Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 47(1); 2013 > Article
-
Brief Case Report
Fine Needle Aspiration Cytology of Postoperative Spindle Cell Nodule in Neck after Thyroidectomy: A Case Report - Myunghee Kang, Seung Yeon Ha1, Hyun Yee Cho1, Jungsuk An1, Dong Hae Chung1, Yoo Seung Chung2
-
Korean Journal of Pathology 2013;47(1):89-91.
DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.1.89
Published online: February 25, 2013
Department of Pathology, Gachon University School of Medicine, Gachon University Gil Medical Center, Incheon, Korea.
1Department of Pathology, Gachon University Gil Medical Center, Incheon, Korea.
2Department of Surgery, Gachon University Gil Medical Center, Incheon, Korea.
- Corresponding Author: Seung Yeon Ha, M.D. Department of Pathology, Gachon University Gil Medical Center, 21 Namdong-daero 774beon-gil, Namdong-gu, Incheon 405-760, Korea. Tel: +82-32-460-3073, Fax: +82-32-460-2394, syha@gilhospital.com
• Received: August 14, 2012 • Revised: October 31, 2012 • Accepted: November 15, 2012
© 2013 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- A 53-year-old female patient visited the hospital for evaluation of an asymptomatic right lateral neck mass. She had undergone a right thyroid lobectomy for treatment of a papillary microcarcinoma 22 months prior. The tumor measured 0.7×0.6 cm in size with a clear resection margin. After the operation, she was followed regularly, and there were no events.
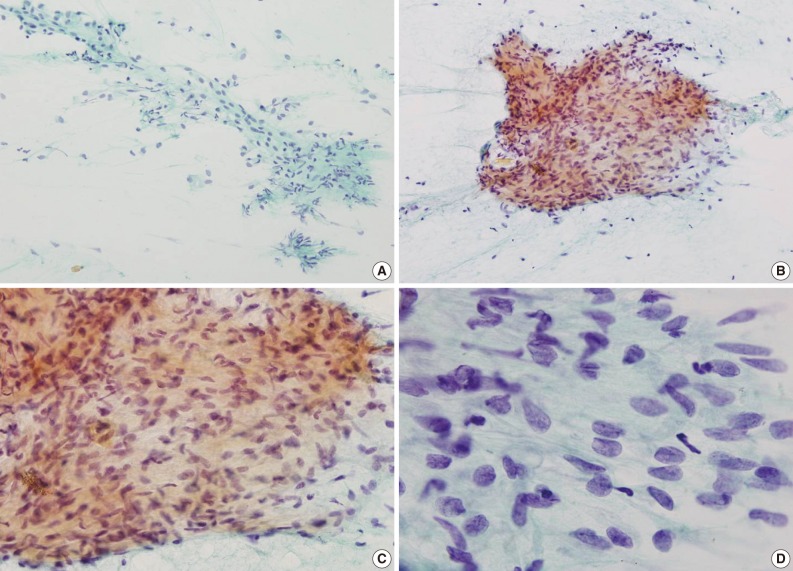
- A hypoechoic mass with multiple calcifications was observed on thyroid ultrasonography, and ultrasonography guided-FNA was performed. The smear of the FNA cytology showed fragments of fibrocollagenous connective tissue and scattered spindle cells (Fig. 1A). Some histiocyte-like cells were aggregated forming vague granulomas (Fig. 1B, C). Loosely scattered young fibroblast-like cells with plump nuclei were observed (Fig. 1D). The cytologic diagnoses were suggestive of nodular fasciitis or a granulomatous reaction to a foreign body.
- The patient had undergone a complete thyroidectomy and neck mass excision. Severe adhesions were observed in the postoperative thyroid bed, and the residual thyroid left lobe was normal in appearance on gross examination.
