Search
- Page Path
- HOME > Search
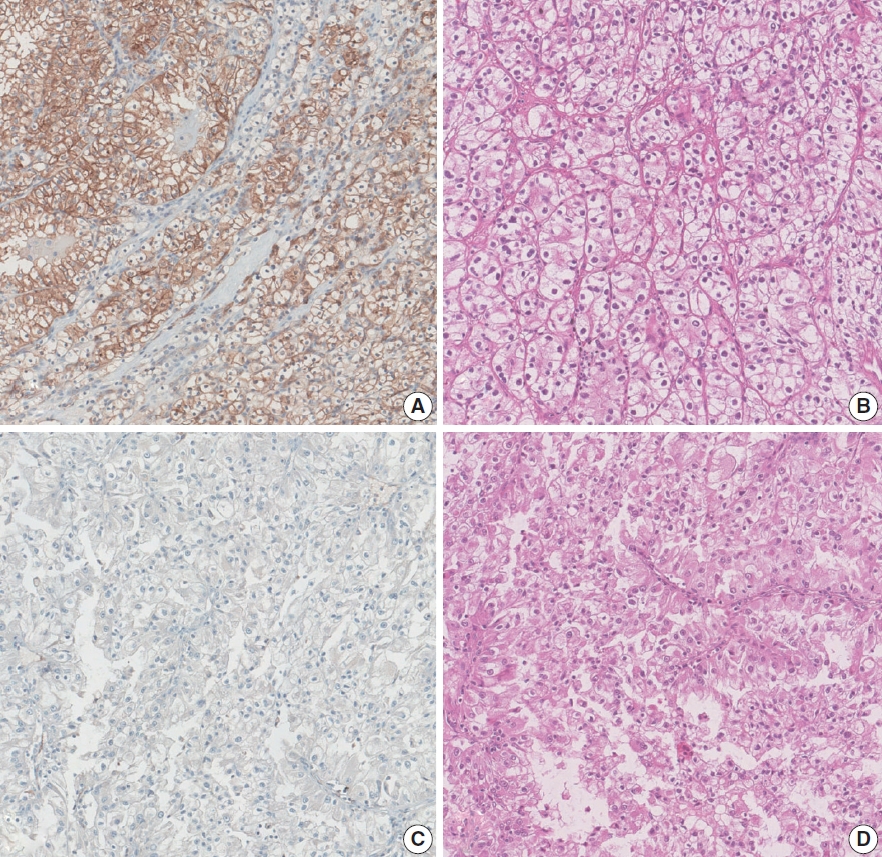
- Histopathologic classification and immunohistochemical features of papillary renal neoplasm with potential therapeutic targets
- Jeong Hwan Park, Su-Jin Shin, Hyun-Jung Kim, Sohee Oh, Yong Mee Cho
- J Pathol Transl Med. 2024;58(6):321-330. Published online September 12, 2024
- DOI: https://doi.org/10.4132/jptm.2024.07.31
- 7,304 View
- 437 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Papillary renal cell carcinoma (pRCC) is the second most common histological subtype of renal cell carcinoma and is considered a morphologically and molecularly heterogeneous tumor. Accurate classification and assessment of the immunohistochemical features of possible therapeutic targets are needed for precise patient care. We aimed to evaluate immunohistochemical features and possible therapeutic targets of papillary renal neoplasms
Methods
We collected 140 papillary renal neoplasms from three different hospitals and conducted immunohistochemical studies on tissue microarray slides. We performed succinate dehydrogenase B, fumarate hydratase, and transcription factor E3 immunohistochemical studies for differential diagnosis and re-classified five cases (3.6%) of papillary renal neoplasms. In addition, we conducted c-MET, p16, c-Myc, Ki-67, p53, and stimulator of interferon genes (STING) immunohistochemical studies to evaluate their pathogenesis and value for therapeutic targets.
Results
We found that c-MET expression was more common in pRCC (classic) (p = .021) among papillary renal neoplasms and Ki-67 proliferation index was higher in pRCC (not otherwise specified, NOS) compared to that of pRCC (classic) and papillary neoplasm with reverse polarity (marginal significance, p = .080). Small subsets of cases with p16 block positivity (4.5%) (pRCC [NOS] only) and c-Myc expression (7.1%) (pRCC [classic] only) were found. Also, there were some cases showing STING expression and those cases were associated with increased Ki-67 proliferation index (marginal significance, p = .063).
Conclusions
Our findings suggested that there are subsets of pRCC with c-MET, p16, c-MYC, and STING expression and those cases could be potential candidates for targeted therapy. -
Citations
Citations to this article as recorded by- Tissue-Based Biomarkers Important for Prognostication and Management of Genitourinary Tumors, Including Surrogate Markers of Genomic Alterations
Leonie Beauchamp, Shreeya Indulkar, Eric Erak, Mohammad Salimian, Andres Matoso
Surgical Pathology Clinics.2025; 18(1): 175. CrossRef - Papillary renal neoplasm with reverse polarity: a case report and literature review
Diego Gonzalez, Kris Kokoneshi, Sam Kwon, Ryan Thomas Mathews, Ryan Michael Antar, Maher Ali, Abiye Kassa, Michael Whalen
Frontiers in Oncology.2025;[Epub] CrossRef
- Tissue-Based Biomarkers Important for Prognostication and Management of Genitourinary Tumors, Including Surrogate Markers of Genomic Alterations
- Loss of aquaporin-1 expression is associated with worse clinical outcomes in clear cell renal cell carcinoma: an immunohistochemical study
- Seokhyeon Lee, Bohyun Kim, Minsun Jung, Kyung Chul Moon
- J Pathol Transl Med. 2023;57(4):232-237. Published online July 11, 2023
- DOI: https://doi.org/10.4132/jptm.2023.06.17
- 5,081 View
- 171 Download
- 3 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Aquaporin (AQP) expression has been investigated in various malignant neoplasms, and the overexpression of AQP is related to poor prognosis in some malignancies. However, the expression of AQP protein in clear cell renal cell carcinoma (ccRCC) has not been extensively investigated by immunohistochemistry with large sample size.
Methods
We evaluated the AQP expression in 827 ccRCC with immunohistochemical staining in tissue microarray blocks and classified the cases into two categories, high and low expression.
Results
High expression of aquaporin-1 (AQP1) was found in 320 cases (38.7%), but aquaporin-3 was not expressed in ccRCC. High AQP1 expression was significantly related to younger age, low TNM stage, low World Health Organization/International Society of Urologic Pathology nuclear grade, and absence of distant metastasis. Furthermore, high AQP1 expression was also significantly associated with longer overall survival (OS; p<.001) and progression-specific survival (PFS; p<.001) and was an independent predictor of OS and PFS in ccRCC.
