Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 51(1); 2017 > Article
-
Original Article
PD-L1 Expression and Combined Status of PD-L1/PD-1–Positive Tumor Infiltrating Mononuclear Cell Density Predict Prognosis in Glioblastoma Patients - Jiheun Han, Yongkil Hong1, Youn Soo Lee
-
Journal of Pathology and Translational Medicine 2017;51(1):40-48.
DOI: https://doi.org/10.4132/jptm.2016.08.31
Published online: December 15, 2016
Department of Hospital Pathology, Seoul St. Mary’s Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea
1Department of Neurosurgery, Seoul St. Mary’s Hospital, College of Medicine, The Catholic University of Korea, Seoul, Korea
- Corresponding Author: Youn Soo Lee, MD, PhD Department of Hospital Pathology, Seoul St. Mary’s Hospital, College of Medicine, The Catholic University of Korea, 222 Banpo-daero, Seocho-gu, Seoul 06591, Korea Tel: +82-2-2258-1613 Fax: +82-2-2258-1628 E-mail: lys9908@catholic.ac.kr
© 2017 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
Background
- Programmed death ligand 1 (PD-L1) in tumor cells is known to promote immune escape of cancer by interacting with programmed cell death 1 (PD-1) in tumor infiltrating immune cells. Immunotherapy targeting these molecules is emerging as a new strategy for the treatment of glioblastoma (GBM). Understanding the relationship between the PD-L1/PD-1 axis and prognosis in GBM patients may be helpful to predict the effects of immunotherapy.
-
Methods
- PD-L1 expression and PD-1–positive tumor infiltrating mononuclear cell (PD-1+tumor infiltrating mononuclear cell [TIMC]) density were evaluated using tissue microarray containing 54 GBM cases by immunohistochemical analysis; the associations with patient clinical outcomes were evaluated.
-
Results
- PD-L1 expression and high PD-1+TIMC density were observed in 31.5% and 50% of GBM cases, respectively. High expression of PD-L1 in tumor cells was an independent and significant predictive factor for worse overall survival (OS; hazard ratio, 4.958; p = .007) but was not a significant factor in disease-free survival (DFS). PD-1+TIMC density was not correlated with OS or DFS. When patients were classified based on PD-1 expression and PD-1+TIMC density, patients with PD-L1+/PD-1+TIMC low status had the shortest OS (13 months, p = .009) and DFS (7 months, p = .053).
-
Conclusions
- PD-L1 expression in GBM was an independent prognostic factor for poor OS. In addition, combined status of PD-L1 expression and PD-1+TIMC density also predicted patient outcomes, suggesting that the therapeutic role of the PD-1/PD-L1 axis should be considered in the context of GBM immunity.
- Patients
- We retrospectively identified GBM patients who were diagnosed and treated in Seoul St. Mary’s Hospital, College of Medicine, The Catholic University of Korea (Seoul, Korea), between 2004 and 2012. Patient clinicopathologic and clinical follow-up data were collected from the medical records. Histologic diagnosis of glioblastoma was performed according to the current World Health Organization (WHO) classification, fourth edition [18]. The ethics committee of Catholic University granted approval for this study (IRB No. KC16RISI0370).
- Construction of tissue microarray
- All tumor tissues were obtained at the time of the first surgery after diagnosis of GBM. A representative tumor area from each case was selected and marked on hematoxylin and eosin (H&E)-stained slides. Formalin-fixed and paraffin-embedded tissue blocks and the corresponding H&E-stained slides were overlaid for tissue microarray (TMA) sampling. A cylindrical core (2 mm in diameter) was obtained for each case. Sectioning of microarray blocks produced 4-µm thick sections.
- Immunohistochemistry
- Microslide tissue sections were deparaffinized with xylene, hydrated using a diluted alcohol series, and immersed in 0.3% H2O2 in methanol to extinguish endogenous peroxidase activity. Sections were then microwaved for 15 minutes in 10 mM citrate buffer (pH 6.0) for antigen retrieval. Each section was blocked with 4% bovine serum albumin in phosphate buffered saline with 0.1% Tween 20 (PBST) for 30 minutes to reduce non-specific staining. Sections were incubated with anti–PD-L1 (1:100, Cell Marque, Rocklin, CA, USA) or anti–PD-1 (1:100, Ventana, Tucson, AZ, USA) antibodies in PBST containing 3 mg/mL goat globulin (Sigma-Aldrich, St. Louis, MO, USA) for 60 minutes at room temperature, followed by three successive washes with a buffer. The sections were then incubated with an antimouse/rabbit antibody (Envision plus, Dako, Carpinteria, CA, USA) for 30 minutes at room temperature. The chromogen used was 3,3'-diaminobenzidine (Dako). The sections were counterstained with Meyer’s hematoxylin. For positive controls, sections of human placenta and tonsil tissue were included in each staining run. Omission of the primary antibody for placenta and tonsil tissue sections was used as a negative control.
