Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 50(5); 2016 > Article
-
Brief Case Report
Pelvic Nodular Histiocytic and Mesothelial Hyperplasia in a Patient with Endometriosis and Uterine Leiomyoma - Yumin Chung, Rehman Abdul, Se Min Jang, Joong Sub Choi1, Kiseok Jang
-
Journal of Pathology and Translational Medicine 2016;50(5):397-400.
DOI: https://doi.org/10.4132/jptm.2016.01.11
Published online: April 4, 2016
Department of Pathology, Hanyang University College of Medicine, Seoul, Korea
1Division of Gynecologic Oncology and Gynecologic Minimally Invasive Surgery, Department of Obstetrics and Gynecology, Hanyang University College of Medicine, Seoul, Korea
- Corresponding Author Kiseok Jang, MD, PhD Department of Pathology, Hanyang University College of Medicine, 222-1 Wangsimniro, Seongdong-gu, Seoul 04763, Korea Tel: +82-2-2290-8248, Fax: +82-2-296-7502, E-mail: medartisan@hanyang.ac.kr
• Received: December 10, 2015 • Revised: January 6, 2016 • Accepted: January 11, 2016
© 2016 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
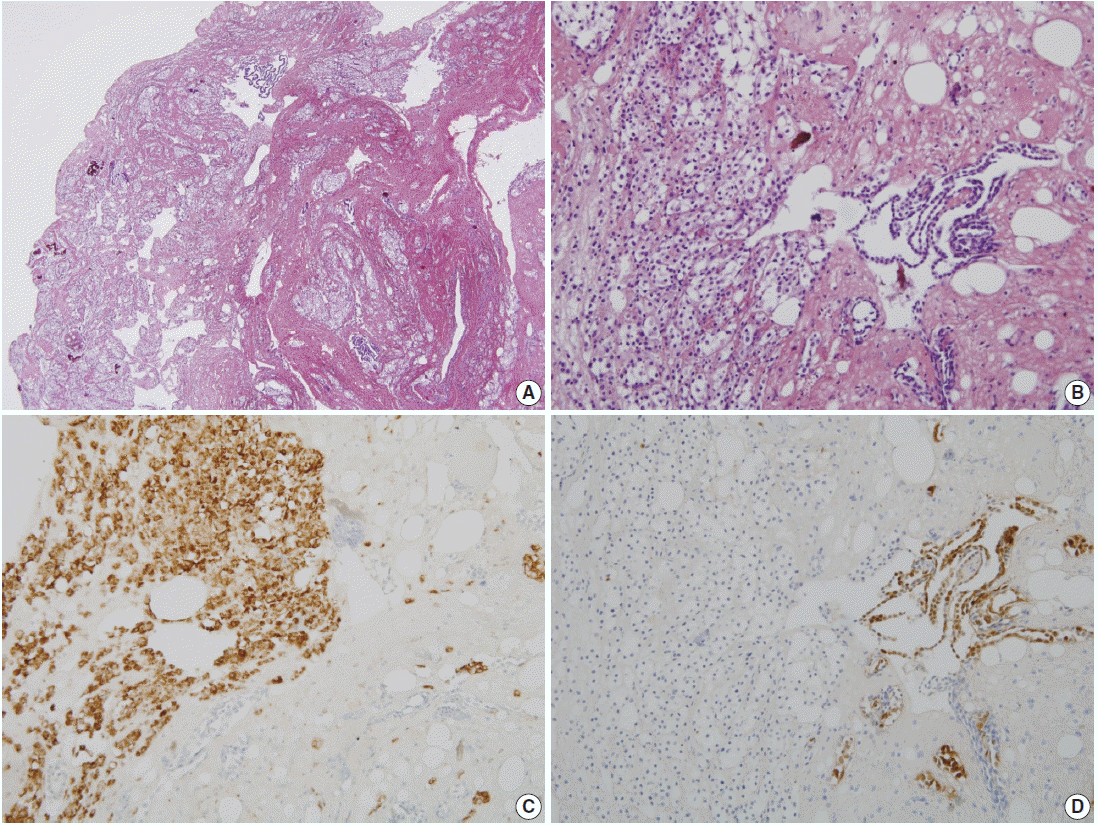
- The patient was a 38-year-old woman complaining of abdominal discomfort and infertility without previous pregnancy history. A 8.3×5-cm-sized intramural type myoma was found on gynecologic sonography. There was no medical history of previous abdominal or pelvic surgery. During laparoscopic myomectomy, a left ovarian cyst (2.6×1.6 cm in size), a bladder peritoneal mass (1.6×1 cm in size), and a small nodule in cul-de-sac cavity were incidentally obtained. The pathologic diagnosis of left ovary cyst and bladder peritoneal mass was endometriosis. Gross examination of the mass in cul-de-sac cavity showed a grayish white and solid nodule, measuring 0.8×0.5 cm in size. Microscopically, two populations of cells were identified. The majority of cells showed nodular clusters of round to polygonal cells with moderate amount of pale to pink granular cytoplasm and ovoid or grooved nuclei. The other cell type was low cuboidal cells of stripped arrangement, which were entrapped in nodular clusters (Fig. 1A, B). Immunohistochemically, the round to polygonal cells in nodular lesions showed positivity for the histiocytic marker (CD68) (Fig. 1C), whereas negative for neuroendocrine markers, such as CD56, synaptophysin, and chromogranin. The low cuboidal cells were immunoreactive for pancytokeratin and the mesothelial markers, such as WT-1 and calretinin (Fig. 1D). These histopathologic features are consistent with NHMH.