Conclusions
Our study revealed the prognostic significance of AQP1 protein expression in ccRCC. These findings could be applied to predict the prognosis of ccRCC. -
Citations
Citations to this article as recorded by- Loss of Aquaporin-1 in Tumor Cells Fosters Intrahepatic Cholangiocarcinoma Progression
César I. Gaspari, Carine Beaupere, Seth Richard, Estanislao Peixoto, Bouchra Lekbaby, Mirko Minini, Branko Dubravcic, Javier Vaquero, Marie Vallette, Ander Arbelaiz, Marion Janona, Corentin Louis, Pauline Le Gall, Cédric Coulouarn, Julieta Marrone, Juan E
The American Journal of Pathology.2026; 196(2): 428. CrossRef - Construction and validation of renal cell carcinoma tumor cell differentiation-related prognostic classification (RCC-TCDC): an integrated bioinformatic analysis and clinical study
Yifan Liu, Keqin Dong, Yuntao Yao, Bingnan Lu, Lei Wang, Guo Ji, Haoyu Zhang, Zihui Zhao, Xinyue Yang, Runzhi Huang, Wang Zhou, Xiuwu Pan, Xingang Cui
Annals of Medicine.2025;[Epub] CrossRef - Prognostic Assessment of Aquaporins in Pancreatic Adenocarcinoma: An In Silico Analysis
Vignesh Krishnasamy, Lalhmingliana, Nachimuthu Senthil Kumar
Current Biotechnology.2025; 14(2): 130. CrossRef - Targeting PLOD2 induces epithelioid differentiation and improves therapeutic response in sarcomatoid renal cell carcinoma
Xiangyu Chen, Dongkui Xu, Yu Ji, Xichen Dong, Xiaomei Dong, Zihan Li, Jingyu Tan, Qianqian Sun, Huixian Xin, Ziwei Liu, Qing Deng, Tao Wen, Yanjun Jia, Xuhui Zhu, Jian Liu
Journal of Advanced Research.2025;[Epub] CrossRef - Serum Exosomal MiR-874 as a Potential Biomarker for Nonsmall Cell Lung Cancer Diagnosis and Prognosis
Amal F. Gharib, Saad S. Al-Shehri, Abdulraheem Almalki, Ayman Alhazmi, Mamdouh Allahyani, Ahmed Alghamdi, Amani A. Alrehaili, Maha M. Bakhuraysah, Althobaiti Naif Saad M., Weal H. Elsawy
Indian Journal of Medical and Paediatric Oncology.2024;[Epub] CrossRef
- Loss of Aquaporin-1 in Tumor Cells Fosters Intrahepatic Cholangiocarcinoma Progression
- Implication of PHF2 Expression in Clear Cell Renal Cell Carcinoma
- Cheol Lee, Bohyun Kim, Boram Song, Kyung Chul Moon
- J Pathol Transl Med. 2017;51(4):359-364. Published online June 13, 2017
- DOI: https://doi.org/10.4132/jptm.2017.03.16
- 9,491 View
- 168 Download
- 11 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Clear cell renal cell carcinoma (CCRCC) is presumed to be associated with adipogenic differentiation. Histone modification is known to be important for adipogenesis, and the function of histone demethylase plant homeodomain finger 2 (PHF2) has been noted. In addition, PHF2 may act as a tumor suppressor via epigenetic regulation of p53 and is reported to be reduced in colon cancer and stomach cancer tissues. In this study, we examined PHF2 expression in CCRCC specimens by immunohistochemistry.
Methods
We studied 254 CCRCCs and 56 non-neoplastic renal tissues from patients who underwent radical or partial nephrectomy between 2000 and 2003 at the Seoul National University Hospital. Tissue microarray blocks were prepared, and immunohistochemical staining for PHF2 was performed.
Results
Among 254 CCRCC cases, 150 cases (59.1%) showed high expression and 104 cases (40.1%) showed low expression. High expression of PHF2 was significantly correlated with a low Fuhrman nuclear grade (p < .001), smaller tumor size (p < .001), low overall stage (p = .003), longer cancer-specific survival (p = .002), and progression-free survival (p < .001) of the patients. However, it was not an independent prognostic factor in multivariate analysis adjusted for Fuhrman nuclear grade and overall stage.
Conclusions
Our study showed that low expression of PHF2 is associated with aggressiveness and poor prognosis of CCRCC. -
Citations
Citations to this article as recorded by- The role of histone demethylase PHF2 as a tumour suppressor in hepatocellular carcinoma by regulating SRXN1
Dexter Kai Hao Thng, Lissa Hooi, Wai Khang Yong, Dennis Kappei, Tan Boon Toh, Edward Kai-Hua Chow
Oncogenesis.2026;[Epub] CrossRef - Phosphoproteomics identifies determinants of PAK inhibitor sensitivity in leukaemia cells
Pedro Casado, Santiago Marfa, Marym M. Hadi, Henry Gerdes, Sandra M. Martin-Guerrero, Farideh Miraki-Moud, Vinothini Rajeeve, Pedro R. Cutillas
Cell Communication and Signaling.2025;[Epub] CrossRef - The role of histone methylation in renal cell cancer: an update
Yanguang Hou, Yan Yuan, Yanze Li, Lei Wang, Juncheng Hu, Xiuheng Liu
Molecular Biology Reports.2023; 50(3): 2735. CrossRef - Phosphorylation of PHF2 by AMPK releases the repressive H3K9me2 and inhibits cancer metastasis
Ying Dong, Hao Hu, Xuan Zhang, Yunkai Zhang, Xin Sun, Hanlin Wang, Weijuan Kan, Min-jia Tan, Hong Shi, Yi Zang, Jia Li
Signal Transduction and Targeted Therapy.2023;[Epub] CrossRef - HIF-1α-mediated augmentation of miRNA-18b-5p facilitates proliferation and metastasis in osteosarcoma through attenuation PHF2
Peng Luo, Yan-dong Zhang, Feng He, Chang-jun Tong, Kai Liu, He Liu, Shi-zhuang Zhu, Jian-zhou Luo, Bing Yuan
Scientific Reports.2022;[Epub] CrossRef - Integration of meta-analysis and supervised machine learning for pattern recognition in breast cancer using epigenetic data
Reza Panahi, Esmaeil Ebrahimie, Ali Niazi, Alireza Afsharifar
Informatics in Medicine Unlocked.2021; 24: 100629. CrossRef - PHF2 regulates homology-directed DNA repair by controlling the resection of DNA double strand breaks
Ignacio Alonso-de Vega, Maria Cristina Paz-Cabrera, Magdalena B Rother, Wouter W Wiegant, Cintia Checa-Rodríguez, Juan Ramón Hernández-Fernaud, Pablo Huertas, Raimundo Freire, Haico van Attikum, Veronique A J Smits
Nucleic Acids Research.2020; 48(9): 4915. CrossRef - Emerging of lysine demethylases (KDMs): From pathophysiological insights to novel therapeutic opportunities
Sarder Arifuzzaman, Mst Reshma Khatun, Rabeya Khatun
Biomedicine & Pharmacotherapy.2020; 129: 110392. CrossRef - Biology and targeting of the Jumonji-domain histone demethylase family in childhood neoplasia: a preclinical overview
Tyler S. McCann, Lays M. Sobral, Chelsea Self, Joseph Hsieh, Marybeth Sechler, Paul Jedlicka
Expert Opinion on Therapeutic Targets.2019; 23(4): 267. CrossRef - MiR-221 Promotes Hepatocellular Carcinoma Cells Migration via Targeting PHF2
Yi Fu, Mingyan Liu, Fengxia Li, Li Qian, Ping Zhang, Fengwei Lv, Wenting Cheng, Ruixing Hou
BioMed Research International.2019; 2019: 1. CrossRef - PHF2 histone demethylase prevents DNA damage and genome instability by controlling cell cycle progression of neural progenitors
Stella Pappa, Natalia Padilla, Simona Iacobucci, Marta Vicioso, Elena Álvarez de la Campa, Claudia Navarro, Elia Marcos, Xavier de la Cruz, Marian A. Martínez-Balbás
Proceedings of the National Academy of Sciences.2019; 116(39): 19464. CrossRef - Plant homeodomain finger protein 2 as a novel IKAROS target in acute lymphoblastic leukemia
Zheng Ge, Yan Gu, Qi Han, Justin Sloane, Qinyu Ge, Goufeng Gao, Jinlong Ma, Huihui Song, Jiaojiao Hu, Baoan Chen, Sinisa Dovat, Chunhua Song
Epigenomics.2018; 10(1): 59. CrossRef
- The role of histone demethylase PHF2 as a tumour suppressor in hepatocellular carcinoma by regulating SRXN1
- Clear Cell Papillary Renal Cell Carcinoma: A Report of 15 Cases Including Three Cases of Concurrent Other-Type Renal Cell Carcinomas
- Jeong Hwan Park, Cheol Lee, Ja Hee Suh, Kyung Chul Moon
- Korean J Pathol. 2012;46(6):541-547. Published online December 26, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.6.541
- 10,265 View
- 65 Download
- 23 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Clear cell papillary renal cell carcinoma (CCPRCC) is a recently established subtype of renal epithelial tumor. The aim of this study was to identify the diagnostic criteria of CCPRCC with an emphasis on immunohistochemical studies, and to report three cases with concurrent other-type renal cell carcinoma (RCC).