- Immunohistochemical analysis
- Two experienced pathologists (Y.S.L. and J.H) performed immunohistochemical analysis for PD-L1 and PD-1 by microscopic observation of the stained TMA slides. Cases were considered PD-L1+ if membranous staining of tumor cells was detected in at least 5% of the cells, irrespective of staining intensity. The cut-off threshold of PD-L1 expression was determined by receiver operating characteristic analysis of the survival rate.
- PD-1 staining in TIMCs was assessed by identification of lymphocytes and macrophages on the basis of morphologic features. All TIMCs with membranous PD-1 expression of moderate to high intensity were manually counted in an entire area for each TMA core. The number of PD-1+TIMCs was divided by the total area of the TMA core (3.14 mm2) to obtain the number of PD-1+TIMCs per unit area (/mm2), the median value of which was used as a cut-off to define low versus high density.
- Statistical analysis
- Data were analyzed using the SPSS 21.0 statistical software package (IBM Corp., Armonk, NY, USA). Differences in patient characteristics between positive and negative PD-L1 expression or high and low density of PD-1+TIMCs were analyzed using chi-square tests, Fisher exact tests, and Student’s t-tests. Comparative analysis of PD-L1 expression and the number of PD-1+ TIMCs was performed using Mann-Whitney tests. Survival time curves were drawn using the Kaplan-Meier method and a log-rank test was used to assess the significance of differences in survival. Survival time included overall survival (OS; the length of time from the date of surgery or biopsy to the date of death from any cause, or to the last follow-up date if the patient is alive) and disease-free survival (DFS; the length of time from the date of surgery or biopsy to recurrence, progress or death from any cause). Univariate and multivariate analyses using the Cox proportional hazard model were performed to identify factors influencing OS and DFS. A step-down procedure was selected for multivariate analysis. In all statistical analyses, a two-tailed p-value less than .05 was considered to indicate a statistically significant difference.