CASE REPORT
- NHMH is a benign lesion, which is characterized by non-neoplastic proliferation of histiocytes and mesothelial cells. This lesion is very rare and only 20 cases have been reported in the literature (Table 1). Although patients with these tumors range in age from 2 to 80 years, approximately 70% of the patients are over 40 years old with a mean age of 50.56. This lesion exhibits a slightly higher predilection for female in a ratio of 1.33 to 1. NHMHs are mostly incidental findings and occur at the serosal lining. The lung and pleura are the most frequently affected sites and account for 50% of the NHMH cases. The inguinal region, urinary bladder, and pelvis are less commonly affected sites.
- Pathologically, the diagnosis of NHMH is made by identifying nodular proliferation of both histiocytic and mesothelial components supported by immunohistochemistry. The histiocytes are arranged in solid sheets or nests with a mixture of fibrin materials, and they are immunoreactive against CD68. The mesothelial component, which is arranged in a glandular- or striplike structure, is positive for mesothelial markers such as calretinin and WT-1. The nuclear atypia is typically absent.
- Mesothelial/monocytic incidental cardiac excrescence (MICE), a tumour-like lesion similar to NHMH, is also predominantly composed of histiocytes and scattered mesothelial cells [10]. It can occur incidentally in pericardium, heart chamber and valve, and it has often been found during cardiac valve replacement surgery. MICE are also considered as a reactive condition. Therefore, NHMH and MICE may belong to the same disease entity.
- NHMH is considered a reactive lesion which results from irritation by inflammation, mechanical trauma, or adjacent tumors [2,6]. It has been postulated that the nodular aggregation of these reactive cells is mediated by adhesion molecules, such as CD34 [5]. Although our case did not have mechanical irritation such as previous surgery or procedure, the patient had a large intramural leiomyoma and endometriosis as accompanying diseases, supporting the above mentioned pathogenesis.