Methods A total of 515 RCC patients that consecutively underwent surgical resection at Seoul National University Hospital from 1 January 2010 to 31 December 2011 were screened. Each case was reviewed based on the histologic features and was evaluated immunohistochemically.
Results A total of 15 CCPRCCs were identified, which composed 2.9% of the total RCCs. The mean age was 52 years, and the average tumor size was 1.65 cm. All 15 cases showed low nuclear grade, no lymph node metastasis and no distant metastasis. The CCPRCCs showed variable architectural patterns including cystic, trabecular, papillary, and acinar. All of the cases showed moderate to intense immunoreactivity for cytokeratin 7 (CK7). CD10 was negative or showed focal weak positivity. Three cases had concurrent other-type RCC, including a clear cell RCC and an acquired cystic disease-associated RCC.
Conclusions The strong CK7 and negative or focal weak CD10 expression will be useful for the diagnosis of CCPRCC.
-
Citations
Citations to this article as recorded by- Vascular, adipose tissue, and/or calyceal invasion in clear cell tubulopapillary renal cell tumour: potentially problematic diagnostic scenarios
Ankur R Sangoi, Harrison Tsai, Lara Harik, Jonathan Mahlow, Maria Tretiakova, Sean R Williamson, Michelle S Hirsch
Histopathology.2024; 84(7): 1167. CrossRef - Clinical features and Surgical Outcome of Clear Cell Papillary Renal Cell Tumor: result from a prospective cohort
Si Hyun Kim, Jang Hee Han, Seung-hwan Jeong, Hyeong Dong Yuk, Ja Hyeon Ku, Cheol Kwak, Hyeon Hoe Kim, Kyung Chul Moon, Chang Wook Jeong
BMC Urology.2023;[Epub] CrossRef - Coexistence of multiple clear cell papillary renal cell carcinoma with renal oncocytoma: a case report
Amine Hermi, Ahmed Saadi, Seif Mokadem, Ahlem Blel, Marouene Chakroun, Mohamed Riadh Ben Slama
Annals of Medicine & Surgery.2023; 85(5): 2017. CrossRef - Renal Cell Carcinoma in End-Stage Renal Disease: A Review and Update
Ziad M. El-Zaatari, Luan D. Truong
Biomedicines.2022; 10(3): 657. CrossRef - The Clinicopathologic and Molecular Landscape of Clear Cell Papillary Renal Cell Carcinoma: Implications in Diagnosis and Management
Stanley Weng, Renzo G. DiNatale, Andrew Silagy, Roy Mano, Kyrollis Attalla, Mahyar Kashani, Kate Weiss, Nicole E. Benfante, Andrew G. Winer, Jonathan A. Coleman, Victor E. Reuter, Paul Russo, Ed Reznik, Satish K. Tickoo, A. Ari Hakimi
European Urology.2021; 79(4): 468. CrossRef - Clear cell papillary renal cell carcinoma: Characteristics and survival outcomes from a large single institutional series
James E. Steward, Sean Q. Kern, Liang Cheng, Ronald S. Boris, Yan Tong, Clint D. Bahler, Timothy A. Masterson, K. Clint Cary, Hristos Kaimakliotis, Thomas Gardner, Chandru P. Sundaram
Urologic Oncology: Seminars and Original Investigations.2021; 39(6): 370.e21. CrossRef - Clear cell papillary renal cell carcinoma: an update after 15 years
Sean R. Williamson
Pathology.2021; 53(1): 109. CrossRef - Clear Cell Papillary Renal Cell Carcinoma
Jianping Zhao, Eduardo Eyzaguirre
Archives of Pathology & Laboratory Medicine.2019; 143(9): 1154. CrossRef - Clear cell papillary renal cell carcinoma – An indolent subtype of renal tumor
Wei-Jen Chen, Chin-Chen Pan, Shu-Huei Shen, Hsiao-Jen Chung, Chih-Chieh Lin, Alex T.L. Lin, Yen-Hwa Chang
Journal of the Chinese Medical Association.2018; 81(10): 878. CrossRef - Clear cell papillary renal cell carcinoma: A case report and review of the literature
Sung Han Kim, Whi-An Kwon, Jae Young Joung, Ho Kyung Seo, Kang Hyun Lee, Jinsoo Chung
World Journal of Nephrology.2018; 7(8): 155. CrossRef - Clinical features and survival analysis of clear cell papillary renal cell carcinoma: A 10‑year retrospective study from two institutions
Yiqiu Wang, Ying Ding, Jian Wang, Min Gu, Zengjun Wang, Chao Qin, Conghui Han, Hongxia Li, Xia Liu, Pengfei Wu, Guangchao Li
Oncology Letters.2018;[Epub] CrossRef - A contemporary series of renal masses with emphasis on recently recognized entities and tumors of low malignant potential: A report based on 624 consecutive tumors from a single tertiary center
Maria Rosaria Raspollini, Ilaria Montagnani, Rodolfo Montironi, Liang Cheng, Guido Martignoni, Andrea Minervini, Sergio Serni, Giulio Nicita, Marco Carini, Antonio Lopez-Beltran
Pathology - Research and Practice.2017; 213(7): 804. CrossRef - Renal Neoplasms With Overlapping Features of Clear Cell Renal Cell Carcinoma and Clear Cell Papillary Renal Cell Carcinoma
Hari P. Dhakal, Jesse K. McKenney, Li Yan Khor, Jordan P. Reynolds, Cristina Magi-Galluzzi, Christopher G. Przybycin
American Journal of Surgical Pathology.2016; 40(2): 141. CrossRef - New and emerging renal tumour entities
Naoto Kuroda, Ondřej Hess, Ming Zhou
Diagnostic Histopathology.2016; 22(2): 47. CrossRef - Immunohistochemical Panel for Differentiating Renal Cell Carcinoma with Clear and Papillary Features
Hanan AlSaeid Alshenawy
Pathology & Oncology Research.2015; 21(4): 893. CrossRef - Immunohistochemical panel for differentiating renal cell carcinoma with clear and papillary features
Hanan AlSaeid Alshenawy
Journal of Microscopy and Ultrastructure.2015; 3(2): 68. CrossRef - Clear Cell-Papillary Renal Cell Carcinoma of the Kidney Not Associated With End-stage Renal Disease
Manju Aron, Elena Chang, Loren Herrera, Ondrej Hes, Michelle S. Hirsch, Eva Comperat, Philippe Camparo, Priya Rao, Maria Picken, Michal Michal, Rodolfo Montironi, Pheroze Tamboli, Federico Monzon, Mahul B. Amin
American Journal of Surgical Pathology.2015; 39(7): 873. CrossRef - Papillary or pseudopapillary tumors of the kidney
Fang-Ming Deng, Max X. Kong, Ming Zhou
Seminars in Diagnostic Pathology.2015; 32(2): 124. CrossRef - Do Clear Cell Papillary Renal Cell Carcinomas Have Malignant Potential?