MATERIALS AND METHODS
- Patient characteristics
- The clinical characteristics of the 54 patients are summarized in Table 1. The mean patient age at diagnosis was 57.2 years, with a range of 31 to 85 years. The study group consisted of 26 males (48.1%) and 28 females (51.9%). Eleven patients (20.4%) had secondary GBM that developed from anaplastic astrocytoma and oligodendroglioma. Forty patients (74.1%) underwent total resection, 43 (79.6%) were treated with adjuvant radiotherapy plus concurrent temozolomide, and nine (16.7%) were treated with radiotherapy or temozolomide alone, based on performance status. Thirty-two patients (59.3%) had a single lesion and 22 (40.7%) had multifocal or multicentric lesions. Thirty-six patients (66.7%) were alive at the last follow-up and 40 patients (74.1%) experienced a progression or recurrence. Mean OS and DFS were 17.57 and 12.13 months, respectively.
- PD-L1 expression and PD-1+TIMC density in GBM
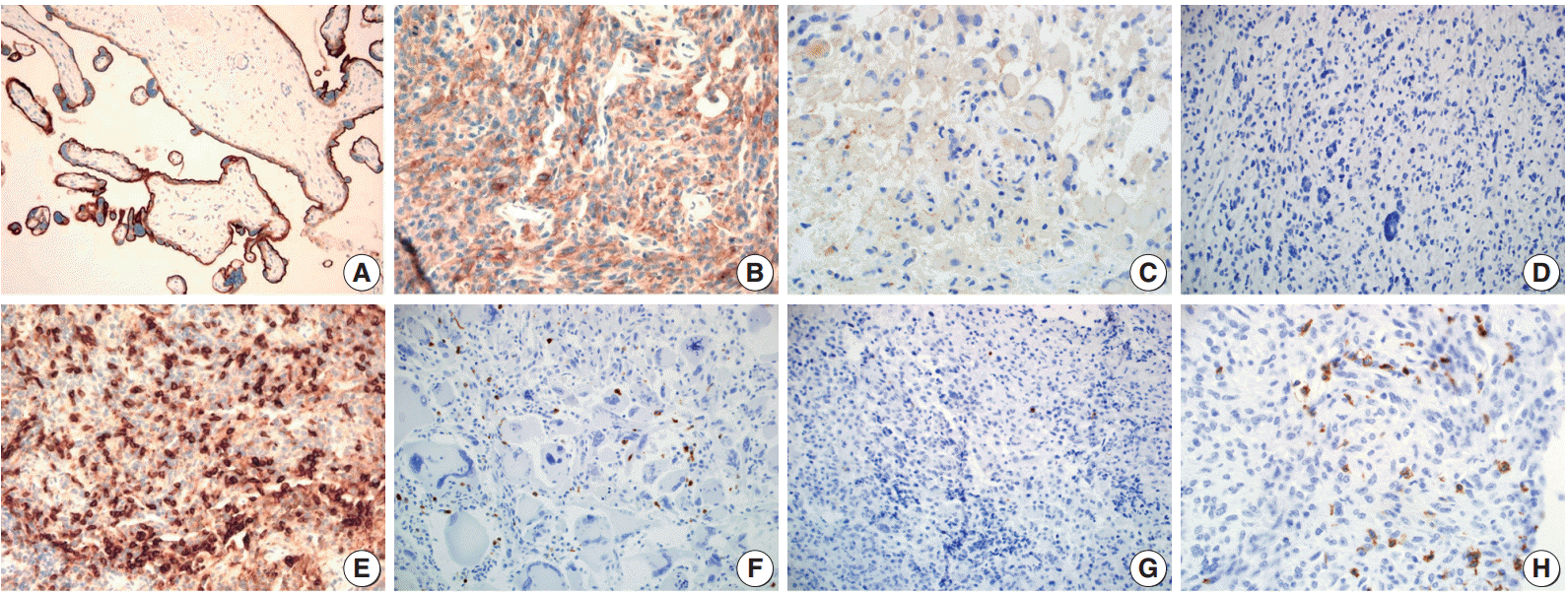
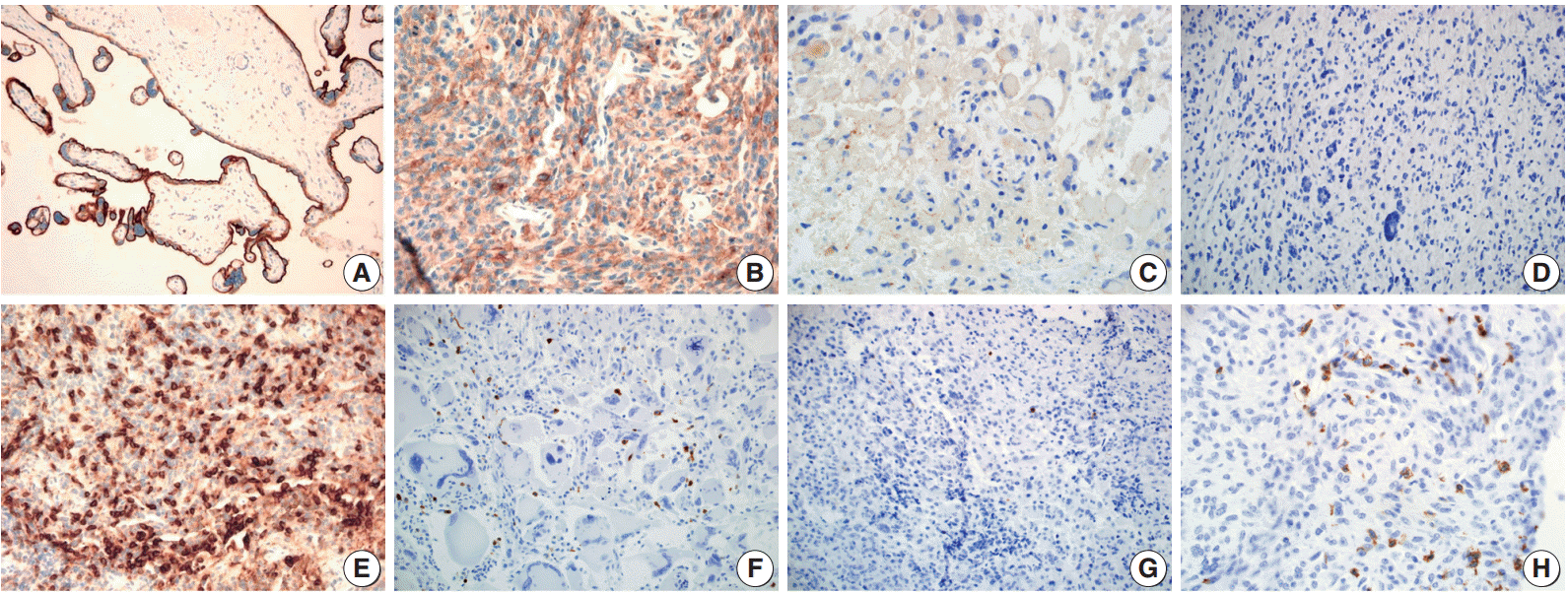
- PD-L1 staining in tumor cells was mostly of weak to moderate intensity with a membranous and cytoplasmic pattern (Fig. 1B, C). In most of the cases, PD-L1 stained only tumor cells. However, in two cases (one case was PD-L1 positive, the other was not) a few dispersed TIMCs were stained with PD-L1 in their cytoplasm or membrane. In total, 17 patients (31.5%) were positive for PD-L1 expression in tumor cells.
- The median PD-1+TIMC density in GBM was 1.75/mm2 (range, 0 to 36.6/mm2), and 27 patients (50%) were classified as PD-1+TIMC high density (Fig. 1F, G). Most of the PD-1+ TIMC were lymphocytes with small round condensed nuclei and rims of cytoplasm. Occasionally, the cells had elongated or kidney shaped nuclei with a scant to moderate amount of cytoplasm (which were considered to be macrophages) that were stained with PD-1 (Fig. 1H).