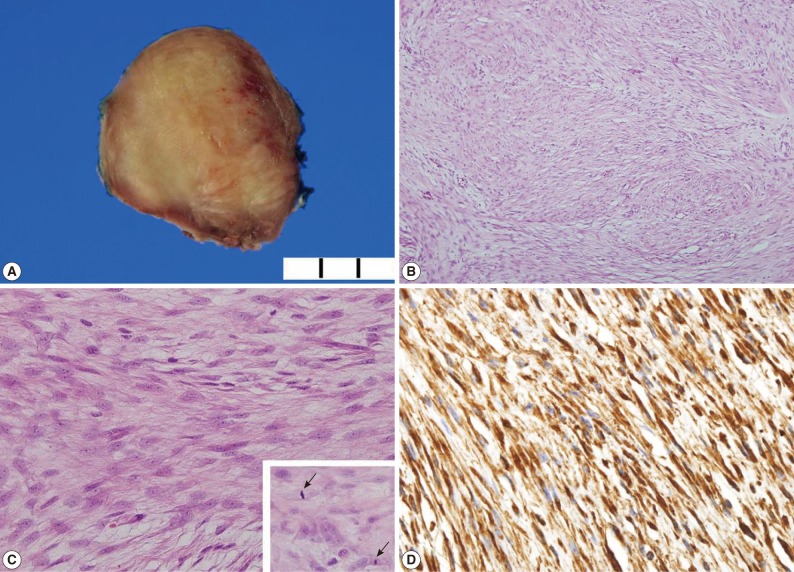
- Grossly, the neck mass measured 4.3×3.5×2.6 cm, with a round, firm, and whitish surface. The cut surface was a homogenous yellow-tan color and was focally hemorrhagic (Fig. 2A). There were no pathologic findings in the thyroid left lobe.
- Microscopically, the mass was found to be composed of bland-looking spindle cells (Fig. 2B), with an indistinct cell border, eosinophilic cytoplasm, and oval nuclei. The nucleoli were inconspicuous (Fig. 2C). Mitotic counts were 6 per 10 high power field without atypism (Fig. 2C, inset). Adhesions on adjacent structures were observed, but did not show an infiltrative pattern.
- The spindle cells were fully reactive in vimentin (prediluted, V9, Dako, Glostrup, Denmark) and focally positive for α-smooth muscle actin (prediluted, 1A4, Dako); however, they were negative for anaplastic lymphoma kinase (ALK; 1 : 50, ALK1, Dako), Cam 5.2 (prediluted, Becton Dickinson, CA, USA), desmin (prediluted, D3, Dako), epithelial membrane antigen (prediluted, E29, Dako), and pancytokeratin (prediluted, AE1/AE3, Dako) (Fig. 2D). Ki-67 labeling index was less than 5%.
CASE REPORT
- Postoperative spindle cell nodules in the thyroidectomy bed are extremely rare.4 According to the literature, the reported sites of postoperative spindle cell nodule included the genitourinary tract, oral cavity, breast, and skin.1-3 Except for cases arising in the skin, all other cases have arisen in previous biopsy or operation sites,1-4 and the cases arising in the skin all had a history of trauma. In 1984, Proppe et al.1 reported eight cases of spindle cell nodules with benign features arising in the lower genitourinary tract. These lesions showed elongated spindle cells that are reactive in vimentin. The stains for muscle specific actin, smooth muscle actin, desmin, and cytokeratin were inconclusive with only some showing positivity.
- There has been controversy with regard to whether lesions containing spindle cell nodules are reactive or neoplastic.2,3,5 ALK gene rearrangement and immunohistochemical positivity for ALK were found in approximately 50% of cases, suggesting that postoperative spindle cell nodules are neoplastic. However, the history of trauma or surgical treatment and the microscopic findings of high vascularity and inflammation support that the nodules are a reactive process.2 There is one report of describing trisomy 7 in postoperative spindle cell nodules.5 However, trisomy 7 is a controversial aberration, which has been found in non-neoplastic tissue as well as in a variety of neoplasms.5
- Due to its high diagnostic accuracy and minimal invasiveness, FNA aspiration is widely used for evaluation of neck masses. The possible spindle cell lesions in neck include schwannoma, nodular fasciitis, fibrous tumor, and sarcoma.6 Schwannomas, which are the most common spindle cell lesion in the neck, consist of spindle cells with moderate cytoplasm and slender, wavy, pointed-end nuclei. These cells are different from postoperative spindle cell nodules. The aspiration specimens of nodular fasciitis are characteristically cellular and single scattered fibroblast-like cells with occasional multinucleated giant cells. Collagen fragments and myxoid substances can often be observed. Neutrophils, eosinophils, lymphocytes, and plasma cells are present in various proportions. However, postoperative spindle cell nodules do not show myxoid substances and inflammatory cells. Sarcomas may show cellular pleomorphism in necrotic backgrounds.6 Metastatic or recurrent cancers should be also investigated in patients with a history of malignancy. Although there is one report of a postoperative spindle cell nodule in the thyroid bed after surgery,4 no articles describing cytologic findings were found. These cytologic findings are different from those for other spindle cell lesions, and are useful for differential diagnosis.
