Diagnostic distribution and pitfalls of glandular abnormalities in cervical cytology: a 25-year single-center study
Article information
Abstract
Background
Detection of glandular abnormalities in Papanicolaou (Pap) tests is challenging. This study aimed to review our institute’s experience interpreting such abnormalities, assess cytohistologic concordance, and identify cytomorphologic features associated with malignancy in follow-up histology.
Methods
Patients with cytologically-detected glandular lesions identified in our pathology records from 1995 to 2020 were included in this study.
Results
Of the 683,197 Pap tests performed, 985 (0.144%) exhibited glandular abnormalities, 657 of which had tissue follow-up available. One hundred eighty-eight cases were cytologically interpreted as adenocarcinoma and histologically diagnosed as malignant tumors of various origins. There were 213 cases reported as atypical glandular cells (AGC) and nine cases as adenocarcinoma in cytology, yet they were found to be benign in follow-up histology. In addition, 48 cases diagnosed with AGC and six with adenocarcinoma cytology were found to have cervical squamous lesions in follow-up histology, including four squamous cell carcinomas. Among the cytomorphological features examined, nuclear membrane irregularity, three-dimensional clusters, single-cell pattern, and presence of mitoses were associated with malignant histology in follow-up.
Conclusions
This study showed our institute’s experience detecting glandular abnormalities in cervical cytology over a 25-year period, revealing the difficulty of this task. Nonetheless, the present study indicates that several cytological findings such as membrane irregularity, three-dimensional clusters, single-cell pattern, and evidence of proliferation could help distinguishing malignancy from a benign lesion.
The introduction of cervical screening has reduced the numbers of new cases and deaths caused by cervical cancer; this success has mainly been attributed to the Papanicolaou (Pap) test, which is a main cervical screening modality used worldwide [1,2]. For instance, under the Korean cervical cancer screening program and between the years 1999 and 2017, new cervical cancer cases and deaths dropped significantly [3]. However, despite its huge success, the Pap test is by no means perfect. According to the 2020 GLOBOCAN estimates, cervical cancer still ranked as the fourth most common malignancy both in incidence (6.5%) and mortality (7.7%) in women globally [4].
Pap test is primarily considered a screening test for squamous cancer and its precursors, exhibiting high specificity for this task [5], while it is often used either as a stand-alone test or in association with human papillomavirus testing, as a part of various screening algorithms [6-9]. However, its diagnostic accuracy regarding glandular cancers and their precursors is considered suboptimal; reasons include the relative rarity of glandular abnormalities in Pap tests, compared to their squamous counterparts, the difficulty sampling them, also the pathologists’ lack of experience with their cytomorphologic criteria and the reported interobserver variability [10-12]. “Atypical glandular cells” (AGC) is an uncommon cytologic interpretation used to interpret cases with cytomorphologic glandular changes exceeding reactive atypia, yet falling short to be reported as in situ or invasive carcinomas [13-15].
Squamous cell carcinoma and adenocarcinoma (ADC) are the first and second most common histologic types of cervical cancer, respectively [16,17]. Notably, whereas the incidence of squamous cell carcinoma has decreased significantly the last years mainly due to the successful cervical screening programs implemented, ADC has not followed a similar trend [18-22]. Adenocarcinomas often behave more aggressively, while they have been associated with worse prognosis and higher metastasis rates, also with worse response to therapy compared to squamous cervical cancers [16,17,23,24]. Consequently, the early detection of cervical ADC or its precursors would directly affect patients’ quality of life and survival rates. However, this task is challenging in both conventional and liquid-based cytology (LBC) [11,25]. Due to the reported suboptimal diagnostic performance of Pap tests for the reasons mentioned before, more data are needed regarding cytologically-detected glandular abnormalities, in order to enhance our ability to detect them accurately.
In this single-center study, we evaluated the current status, diagnostic distribution, cytohistological association, and pitfalls of glandular abnormalities in cervical cytology. Additionally, we also evaluated selected cytomorphologic findings in Pap tests with glandular abnormalities associated with the presence of malignancy in subsequent follow-up biopsies.
