F | Right nipple | 2.5 × 2.5 × 2 | 6 mo | No recurrence | |
| Koide et al. [5] (2002) | 30 | F | RUO to N | 2.9 × 2.1 | NA | NA |
| Sanati et al. [4] (2005) | 21 | F | Left nipple | 1.5 × 0.9 × 0.8 | NA | NA |
| Chisholm et al. [3] (2010) | 72 | F | Right subareolar | 0.9 × 0.8 × 0.3 | 4 mo | No recurrence |
| Manglik et al. [2] (2010) | 15 | F | Right subareolar (supernumerary nipple) | 1 × 1 × 0.5 | NA | NA |
| Bulut et al. [7] (2015) | 37 | F | Right subareolar | 3.2 × 2.5 × 1.7 | 29 mo | No recurrence |
| Our case | 22 | F | Right subareolar | 1.1 × 0.6 × 0.6 | 3 yr | No recurrence |
- 1. Wee A, Tan CE, Raju GC. Nerve sheath myxoma of the breast: a light and electron microscopic, histochemical and immunohistochemical study. Virchows Arch A Pathol Anat Histopathol 1989; 416: 163-7. PubMed
- 2. Manglik N, Berlingeri-Ramos AC, Boroumand N, Eltorky M. Nodular mucinosis of the breast in a supernumerary nipple: case report and review of the literature. J Cutan Pathol 2010; 37: 1178-81. ArticlePubMed
- 3. Chisholm C, Greene JF Jr. Nodular mucinosis of the breast: expanding our understanding with an unusual case. Am J Dermatopathol 2010; 32: 187-9. ArticlePubMed
- 4. Sanati S, Leonard M, Khamapirad T, Eltorky MA. Nodular mucinosis of the breast: a case report with pathologic, ultrasonographic, and clinical findings and review of the literature. Arch Pathol Lab Med 2005; 129: e58-61. ArticlePubMedPDF
- 5. Koide N, Akashi-Tanaka S, Fukutomi T, Nanasawa T, Hasegawa T. Nodular mucinosis of the breast: a case report with clinical and imaging findings. Breast Cancer 2002; 9: 261-4. ArticlePubMedPDF
- 6. Michal M, Ludvíková M, Zámecnik M. Nodular mucinosis of the breast: report of three cases. Pathol Int 1998; 48: 542-4. ArticlePubMed
- 7. Bulut T, Celik B, Nassar A, Yalcin AD. Nodular mucinosis of breast: a case report. J Med Cases 2015; 6: 457-9. Article
- 8. Stratakis CA, Carney JA, Lin JP, et al. Carney complex, a familial multiple neoplasia and lentiginosis syndrome: analysis of 11 kindreds and linkage to the short arm of chromosome 2. J Clin Invest 1996; 97: 699-705. ArticlePubMedPMC
REFERENCES
Figure & Data
References
Citations

- Practical approach to diagnosis of breast lesions with heterologous components
Abeer M Shaaban, Cecily Quinn, Emad Rakha
Diagnostic Histopathology.2024; 30(2): 100. CrossRef - Nodular Mucinosis of the Breast: A Case Report
Ana Y Sandoval-Mussi, Ana S Armenta-Quiroga, Alba Mayra Padilla-Correa, Roberto Enrique Hernandez Peña
Cureus.2024;[Epub] CrossRef - New and emerging conditions of acquired cutaneous mucinoses in adults
F. Rongioletti
Journal of the European Academy of Dermatology and Venereology.2022; 36(7): 1016. CrossRef - Altered presence of extra cellular matrix components in murine skin cancer: Modulation by Azadirachta indica leaf extract
N.A. Chugh, A. Koul
Journal of Traditional and Complementary Medicine.2021; 11(3): 197. CrossRef - Mucinosis nodular de la mama
Bernardo Weil Lara, Daniela Pérez Martínez, Beatriz Romero Madrid
Revista Española de Patología.2020; 53(1): 42. CrossRef - Lycopene enriched tomato extract suppresses chemically induced skin tumorigenesis in mice
Ashwani Koul, Mohinder Pal Bansal, Aniqa Aniqa, Harsh Chaudhary, Neha Arora Chugh
International Journal for Vitamin and Nutrition Research.2020; 90(5-6): 493. CrossRef - A review of mucinous lesions of the breast
Paula S. Ginter, Xiaoyu Tang, Sandra J. Shin
The Breast Journal.2020; 26(6): 1168. CrossRef - Mesenchymal Lesions of the Breast: What Radiologists Need to Know
Debra S. Whorms, Michael D. C. Fishman, Priscilla J. Slanetz
American Journal of Roentgenology.2018; 211(1): 224. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure

Fig. 1.
| Reference | Age (yr) | M/F | Location | Size (cm) | Follow-up | Prognosis |
|---|---|---|---|---|---|---|
| Michal et al. [6] (1998) | 40 | M | Left nipple | 2 × 1.5 × 1.5 | 6 yr | No recurrence |
| 28 | F | Right nipple | 1.5 × 1.5 × 1 | 3 yr | No recurrence | |
| 29 | F | Right nipple | 2.5 × 2.5 × 2 | 6 mo | No recurrence | |
| Koide et al. [5] (2002) | 30 | F | RUO to N | 2.9 × 2.1 | NA | NA |
| Sanati et al. [4] (2005) | 21 | F | Left nipple | 1.5 × 0.9 × 0.8 | NA | NA |
| Chisholm et al. [3] (2010) | 72 | F | Right subareolar | 0.9 × 0.8 × 0.3 | 4 mo | No recurrence |
| Manglik et al. [2] (2010) | 15 | F | Right subareolar (supernumerary nipple) | 1 × 1 × 0.5 | NA | NA |
| Bulut et al. [7] (2015) | 37 | F | Right subareolar | 3.2 × 2.5 × 1.7 | 29 mo | No recurrence |
| Our case | 22 | F | Right subareolar | 1.1 × 0.6 × 0.6 | 3 yr | No recurrence |
M, male; F, female; RUO to N, right upper outer to nipple; NA, not available.

 E-submission
E-submission