- No significant relationship between PD-L1 expression and PD-1+TIMC density was detected.
- Correlations between PD-L1 expression and PD-1+TIMC density and GBM patient characteristics
- Patient characteristics and their associations with PD-L1 expression and PD-1+TIMC density are summarized in Table 2. PD-L1 expression was significantly more frequent in patients who had died by the last follow up than in survivors (p=.038). No significant correlations were observed between PD-1+ TIMC density and patient characteristics.
- Prognostic implication of PD-L1 expression and PD-1+TIMC density for GBM
- Univariate analysis revealed that PD-L1 expression was significantly associated with poor OS (p=.024; hazard ratio [HR], 3.058; 95% confidence interval [CI], 1.16 to 8.06) (Table 3), whereas none of the other factors, including PD-1+TIMC density, were significantly associated with OS. Multivariate analyses demonstrated that PD-L1 expression was an independent and significant predictive factor for worse OS (p=.007; HR, 4.958; 95% CI, 1.557 to 15.79) (Table 3).
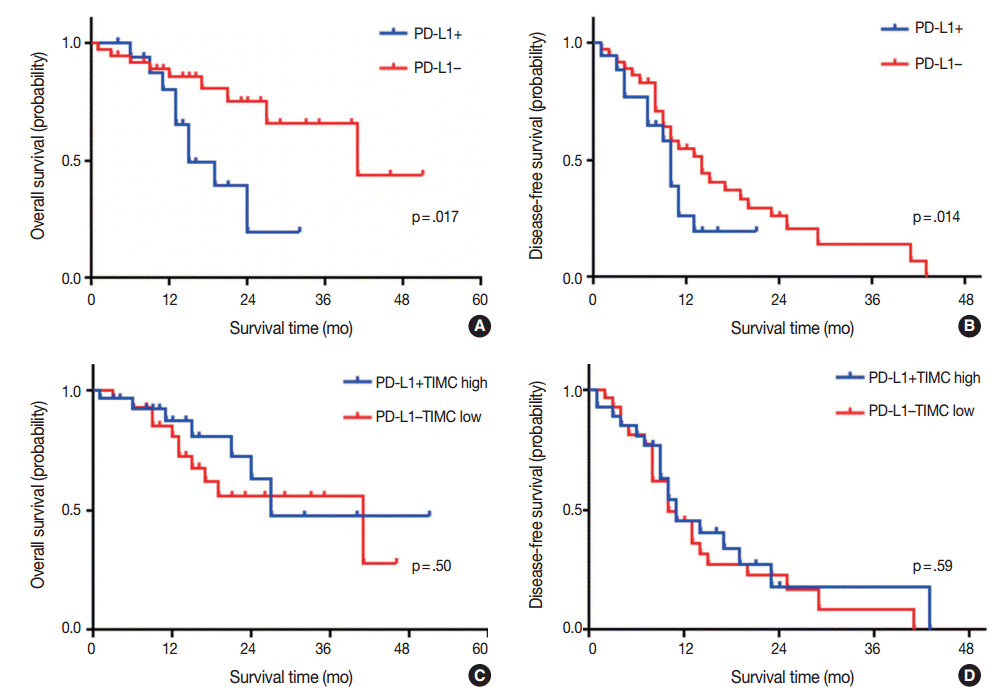
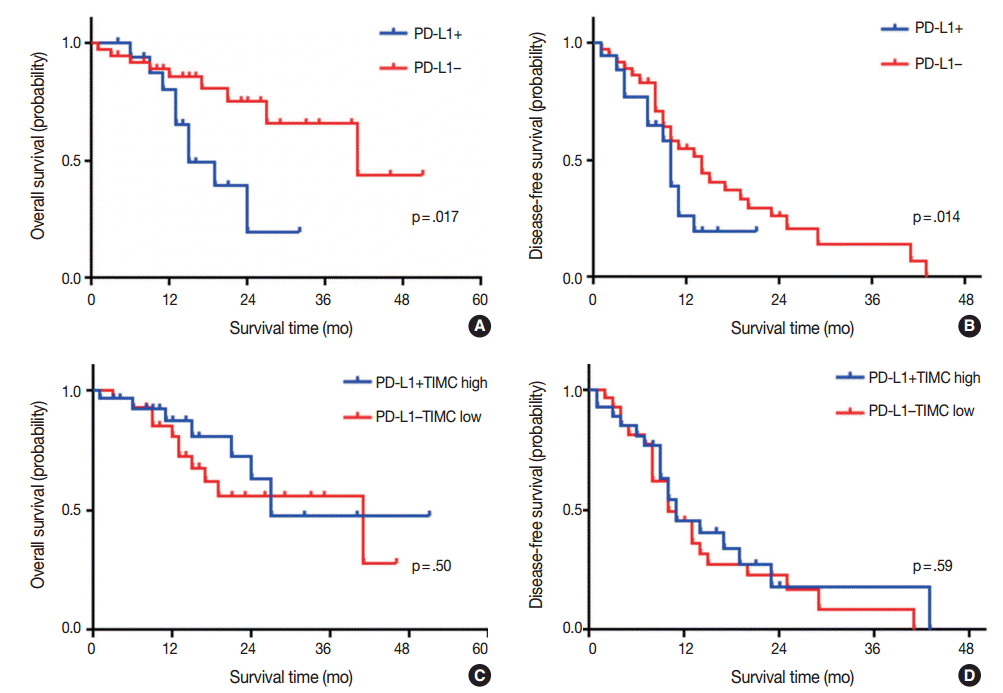
- Kaplan-Meier survival analysis revealed that patients with PD-L1 expression exhibited significantly shorter OS (median OS, 15 months vs 41 months, p=.017) (Fig. 2A), but that there was no significant difference in DFS (median DFS, 10 months vs 14 months; p=.14) (Fig. 2B). There were no significant differences in OS or DFS according to PD-1+TIMC density (Fig. 2C, D).