Mairo L. Diolombi, Liang Cheng, Pedram Argani, Jonathan I. Epstein
American Journal of Surgical Pathology.2015; 39(12): 1621. CrossRef - Targeted next‐generation sequencing and non‐coding RNA expression analysis of clear cell papillary renal cell carcinoma suggests distinct pathological mechanisms from other renal tumour subtypes
Charles H Lawrie, Erika Larrea, Gorka Larrinaga, Ibai Goicoechea, María Arestin, Marta Fernandez‐Mercado, Ondrej Hes, Francisco Cáceres, Lorea Manterola, José I López
The Journal of Pathology.2014; 232(1): 32. CrossRef - Clear cell papillary renal cell carcinoma is the fourth most common histologic type of renal cell carcinoma in 290 consecutive nephrectomies for renal cell carcinoma
Haijun Zhou, Shaojiang Zheng, Luan D. Truong, Jae Y. Ro, Alberto G. Ayala, Steven S. Shen
Human Pathology.2014; 45(1): 59. CrossRef - Clear cell papillary renal cell carcinoma: Incidence, morphological features, immunohistochemical profile, and biologic behavior: A single institution study
Borislav A. Alexiev, Cinthia B. Drachenberg
Pathology - Research and Practice.2014; 210(4): 234. CrossRef - MRI Phenotype in Renal Cancer
Naomi Campbell, Andrew B. Rosenkrantz, Ivan Pedrosa
Topics in Magnetic Resonance Imaging.2014; 23(2): 95. CrossRef
- Vascular, adipose tissue, and/or calyceal invasion in clear cell tubulopapillary renal cell tumour: potentially problematic diagnostic scenarios
- The EGFR Protein Expression and the Gene Copy Number Changes in Renal Cell Carcinomas.
- Sangho Lee, Jungsuk An, Aeree Kim, Young Sik Kim, Insun Kim
- Korean J Pathol. 2009;43(5):413-419.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.5.413
- 4,742 View
- 21 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The epidermal growth factor receptor (EGFR) is known to be involved in many tumor promoting activities. EGFR inhibition has been tried as a therapeutic modality in many human malignancies.
METHODS
The expression of EGFR protein and the gene copy number changes were studied in 135 clear cell carcinomas and 16 papillary renal cell carcinomas (RCCs), and these tumors were diagnosed between 1995 and 1997.
RESULTS
An EGFR protein expression (2+ and 3+) was found in 54.1% of the clear cell RCCs and in 43.8% of the papillary RCCs. In the clear cell RCCs, its expression was associated with male gender, the tumor size (> or =4 cm) and high T stages (T2 and T3), with statistical significance. Trisomy and polysomy of the EGFR gene were found in 27 (25.7%) and 40 (38.1%) of 105 clear cell RCCs, respectively. Trisomy and polysomy were correlated with an EGFR protein expression and a high clinical T stage, with statistical significance. Among 15 papillary RCCs, 13 tumors showed trisomy (86.7%) and one showed polysomy (6.7%). Amplification was not found in both the clear cell and papillary type RCCs.
CONCLUSIONS
A considerable numbers of RCCs showed an overexpression of EGFR protein and increased EGFR gene copy numbers, yet the clinical significance of conducting a FISH study in RCC patients seems to be limited. -
Citations
Citations to this article as recorded by- EGFR protein overexpression correlates with chromosome 7 polysomy and poor prognostic parameters in clear cell renal cell carcinoma
Gordana Đorđević, Koviljka Matušan Ilijaš, Ita Hadžisejdić, Anton Maričić, Blaženka Grahovac, Nives Jonjić
Journal of Biomedical Science.2012;[Epub] CrossRef
- EGFR protein overexpression correlates with chromosome 7 polysomy and poor prognostic parameters in clear cell renal cell carcinoma
- The Relationship between Prognostic Factors and the Expression Pattern of Fascin and E-cadherin in Renal Cell Carcinoma.
- Sung Hee Kang, Seoung Wan Chae, Kyoung Bun Lee, Dong Hoon Kim, Min Kyoung Kim, Jin Hee Sohn
- Korean J Pathol. 2009;43(2):139-144.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.2.139
- 3,548 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Fascin is associated with motility in various transformed cells. Overexpression of fascin is known to aid in the progression of some cancers and is associated with a poor prognosis. E-cadherin is a major protein of epithelial cells and its expression is involved in the regulation of cell proliferation and differentiation. The aim of this study was to determine the expression pattern for fascin and E-cadherin and how it is related to the prognostic factors for renal cell carcinoma (RCC).
METHODS
The expression of fascin and E-cadherin was evaluated in 208 RCCs including 175 clear cell, 20 papillary, and 9 chromophobe types using tissue array analysis.
RESULTS
The expression of fascin increased as the tumor stage (p=0.00) and Fuhrman grade (p=0.00) increased. A high positive rate of expression for fascin was observed in cases with sarcomatoid changes (p=0.27). E-cadherin expression was seen in the distal tubules and collecting ducts of normal kidneys with a membranous pattern. The positive rate of expression for E-cadherin increased as the Fuhrman grade increased (1, 0%; 2, 23.2%; 3, 34.9%; and 4, 53.8%, p=0.00). An inverse correlation in RCCs was observed in the expression of fascin and E-cadherin (p=0.026, r=-0.158).
CONCLUSIONS
In patients with RCC, the increased expression of fascin and E-cadherin was positively correlated to poor prognostic factors such as a higher Fuhrman nuclear grade and advanced pTNM stage.
- A Pathologic Study of Renal Cell Carcinoma: Correlation between clinical and morphologic parameters and prognosis.
- Hye Seon Ahn, Moon Hyang Park
- Korean J Pathol. 1992;26(6):561-572.
- 1,893 View
- 12 Download
-
 Abstract
Abstract
 PDF
PDF - The prognostic significance of morphologic parameters was evaluated in 36 cases of renal cell carcinoma diagnosed during five years(1986~1990). We reviewed and classified on the basis of pathologic stage, tumor size, histologic pattern, cell type and nuclear grade. Mean age was 51 years old. Average tumor size was 7.3 cm in diameter. Six of 35 patients died of disease. Overall mean survival was 43.3+/-7.3 months. An increasing nuclear grade was generally correlated with a decrease in cummlative survival rate. Similarly, a higher stage at the time of diagnosis could predicated a low survival rate only for high nuclear grade carcinoma. There was an apparent positive correlation between grade and age, grade and size, grade and cell type, cell type and histologic pattern as well as stage and age. This positive correlations are in part a function of nuclear grade; only 20% of grade 3 & 4 tumor consisted of clear cells whereass 71% of grade 1 & 2 consisted of clear cell type. All 6 cases of granular cell types and 50% of mixed cell type were grade 3 & 4. The tumor size of the primary was well correlated with the nuclear grade. Nuclear grade was the most significant factor among the morphologic parameters studied.
- A Pathological Study of Renal Cell Carcinoma.
- Kwang Hwa Park, Dong Hwan Shin, In Joon Choi
- Korean J Pathol. 1989;23(3):322-330.