- Although benign-looking cytological findings support that the NHMH represents benign reactive proliferation of histiocytes and mesothelial cells, the lesion can be confused with other mesothelial lesions and neoplasms such as low-grade neuroendocrine tumors, mesothelioma, granulosa cell tumor, Langerhans cell histiocytosis, metastatic carcinoma, seminoma and malignant lymphoma. Therefore, immunohistochemical studies as well as histologic examination with proper clinical history provide clues to obtain an accurate diagnosis. In the present case, the solid pattern of histiocytic proliferation with a delicate capillary network (Fig. 1B) was morphologically similar to the histologic finding of a metastatic renal cell carcinoma and paragangioma, which were excluded by immunohistochemistry.
- In conclusion, it is important that pathologists should be aware of this entity and correlate clinically, histologically, and immunohistochemically to make a correct diagnosis.
DISCUSSION
Fig. 1.Pathologic findings. (A) Incidentally obtained pelvic nodule reveals a nodular histiocytic and mesothelial hyperplasia, which is a nodular proliferation of two different cell types, histiocytes and mesothelial cells. (B) High power view shows collection of larger histiocytes, which is admixed with fibrin materials, and strips of smaller mesothelial cells. (C) The histiocytes are immunoreactive for CD68. (D) The mesothelial cells are positive for calretinin.
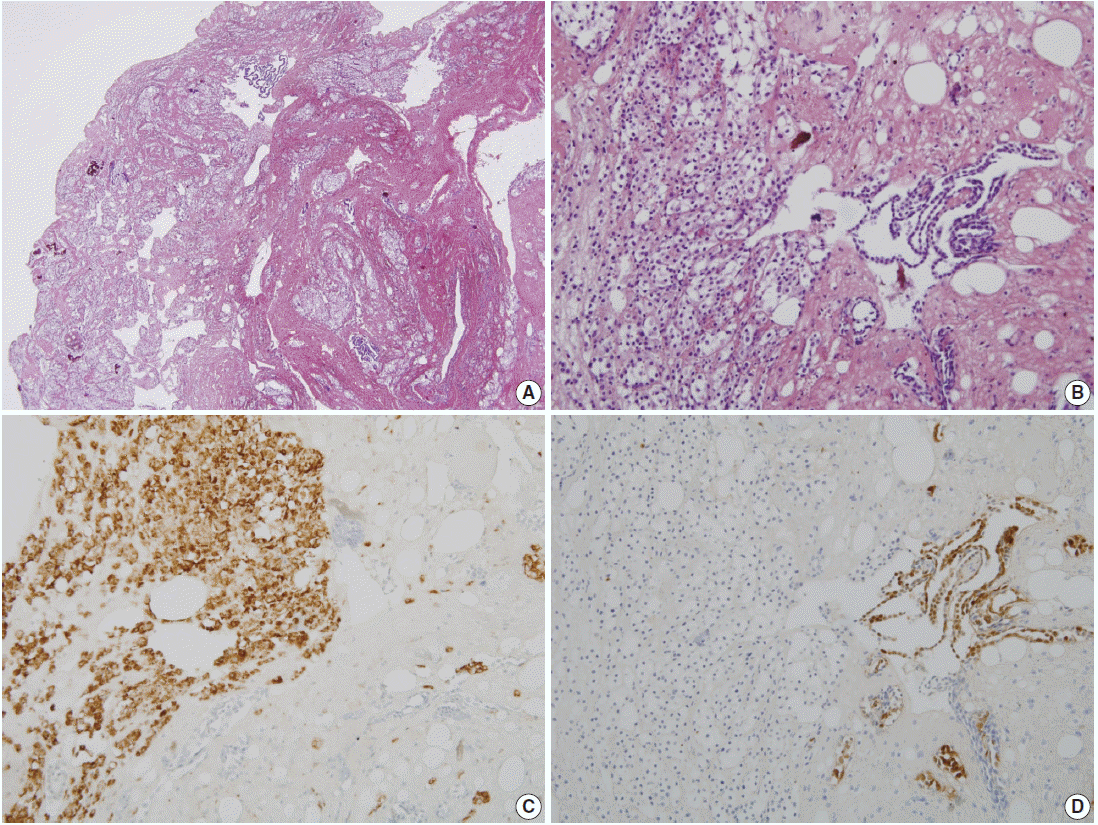

Table 1.Clinical features and pathologicdifferential diagnosis based on previously reported and present cases
| No. | Age (yr)/Sex | Site | Underlying condition | Differential diagnosis | Reference |
|---|---|---|---|---|---|
| 1 | 57/M | Lung (LLL) | Old TBC lesions | Neuroendocrine neoplasm | Chan et al. [2] |
| 2 | 51/F | Lung (RLL) | Weil-Felix agglutination test (+), possible rickettsial pneumonia | Neuroendocrine neoplasm, ectopic meningioma | Chan et al. [2] |
| 3 | 23/F | Lleura | Metastatic sarcoma to lung | Metastatic sarcoma | Ordonez et al. [3] |
| 4 | 78/F | Pleura | Unknown | Metastatic adenocarcinoma, epithelioid hemangioendothelioma | Ordonez et al. [3] |
| 5 | 80/F | Pleura | Unknown | Malignant mesothelioma, metastatic carcinoma, ectopic meningioma, paraganglioma | Choi and Song [4] |
| 6 | Elderly/M | Pleura | Carcinoma in the lung | Primary or metastatic carcinoma, carcinoid tumor, mesothelioma, histiocytosis X | Chikkamuniyappa et al. [6] |
| 7 | 53/F | Pleura | Multiple bilateral lung nodules | Primary or metastatic carcinoma, carcinoid tumor, mesothelioma, histiocytosis X | Chikkamuniyappa et al. [6] |