MATERIALS AND METHODS
In this retrospective study, the records of Seoul National University Hospital were searched within the period from January 1995 to December 2020 to identify all reported cervical cytology cases with glandular abnormalities. These cases were prepared either as LBC slides or conventional smears. Among the 683,197 Pap tests over this 25-year period, 985 cases from 923 patients were reported with a glandular abnormality, while the 657 of these with available surgical pathology follow-up were included in the study. Of the 985 Pap tests, 322 (32.7%) were prepared as conventional smears, whereas 663 (67.3%) as LBC. The cytologic interpretations regarding the glandular abnormalities were made by board-certified cytopathologists of our laboratory, based on the following categories of the Bethesda system [5,26]: atypical glandular cells not otherwise specified (AGC-NOS), atypical endocervical cells (AGC-EC), atypical endometrial cells (AGC-EM), atypical glandular cells favor neoplastic (AGC-FN), and ADC. Several Pap tests that were diagnosed as atypical glandular cells of undetermined significance, favor reactive based on the Bethesda system 1991, were considered AGC-NOS lesions in 2014 Bethesda system. Surgical pathology follow-up included any of the following samples: cervical biopsies, endocervical curettages, loop electrosurgical excision procedure or conizations, endometrial curettages, and hysterectomies.
A few cytomorphologic features of selected Pap test cases exhibiting glandular abnormalities and cytohistologic discrepant findings were also compared between the cases subsequently found to be histologically benign and malignant, to identify cytologic criteria associated with malignancy. These features included architectural characteristics (overlapping; presence of single cells; and presence of three-dimensional clusters), nuclear enlargement, irregular nuclear membranes, increased nuclear-to-cytoplasm (N/C) ratio, nuclear hyperchromasia, prominent nucleoli, and mitotic activity. The Fisher exact test was used to identify the importance of cytomorphologic features in the diagnosis of malignancies. A p-value of <.05 was considered statistically significant.
RESULTS
Distribution of glandular abnormalities in cervical cytology
Among 683,197 Pap tests interpreted from January 1995 to December 2020 in our center, the number of cases with glandular abnormalities was 985 (0.144%), of which 244 (24.8%) were diagnosed as ADC. In the cytological evaluation of the 741 cases with AGC, the distribution of AGC subcategories according to the Bethesda system was as follows: AGC-NOS 667 (67.7%), AGC-EC 32 (3.2%), AGC-EM 16 (1.6%), and AGC-FN 26 (2.6%) (Fig. 1). The mean age of the patients was 49 years (range, 14 to 86 years).
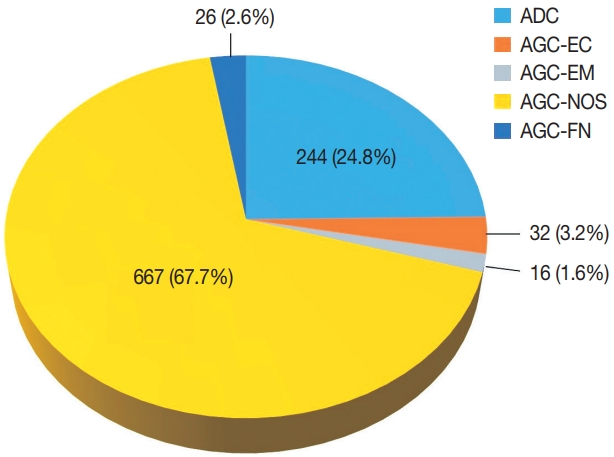
Distribution of glandular abnormalities in the Papanicolaou tests interpreted in our institute over a 25-year period. ADC, adenocarcinoma; AGC-EC, atypical endocervical cells; AGC-EM, atypical endometrial cells; AGC-NOS, atypical glandular cells not otherwise specified; AGC-FN, atypical glandular cells favor neoplastic.