- 2,236 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - The most common malignant renal neoplasm is renal cell carcinoma. It is estimated that renal cell carcinoma accounts for 1% of all primary malignancies in Korea. Rell cell carcinoma presents diverse clinical courses with gross, histopathologic features. It has been known to be very difficult tumor to predict its clinical prognosis. In Korea, many studies have been reported concerning the clinical aspects of renal cell carcinoma. However, pathological studies of renal cell carcinoma are very few even though studies of nuclear grade have been attempted recently. We reviewed 93 cases of renal cell carcinoma examined in the period from 1978 to 1987 in the department of pathology, Yonsei university college of medicine, Yongdong Severance hospital, Wonju college of medicine and analyzed the histopathologic classification, including nuclear grade according to the Fuhrman's method. We abtained the following results by studying the relationship of the factors which had been known as correlated with the prognosis. 1) The ages of patients ranged from 9 to 74 years with a peak in the 6th decade. 2) The most common symptoms of the patients were hematuria, mass and pain, in that oder, and 7 patients complained to specific symptoms. The incidentally found cases characterized stage I, nuclear grade 2 small tumor size (not more than 4 cm) and clear cell type. 3) The renal cell carcinoma was more frequently located in the left kidney than the right by a ratio of 1.25 : 1. The incidence of intrarenal location was divided to the upper pole, 40% : mid portion, 29% : lower pole, 23% : diffuse involvement, 8%. The tumor shoing diffuse growth pattern had a large size, high nuclear grade and mixed cells. 4) The tumor size averaged 8 cm and there was no significant relationship between the size and stage. Seven cases of neoplasms not more than 3 cm were seen, of which 2 cases revealed an outcome of distant metastasis. 5) The histological pattern showed major solid, 53% : tubular, 11% : mixed, 18% : papillary, 9% and sarcomatoid type 9%. The sarcomatoid type was characterized by grade 4, a larger size(more than 10 cm), advanced stage. 6) There was no special relationship between the stage and grade but mostly grade 2 occupied the stage I. 7) The clear cell type was predominantly noted at grade 2 (65%), at the stage I (63%), granular or mixed cell type at grade 3 (87%), 4 (70%). According to these results, the tumors showing a sarcomatoid histologic pattern, diffuse growth pattern had unfavorable prognostic factors, and are thus estimated to have a poor prognosis. But the case which were incidentally found have favorable prognostic factors and probably a better prognosis. The tumor size alone can not exactly predict the metastasis and is not correlated with the stage. Small renal cell neoplasm (not more than 3 cm) generally has unfavorable prognostic factors and should be considered potentially malignant. The high grade frequently has granular cytoplasm. This represents the relationship between grade and cytoplasm, poor prognosis in the granular cell than the clear. The renal cell carcinoma shows variable prognosis and thus the prognosis should be estimated by all the factors. Nuclear grade can be used as one of the useful prognostic factors.
- Chromophobe Renal Cell Carcinoma.
- Yeong Jin Choi, Tae Kon Hwang, Youn Soo Lee, Eun Jung Lee, Seok Jin Kang, Byung Kee Kim, Sang In Shim
- Korean J Pathol. 1999;33(4):259-266.
- 2,241 View
- 26 Download
-
 Abstract
Abstract
 PDF
PDF - We report 13 chromophobe renal cell carcinomas (10.8%) observed among 120 renal cell carcinomas in adults. The average age was 53 (range: 34-72) years old, and 6 were males and 7 females. The mean tumor size was 10 (range: 5-17) cm, mean nuclear grade 2.4, and mean Robson's stage was 1.9. There were two distinct histologic variants; typical variant (n=9) and eosinophilic variant (n=4). Both of them showed typical light microscopic features and positive reaction with Hale's colloidal iron and carbonic anhydrase II, a marker protein of intercalated cells of renal collecting ducts. A strong positive immunoreactivity for epithelial membrane antigen was noted in the cytoplasm in 12 of 13 tumors. Numerous microvesicles, 180~440 nm in diameter, were identified ultrastructurally. DNA aneuploidy was found in 3 out of 10 cases. Neither local recurrence nor metastasis have been identified during the following period of 4~144 (mean 48) months.
- Immunohistochemical Markers for Metastasis in Clear Cell Renal Cell Carcinoma.
- Kyungeun Kim, Cheryn Song, Jae Y Ro, Hanjong Ahn, Yong Mee Cho
- Korean J Pathol. 2008;42(2):81-86.
- 2,572 View
- 25 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Renal cell carcinoma (RCC) is notorious for its high metastatic potential, and 30% of RCC patients present with metastatic disease at the initial presentation and 50% of them will develop metastasis or recurrence after radical surgery.
METHODS
In an attempt to identify the best predictive marker(s) for metastasis in patients with clear cell RCCs (CRCCs), we examined the expression patterns of 7 metastasis/prognosis-related markers by constructing a tissue microarray including primary CRCC specimens from 30 metastatic and 60 nonmetastatic CRCCs. The markers we studied were Ki-67, MUC1, CD44s, PTEN, gelsolin, CA9 and p53.
RESULTS
The expressions of Ki-67, PTEN, CD44s, gelsolin and p53 were increased, whereas those of MUC1 and CA9 were decreased in the metastatic CRCCs compared with the non-metastatic CRCCs. The receiver operating characteristic curve-area under the curve (AUC) value of Ki-67 was 0.671, which was the highest among the 7 markers. The optimal cut-off value, sensitivity and specificity of the Ki-67 expression were 1.67%, 86.7% and 41.7%, respectively.
CONCLUSIONS
These results demonstrate that the Ki-67 expression was increased in metastatic CRCCs, and it had the highest predictive value among the 7 markers. This suggests that Ki-67 could be an excellent predictive marker for metastasis in CRCC patients.
- A Study on the Expression of p53 Oncogene Products, PCNA Index and DNA Ploidy in Renal Cell Carcinoma.
- Jong Jae Jung, Ji Shin Lee, Chan Choi
- Korean J Pathol. 1997;31(7):672-682.
- 1,984 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - Mutant p53 is associated with the advanced stages of some human tumor but there is a wide variation in the reported incidence of p53 mutation in renal cell carcinoma and its prognostic significances. We designed this study to assess the expression of p53 in renal cell carcinomas and to compare with the established prognostic factors. Immunoreactivity for p53 protein and proliferating cell nuclear antigen (PCNA) were assessed in 44 cases of primary renal cell carcinoma, and flow cytometric analysis of DNA ploidy was perfon-ned in 37 of those cases. p53 protein was over-expressed in 16/44 (36.4%) renal cell carcinomas and 5 rumors had more than 10 immunoreactive tumor cells. The expression of p53 protein was positively related to nuclear grade (p=0.007) and PCNA index (p=0.002), but was independent of stage and DNA ploidy. In univariate survival analysis, stage (p<0.001), nuclear grade (p=0.017), DNA ploidy (p=0.045) and PCNA index (p<0.001) were significantly associated with patient survival. However, considering the stage, all of the last three factors had no prognostic influence. Cases showing strong positivity of p53 expression had worse prognosis than those with no or weak p53 expression, especially in early lesions (stage I,II) (p<0.001).
- A Case Report of Renal Cell Carcinoma in a Polycystic Kidney: A case report.
- Kyoung Chan Choi, Joon Hyuk Choi, Won Hee Choi
- Korean J Pathol. 1996;30(1):57-60.
- 2,097 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - A forty-nine-year-old woman with polycystic disease had a right nephrectomy for what was preoperatively thought to be a polycystic disease, but at surgery turned out to be a tumor based on frozen section. Microscopic examination revealed papillary type, renal cell carcinoma with classical features of adult polycystic kidneys. Radiologic findings revealed multiple cysts in the liver. The clinical recognition of a carcinoma developing in polycystic kidneys is often difficult because of the presence of preexisting large renal masses and occasional hematuria. Renal cell carcinoma should be thought of when confronted with abdominal pain or back pain, severe hematuria, sudden dysuria or a new renal mass occurring in a patient with polycystic kidneys.
- The Prognostic Implications of the Histologic Subtype and the Expression of Phosphorylated ERK 1/2 in Papillary Renal Cell Carcinoma.
- Bo Sung Kim, Dong Il Kim, Tae Hoon Kang, Eun Shin, Kyung Chul Moon
- Korean J Pathol. 2008;42(4):215-222.
- 2,107 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The authors of this study wanted to confirm the prognostic implication of the histologic subtype; further, we wanted to explore the expression of phosphorylated extracellular signal-regulated kinase 1/2 (pERK) in papillary renal cell carcinoma (PRCC) and determine its clinicopathologic and prognostic significance.
METHODS
A total of 45 patients who underwent nephrectomy for PRCC were enrolled in this study. The hematoxylin and eosin slides were reviewed and pERK immunohistochemistry was performed.