- Classification of patients based on PD-L1 expression and PD-1+TIMC density
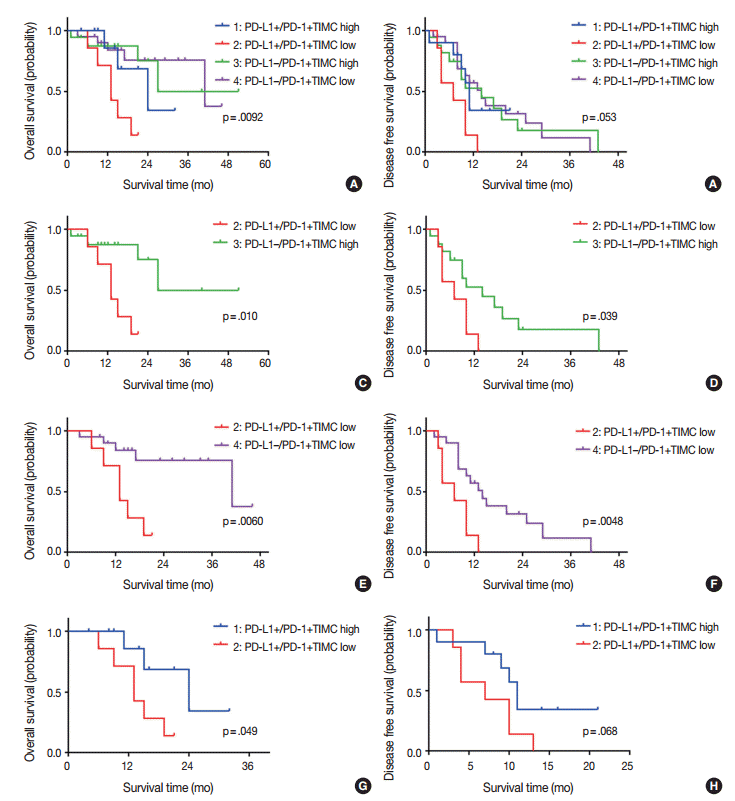
- We divided patients into four groups according to their PD-L1 expression status and PD-1+TIMC density: PD-L1+/PD-1+ TIMC high (group 1; 10 patients, 18.5%), PD-L1+/PD-1+ TIMC low (group 2; 7 patients, 13%), PD-L1–/PD-1+TIMC high (group 3; 17 patients, 31.5%), and PD-L1–/PD-1+TIMC low (group 4; 20 patients, 37%). The median OS was 24 months in group 1, 13 months in group 2, 27 months in group 3, and 41 months in group 4 (p=.0092) (Fig. 3A). The median DFS was 11 months in group 1, 7 months in group 2, and 24 months in groups 3 and 4 (p=.053) (Fig. 3B). Patients in group 2 had significantly worse rates of OS (Fig. 3C, E) and DFS (Fig. 3D, F) than those in groups 3 and 4. They also tended to have shorter OS (p=.049) (Fig. 3G) and DFS (p=.068) (Fig. 3H) than those in group 1.
- Histologically, the GBM of group 2 tended to show marked tumor cellularity, low density of TIMCs, and a high Ki-67 index (≥20%). Patients in group 2 were younger at the age of diagnosis than the other groups, although this difference was not statistically significant (Table 4).
RESULTS
- The expression rate of PD-L1 in glioblastoma patients in our study was 31.5%, which is comparable to that of other solid tumors, such as ~30% for melanoma [19] and ~36% for non-small cell lung cancer [20]. In recent studies, 38.3% of GBM [8] and 37.6% for newly diagnosed GBM [7] had at least 5% PD-L1 expression.