Assessment of cytohistologic concordance in our cohort
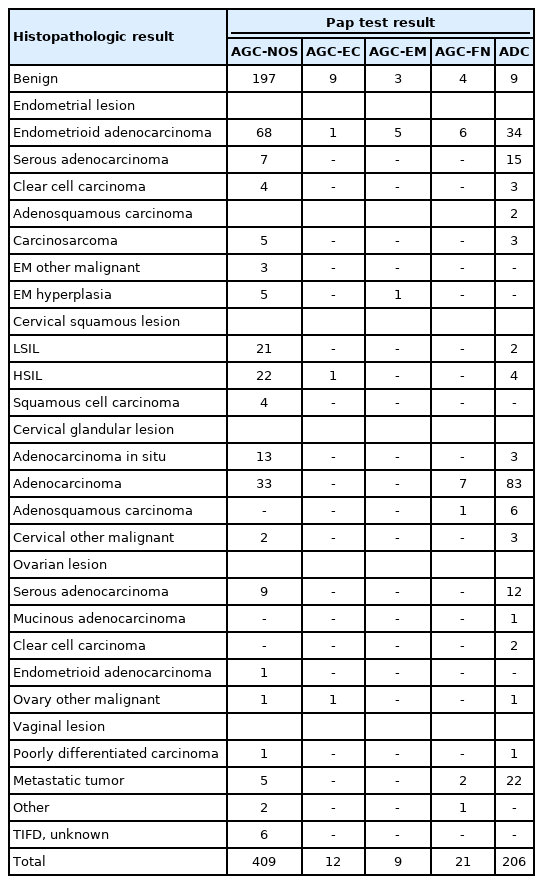
Of the 985 Pap tests interpreted with glandular abnormalities, histologic follow-up was available for 657 cases (66.7%). Among them, 409 cases (62.3%) were interpreted as AGC-NOS, 206 (31.4%) as ADC, 21 (3.2%) as AGC-FN, 12 (1.8%) as AGC-EC, and nine (1.4%) as AGC-EM. The cytohistologic concordance was summarized by referring to the Quality Improvement program recommended by the Korean Society for Cytopathology [27].
Table 1 shows the cytohistopathological correlations of the patients according to subclassification of glandular lesions. One hundred eighty-eight cases were cytologically interpreted as ADC and histologically diagnosed as malignant tumors, including the cervix, endometrium, ovary, and other organ origins. Among the cases with AGC Pap test interpretation, 213 were found to be benign in follow-up histology, while most of the others were diagnosed as malignant lesions. In addition, there were 48 cases diagnosed with an AGC and six cases with ADC cytologically, where a cervical squamous lesion was detected in their paired histology, including four squamous cell carcinomas. There was also a reported coexistence of glandular and squamous abnormalities in 50 Pap tests (AGC-NOS, 44; AGC-EM, 1; AGC-FN, 1; ADC, 4); these cases were solely categorized based on their glandular component. Notably, nine cases with an ADC cytologic interpretation were histologically diagnosed as benign.
Cytomorphologic features of AGC associated with malignancy in follow-up histology
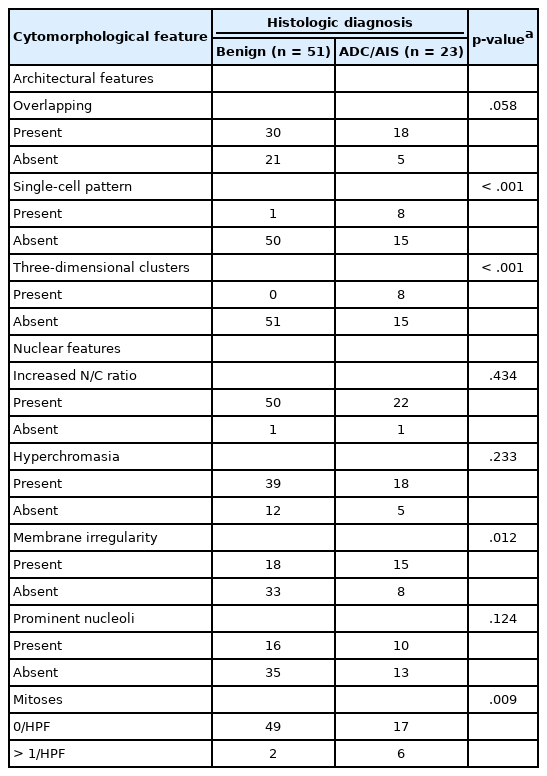
We also reviewed a few cytomorphologic features in some of our cytology AGC cases exhibiting cytohistologic discordance. Seventy-four AGC cases with available slides in our records were selected. Fifty-one cases with AGC cytology diagnosed as benign, 14 as cervical ADC, and nine as cervical ADC in situ (AIS) in their follow-up histology were included. Histologically, cases diagnosed with diseases other than cervical ADC or AIS were excluded. We examined the abnormal glandular cells in these Pap tests to identify cytomorphologic features associated with subsequent malignant histology. Table 2 shows the comparison of selected features in the 74 eligible cases examined, according to their histologic follow-up. Whereas irregular nuclear membranes, three-dimensional clusters, single-cell pattern, and presence of mitoses were statistically significant (p<.05) for the presence of malignancy, increased N/C ratios, overlapping, nuclear hyperchromasia, and prominent nucleoli were not (p>.05). Fig. 2 shows some cytomorphologic features of the Pap smear samples from some AGC cases, histologically-confirmed as malignant.