RESULTS
Type 2 PRCC was significantly correlated with a larger tumor size (p=0.030), a higher nuclear grade (p<0.001), a more advanced tumor stage (p=0.041) and more frequent distant metastasis (p=0.019). The tumors were pERK-low (0 and 1+) in 30 cases (66.7%) and pERK-high (2+) in 15 cases (33.3%). The pERK-high PRCC was significantly associated with a smaller tumor size (p=0.001) and an earlier tumor stage (p=0.004). On the univariate analysis, the histologic subtype, the TNM stage and the pERK status were significantly associated with progression-free survival (PFS). Multivariate analysis showed that the histologic subtype (hazard ratio 22.81, p=0.042) and the TNM stage (hazard ratio 23.48, p=0.009) were independent prognostic factors for PFS.
CONCLUSIONS
Type 2 PRCC, together with the TNM stage, was identified as one of independent poor prognostic factors for PFS. The pERK status was a prognostic factor for PFS on the univariate analysis, but not on the multivariate analysis.
- Correlation between Nuclear Grades and the Numbers of AgNORs and PCNA Labeling Indices in Renal Cell Carcinoma.
- Hye Jin Lee, Young Im Han, Kang Suek Suh, Sun Kyung Lee
- Korean J Pathol. 1996;30(2):132-139.
- 1,858 View
- 12 Download
-
 Abstract
Abstract
 PDF
PDF - The author examined the number of AgNORs and PCNA labeling indices by histochemical and immunohistochemical studies in 20 cases of renal cell carcinoma, composed of 5 cases according to the nuclear grades. The results obtained are summarized as follows; 1) Mean number of AgNORs according to the nuclear grades of renal cell carcinoma were 1.38+/-0.40 (mean+/-standard deviation) for Grade I, 2.53+/-0.33 for Grade II, 5.43+/-0.66 for Grade III, and 7.88+/-0.72 for Grade IV. The mean numbers of AgNORs according to the nuclear grades were significantly increased(p=0.0005). 2) PCNA labeling indices (positive nuclear ratio) according to the nuclear grades of renal cell carcinoma were 5.90+/-2.36 for Grade I, 19.30+/-6.71 for Grade II, 45.73+/-8.62 for Grade III, and 61.83+/-6.34 for Grade IV. Also, the PCNA labeling indices according to the nuclear grades were significantly increased(p=0.0008). 3) The mean numbers of AgNORs directly correlated with the PCNA labeling indices (r=0.9861, p<0.001). On the basis of the above results, it was considered that the numbers of AgNORs and PCNA labeling indices as markers of proliferative activity of tumor cells correlate well with the nuclear grades of renal cell carcinoma.
- Multilocular Cystic Renal Cell Carcinoma.
- Myoung Jin Ju, Kee Tac Jang, Je Geun Chi
- Korean J Pathol. 1997;31(11):1240-1243.
- 1,992 View
- 10 Download
-
 Abstract
Abstract
- Multilocular cystic renal cell carcinoma is a distinct subtype of renal cell carcinoma with its pathological characteristics and good prognosis. Multilocular renal cysts and renal cell carcinoma with cystic change are important differential diagnoses. We report a case of multilocular cystic renal cell carcinoma in a 37-year-old woman who came to the hospital because of the right renal mass. The removed right kidney showed a 6x4 cm well defined cystic mass in the lower pole. On cut section there were multiple cavities in the mass, filled with serosanguineous fluid and focal yellowish solid area. Microscopically, these cysts were lined by a single layer of flat or cuboidal cells consisted of clear cytoplasm with small central nuclei. In some portions of the tumor, the clear neoplastic cells formed sheets within the septa or walls of the cysts.
- Tumor Angiogenesis in Renal Cell Carcinoma.
- Ji Shin Lee, Jong Jae Jung, Chang Soo Park
- Korean J Pathol. 1999;33(11):1055-1060.
- 1,931 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - Angiogenesis is essential for the growth of solid tumors. Microvessel counts, which represent a measure of tumor angiogenesis, have been correlated with the overall survival of patients with a variety of malignancies. However, the significance of angiogenesis in renal cell carcinoma remains controversial. To determine whether angiogenesis correlates with prognosis of patients with renal cell carcinoma, we counted the microvessels within the primary tumors and compared their numbers with patients' prognosis. Tumor specimens from 42 patients were investigated. Microvessels were stained with anti-CD34 and anti-factor VIII-related antigen monoclonal antibodies. Significant correlation between microvessel counts for two antibodies was observed (r=0.875, p<0.01), although microvessel counts for CD34 were approximately two times higher. Microvessel counts were higher in clear cell than in non-clear cell carcinoma (p<0.05). These results suggest that immunostaining with anti-CD34 antibody may provide a more sensitive and accurate measure of tumor angiogenesis. There was no correlation between microvessel counts and nuclear grade, or TNM stage. In univariate analyses, nuclear grade and TNM stage were significantly associated with patient survival (p<0.01). But further studies on tumor angiogenesis of renal cell carcinoma are needed before it can be adopted as a prognostic marker.
- Correlation of Clinical Stage and Presumptive Prognostic Factors in Renal Cell Carcinoma.
- Jin Ye Yoo, Hye Jae Cho
- Korean J Pathol. 1999;33(11):1061-1066.
- 2,022 View
- 16 Download
-
 Abstract
Abstract
 PDF
PDF - Renal cell carcinoma is the most common primary cancer of the kidney. The tumor stage is a reliable prognostic marker in renal cell carcinoma which is significantly associated with patient survival. But assessment of other prognostic factors has produced varying and often conflicting results. We reevaluated the significance of varied prognostic parameters in 33 cases of renal cell carcinoma; clinical stage, cell type, histologic pattern, DNA ploidy, Ki-67 labeling index, and bcl-2 oncoprotein expression. We could not statistically prove that DNA ploidy and bcl-2 expression were related to any examined parameters. Cell type was not related to clinical stage nor nuclear grade but there was a significant correlation (p=0.002) between cell type and histologic pattern. Nuclear grade (p=0.007) and Ki-67 labeling index (p=0.036) were significantly related to clinical stage, suggesting their value as complementary prognostic markers for renal cell carcinoma.
- Urine Cytology of Renal Cell Carcinoma: Analysis of 11 cases.
- Yi Kyeong Chun, Hye Jae Cho, Ill Hyang Ko
- J Pathol Transl Med. 1994;5(2):137-142.
- 4,258 View
- 166 Download
-
 Abstract
Abstract
 PDF
PDF - Urine cytology is of limited value in the diagnosis of renal cell carcinoma with reported detection rates of 0~80%. The aim of this study is to demonstrate the usefulness of urine cytology in renal cell carcinoma, In the eleven histologically proven cases of renal cell carcinoma, urinary smears were reevaluated. The cytologic results were as follows; positive for malignant cells in 3 cases (27%), suspicious in 2 cases (18%) and negative in 6 cases (55%). The average diameter of the tumor of the 5 cases reported as positive or suspicious for malignant cells was 9.7cm and 3 had invaded the renal pelvis. The other 6 tumors, reported as negative, were 5.7cm in average diameter and one of them showed involvement of the renal pelvis. These results suggest that urine cytology is considered unsatisfactory in the early detection of renal cell carcinoma. However. careful examination of urinary smear could improye the detection rate especially in more advanced cases involving the renal pelvis as well as those of larger tumors.
- Renal Cell Carcinoma Associated with Rhabdomyosarcomatous Component: Report of a case.
- Mee Soo Chang, Mi Kyung Jee, Kyo Young Lee, Sang In Shim, Sun Moo Kim
- Korean J Pathol. 1987;21(1):40-44.
- 2,029 View
- 13 Download
-
 Abstract
Abstract
 PDF
PDF - Renal cell carcinoma, intimately associated with a sarcomatous component, is a rare malignant renal tumor. There is disagreement whether these represent true sarcomas or are sarcomatoid metaplasia. Therefore, this sarcomatous component is at times still a troublesome problem for pathologists. In March, 1986, we experienced a case of renal cell carcinoma associated with rhabdomyosarcomatous component in 47 year-old woman who had a rapidly enlarged, palpable abdominal mass. Grossly, a spherical renal cell carcinoma, 17x14x10 cm, in upper and middle portions of the right kidney showed extension through the renal capsule into the perirenal fat. Area of myxoid change was evident in the reanl cell carcinoma, with extensive hemorrhagic necrosis. Microscopically, in the myxoid area, there was malignant spindle cell proliferation in which many rhabdomyoblasts showing distinct cross striation could be demonstrated. This rhabdomyosarcomatous component intermixed with renal cell carcinoma of clear cell type could be also identified in the focal area.