| 8 | 79/M | Lung | Past history of ischemic cardiac disease | Malignancy | Rossi et al. [8] |
| 9 | 76/F | Lung (RLL) | Bilateral pneumonia (history of chronic l ymphocytic leukemia) | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 10 | 40/F | Lung (LUL) | Consolidation (lung), scleroderma | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 11 | 44/F | Lung (RLL) | History of pancreatic carcinoma, history of chemopneumonitis | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 12 | 78/F | Lung (LUL) | Lung mass | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 13 | 46/M | Lung (LLL) | Bilateral infiltrates (lung) (s/p heart transplant) | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 14 | 62/M | Lung (LLL) | Bilateral infiltrates (lung) (s/p heart transplant) | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 15 | 2/M | Inguinal | Strangulated hernia | - | Chan et al. [2] |
| 16 | 71/M | Inguinal | Relapsed inguinal hernia | - | Suarez-Vilela and Izquierdo-Garcia [5] |
| 17 | 5/M | Inguinal | - | Neuroendocrine tumors, Langerhans cell histiocytosis, seminoma, mesothelioma | Cai et al. [9] |
| 18 | 36/F | Pelvis | Infertility | Well-differentiated adenocarcinoma, leukemia/lymphoma | Chikkamuniyappa et al. [6] |
| 19 | 37/F | Pelvis | Endometriosis | Well-differentiated adenocarcinoma, leukemia/lymphoma | Chikkamuniyappa et al. [6] |
| 20 | 74/M | Bladder | Noninvasive papillary transitional cell carcinoma | Invasive transitional cell carcinoma into the lamina propria | Ordonez et al. [3] |
| Present case | 38/F | Pelvis | Uterine leiomyoma endometriosis | Metastatic renal cell carcinoma, paraganglioma |
- 1. Rosai J, Dehner LP. Nodular mesothelial hyperplasia in hernia sacs: a benign reactive condition simulating a neoplastic process. Cancer 1975; 35: 165-75. ArticlePubMed
- 2. Chan JK, Loo KT, Yau BK, Lam SY. Nodular histiocytic/mesothelial hyperplasia: a lesion potentially mistaken for a neoplasm in transbronchial biopsy. Am J Surg Pathol 1997; 21: 658-63. ArticlePubMed
- 3. Ordonez NG, Ro JY, Ayala AG. Lesions described as nodular mesothelial hyperplasia are primarily composed of histiocytes. Am J Surg Pathol 1998; 22: 285-92. ArticlePubMed
- 4. Choi YL, Song SY. Cytologic clue of so-called nodular histiocytic hyperplasia of the pleura. Diagn Cytopathol 2001; 24: 256-9. ArticlePubMed
- 5. Suarez-Vilela D, Izquierdo-Garcia FM. Nodular histiocytic/mesothelial hyperplasia: a process mediated by adhesion molecules? Histopathology 2002; 40: 299-300. ArticlePubMedPDF
- 6. Chikkamuniyappa S, Herrick J, Jagirdar JS. Nodular histiocytic/mesothelial hyperplasia: a potential pitfall. Ann Diagn Pathol 2004; 8: 115-20. ArticlePubMed