- PD-L1 expression has been observed, not only in tumor cells, but also in non-cancerous interstitial cells [21] and stromal lymphocytes [22]. Nduom et al. [8] also observed that lymphocytes consisted of nearly 30% PD-L1 positive cells in GBM. However, in our study, PD-L1–positive lymphocytes were found in only two out of 54 cases and their proportions were not significant. These differences may result from the use of different antibodies, differences in counting or detection methods, or different definitions for positivity. In addition, GBM is known to create an immunosuppressive microenvironment, resulting in sparse TILs in GBM relative to other solid tumors, which might affect the proportion of PD-L1 positive lymphocytes.
- In the present study, patients with PD-L1 expression showed significantly poorer OS. However, the relationship between PD-L1 expression and prognosis in patients with GBM remains unclear. Recent studies have evaluated the prognostic implications of PD-L1 expression in GBM [7,8] and glioma [23] with inconsistent findings. Although the precise mechanism by which intratumoral PD-L1 negatively affects patient prognosis is yet to be determined, PD-L1 has been expressed in different cancer types, including kidney, liver, ovarian, pancreatic, lung, and gastric cancer, and PD-L1 expression by tumor cells has been reported to strongly correlate with a poor prognosis [24-29].
- Traditionally, the central nervous system has been presumed to be an immune privileged organ, primarily due to an intact blood-brain barrier (BBB). However, in GBM, the integrity of the BBB is compromised, enabling activated macrophages and lymphocytes to migrate across the BBB into the brain parenchyma [30]. Inflammatory infiltrates in GBM are relatively sparse; in the present study, the median density of PD-1+TIMCs was 1.75/mm2, which is much lower than in other solid tumors, such as lung cancer (33.4 PD-1+TILs/mm2) [31]. Presurgical corticosteroid treatment may affect the number of TIMCs, although Berghoff et al. [32] found that corticosteroids did not affect the amount of TILs in melanoma brain metastases. It is known that GBM creates an immunosuppressive microenvironment by producing immunosuppressive cytokines, such as transforming growth factor β, prostaglandin-E, indoleamine 2,3-dioxygenase, interleukin 10, and STAT3 [33]. In addition, ineffective presentation of tumor antigens by APCs or recruitment of immunosuppressive cells, such as regulatory T cells (Treg) or myeloid-derived suppressor cells, is known to contribute to an immunosuppressive condition [33]. The scarcity of PD-1+ infiltrating immune cells, targets of anti–PD-1 therapy, might imply reduced efficacy of the treatment.
- No relationship between PD-1 expression and clinical outcomes was observed in the present study, although previous studies have shown inconsistent results [12,34]. In a subgroup analysis dividing patients into four groups according to PD-L1 expression and PD-1+TIMC density, group 2 (PD-L1+/PD-1+TIMC low) had a significantly worse OS than the other three groups. This finding was in accordance with the poor prognostic effect of PD-L1 expression. In addition, the significant difference in OS between groups 1 and 2, both of which were PD-L1 positive, and the similar clinical outcomes of groups 1, 3, and 4, suggest that the prognostic impact of PD-L1 expression on GBM should be evaluated with PD-1+TIMC density. Thus, the combined status of PD-L1 expression with PD-1+TIMC density may more precisely predict clinical outcomes.
- The PD-L1 expression in GBM is mediated by IFN-γ produced in an active immune response to the tumor or a constitutive oncogenic signaling pathway via the loss of PTEN [10]. Harter et al. [35] found a loco-regional overlap between TILs and PD-L1 expression in brain metastasis, suggesting induction of PD-L1 in brain metastasis by anti-tumor immune response. However, we observed that PD-L1–positive GBM tended to have equivocal (group 1) or even lower (group 2) TIMC density than PD-L1–negative groups, indicating that an intrinsic pathway might be associated with PD-L1 overexpression in GBM.
- Our study has several limitations. First, the population enrolled in this study was relatively small, which could limit the statistical estimation. Second, TMA could not fully reflect the heterogeneity of GBM or the focal expression pattern of PD-L1, thus a false-negative evaluation could be possible. Lastly, as our study is retrospective, unknown factors that influence patient clinical outcomes might be present.
- In summary, our study yielded two major findings: first, PD-L1 expression of GBM was an independent prognostic factor associated with poor OS; second, classification of patients based on PD-L1 expression and PD-1+TIMC density also predicts patient survival. Our results suggest that PD-L1 expression might be a useful prognostic factor and should be considered in the context of PD-1+TIMCs. The combination of PD-L1 expression status and PD-1+TIMC density appears to more effectively predict patient prognosis and might be helpful for selection of appropriate candidates for immunotherapy and for evaluating immunotherapeutic efficacy.