- E-Cadherin Expression in Renal Cell Carcinoma according to the Mainz Classification.
- Ju Han Lee, Hyun Deuk Cho, Dale Lee, Nam Hee Won
- Korean J Pathol. 1999;33(12):1131-1138.
- 2,538 View
- 27 Download
-
 Abstract
Abstract
 PDF
PDF - According to the Mainz classification, renal cell carcinoma (RCC) consists of three subtypes: each has characteristic genetic alterations within the chromosomal or mitochondrial DNA. The three subtypes are: clear cell type, chromophil type, and chromophobe type. E-cadherin is a Ca++-dependent adhesion molecule which plays a major role in the maintenance of intercellular adhesion in epithelial tissues. In a normal kidney, E-cadherin is expressed in the distal tubule and the collecting duct, but not in the proximal tubule. We reclassified 110 cases of RCC according to mainz classification. Immunohistochemical staining for E-cadherin was done on twenty eight cases of RCC, including 18 cases of clear cell type, four cases of chromophil type, and six cases of chromophobe type. The results were as follows: 1) of the 110 cases of RCC, 96 cases (87.3%) were of clear cell type, four cases (3.6%) of chromophil type, and ten cases (9.1%) of chromophobe type, 2) there was no significant correlation between the nuclear grade and clinical stage according to each subtype, 3) E-cadherin expression showed a strong positive reaction along the cell membranes in all six cases of chromophobe type. The differential expression of E-cadherin in RCC may suggest that the chromophobe type may have different biologic characteristics from other types of RCC.
- Renal Cell Carcinoma Associated with Xp11.2 Translocation: Clinicopathologic and Immunohistochemical Findings of 4 Cases.
- Sanghui Park, Ji Eun Kwon, Yeon Lim Suh
- Korean J Pathol. 2005;39(6):406-411.
- 2,096 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The new WHO classification includes the recently described renal cell carcinomas (RCC) that are associated with several different translocations, involving chromosome Xp11.2, and they all result in gene fusions involving the TFE3 gene. The authors describe the clinicopathologic and immunohistochemical findings of 4 patients who had the morphologic features of RCC with Xp11.2 translocations.
METHODS
Among 9 surgically resected and pathologically proven pediatric RCCs, 4 showed a typical RCC histopathology with the Xp11.2 translocation. Immunohistochemical stains were performed for TFE3, AE1/AE3, epithelial membrane antigen, vimentin, HMB45, S-100 protein and CD10.
RESULTS
The 4 study subjects included one male and 3 females, and their chief complaints were gross hematuria and abdominal pain. Histologically, the tumors showed two different histologic types: type 1 tumors (2 cases) that corresponded to those of ASPL-TFE3 RCC, and type 2 tumors (2 cases) that corresponded to PRCC-TFE3 RCC. Nuclear TFE3 immunostaining was seen in 3 cases. All the tumors were immunoreactive for CD10, and vimentin and cytokeratin were expressed in 3 cases and HMB-45 was expressed in 2 cases.
CONCLUSIONS
Our results show that significant numbers of pediatric RCC are translocation-related. Therefore, when one encounters an RCC in the pediatric population, the possibility of a translocation-related RCC should be kept in mind.
- Metastatic Renal Cell Carcinoma in Maxillary Sinus: A case report.
- Gyeong Yeob Gong, Chang Hun Lee, Kang Suek Suh, Sun Kyung Lee
- Korean J Pathol. 1991;25(4):392-394.
- 2,203 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - Metastases to the sinonasal tract are infrequent occurrences from primaries below the clavicles. The total number of reported cases to date is less than 100. There is, however, complete unanimity concerning the histologic type of metastatic neoplasm most often encountered. An interesting phenomenon, generally attributable only to breast and renal cell carcinoma, is the late recurrence of the malignant tumor, even 10 or more years after operation. A 61 year-old-male was admitted to ENT due to frequent epistaxis and right facial swelling. CT scan revealed a huge soft tissue density mass I right maxillary sinus with extension into nasopharynx and deviation of nasal septum. The histologic diagnosis was metastatic renal cell carcinoma. He had left nephrectomy because of renal cell carcinoma, 14 years ago. We report a case of metastatic renal cell carcinoma of maxillary sinus in view of rarity, and a brief review of the literature related to this type of tumor is presented.
- Expression of Heat Shock Protein 27 and Apoptosis in Renal Cell Carcinomas.
- Ghil Suk Yoon
- Korean J Pathol. 2006;40(1):39-45.
- 2,194 View
- 23 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Heat shock protein 27 (HSP27) is induced by heat shock and other pathophysiologic stresses, including neoplastic transformation. We examined the relationship between the HSP27 expression and the clinical and histologic parameters to elucidate the biologic and prognostic significance of HSP27 in renal cell carcinomas (RCCs). Its regulation of apoptosis in RCC development was also observed.
METHODS
We performed immunohistochemical studies for HSP27, caspase 3 and TUNEL on paraffin-embedded tissue microarray specimens from 48 RCCs.
RESULTS
There was a tendency to higher expression of HSP27 in the RCC than in normal renal tubular cells. Of the 48 RCCs, the HSP27 expression was positive in 38 cases. An inverse relationship was found between the Fuhrman nuclear grade and HSP27 expression, but this was without statistical significance (r=-0.218, p=0.093). No relationship between the HSP27 expression and the other parameters was observed. Also, no statistically significant difference was observed between apoptosis and the HSP27 expression more (p=0.951).
CONCLUSIONS
Although HSP27 expression was increased in RCC than in normal renal tubular cell the HSP27 expression may not be a powerful and statistically significant prognostic indicator in patients with RCC.
- Cytologic Features of Renal Cell Carcinoma: Clear Cell, Granular Cell and Oncocytoma.
- Yeong Jin Choi, Youn Soo Lee, Mi Seon Kwon, Kyo Young Lee, Byung Kee Kim, Sang In Shim
- J Pathol Transl Med. 1996;7(1):31-37.
- 3,164 View
- 141 Download
-
 Abstract
Abstract
 PDF
PDF - It is well known that fine needle aspiration biopsy(FNAB) is very useful and has a high accuracy rate in the diagnosis of renal neoplasms. Although there is some indecision to perform the FNAB for a rare possibility of tumor seeding along the biopsy needle tract, it tends to be used increasingly. As in the cytologic diagnosis of metastatic lesion through out the body, renal cell carcinoma should nearly always be considered in the differential diagnosis, the precise understainding of cytologic features of renal cell carcinoma with various cell types and architectural patterns is necessarily required. In this report, we present three cases of primary renal cell tumors, two of renal cell carcinomas and one of oncocytoma, preponderantly emphasizing the cytologic differential points in the FNAB specimen.
- Epidermal Growth Factor Receptor Expression and Cell Proliferation in Renal Cell Carcinoma.
- Ji Shin Lee, Jong Jae Jung, Min Cheol Lee, Chang Soo Park
- Korean J Pathol. 2000;34(4):273-279.
