Search
- Page Path
- HOME > Search
Original Articles
- Significance of KM55 immunohistochemical staining in the diagnosis and prognosis of IgA nephropathy
- Hoe In Jeong, Beom Jin Lim, Minsun Jung
- J Pathol Transl Med. 2026;60(1):69-82. Published online January 14, 2026
- DOI: https://doi.org/10.4132/jptm.2025.09.17
- 2,741 View
- 182 Download
-
 Abstract
Abstract
 PDF
PDF - Background
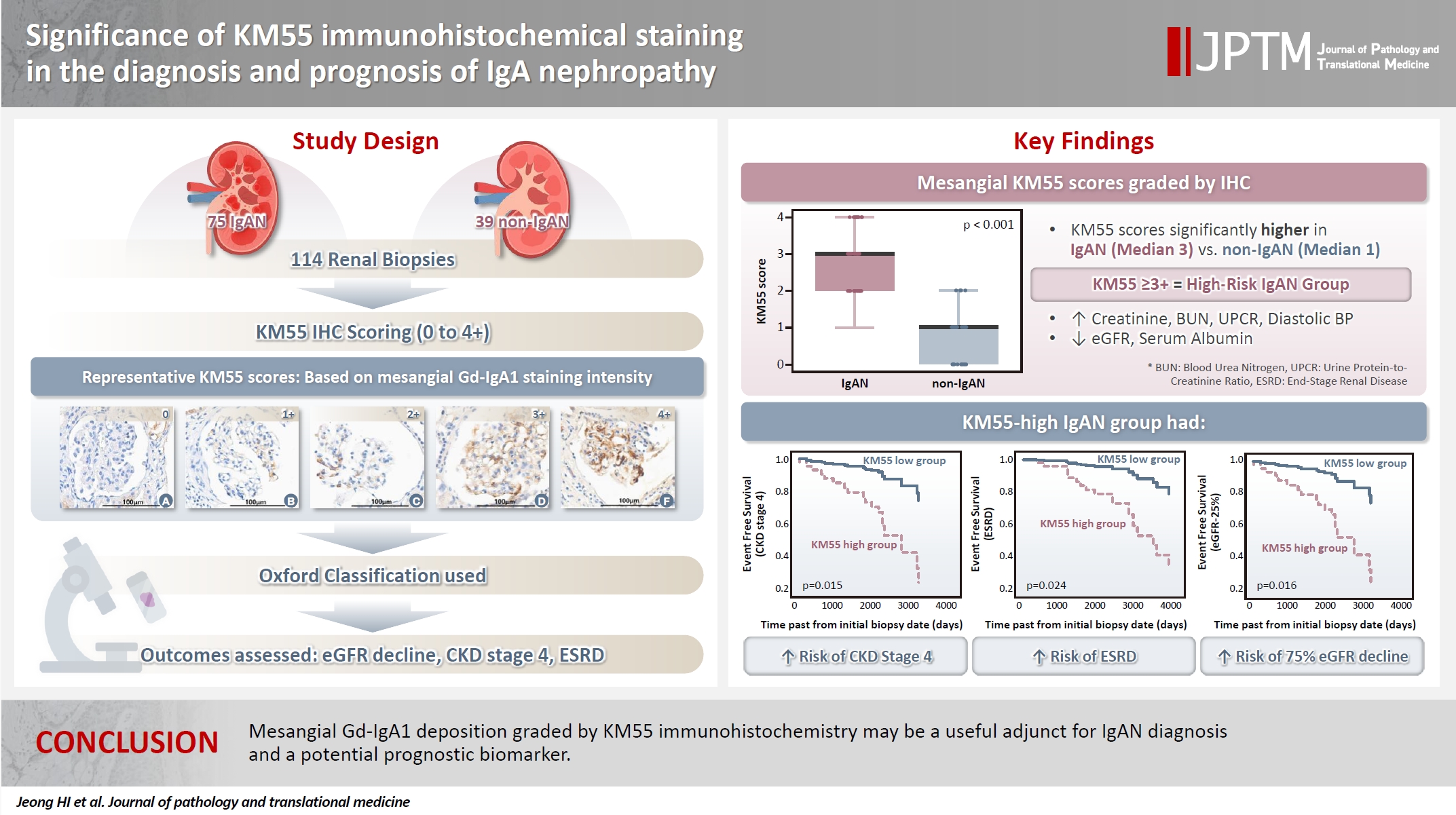
Galactose-deficient IgA1 (Gd-IgA1) plays a crucial role in IgA nephropathy (IgAN). The monoclonal antibody KM55 has emerged as a simplified method for detecting Gd-IgA1; however, the clinicopathological significance of immunohistochemistry for Gd-IgA1 remains underexplored. This study evaluated the prognostic and clinicopathological significance of KM55 immunohistochemistry in IgAN. Methods: A total of 114 native kidney biopsies showing at least mild mesangial IgA positivity on immunofluorescence were retrospectively analyzed. Patients were categorized as having IgAN or non-IgAN diseases. The KM55 immunohistochemical staining was graded as 0, 1+, 2+, 3, or 4+. Data on Oxford classification, laboratory parameters, and renal outcomes were collected. Results: The IgAN group showed significantly higher KM55 scores than the non-IgAN group (median: 3 vs. 1; p < .001). IgAN cases were further stratified into KM55-high (≥3+, n = 38) and -low groups (≤2+, n = 37). The KM55-high group had significantly higher diastolic blood pressure, blood urea nitrogen, creatinine, urine protein/creatinine ratio, and Oxford mesangial hypercellularity scores, along with lower estimated glomerular filtration rate (eGFR) and serum albumin. Cox analysis revealed significantly poorer outcomes in the KM55-high group for chronic kidney disease stage 4 (p = .015), end-stage renal disease (p = .024), and 75% eGFR decline (p = .016). Conclusions: Mesangial Gd-IgA1 deposition graded by KM55 immunohistochemistry may be a useful adjunct for IgAN diagnosis and a potential prognostic biomarker.
- Aberrant Blood Vessel Formation Connecting the Glomerular Capillary Tuft and the Interstitium Is a Characteristic Feature of Focal Segmental Glomerulosclerosis-like IgA Nephropathy
- Beom Jin Lim, Min Ju Kim, Soon Won Hong, Hyeon Joo Jeong