- 7. Bejarano PA, Garcia MT, Ganjei-Azar P. Mesothelial cells in transbronchial biopsies: a rare complication with a potential for a diagnostic pitfall. Am J Surg Pathol 2007; 31: 914-8. PubMed
- 8. Rossi G, Cavazza A, Guicciardi N, Marchioni A. Nodular histiocytic/mesothelial hyperplasia on transthoracic biopsy: another source of potential pitfall in a lesion frequently present in spontaneous pneumothorax. Histopathology 2008; 52: 250-2. ArticlePubMed
- 9. Cai Z, Xie Q, Wang X, Guo B, Wang X, Wang K. Nodular histiocytic/mesothelial hyperplasia: a clinicopathologic analysis of 7 cases. Zhonghua Bing Li Xue Za Zhi 2014; 43: 256-9. PubMed
- 10. Jiao N, Zhang W, Wang W, et al. Mesothelial/monocytic incidental cardiac excrescence: a case report and review of literature. Int J Clin Exp Pathol 2014; 7: 6219-24. PubMedPMC
REFERENCES
Figure & Data
References
Citations
Citations to this article as recorded by 

- Nodular Histiocytic Aggregates of the Greater Omentum Mimicking Peritoneal Carcinomatosis on Imaging
Nada Elmukhtar, Jawad Al-Khalaf, Ali Alsehaiw, Lobaina Abozaid
Cureus.2024;[Epub] CrossRef - Papillary Histiocytic and Mesothelial Hyperplasia of the Ovary Related to a Huge Uterus: A Case Report
Kyeoungseo Park, Kyeongmin Kim, Yon Hee Kim, Yoon Mee Jeen, Dong Won Kim, So-Young Jin, In Ho Choi
Soonchunhyang Medical Science.2023; 29(1): 10. CrossRef - Primary umbilical endometriosis coexisiting with multiple uterine fibroids
S. G. Mba, C. A. Omeke, J. T. Enebe, O. C. Anyanwu
International Journal of Surgery Case Reports.2022; 94(C): 107129. CrossRef - Cytomorphology of nodular histiocytic/mesothelial hyperplasia
Xiaobing Jin, Xin Jing, Jonathan B. McHugh, Liron Pantanowitz
Diagnostic Cytopathology.2022;[Epub] CrossRef - Pleural nodular mesothelial/histiocytic hyperplasia associated with syphilis
Kyra B. Berg, Peter D. Liebling, Melanie J. Kubik, Richard Attanoos, Francoise Galateau-Salle, Victor Roggli, Mark Wick, Andrew M. Churg
Human Pathology: Case Reports.2018; 13: 18. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure
Pelvic Nodular Histiocytic and Mesothelial Hyperplasia in a Patient with Endometriosis and Uterine Leiomyoma

Fig. 1. Pathologic findings. (A) Incidentally obtained pelvic nodule reveals a nodular histiocytic and mesothelial hyperplasia, which is a nodular proliferation of two different cell types, histiocytes and mesothelial cells. (B) High power view shows collection of larger histiocytes, which is admixed with fibrin materials, and strips of smaller mesothelial cells. (C) The histiocytes are immunoreactive for CD68. (D) The mesothelial cells are positive for calretinin.