- In conclusion, awareness of postoperative spindle cell nodules as part of the patient history is helpful in making a diagnosis of spindle cell lesions by FNA.
DISCUSSION
Acknowledgments
Acknowledgments
- 1. Proppe KH, Scully RE, Rosai J. Postoperative spindle cell nodules of genitourinary tract resembling sarcomas: a report of eight cases. Am J Surg Pathol 1984; 8: 101-108. ArticlePubMed
- 2. Lott S, Lopez-Beltran A, Maclennan GT, Montironi R, Cheng L. Soft tissue tumors of the urinary bladder, part I: myofibroblastic proliferations, benign neoplasms, and tumors of uncertain malignant potential. Hum Pathol 2007; 38: 807-823. ArticlePubMed
- 3. Hirsch MS, Dal Cin P, Fletcher CD. ALK expression in pseudosarcomatous myofibroblastic proliferations of the genitourinary tract. Histopathology 2006; 48: 569-578. ArticlePubMed
- 4. Kim SW, Oh YL, Choi JY, Lee JI, Chung JH, Kim JS. Postoperative spindle cell nodule after thyroidectomy: a case mimicking recurrence with anaplastic transformation of thyroid cancer. Head Neck 2013; 35: E13-E17. ArticlePubMed
- 5. Micci F, Haugom L, Abeler VM, Bjerkehagen B, Heim S. Trisomy 7 in postoperative spindle cell nodules. Cancer Genet Cytogenet 2007; 174: 147-150. ArticlePubMed
- 6. An J, Oh YL, Shin JH, Jeong HS. Primary schwannoma of the thyroid gland: a case report. Acta Cytol 2010; 54(5 Suppl): 857-862. PubMed
REFERENCES
Fig. 1Cytologic findings. (A) Fragments of fibrocollagenous tissue and scattered spindle cells and (B, C) vague granulomas are observed. (D) On high power view, spindle cells with plump nuclei and indistinctive nucleoli are observed.
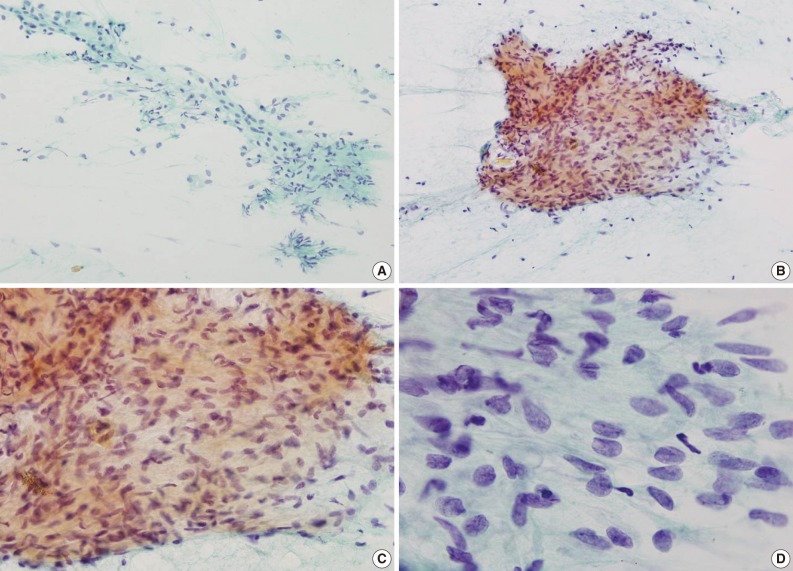

Fig. 2Gross and microscopic findings. (A) The cut surface of the mass is a homogenous yellow-tan color. (B) The tumor consists of a spindle cell proliferation. (C) The high power view shows homogenous bland-looking spindle cells with plump nuclei and indistinctive nucleoli (inset). Mitoses are occasionally observed (arrows). (D) Spindle cells are reactive in vimentin.