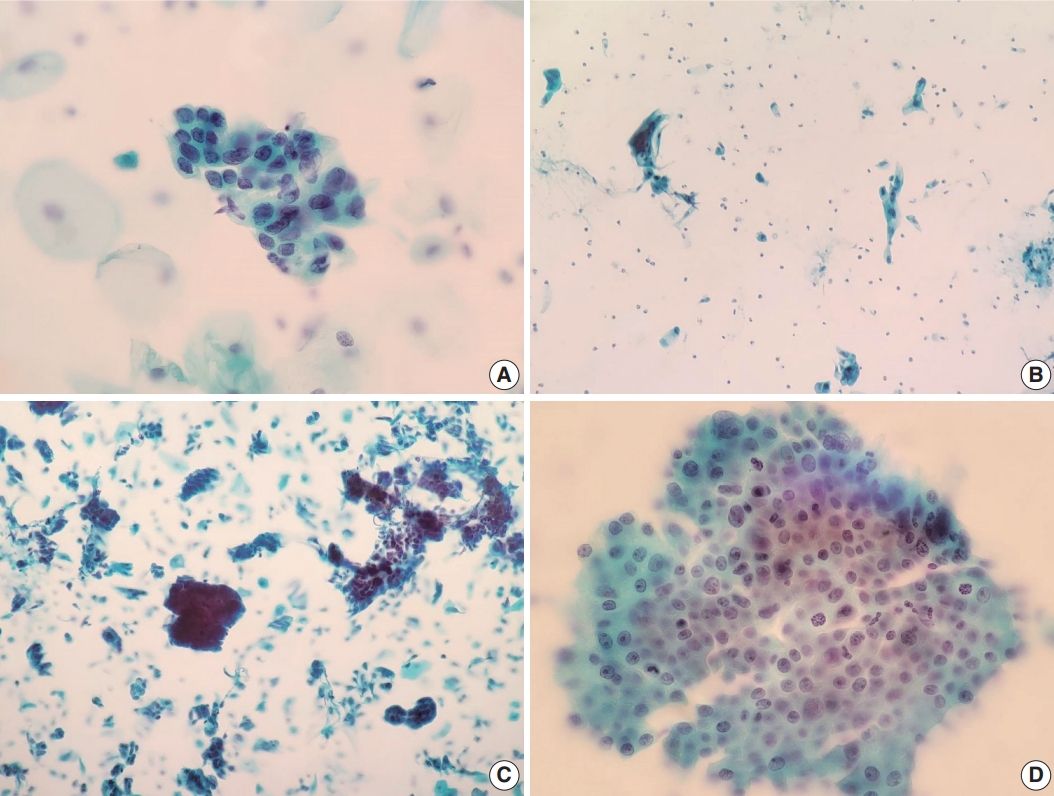
Cytomorphologic features of histologically-confirmed malignant cases. (A) Atypical glandular cells not otherwise specified (AGC-NOS). Groups of cells showing nuclear membrane irregularity. Follow-up histology revealed adenocarcinoma in situ (Papanicolaou [Pap] stain). (B) AGC-NOS. Some scattered atypical cells showing single-cell pattern. Follow-up histology revealed adenocarcinoma (Pap stain). (C) AGC-NOS. Cell clusters showing three-dimensional architecture with sharper, smoother margins. Follow-up revealed adenocarcinoma (Pap stain). (D) Atypical glandular cells favor neoplastic. Sheet of crowded cells with mitotic activity. Histological diagnosis was adenocarcinoma (Pap stain).