Fig. 1.
Pelvic Nodular Histiocytic and Mesothelial Hyperplasia in a Patient with Endometriosis and Uterine Leiomyoma
| No. | Age (yr)/Sex | Site | Underlying condition | Differential diagnosis | Reference |
|---|---|---|---|---|---|
| 1 | 57/M | Lung (LLL) | Old TBC lesions | Neuroendocrine neoplasm | Chan et al. [2] |
| 2 | 51/F | Lung (RLL) | Weil-Felix agglutination test (+), possible rickettsial pneumonia | Neuroendocrine neoplasm, ectopic meningioma | Chan et al. [2] |
| 3 | 23/F | Lleura | Metastatic sarcoma to lung | Metastatic sarcoma | Ordonez et al. [3] |
| 4 | 78/F | Pleura | Unknown | Metastatic adenocarcinoma, epithelioid hemangioendothelioma | Ordonez et al. [3] |
| 5 | 80/F | Pleura | Unknown | Malignant mesothelioma, metastatic carcinoma, ectopic meningioma, paraganglioma | Choi and Song [4] |
| 6 | Elderly/M | Pleura | Carcinoma in the lung | Primary or metastatic carcinoma, carcinoid tumor, mesothelioma, histiocytosis X | Chikkamuniyappa et al. [6] |
| 7 | 53/F | Pleura | Multiple bilateral lung nodules | Primary or metastatic carcinoma, carcinoid tumor, mesothelioma, histiocytosis X | Chikkamuniyappa et al. [6] |
| 8 | 79/M | Lung | Past history of ischemic cardiac disease | Malignancy | Rossi et al. [8] |
| 9 | 76/F | Lung (RLL) | Bilateral pneumonia (history of chronic l ymphocytic leukemia) | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 10 | 40/F | Lung (LUL) | Consolidation (lung), scleroderma | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 11 | 44/F | Lung (RLL) | History of pancreatic carcinoma, history of chemopneumonitis | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 12 | 78/F | Lung (LUL) | Lung mass | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 13 | 46/M | Lung (LLL) | Bilateral infiltrates (lung) (s/p heart transplant) | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 14 | 62/M | Lung (LLL) | Bilateral infiltrates (lung) (s/p heart transplant) | Non-small cell carcinoma, neuroendocrine tumors, ectopic meningioma | Bejarano et al. [7] |
| 15 | 2/M | Inguinal | Strangulated hernia | - | Chan et al. [2] |
| 16 | 71/M | Inguinal | Relapsed inguinal hernia | - | Suarez-Vilela and Izquierdo-Garcia [5] |
| 17 | 5/M | Inguinal | - | Neuroendocrine tumors, Langerhans cell histiocytosis, seminoma, mesothelioma | Cai et al. [9] |
| 18 | 36/F | Pelvis | Infertility | Well-differentiated adenocarcinoma, leukemia/lymphoma | Chikkamuniyappa et al. [6] |
| 19 | 37/F | Pelvis | Endometriosis | Well-differentiated adenocarcinoma, leukemia/lymphoma | Chikkamuniyappa et al. [6] |
| 20 | 74/M | Bladder | Noninvasive papillary transitional cell carcinoma | Invasive transitional cell carcinoma into the lamina propria | Ordonez et al. [3] |
| Present case | 38/F | Pelvis | Uterine leiomyoma endometriosis | Metastatic renal cell carcinoma, paraganglioma |
Table 1. Clinical features and pathologicdifferential diagnosis based on previously reported and present cases
M, male; LLL, left lower lobe; TBC, tuberculosis; RLL, right lower lobe; LUL, left upper lobe.

 E-submission
E-submission