DISCUSSION
- 1. Wen PY, Kesari S. Malignant gliomas in adults. N Engl J Med 2008; 359: 492-507. ArticlePubMed
- 2. Weller M, van den Bent M, Hopkins K, et al. EANO guideline for the diagnosis and treatment of anaplastic gliomas and glioblastoma. Lancet Oncol 2014; 15: e395-403. ArticlePubMed
- 3. Thomas RP, Xu LW, Lober RM, Li G, Nagpal S. The incidence and significance of multiple lesions in glioblastoma. J Neurooncol 2013; 112: 91-7. ArticlePubMedPDF
- 4. Chen DS, Mellman I. Oncology meets immunology: the cancer-immunity cycle. Immunity 2013; 39: 1-10. ArticlePubMed
- 5. Ahmadzadeh M, Johnson LA, Heemskerk B, et al. Tumor antigenspecific CD8 T cells infiltrating the tumor express high levels of PD-1 and are functionally impaired. Blood 2009; 114: 1537-44. ArticlePubMedPMCPDF
- 6. Okazaki T, Honjo T. PD-1 and PD-1 ligands: from discovery to clinical application. Int Immunol 2007; 19: 813-24. ArticlePubMed
- 7. Berghoff AS, Kiesel B, Widhalm G, et al. Programmed death ligand 1 expression and tumor-infiltrating lymphocytes in glioblastoma. Neuro Oncol 2015; 17: 1064-75. ArticlePubMed
- 8. Nduom EK, Wei J, Yaghi NK, et al. PD-L1 expression and prognostic impact in glioblastoma. Neuro Oncol 2016; 18: 195-205. ArticlePubMed
- 9. Sanmamed MF, Chen L. Inducible expression of B7-H1 (PD-L1) and its selective role in tumor site immune modulation. Cancer J 2014; 20: 256-61. ArticlePubMedPMC
- 10. Han SJ, Ahn BJ, Waldron JS, et al. Gamma interferon-mediated superinduction of B7-H1 in PTEN-deficient glioblastoma: a paradoxical mechanism of immune evasion. Neuroreport 2009; 20: 1597-602. ArticlePubMed
- 11. Keir ME, Butte MJ, Freeman GJ, Sharpe AH. PD-1 and its ligands in tolerance and immunity. Annu Rev Immunol 2008; 26: 677-704. ArticlePubMedPMC
- 12. Thompson RH, Dong H, Lohse CM, et al. PD-1 is expressed by tumor-infiltrating immune cells and is associated with poor outcome for patients with renal cell carcinoma. Clin Cancer Res 2007; 13: 1757-61. ArticlePubMedPDF
- 13. Muenst S, Soysal SD, Gao F, Obermann EC, Oertli D, Gillanders WE. The presence of programmed death 1 (PD-1)-positive tumorinfiltrating lymphocytes is associated with poor prognosis in human breast cancer. Breast Cancer Res Treat 2013; 139: 667-76. ArticlePubMedPDF
- 14. Webb JR, Milne K, Nelson BH. PD-1 and CD103 are widely coexpressed on prognostically favorable intraepithelial CD8 T cells in human ovarian cancer. Cancer Immunol Res 2015; 3: 926-35. ArticlePubMedPDF
- 15. Taube JM, Anders RA, Young GD, et al. Colocalization of inflammatory response with B7-h1 expression in human melanocytic lesions supports an adaptive resistance mechanism of immune escape. Sci Transl Med 2012; 4: 127ra37.ArticlePubMedPMC
- 16. Teng MW, Ngiow SF, Ribas A, Smyth MJ. Classifying cancers based on T-cell infiltration and PD-L1. Cancer Res 2015; 75: 2139-45. ArticlePubMedPMCPDF
- 17. Dudley ME, Wunderlich JR, Robbins PF, et al. Cancer regression and autoimmunity in patients after clonal repopulation with antitumor lymphocytes. Science 2002; 298: 850-4. PubMedPMC
- 18. Louis DN, Ohgaki H, Wiestler OD, Cavanee WK. WHO classification of tumours of the central nervous system. Lyon: IARC Press, 2007; 4th.
