Search
- Page Path
- HOME > Search
- Prognostic significance of BLK expression in R-CHOP treated diffuse large B-cell lymphoma
- Soyeon Choi, Yoo Jin Lee, Yunsuk Choi, Misung Kim, Hyun-Jung Kim, Ji Eun Kim, Sukjoong Oh, Seoung Wan Chae, Hee Jeong Cha, Jae-Cheol Jo
- J Pathol Transl Med. 2022;56(5):281-288. Published online September 13, 2022
- DOI: https://doi.org/10.4132/jptm.2022.07.26
- 5,900 View
- 108 Download
- 3 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The aim of the present study was to evaluate the prognostic significance of B-cell lymphocyte kinase (BLK) expression for survival outcomes in diffuse large B-cell lymphoma (DLBCL) patients treated with R-CHOP.
Methods
We retrospectively analyzed the medical records of 89 patients from two tertiary referral hospitals. The expression of BLK, SYK, and CDK1 were evaluated in a semiquantitative method using an H-score, and the proportions of BCL2 and C-MYC were evaluated.
Results
A total of 89 patients received R-CHOP chemotherapy as a first-line chemotherapy. The expression rates of BLK in tumor cells was 39.2% (n = 34). BLK expression status was not significantly associated with clinical variables; however, BLK expression in tumor cells was significantly associated with the expression of both C-MYC and BCL2 (p = .003). With a median follow-up of 60.4 months, patients with BLK expression had significantly lower 5-year progression-free survival (PFS) and overall survival rates (49.8% and 60.9%, respectively) than patients without BLK expression (77.3% and 86.7%, respectively). In multivariate analysis for PFS, BLK positivity was an independent poor prognostic factor (hazard ratio, 2.208; p = .040).
Conclusions
Here, we describe the clinicopathological features and survival outcome according to expression of BLK in DLBCL. Approximately 39% of DLBCL patients showed BLK positivity, which was associated as a predictive marker for poor prognosis in patients who received R-CHOP chemotherapy. -
Citations
Citations to this article as recorded by- Exploring the cell-free total RNA transcriptome in diffuse large B-cell lymphoma and primary mediastinal B-cell lymphoma patients as biomarker source in blood plasma liquid biopsies
Philippe Decruyenaere, Edoardo Giuili, Kimberly Verniers, Jasper Anckaert, Katrien De Grove, Malaïka Van der Linden, Dries Deeren, Jo Van Dorpe, Fritz Offner, Jo Vandesompele
Frontiers in Oncology.2023;[Epub] CrossRef
- Exploring the cell-free total RNA transcriptome in diffuse large B-cell lymphoma and primary mediastinal B-cell lymphoma patients as biomarker source in blood plasma liquid biopsies
- Primary hepatic extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue
- Soyeon Choi, Ji Hye Kim, Kyungbin Kim, Misung Kim, Hye Jeong Choi, Young Min Kim, Jae Hee Suh, Min Jung Seo, Hee Jeong Cha
- J Pathol Transl Med. 2020;54(4):340-345. Published online April 15, 2020
- DOI: https://doi.org/10.4132/jptm.2020.03.18
- 8,458 View
- 136 Download
- 14 Web of Science
- 14 Crossref
-
 Abstract
Abstract
 PDF
PDF - Extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma), is one of the specific type of low-grade B-cell lymphoma not infrequently found worldwide. It typically involves mucosal sites such as stomach and conjunctiva; however, primary hepatic MALT lymphoma has been extremely rarely reported. We describe a case of hepatic MALT lymphoma in a 70-year-old male patient who underwent left hepatectomy due to the incidentally detected liver masses at a medical checkup. The resected specimen revealed multinodular masses consisting of small-to-intermediate-sized lymphoid cells with serpentine pattern and focal lymphoepithelial lesions. The tumor cells were diffusely positive for CD20 and Bcl-2 but negative for CD3, CD10, CD5, CD23, CD43, and cyclinD1. The Ki-67 labeling index was 10% and immunoglobulin heavy chain gene rearrangement study confirmed monoclonal proliferation. In this paper, we discuss several unique clinicopathologic characteristics which will be helpful to the differential diagnosis of hepatic MALT lymphoma.
-
Citations
Citations to this article as recorded by- Oral administration of Limosilactobacillus reuteri VHProbi® M07 alleviates ovalbumin-induced allergic asthma in mice
Guoqing Meng, Hongchang Cui, Congrui Feng, Chaoqun Guo, Lei Song, Zhi Duan, Misbahuddin Rafeeq
PLOS ONE.2025; 20(1): e0317587. CrossRef - Response‑adapted involved site radiation therapy for hepatic marginal zone B‑cell lymphoma: A case report
Shin-Ting Chen, Yu-Guang Chen, Wen-Yen Huang, Cheng-Hsiang Lo
Oncology Letters.2025;[Epub] CrossRef - Management approaches for primary hepatic lymphoma: 10 year institutional experience with comprehensive literature review
Jennifer Ma, Remy Daou, Josiane Bou Eid, Beatrice Fregonese, Joe El-Khoury, N. Ari Wijetunga, Brandon S. Imber, Joachim Yahalom, Carla Hajj
Frontiers in Oncology.2025;[Epub] CrossRef - Primary Hepatic Mucosa-Associated B-Cell Lymphoma in a Patient with Primary Sclerosing Cholangitis—A Case Ultimately Requiring Liver Transplantation
Jerica Novak, Mihajlo Đokić, Miha Petrič, Diana Vozlič, Milanka Živanović, Branislava Ranković, Blaž Trotovšek
Diagnostics.2025; 15(16): 2082. CrossRef - Primary Hepatic Mucosa-Associated Lymphoid Tissue Lymphoma: A Case Report and Literature Review
Sook Hyun Shin, Jeong-Ju Yoo, Sang Gyune Kim, Young Seok Kim, Susie Chin
Clinical Ultrasound.2025; 10(2): 119. CrossRef - Primary hepatic mucosa-associated lymphoid tissue lymphoma: a case report and literature review
Tao He, Jieyu Zou
Frontiers in Oncology.2024;[Epub] CrossRef - “Speckled Enhancement” on Gd-EOB-DTPA Enhanced MR Imaging of Primary Hepatic Mucosa-associated Lymphoid Tissue Lymphoma
Ryota Hyodo, Yasuo Takehara, Ayumi Nishida, Masaya Matsushima, Shinji Naganawa
Magnetic Resonance in Medical Sciences.2023; 22(3): 273. CrossRef - Primary hepatic extranodal marginal zone B-cell mucosa-associated lymphoid tissue lymphoma treated by laparoscopic partial hepatectomy: a case report
Keisuke Okura, Satoru Seo, Hironori Shimizu, Hiroto Nishino, Tomoaki Yoh, Ken Fukumitsu, Takamichi Ishii, Koichiro Hata, Hironori Haga, Etsuro Hatano
Surgical Case Reports.2023;[Epub] CrossRef - Incidental Findings in Pediatric Patients: How to Manage Liver Incidentaloma in Pediatric Patients
Andrius Cekuolis, Dagmar Schreiber-Dietrich, Rasa Augustinienė, Heike Taut, Judy Squires, Edda L. Chaves, Yi Dong, Christoph F. Dietrich
Cancers.2023; 15(8): 2360. CrossRef - Primary hepatic mucosa‐associated lymphoid tissue lymphoma: Case report and literature review
Wing Yu Lau, Kit‐Man Ho, Fiona Ka‐Man Chan, Shi Lam, Kai‐Chi Cheng
Surgical Practice.2022; 26(1): 56. CrossRef - 18F-FDG Versus 68Ga-FAPI PET/CT in Visualizing Primary Hepatic Extranodal Marginal Zone Lymphoma of Mucosa-Associated Lymphoid Tissue
Yizhen Pang, Long Zhao, Qihang Shang, Tinghua Meng, Haojun Chen
Clinical Nuclear Medicine.2022; 47(4): 375. CrossRef - Primary hepatopancreatobiliary lymphoma: Pathogenesis, diagnosis, and management
Qianwen Wang, Kangze Wu, Xuzhao Zhang, Yang Liu, Zhouyi Sun, Shumei Wei, Bo Zhang
Frontiers in Oncology.2022;[Epub] CrossRef - Positive effect of Bifidobacterium animalis subsp. lactis VHProbi YB11 in improving gastrointestinal movement of mice having constipation
Hongchang Cui, Qian Wang, Congrui Feng, Chaoqun Guo, Jingyan Zhang, Xinping Bu, Zhi Duan
Frontiers in Microbiology.2022;[Epub] CrossRef - A case of primary hepatic extranodal marginal zone B-cell mucosa-associated lymphoid tissue (MALT) lymphoma treated by radiofrequency ablation (RFA), and a literature review
Zhe Xu, Chong Pang, Jidong Sui, Zhenming Gao
Journal of International Medical Research.2021;[Epub] CrossRef
- Oral administration of Limosilactobacillus reuteri VHProbi® M07 alleviates ovalbumin-induced allergic asthma in mice
- Programmed death-ligand 1 expression and its correlation with clinicopathological parameters in gallbladder cancer
- Ji Hye Kim, Kyungbin Kim, Misung Kim, Young Min Kim, Jae Hee Suh, Hee Jeong Cha, Hye Jeong Choi
- J Pathol Transl Med. 2020;54(2):154-164. Published online February 10, 2020
- DOI: https://doi.org/10.4132/jptm.2019.11.13
- 10,379 View
- 176 Download
- 16 Web of Science
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Immunomodulatory therapies targeting the interaction between programmed cell death protein 1 and programmed death-ligand 1 (PD-L1) have become increasingly important in anticancer treatment. Previous research on the subject of this immune response has established an association with tumor aggressiveness and a poor prognosis in certain cancers. Currently, scant information is available on the relationship between PD-L1 expression and gallbladder cancer (GBC).
Methods
We investigated the expression of PD-L1 in 101 primary GBC cases to determine the potential association with prognostic impact. PD-L1 expression was immunohistochemically assessed using a single PD-L1 antibody (clone SP263). Correlations with clinicopathological parameters, overall survival (OS), or progression- free survival (PFS) were analyzed.
Results
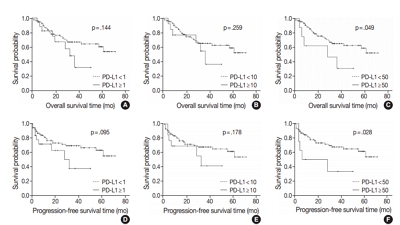
PD-L1 expression in tumor cells at cutoff levels of 1%, 10%, and 50% was present in 18.8%, 13.8%, and 7.9% of cases. Our study showed that positive PD-L1 expression at any cutoff was significantly correlated with poorly differentiated histologic grade and the presence of lymphovascular invasion (p < .05). PD-L1 expression at cutoff levels of 10% and 50% was significantly positive in patients with perineural invasion, higher T categories, and higher pathologic stages (p < .05). Additionally, there was a significant association noted between PD-L1 expression at a cutoff level of 50% and worse OS or PFS (p = .049 for OS, p = .028 for PFS). Other poor prognostic factors included histologic grade, T category, N category, pathologic stage, lymphovascular invasion, perineural invasion, growth pattern, and margin of resection (p < .05).
Conclusions
The expression of PD-L1 in GBC varies according to cutoff level but is valuably associated with poor prognostic parameters and survival. Our study indicates that the overexpression of PD-L1 in GBC had a negative prognostic impact. -
Citations
Citations to this article as recorded by- A novel machine learning-based model for precise prediction of postoperative recurrence in gallbladder cancer: development and multicenter validation across four centers
Jiajia He, Weilv Xiong, Hongxia Chen, Qunyan Pan, Weiyue Ji
World Journal of Surgical Oncology.2026;[Epub] CrossRef - PD-L1 Expression in Biliary Tract Cancer: Comparison Across Antibody Clones and Role as a Predictor of Response to Chemoimmunotherapy: A Meta-Analysis
Juan J. Juarez-Vignon Whaley, Soravis Osataphan, Ben Ponvilawan, Nipith Charoenngam, Mary Linton Peters
JCO Precision Oncology.2025;[Epub] CrossRef - An MRI-based model for preoperative prediction of tertiary lymphoid structures in patients with gallbladder cancer
Ying Xu, Zhuo Li, Weihua Zhi, Yi Yang, Jingzhong Ouyang, Yanzhao Zhou, Zeliang Ma, Sicong Wang, Lizhi Xie, Jianming Ying, Jinxue Zhou, Xinming Zhao, Feng Ye
Insights into Imaging.2025;[Epub] CrossRef - Lacking Immunotherapy Biomarkers for Biliary Tract Cancer: A Comprehensive Systematic Literature Review and Meta-Analysis
Giorgio Frega, Fernando P. Cossio, Jesus M. Banales, Vincenzo Cardinale, Rocio I. R. Macias, Chiara Braconi, Angela Lamarca
Cells.2023; 12(16): 2098. CrossRef - Gallbladder carcinomas: review and updates on morphology, immunohistochemistry, and staging
Whayoung Lee, Vishal S. Chandan
Human Pathology.2023; 132: 149. CrossRef - Prognostic Relevance of PDL1 and CA19-9 Expression in Gallbladder Cancer vs. Inflammatory Lesions
Neetu Rawal, Supriya Awasthi, Nihar Ranjan Dash, Sunil Kumar, Prasenjit Das, Amar Ranjan, Anita Chopra, Maroof Ahmad Khan, Sundeep Saluja, Showket Hussain, Pranay Tanwar
Current Oncology.2023; 30(2): 1571. CrossRef - Identification of genes associated with gall bladder cell carcinogenesis: Implications in targeted therapy of gall bladder cancer
Ishita Ghosh, Ruma Dey Ghosh, Soma Mukhopadhyay
World Journal of Gastrointestinal Oncology.2023; 15(12): 2053. CrossRef - CD73 and PD-L1 as Potential Therapeutic Targets in Gallbladder Cancer
Lu Cao, Kim R. Bridle, Ritu Shrestha, Prashanth Prithviraj, Darrell H. G. Crawford, Aparna Jayachandran
International Journal of Molecular Sciences.2022; 23(3): 1565. CrossRef - Evolving Role of Immunotherapy in Advanced Biliary Tract Cancers
Sandra Kang, Bassel F. El-Rayes, Mehmet Akce
Cancers.2022; 14(7): 1748. CrossRef - Novel immune scoring dynamic nomograms based on B7-H3, B7-H4, and HHLA2: Potential prediction in survival and immunotherapeutic efficacy for gallbladder cancer
Chao Lv, Shukun Han, Baokang Wu, Zhiyun Liang, Yang Li, Yizhou Zhang, Qi Lang, Chongli Zhong, Lei Fu, Yang Yu, Feng Xu, Yu Tian
Frontiers in Immunology.2022;[Epub] CrossRef - PD-1 inhibitors plus nab-paclitaxel-containing chemotherapy for advanced gallbladder cancer in a second-line setting: A retrospective analysis of a case series
Sirui Tan, Jing Yu, Qiyue Huang, Nan Zhou, Hongfeng Gou
Frontiers in Oncology.2022;[Epub] CrossRef - Expression of HER2 and Mismatch Repair Proteins in Surgically Resected Gallbladder Adenocarcinoma
You-Na Sung, Sung Joo Kim, Sun-Young Jun, Changhoon Yoo, Kyu-Pyo Kim, Jae Hoon Lee, Dae Wook Hwang, Shin Hwang, Sang Soo Lee, Seung-Mo Hong
Frontiers in Oncology.2021;[Epub] CrossRef - Programmed Death Ligand-1 (PD-L1) Is an Independent Negative Prognosticator in Western-World Gallbladder Cancer
Thomas Albrecht, Fritz Brinkmann, Michael Albrecht, Anke S. Lonsdorf, Arianeb Mehrabi, Katrin Hoffmann, Yakup Kulu, Alphonse Charbel, Monika N. Vogel, Christian Rupp, Bruno Köhler, Christoph Springfeld, Peter Schirmacher, Stephanie Roessler, Benjamin Goep
Cancers.2021; 13(7): 1682. CrossRef - Immune Microenvironment in Gallbladder Adenocarcinomas
Pallavi A. Patil, Kara Lombardo, Weibiao Cao
Applied Immunohistochemistry & Molecular Morphology.2021; 29(8): 557. CrossRef - Molecular Targets and Emerging Therapies for Advanced Gallbladder Cancer
Matteo Canale, Manlio Monti, Ilario Giovanni Rapposelli, Paola Ulivi, Francesco Giulio Sullo, Giulia Bartolini, Elisa Tiberi, Giovanni Luca Frassineti
Cancers.2021; 13(22): 5671. CrossRef - Overview of current targeted therapy in gallbladder cancer
Xiaoling Song, Yunping Hu, Yongsheng Li, Rong Shao, Fatao Liu, Yingbin Liu
Signal Transduction and Targeted Therapy.2020;[Epub] CrossRef
- A novel machine learning-based model for precise prediction of postoperative recurrence in gallbladder cancer: development and multicenter validation across four centers
- Prognostic Significance of Absolute Lymphocyte Count/Absolute Monocyte Count Ratio at Diagnosis in Patients with Multiple Myeloma
- Su-Jin Shin, Jin Roh, Misung Kim, Min Jung Jung, Young Wha Koh, Chan-Sik Park, Dok Hyun Yoon, Cheolwon Suh, Chan-Jeong Park, Hyun Sook Chi, Jooryung Huh
- Korean J Pathol. 2013;47(6):526-533. Published online December 24, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.6.526
- 14,296 View
- 89 Download
- 28 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Absolute lymphocyte count (ALC) in peripheral blood has recently been reported to be an independent prognostic factor in multiple myeloma (MM). Previous studies indicated that the absolute monocyte count (AMC) in peripheral blood reflects the state of the tumor microenvironment in lymphomas. Neither the utility of the AMC nor its relationship with ALC has been studied in MM.
Methods The prognostic value of ALC, AMC, and the ALC/AMC ratio at the time of diagnosis was retrospectively examined in 189 patients with MM.
Results On univariate analysis, low ALC (<1,400 cells/µL), high AMC (≥490 cells/µL), and low ALC/AMC ratio (<2.9) were correlated with worse overall survival (OS) (p=.002, p=.038, and p=.001, respectively). On multivariate analysis, the ALC/AMC ratio was an independent prognostic factor (p=.047), whereas ALC and AMC were no longer statistical significant. Low ALC, high AMC, and low ALC/AMC ratio were associated with poor prognostic factors such as high International Staging System stage, plasmablastic morphology, hypoalbuminemia, and high β2-microglobulin.
Conclusions Univariate analysis demonstrated that changes in ALC, AMC, and the ALC/AMC ratio are associated with patient survival in MM. Multivariate analysis showed that, of these factors, the ALC/AMC ratio was an independent prognostic factor for OS.
-
Citations
Citations to this article as recorded by- Association between systemic immune-inflammatory markers and monoclonal gammopathy of undetermined significance in the elderly population: findings from the National health and nutrition examination survey
Chengpeng Zhang, Kangyan Hou, Dongjun Lin, Cong Xu
Clinical and Experimental Medicine.2026;[Epub] CrossRef - Low peripheral blood B lymphocyte count predicts poor outcome in patients with multiple myeloma
Yuqi Wang, Zhongxin Zheng, Qiaoxi Kang, Linjing Cai, Shanshan Zhang, Huan Chen, Youhai Yuan, Hanzhen Zhang, Xiaolei Wei, Ru Feng, Yongqiang Wei
Immunobiology.2025; 230(4): 153096. CrossRef - Inflammatory markers from routine blood tests predict survival in multiple myeloma: a Systematic Review and meta-analysis
Mengjiao Luo, Ling Qin, Yujie Li, Qianru Mei, Qiaoping Wu, Xudong Feng
Frontiers in Immunology.2025;[Epub] CrossRef - Variation of peripheral blood-based biomarkers for response of anti-PD-1 immunotherapy in non-small-cell lung cancer
Xiaoming Wang, Dayu Chen, Yuyan Ma, Dongping Mo, Feng Yan
Clinical and Translational Oncology.2024; 26(8): 1934. CrossRef - Descriptive analysis and prognostic factors in cats with myeloma-related disorders: A multicenter retrospective study of 50 cases
Lorris Lecot, Isabelle Desmas-Bazelle, Sarah Benjamin, Pauline De Fornel, Frédérique Ponce, Matthew Kornya, Loïc Desquilbet, Claire Beaudu-Lange, Catherine Ibisch, David Sayag, Ghita Benchekroun, Jérémy Béguin
Journal of Veterinary Internal Medicine.2024; 38(3): 1693. CrossRef - Clinical features and treatment of newly diagnosed multiple myeloma with secondary myelofibrosis: a retrospective study
Han Xu, Yujie Xu, Mengying Wang, Chunxia Mao, Junxia Huang, Tianlan Li, Yan Gao, Shanshan Liu, Jingjing Zhou, Yi Zhang, Xianqi Feng
Therapeutic Advances in Hematology.2024;[Epub] CrossRef - Definers and drivers of functional high-risk multiple myeloma: insights from genomic, transcriptomic, and immune profiling
Rahul Banerjee, Kara I. Cicero, Sarah S. Lee, Andrew J. Cowan
Frontiers in Oncology.2023;[Epub] CrossRef - Normal Absolute Monocyte Count in Combination with Normal/High Absolute Lymphocyte Count at the Time of Relapse is Associated with Improved Survival in Patients with Early Relapsed Acute Myeloid Leukemia
Yu Zhang, Kanchun Dai, Qianying Zhang, Yisha Huang, Yiyun Feng, Deeksha Bhardwaj, Kang Yu, Jianhua Feng
Cancer Investigation.2021; 39(6-7): 550. CrossRef - Real World Experience of Daratumumab: Evaluating Lymphopenia and Adverse Events in Multiple Myeloma Patients
Francesca Cottini, Ying Huang, Nita Williams, Naresh Bumma, Abdullah M. Khan, Maria Chaudhry, Srinivas Devarakonda, Yvonne A. Efebera, Don M. Benson, Ashley E. Rosko
Frontiers in Oncology.2021;[Epub] CrossRef - Are the Derived Indexes of Peripheral Whole Blood Cell Counts (NLR, PLR, LMR/MLR) Clinically Significant Prognostic Biomarkers in Multiple Myeloma? A Systematic Review And Meta-Analysis
Xinwen Zhang, Jialin Duan, Zhenyu Wen, Hao Xiong, Xiaomin Chen, Yang Liu, Kunyu Liao, Chunlan Huang
Frontiers in Oncology.2021;[Epub] CrossRef - Combined immune score of lymphocyte to monocyte ratio and immunoglobulin levels predicts treatment-free survival of multiple myeloma patients after autologous stem cell transplant
Karen Sweiss, Jonathan Lee, Nadim Mahmud, Gregory S. Calip, Youngmin Park, Dolores Mahmud, Damiano Rondelli, Pritesh R. Patel
Bone Marrow Transplantation.2020; 55(1): 199. CrossRef - Low absolute CD4+ T cell counts in peripheral blood predict poor prognosis in patients with newly diagnosed multiple myeloma
Yan Gu, Yuanyuan Jin, Jie Ding, Wu Yujie, Qinglin Shi, Xiaoyan Qu, Sishu Zhao, Jianyong Li, Chen Lijuan
Leukemia & Lymphoma.2020; 61(8): 1869. CrossRef Normal Absolute Monocyte Count at the Time of Relapse is Associated with Improved Survival After First Salvage Therapy in Adult Patients with Early Relapsed B-Lineage Acute Lymphoblastic Leukemia
Yi-fen Shi, Na Wang, Zi-yang Huang, Rong-rong Chen, Yi-sha Huang, Yi-yi Zhu, Chong-yun Xing, Bin Liang, Kang Yu, Jian-hua Feng
Cancer Management and Research.2020; Volume 12: 7097. CrossRef- Peripheral blood biomarkers of early immune reconstitution in newly diagnosed multiple myeloma
Moritz Binder, S. Vincent Rajkumar, Martha Q. Lacy, Morie A. Gertz, Francis K. Buadi, Angela Dispenzieri, Yi L. Hwa, Amie Fonder, Miriam Hobbs, Suzanne R. Hayman, Steven R. Zeldenrust, John A. Lust, Stephen J. Russell, Nelson Leung, Prashant Kapoor, Ronal
American Journal of Hematology.2019; 94(3): 306. CrossRef - Effect of absolute monocyte count post-transplant on the outcome of patients with acute myeloid leukemia undergoing myeloablative allogeneic hematopoietic stem cell transplant with busulfan and cyclophosphamide conditioning
Liyuan Tang, Na Wang, Chongyun Xing, Qiang Zhuang, Bin Liang, Lan Sun, Yi Chen, Yan Qian, Zhijian Shen, Songfu Jiang, Kang Yu, Jianhua Feng
Leukemia Research.2018; 69: 60. CrossRef - A lower ALC/AMC ratio is associated with poor prognosis of peripheral T-cell lymphoma-not otherwise specified
Qian Li, Shuang Gao, Jing Ma, Su Liu, Yuanfang Yue, Lin Chen, Han Li, Xue Wang, Dongying Li, Zeng Cao, Zhigang Zhao, Xiaofang Wang, Yong Yu, Yizhuo Zhang, Yafei Wang
Leukemia Research.2018; 73: 5. CrossRef - Peripheral Blood Lymphocyte-to-Monocyte Ratio as a Useful Prognostic Factor in Newly Diagnosed Multiple Myeloma
Ying Tian, Yue Zhang, Wan-Qiu Zhu, Xiao-Lei Chen, He-Bing Zhou, Wen-Ming Chen
BioMed Research International.2018; 2018: 1. CrossRef - Significance of the absolute lymphocyte/monocyte ratio as a prognostic immune biomarker in newly diagnosed multiple myeloma
T Dosani, F Covut, R Beck, J J Driscoll, M de Lima, E Malek
Blood Cancer Journal.2017; 7(6): e579. CrossRef - Lymphocyte-to-monocyte ratio can predict mortality in pancreatic adenocarcinoma
Gurshawn Singh, Ammar Nassri, David Kim, Hong Zhu, Zeeshan Ramzan
World Journal of Gastrointestinal Pharmacology and Therapeutics.2017; 8(1): 60. CrossRef - Bone marrow microenvironmental CD4 + and CD8 + lymphocyte infiltration patterns define overall- and progression free survival in standard risk multiple myeloma – an analysis from the Austrian Myeloma Registry
Wolfgang Willenbacher, Ella Willenbacher, Claudia Zelle-Rieser, Rainer Biedermann, Roman Weger, Karin Jöhrer, Andrea Brunner
Leukemia & Lymphoma.2016; 57(6): 1478. CrossRef - Absolute lymphocyte count as a prognostic marker in newly diagnosed multiple myeloma patients
C. Suriu, L. Akria, D. Azoulay, E. Shaoul, M. Barhoum, A. Braester
International Journal of Laboratory Hematology.2016;[Epub] CrossRef - The Peripheral Blood Mononuclear Cell Count Is Associated With Bone Health in Elderly Men
Xianfeng Lin, Hejun Yu, Chenchen Zhao, Yu Qian, Dun Hong, Kangmao Huang, Jian Mo, An Qin, Xiangqian Fang, Shunwu Fan
Medicine.2016; 95(15): e3357. CrossRef - Prognostic role of lymphocyte to monocyte ratio for patients with cancer: evidence from a systematic review and meta-analysis
Liangyou Gu, Hongzhao Li, Luyao Chen, Xin Ma, Xintao Li, Yu Gao, Yu Zhang, Yongpeng Xie, Xu Zhang
Oncotarget.2016; 7(22): 31926. CrossRef - Do lymphocytes count in myeloma? Are we absolutely sure?
Tamar Tadmor
Leukemia & Lymphoma.2015; 56(5): 1193. CrossRef - Absolute lymphocyte count is unrelated to overall survival in newly diagnosed elderly patients with multiple myeloma treated with immunomodulatory drugs
Mariasanta Napolitano, Giorgia Saccullo, Roberto Bono, Antonio Branca, Clotilde Cangialosi, Salvatrice Mancuso, Simona Raso, Gerlando Quintini, Maria Grazia Lipari, Francesco Fabbiano, Giorgina Specchia, Alberto Dolce, Francesco Di Raimondo, Sergio Siragu
Leukemia & Lymphoma.2015; 56(5): 1507. CrossRef - Distinct Transcriptional and Anti-Mycobacterial Profiles of Peripheral Blood Monocytes Dependent on the Ratio of Monocytes: Lymphocytes
Vivek Naranbhai, Helen A. Fletcher, Rachel Tanner, Matthew K. O'Shea, Helen McShane, Benjamin P. Fairfax, Julian C. Knight, Adrian V.S. Hill
EBioMedicine.2015; 2(11): 1619. CrossRef - Prognostic value of absolute monocyte count in chronic lymphocytic leukaemia
László Szerafin, János Jakó, Ferenc Riskó
Orvosi Hetilap.2015; 156(15): 592. CrossRef - The lymphocyte to monocyte ratio in peripheral blood represents a novel prognostic marker in patients with pancreatic cancer
Michael Stotz, Joanna Szkandera, Tatjana Stojakovic, Julia Seidel, Hellmut Samonigg, Peter Kornprat, Renate Schaberl-Moser, Fridericke Seggewies, Gerald Hoefler, Armin Gerger, Martin Pichler
Clinical Chemistry and Laboratory Medicine (CCLM).2015;[Epub] CrossRef
- Association between systemic immune-inflammatory markers and monoclonal gammopathy of undetermined significance in the elderly population: findings from the National health and nutrition examination survey

 E-submission
E-submission



 First
First Prev
Prev