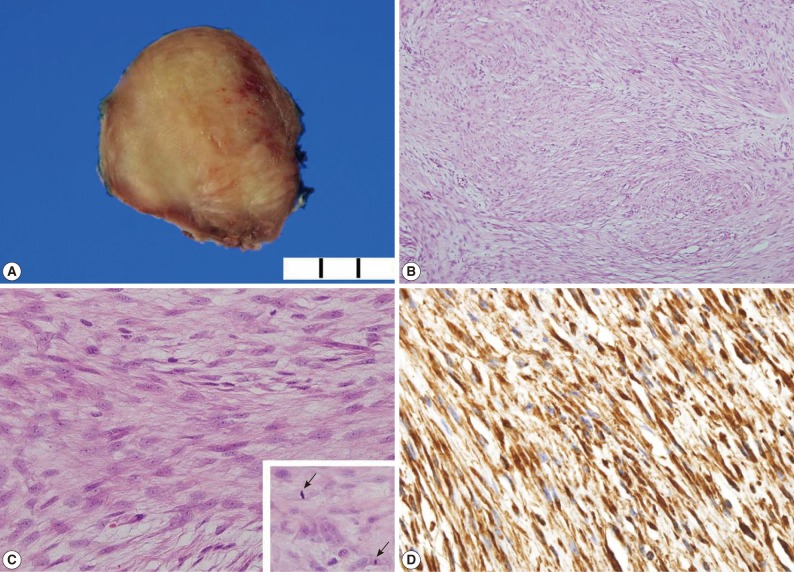

Figure & Data
References
Citations
Citations to this article as recorded by 

- Post-surgical thyroid bed myofibroma simulating a recurrent papillary thyroid carcinoma: A case report and review of the literature
Jun Hyeon Park, Kyung Sik Yi, Chi-Hoon Choi, Yook Kim, Jisun Lee, Yeongtae Park, Ok-Jun Lee
Medicine.2024; 103(2): e36945. CrossRef - USP6‐associated neoplasm as a tentative subset of postoperative spindle cell nodule
Lili Sun, Zehua Zhao, Yanmei Zhu
Histopathology.2023; 82(4): 587. CrossRef - Diagnostic Performance of Core Needle Biopsy for Characterizing Thyroidectomy Bed Lesions
So Yeong Jeong, Jung Hwan Baek, Sae Rom Chung, Young Jun Choi, Dong Eun Song, Ki-Wook Chung, Won Woong Kim, Jeong Hyun Lee
Korean Journal of Radiology.2022; 23(10): 1019. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure
Fine Needle Aspiration Cytology of Postoperative Spindle Cell Nodule in Neck after Thyroidectomy: A Case Report


Fig. 1 Cytologic findings. (A) Fragments of fibrocollagenous tissue and scattered spindle cells and (B, C) vague granulomas are observed. (D) On high power view, spindle cells with plump nuclei and indistinctive nucleoli are observed.
Fig. 2 Gross and microscopic findings. (A) The cut surface of the mass is a homogenous yellow-tan color. (B) The tumor consists of a spindle cell proliferation. (C) The high power view shows homogenous bland-looking spindle cells with plump nuclei and indistinctive nucleoli (inset). Mitoses are occasionally observed (arrows). (D) Spindle cells are reactive in vimentin.
Fig. 1
Fig. 2
Fine Needle Aspiration Cytology of Postoperative Spindle Cell Nodule in Neck after Thyroidectomy: A Case Report

 E-submission
E-submission