DISCUSSION
Although the efficacy of cervical cytology diagnosing squamous cell carcinoma and its precursors is well-established, detecting glandular abnormalities is a challenge due to their rarity, pathologists’ lack of experience with their cytomorphologic criteria, and poor interobserver reproducibility [10-12]. The aim of the present single-center study was to investigate the diagnostic distribution and assess the cytohistologic concordance of glandular abnormalities in cervical cytology, also to identify selected cytomorphologic findings associated with malignancy in follow-up surgical pathology.
According to our findings, glandular abnormalities accounted for 0.144% of all cervical cytology cases in our center from 1995 to 2020, showing their rarity and the diagnostic challenge interpreting them. This finding is consistent with what is reported in the literature [15,28,29]. In respect of the distribution of glandular lesions, none was diagnosed as AIS in cytology. Of the 16 cases that were histologically-confirmed to be cervical AIS, 13 were interpreted as AGC-NOS and three as ADC in cytology. This indicates that identifying AIS in cytology is a rather challenging task. Previous studies have identified the pitfalls of the AIS cytologic diagnosis, also its suboptimal accuracy and low levels of interobserver agreement [30-32]. Some authors have also reported that many AIS lesions could be interpreted as AGC, AGC-FN, ADC, or squamous intraepithelial lesions in cervical cytology [32,33].
Assessing the cytohistologic correlation of the glandular abnormalities detected in our cervical cytology cohort, we found that most Pap test cases reported to have glandular abnormalities cytologically actually had some significant lesions in their subsequent histopathology. One hundred eighty-eight out of 657 cases (28.6%) were turned out to be completely concordant, all of which were diagnosed as malignant tumors in follow-up histology (including cervical 92, endometrial, and ovarian 73). Also, there were 121 cases reported as AGC in cervical cytology, which turned out to be malignant tumors of various origins. On the other hand, 213 AGC Pap tests were histologically benign. Zhao et al. [25] analyzed 662 patients with an AGC cytologic interpretation and available tissue biopsy material and found that AGC cytology revealed cancer in 15.3% of the cases during histologic follow-up, most likely located in the cervix (8.3%), the endometrium (6.3%), and the ovaries (0.6%), respectively. In another study by Pradhan et al. [34], the histologic diagnoses of 3,709 AGC cases consisted of: negative (70.5%), cervical intraepithelial neoplasia/low grade squamous intraepithelial lesion (LSIL) and high grade squamous intraepithelial lesion (HSIL) (20.7%), endometrial ADC (5.5%), endocervical AIS and ADC (1.9%), and metastatic carcinomas (0.5%).
We also reviewed 74 AGC Pap tests to identify any cytomorphologic feature differences between the cases confirmed as benign and malignant during follow-up surgical pathology. In this examination, irregular nuclear membranes, three-dimensional clusters, single-cell pattern, and presence of mitoses were found to be significantly associated with malignancy in subsequent histology. On the contrary, no significant association was identified regarding increased N/C ratio, nuclear hyperchromasia, prominent nucleoli, or overlapping. These particular findings are largely concordant with what has so far been reported the literature. Raab et al. [35] showed that the presence of single dysplastic cells, nuclear membrane irregularities, and reduced amount of cytoplasm indicated cancer or a cancer precursor in histology. In another study by Yucel Polat et al. [29], the presence of feathering, papillary pattern, polarity loss, 3D clusters, irregular nuclear membranes, and prominent nucleoli were found to be significant; in contrast, the formation of rosettes, overlapping, increased N/C ratio, and nuclear hyperchromasia were not significantly associated with cancer in follow-up histology. Torres et al. [36] showed that finding cells exhibiting high N/C ratio and dyskeratosis indicated intraepithelial neoplasia or cancer, whereas glandular lesions were composed of cells with reduced amount of cytoplasm, nuclear membrane irregularity, and macronuleoli. Lastly, Reynolds et al. [37] reported that the presence of single dysplastic cells, 3D clusters, intracytoplasmic neutrophils, increased N/C ratio and larger nuclei, nuclear border irregularity, reniform-shaped nuclei, polarity loss, overlapping, and macronucleoli were significantly associated with a clinically significant lesion (HSIL or cancer) in surgical pathology follow-up.