- 2,271 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - The epidermal growth factor receptor (EGFR) is a transmembrane glycoprotein whose expression is a possible cause of increased tumor cell proliferation and has recently been proposed as a prognostic parameter in some tumors. Expression of EGFR was studied immunohistochemically in 62 cases of human renal cell carcinomas to evaluate their possible prognostic roles. We also examined the correlation between EGFR expression and cell proliferation by immunohistochemical staining for proliferating cell nuclear antigen (PCNA). Fifty-six cases (90.3%) expressed EGFR, with staining largely confined to the cell membrane and cytoplasm. Staining intensity of EGFR was directly correlated with nuclear grade (p=0.000) and TNM stage (p=0.015). PCNA index was significantly higher in EGFR-positive tumors than in EGFR- negative tumors. There was a statistically significant positive correlation between PCNA index and increasing staining intensity of EGFR (p=0.000). In univariate survival analysis, EGFR expression was significantly associated with shortened survival. However, EGFR expression was not an independent prognostic factor by multivariate analysis. These findings suggest that EGFR expression may be an important cause of tumor cell proliferation in renal cell carcinoma and further studies are needed to evaluate whether EGFR expression analysis provides independent prognostic information.
- Sarcomatoid Renal Cell Carcinoma; Special Reference to its Distinction from Carcinosarcoma.
- Kee Taek Jang, Yeon Mee Kim, Je Geun Chi
- Korean J Pathol. 1998;32(5):378-381.
- 1,889 View
- 10 Download
-
 Abstract
Abstract
- Sarcomatoid renal cell carcinoma is an uncommon tumor that has to be distinguished from renal carcinosarcoma. We have described three cases of sarcomatoid renal cell carcinoma showing different clinical and light microscopic features. An ultrastructural study of the tumor cells from the sarcomatoid area revealed frequent desmosomal junction, confirming the epithelial nature of the neoplasm. All three cases showed an aggressive clinical course and tended to invade adjacent organs or tissues. We believe that an histological and immunohistochemical examination in conjunction with an electron microscopic examination are necessary to diagnose sarcomatoid renal cell carcinoma.
- Analysis of Gene Expression in Renal Cell Carcinomas Using cDNA Microarray: Reduced Expression of Decorin in Renal Cell Carcinomas.
- Jin Sook Lee, Kang Suek Suh, Kyung Un Choi, Jee Yeun Kim, Do Youn Park
- Korean J Pathol. 2003;37(4):232-238.
- 1,951 View
- 14 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Identification of the genes expressed differentially in renal cell carcinoma (RCC)but not in the non-cancerous kidney is important for understanding the molecular basis ofrenal cell carcinoma and for defining possible prognostic value and therapeutic intervention.We investigated the changes in gene expression accompanying the development and progression of kidney cancer by cDNA microarrays.
METHODS
To identify molecular alterations in renal cell carcinoma, we measured expression profiles for paired neoplastic and noncancerouskidney samples from an individual by means of a cDNA microarry representing 7, 500genes. Of the differentially expressed genes, we assessed the decorin gene at the proteinlevel using immunohistochemistry.
RESULTS
The 60 genes were noted to have more than a fivefold change in expression (either increased or decreased) in RCC compared to the noncancerouskidney. The changed genes are those associated with signal transduction, metabolizingenzymes, the cytoskeleton, cell adhesion, cell cycle control, modulation of transcription, the tumor suppressor gene and tumor antigens. Under immunohistochemistry, the expressionof decorin was significantly decreased in the tumor than in the non-cancerous kidney.The expression rate of decorin was not associated with the patient's sex, age, histologic type, Fuhrmann nuclear grade and T stage.
CONCLUSION
The author predicted that these geneexpression profiling experiments will lead to improvements in the basic understanding of renaltumor pathogenesis and will promote the discovery of novel molecular markers for renal tumordiagnosis and therapy.
- Multilocular Cystic Renal Cell Carcinoma: A case report.
- Ki Jung Yun, Weon Cheol Han, Chan Choi, Hyung Bae Moon, Joung Sik Rim
- Korean J Pathol. 1992;26(3):314-316.
- 2,077 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - Multilocular cystic renal cell carcinoma appears to be a distinct and rare subtype of renal cell carcinoma with characteristic gross and microscopic features. Multilocular cystic renal cell carcinoma should be separated from multilocular cyst, multilocular cystic nephroma, and renal cell carcinoma with cystic degeneration. We present a case of multilocular cystic renal cell carcinoma. A 61-year-old man presented with right flank pain for 4 years. The computerized tomography revealed multilocular cystic mass in the upper pole of right kidney. The cystic mass measured 4.5x4 cm. The cyst was multilocular and locules not communicated with each other. The solid area was not present. Microscopically, the locules were lined by flat or cuboidal neoplastic clear cells. The clear cells were focally aggregated in the septa. The nephron was not present in the septa.
- Eosinophilic Cytoplasmic Globules in Papillary Renal Cell Carcinoma: A Case Report.
- Ok Ran Shin, Jae Young Park, Hae Kyung Lee, Young Seok Lee, Chang Hee Han, Sung Hak Kang, Kyo Young Lee, Yeong Jin Choi
- Korean J Pathol. 2006;40(6):466-468.
- 2,455 View
- 28 Download
-
 Abstract
Abstract
 PDF
PDF - Eosinophilic cytoplasmic globules may be seen in a variety of neoplastic and nonneoplastic conditions and are most often associated with alpha-1-antitrypsin deficiency, several pathologic liver conditions and yolk sac tumors. A few cases of eosinophilic cytoplasmic globules in renal cell carcinoma have been reported but there has only been one report of papillary type. We report another case of papillary renal cell carcinoma with eosinophilic cytoplasmic globules, which is similar to a Mallory body but with different properties.
- Fine Needle Aspiration Cytology of Papillary Renal Cell Carcinoma: A Case Report.
- Yeong Ju Woo, Sung Sook Kim, Jong Wha Lee
- J Pathol Transl Med. 1998;9(1):95-98.
- 2,169 View
- 47 Download
-
 Abstract
Abstract
 PDF
PDF - Papillary renal cell carcinoma(RCC) is an uncommon subtype of RCC that has distinctive gross, histologic, and cytogenetic features. The cytologic features of FNA are abundant papillary clusters and relatively few single cells. The cells are usually small and contain uniform nuclei; numerous macrophages with foamy cytoplasm are often found in the background. We describe a case of papillary renal cell carcinoma evaluated by fine needle aspiration cytology(FNAC) in a 42 year-old man. The smear showed a few papillary clusters and numerous macrophages with foamy cytoplasm in the background. With adequate cellularity, papillary RCC can be distinguished reliably from non-papillary RCC by FNAC.
- Loss of Heterozygosity at VHL, FHIT, and p16 Loci in Nonpapillary Renal Cell Carcinoma.
- Won Sang Park, Seung Myung Dong, Yong Hyun Cho, Tae Gon Hwang, Su Young Kim, Min Sun Shin, Jae Ho Pi, Suk Hyung Lee, Nam Jin Yoo, Jung Young Lee
- Korean J Pathol. 1999;33(1):8-14.
- 2,028 View
- 21 Download
-
 Abstract
Abstract
 PDF
PDF - The objectives of this study were to characterize the alterations of 3p and 9p in sporadic renal cell carcinomas (RCC) and to assess the relationship between the clinical stages or tumor size and the alteration of these chromosomes. Thirty eight archival, paraffin embedded tissue sections from 38 patients with RCC were analyzed for loss of heterozygosity (LOH) at 3p and 9p with 11 microsatellite markers. LOH was detected in 81.6% (31/38) and 37.8% (14/37) at 3p and 9p, respectively. The frequencies of LOH at VHL and FHIT locus were 75.6% and 72.2%, respectively. Twelve cases out of 38 showed LOH at both 9p21 and 3p. The loss of 3p in the samples tested was not related to clinical stages and tumor size, but that of 9p21 was significantly associated with advanced stage and larger tumor size. These results support that 3p deletion, including VHL and FHIT gene, play a critical role in the tumorigenesis of sporadic RCC, especially at early stage, and that 9p21 may contribute to the progression of sporadic RCC.

 E-submission
E-submission


 First
First Prev
Prev