- J Pathol Transl Med. 2016;50(3):211-216. Published online April 11, 2016
- DOI: https://doi.org/10.4132/jptm.2016.02.01
- 10,400 View
- 75 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Segmental glomerulosclerosis without significant mesangial or endocapillary proliferation is rarely seen in IgA nephropathy (IgAN), which simulates idiopathic focal segmental glomerulosclerosis (FSGS). We recently recognized aberrant blood vessels running through the adhesion sites of sclerosed tufts and Bowman’s capsule in IgAN cases with mild glomerular histologic change.
Methods
To characterize aberrant blood vessels in relation to segmental sclerosis, we retrospectively reviewed the clinical and histologic features of 51 cases of FSGS-like IgAN and compared them with 51 age and gender-matched idiopathic FSGS cases.
Results
In FSGS-like IgAN, aberrant blood vessel formation was observed in 15.7% of cases, 1.0% of the total glomeruli, and 7.3% of the segmentally sclerosed glomeruli, significantly more frequently than in the idiopathic FSGS cases (p = .009). Aberrant blood vessels occasionally accompanied mild cellular proliferation surrounding penetrating neovessels. Clinically, all FSGS-like IgAN cases had hematuria; however, nephrotic range proteinuria was significantly less frequent than idiopathic FSGS.
Conclusions
Aberrant blood vessels in IgAN are related to glomerular capillary injury and may indicate abnormal repair processes in IgAN. -
Citations
Citations to this article as recorded by- Twin Glomeruli: a Newly Discovered Marker of Neonephrogenesis in the Ischemia–Reperfusion Injured Adult Mouse Kidney
Hanguk Hwang, Dongju Woo, You Ri Park, Min Jung Kong, Heedong Lee, Kwon Moo Park, Yong Seok Nam, Je-Yong Choi, Sungwook Nam, Eon Jung Nam, Sun-Hee Park, Hongtae Kim, Sang Yeon Lee, Soo Ho Lee, Jeong Ok Lim, Mae Ja Park
Tissue Engineering and Regenerative Medicine.2026; 23(2): 253. CrossRef - IgA nephropathy
Maria F. Soares, Ian S.D. Roberts
Current Opinion in Nephrology and Hypertension.2017; 26(3): 165. CrossRef
- Twin Glomeruli: a Newly Discovered Marker of Neonephrogenesis in the Ischemia–Reperfusion Injured Adult Mouse Kidney

 E-submission
E-submission

 First
First Prev
Prev