- 19. Weber JS, Kudchadkar RR, Yu B, et al. Safety, efficacy, and biomarkers of nivolumab with vaccine in ipilimumab-refractory or -naive melanoma. J Clin Oncol 2013; 31: 4311-8. ArticlePubMedPMC
- 20. Velcheti V, Schalper KA, Carvajal DE, et al. Programmed death ligand-1 expression in non-small cell lung cancer. Lab Invest 2014; 94: 107-16. ArticlePubMedPDF
- 21. Droeser RA, Hirt C, Viehl CT, et al. Clinical impact of programmed cell death ligand 1 expression in colorectal cancer. Eur J Cancer 2013; 49: 2233-42. ArticlePubMed
- 22. Tokito T, Azuma K, Kawahara A, et al. Predictive relevance of PD-L1 expression combined with CD8+ TIL density in stage III non-small cell lung cancer patients receiving concurrent chemoradiotherapy. Eur J Cancer 2016; 55: 7-14. ArticlePubMed
- 23. Zeng J, Zhang XK, Chen HD, Zhong ZH, Wu QL, Lin SX. Expression of programmed cell death-ligand 1 and its correlation with clinical outcomes in gliomas. Oncotarget 2016; 7: 8944-55. ArticlePubMedPMC
- 24. Hamanishi J, Mandai M, Iwasaki M, et al. Programmed cell death 1 ligand 1 and tumor-infiltrating CD8+ T lymphocytes are prognostic factors of human ovarian cancer. Proc Natl Acad Sci U S A 2007; 104: 3360-5. ArticlePubMedPMC
- 25. Gao Q, Wang XY, Qiu SJ, et al. Overexpression of PD-L1 significantly associates with tumor aggressiveness and postoperative recurrence in human hepatocellular carcinoma. Clin Cancer Res 2009; 15: 971-9. ArticlePubMedPDF
- 26. Wang L, Ma Q, Chen X, Guo K, Li J, Zhang M. Clinical significance of B7-H1 and B7-1 expressions in pancreatic carcinoma. World J Surg 2010; 34: 1059-65. ArticlePubMedPDF
- 27. Thompson RH, Kuntz SM, Leibovich BC, et al. Tumor B7-H1 is associated with poor prognosis in renal cell carcinoma patients with long-term follow-up. Cancer Res 2006; 66: 3381-5. ArticlePubMedPDF
- 28. Wang A, Wang HY, Liu Y, et al. The prognostic value of PD-L1 expression for non-small cell lung cancer patients: a meta-analysis. Eur J Surg Oncol 2015; 41: 450-6. ArticlePubMed
- 29. Liu YX, Wang XS, Wang YF, et al. Prognostic significance of PD-L1 expression in patients with gastric cancer in East Asia: a meta-analysis. Onco Targets Ther 2016; 9: 2649-54. PubMedPMC
- 30. Razavi SM, Lee KE, Jin BE, Aujla PS, Gholamin S, Li G. Immune evasion strategies of glioblastoma. Front Surg 2016; 3: 11.ArticlePubMedPMC
- 31. Kim MY, Koh J, Kim S, Go H, Jeon YK, Chung DH. Clinicopathological analysis of PD-L1 and PD-L2 expression in pulmonary squamous cell carcinoma: comparison with tumor-infiltrating T cells and the status of oncogenic drivers. Lung Cancer 2015; 88: 24-33. ArticlePubMed
- 32. Berghoff AS, Ricken G, Widhalm G, et al. Tumour-infiltrating lymphocytes and expression of programmed death ligand 1 (PD-L1) in melanoma brain metastases. Histopathology 2015; 66: 289-99. ArticlePubMed
- 33. Nduom EK, Weller M, Heimberger AB. Immunosuppressive mechanisms in glioblastoma. Neuro Oncol 2015; 17 Suppl 7: vii9-vii14. PubMed
- 34. Duchnowska R, Peksa R, Radecka B, et al. Immune response in breast cancer brain metastases and their microenvironment: the role of the PD-1/PD-L axis. Breast Cancer Res 2016; 18: 43.PubMedPMCPDF
- 35. Harter PN, Bernatz S, Scholz A, et al. Distribution and prognostic relevance of tumor-infiltrating lymphocytes (TILs) and PD-1/PD-L1 immune checkpoints in human brain metastases. Oncotarget 2015; 6: 40836-49. ArticlePubMedPMC
REFERENCES
Figure & Data
References
Citations

- Dual biomarker role of PD-L1 and LC3B in glioblastoma: prognostic and therapeutic potential
Rana Fathy Torky, Rania Makboul, Dalia M. Badary, Wael M. A. El-Ghani, Ahmed El-Hakeem, Rabab M. H. El Ghorori
Neurosurgical Review.2026;[Epub] CrossRef - Expression features of targets for anti-glioma CAR-T cell immunotherapy
Peng Zhang, Chunzhao Li, Yi Wang, Xiaohan Chi, Tai Sun, Qianhe Zhang, Yang Zhang, Nan Ji
Journal of Neuro-Oncology.2025; 171(1): 179. CrossRef - Expression of Programmed Cell Death-Ligand 1 (PD-L1) in Astrocytic Tumors and Its Correlation With Histopathological Grade and Proliferative Index (Ki-67): A Cross-Sectional Study
Namita Singh, Ranjana Giri, Prita Pradhan, Diptiranjan Satapathy, Ipsita Debata
Cureus.2025;[Epub] CrossRef - Prognostic significance of PD-L1 and CD45RO+ cells in glioblastoma: The modulating role of MMR status
Yousef Mohammadi, Elina Kaviani, Simin Ahmadvand, Amirreza Dehghanian, Abbas Ghaderi
Journal of Neuroimmunology.2025; 406: 578669. CrossRef - PD-L1 Clones and Their Relevance in Glioblastoma, IDH-Wildtype: A Comparative Analysis
Michal Hendrych, Frantisek Vana, Marketa Hermanova, Radek Lakomy, Tomas Kazda, Kvetoslava Matulova, Alena Kopkova, