Search
- Page Path
- HOME > Search
Original Articles
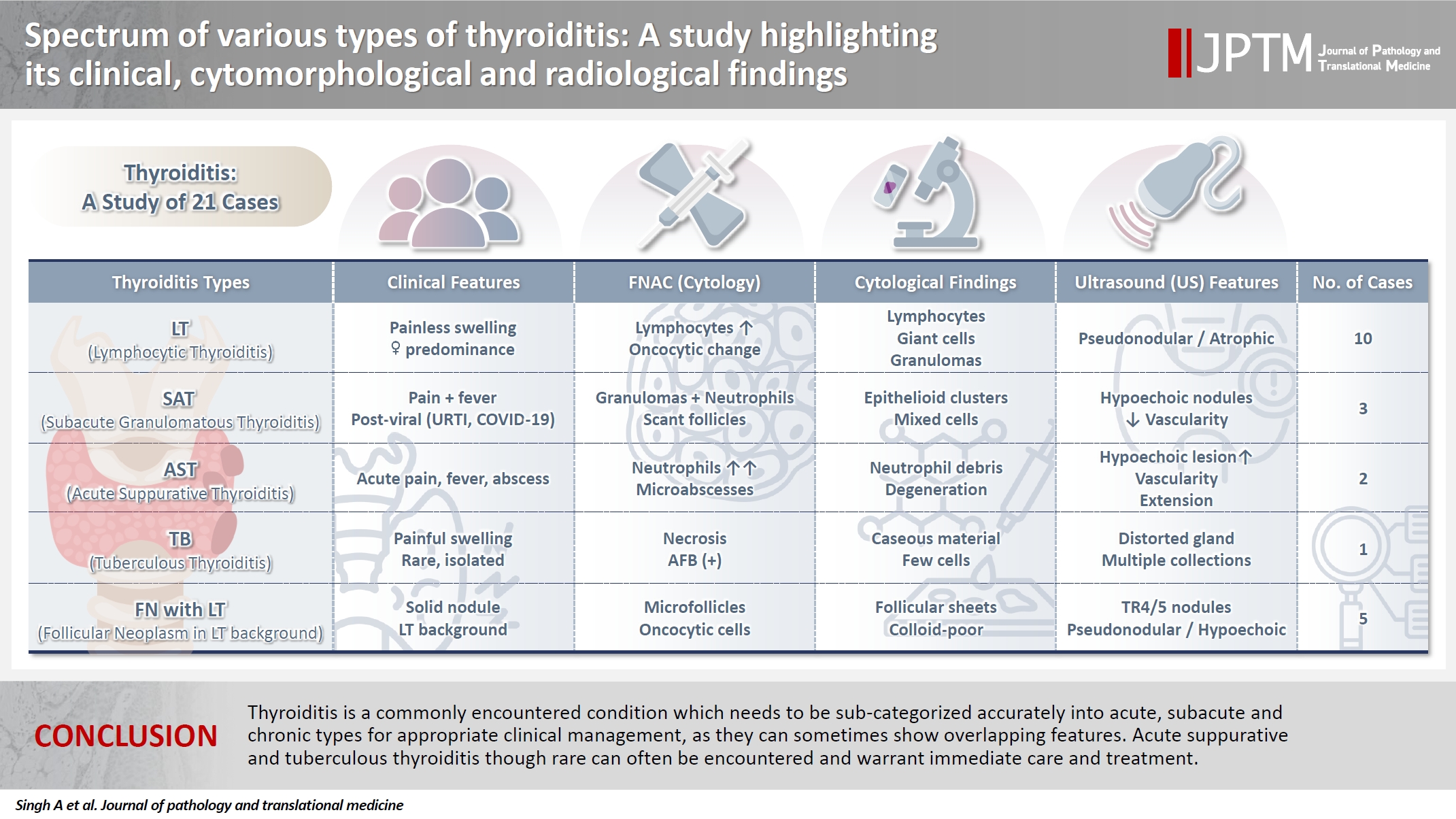
- Spectrum of thyroiditis types: clinical, cytomorphological, and radiological findings
- Anam Singh, Indrajeet Kundu
- J Pathol Transl Med. 2025;59(6):421-433. Published online November 6, 2025
- DOI: https://doi.org/10.4132/jptm.2025.08.13
- 4,653 View
- 205 Download
-
 Abstract
Abstract
 PDF
PDF - Background
Thyroiditis encompasses a range of inflammatory conditions affecting the thyroid gland. Lymphocytic thyroiditis (LT) is a common form of thyroiditis, with acute suppuration of the thyroid, while tuberculous thyroiditis is relatively rare. Fine-needle aspiration cytology (FNAC) remains a safe and cost-effective tool for diagnosing thyroid-related diseases, especially when paired with ultrasound (US) and clinical examination. Methods: This is a cross-sectional study including 21 cases. The cases were reported as thyroiditis on US and FNAC, and the findings were correlated with patient clinical history, symptoms during presentation, and serological profiles. Results: The cases of thyroiditis encompassed the more common forms, LT and subacute granulomatous thyroiditis (SAT), as well as relatively rare forms like tuberculous thyroiditis and thyroid abscess. Cases of follicular neoplasms (FN) arising in the context of LT also are included in this study. The case of tuberculous thyroiditis presented as a bulky thyroid gland that appeared heterogeneous on US with extensive necrosis on FNAC. The cases of thyroid abscess and SAT presented with painful neck swellings, with granulomas in the latter cases. US features of LT showed an array of appearances ranging from pseudonodular to an atrophic thyroid gland. All cases of FN showed a lymphocytic background. Conclusions: Thyroiditis is a commonly encountered condition that needs to be sub-categorized accurately into acute, subacute, and chronic types for appropriate clinical management, as they can sometimes show overlapping features. Though rare, acute suppurative and tuberculous thyroiditis are often encountered and warrant immediate care and treatment.
- Do Helper T Cell Subtypes in Lymphocytic Thyroiditis Play a Role in the Antitumor Effect?
- Seok Woo Yang, Seong-Ho Kang, Kyung Rae Kim, In Hong Choi, Hang Seok Chang, Young Lyun Oh, Soon Won Hong
- J Pathol Transl Med. 2016;50(5):377-384. Published online September 15, 2016
- DOI: https://doi.org/10.4132/jptm.2016.07.25
- 10,714 View
- 108 Download
- 3 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Papillary thyroid carcinoma (PTC) is frequently accompanied by lymphocytic thyroiditis (LT). Some reports claim that Hashimoto’s thyroiditis (the clinical form of LT) enhances the likelihood of PTC; however, others suggest that LT has antitumor activity. This study was aimed to find out the relationship between the patterns of helper T cell (Th) cytokines in thyroid tissue of PTC with or without LT and the clinicopathological manifestation of PTC.
Methods
Fresh surgical samples of PTC with (13 cases) or without (10 cases) LT were used. The prognostic parameters (tumor size, extra-thyroidal extension of PTC, and lymph node metastasis) were analyzed. The mRNA levels of two subtypes of Th cytokines, Th1 (tumor necrosis factor α [TNF-α], interferon γ [IFN-γ ], and interleukin [IL] 2) and Th2 (IL-4 and IL-10), were analyzed. Because most PTC cases were microcarcinomas and recent cases without clinical follow-up, negative or faint p27 immunoreactivity was used as a surrogate marker for lymph node metastasis.
Results
PTC with LT cases showed significantly higher expression of TNF-α (p = .043), IFN-γ (p < .010), IL-4 (p = .015) than those without LT cases. Although the data were not statistically significant, all analyzed cytokines (except for IL-4) were highly expressed in the cases with higher expression of p27 surrogate marker.
Conclusions
These results indicate that mixed Th1 (TNF-α, IFN-γ , and IL-2) and Th2 (IL-10) immunity might play a role in the antitumor effect in terms of lymph node metastasis. -
Citations
Citations to this article as recorded by- Papillary thyroid carcinoma with Hashimoto’s thyroiditis: impact and correlation
Shengpeng Yao, Hong Zhang
Frontiers in Endocrinology.2025;[Epub] CrossRef - Obesity and Thyroid Cancer Risk: An Update
Fabiana Franchini, Giuseppe Palatucci, Annamaria Colao, Paola Ungaro, Paolo Emidio Macchia, Immacolata Cristina Nettore
International Journal of Environmental Research and Public Health.2022; 19(3): 1116. CrossRef - Association between Hashimoto thyroiditis and clinical outcomes of papillary thyroid carcinoma: A meta-analysis
Qizhi Tang, Weiyu Pan, Liangyue Peng, Francis Moore
PLOS ONE.2022; 17(6): e0269995. CrossRef - The Heat Shock Protein Story—From Taking mTORC1,2 and Heat Shock Protein Inhibitors as Therapeutic Measures for Treating Cancers to Development of Cancer Vaccines
Peter Chin Wan Fung, Regina Kit Chee Kong
Journal of Cancer Therapy.2017; 08(11): 962. CrossRef
- Papillary thyroid carcinoma with Hashimoto’s thyroiditis: impact and correlation
Case Report
- A Branchial Cleft Cyst-Like Lymphoepithelial Cyst in the Thyroid Gland: A case report.
- Gil Hyun Kang, Jee Soo Kim, Haing Sub R Chung
- Korean J Pathol. 1999;33(7):533-536.
- 2,815 View
- 59 Download
-
 Abstract
Abstract
 PDF
PDF - The lymphoepithelial cyst (LEC) rarely occurs in the thyroid gland. The LEC has been thought to be related to developmental rest, namely solid cell nest, which is derived from ultimobranchial body. We report a case of lymphoepithial cyst in a 34- year-old woman clinically diagnosed with Hashimoto's thyroiditis. The cyst was located in mid to lower portion of the left lobe. It was a single unilocular cyst, which for the most part was lined with squamous epithelium, and at certain foci with ciliated columnar epithelium. The cyst wall showed a dense lymphocytic infiltration, numerous lymphoid follicles with germinal centers and admixed thyroid follicles. This morphology is similar to the branchial cleft cyst, with the exception of the thyroid follicles in the cyst wall. Near the cyst were several solid epidermoid cell nests. Immunohistochemical stain of this cyst-lining epithelium and solid cell nests showed CEA positivity. In view of the similarity in histomorphology and CEA positivity to branchial cleft cyst of the lateral neck, the LEC of the thyroid could also have been of branchial origin. However, the admixed thyroid follicles in the cyst wall suggests that the LEC of the thyroid gland might have derived from another branchial cleft as a ultimobranchial body, because it has the potential for thyroid follicular differentiation.
Original Article
- Ovarian mature cystic teratoma with histologic features of chronic thyroiditis: Histologic analysis of 4 cases.
- Doo Hyun Chung, Weon Seo Park, Soo Min Kang, Eun Sil Yu, Seong Hoe Park
- Korean J Pathol. 1992;26(3):209-214.
- 2,338 View
- 15 Download
-
 Abstract
Abstract
 PDF
PDF - We have reviewed ovarian mature cystic teratomas with features of chronic thyroiditis that were diagnosed at the department of pathology, Seoul National University Hospital during 7 years, 1984-1991. Twenty three case(8%) containing thyroid tissue among 285 ovarian mature teratomas were available for histopathologic examination. Among these, 4 cases(1.4%) showed lymphocytic infiltration with lymphoid follicle formation. These four cases were examined according to the strict histologic criteria of autoimmune thyroiditis and reactive non-autoimmune thyroiditis for the purpose of differentiation of pathogenesis. Two cases were similar to autoimmune in nature and the other two cases simply seemed to reflect reactive features to adjacent stimulating elements. In conclusion, thyroid tissue present in ovarian cystic teratoma may have histologic features of chronic thyroiditis of either autoimmune or non-autoimmune origin.

 E-submission
E-submission

 First
First Prev
Prev