Whenever possible, it is necessary to identify the cytomorphologic differences between squamous and glandular abnormalities in Pap tests, in addition to the cytologic features observed in benign glandular lesions that could mimic malignancy, to reduce potential misinterpretations. AGC is often found to be a benign lesion or a squamous intraepithelial lesion (e.g., a HSIL with endocervical gland involvement), rather than a glandular abnormality, in follow-up histology [34,38]. HSIL with endocervical gland involvement could indeed be misinterpreted as a glandular abnormality in cervical cytology. However, the loss of polarity within the hyperchromatic crowded groups, the flattening of the cells at the periphery of such groups, and the identification of single squamous dyskaryotic cells could help identify such lesions as squamous rather than glandular [26,38].
Some cases in our cohort included histologically benign cases interpreted as ADCs in cytology. Interestingly, among the cases interpreted as AGCs or ADCs in cytology, there were a few cases that were neither ADC nor squamous cell carcinoma in histology, including a smooth muscle tumor of uncertain malignant potential, an ovarian diffuse large B-cell lymphoma, an extramammary Paget disease of vulva, a small cell carcinoma, and a poorly differentiated carcinoma of cervix. The pathologists’ lack of experience and/or the presence of ambiguous cytomorphological criteria may be responsible for their misinterpretation.
A limitation of this study is that a few of our cases cytologically containing both glandular and squamous abnormalities (e.g., ACG-NOS and atypical squamous cells-cannot exclude HSIL (ASC-H) were solely classified based on their glandular component in this study, before assessing our cases’ distribution and cytology-histology correlation. According to the literature, glandular and squamous lesions in the cervix often coexist [39,40]. In our study, 50 of the 657 cases with histologic follow-up diagnosis were found to have both glandular and squamous abnormalities in their cytology reports. Forty-four of 409 AGC-NOS cases exhibited such coexistence, whereas 19 of them were finally diagnosed as cervical squamous neoplasias (LSIL, HSIL, or invasive squamous cell carcinoma) during surgical pathology follow-up, without any glandular lesions present. As previously mentioned, we evaluated only the glandular component for the cytohistologic correlation assessment of such cases. For example, a case interpreted as AGC-NOS and ASC-H in cytology followed by an LSIL diagnosis in histology, was regarded as a lesion with AGC-NOS only, ignoring its cytologic interpretation about squamous component. This way of classification, however, can be controversial, as it may not carry a major clinical impact when AGC patients end up having a squamous lesion.
In conclusion, this study showed the current status of glandular abnormalities detected by cervical cytology in a single center over a 25-year-period. They revealed a few cytomorphologic features, such as nuclear membrane irregularity, three-dimensional clusters, single-cell pattern and presence of mitoses, associated with malignancy in follow-up histology. As detecting glandular lesions is rare in Pap tests and pathologists are often unfamiliar with them, we hope this study will add some value to the relevant literature.
Notes
Ethics Statement
All procedures performed in the current study were approved by the Institutional Review Board (IRB) of Seoul National University Hospital (IRB No. H-2112-004-1277) in accordance with the 1964 Helsinki declaration and its later amendments. The committee waived the demand to obtain informed consent.
Availability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Code Availability
Not applicable.
Author contributions
Conceptualization: CL, HSR. Data curation: JAS. Investigation: JAS. Methodology: JAS, CL, HSR. Supervision: CL. Visualization: JAS. Writing— original draft: JAS. Writing—review & editing: CL, IPN, HK. Approval of final manuscript: all authors.
Conflicts of Interest
HK, a contributing editor of the Journal of Pathology and Translational Medicine, was not involved in the editorial evaluation or decision to publish this article. All remaining authors have declared no conflicts of interest.
Funding Statement
No funding to declare.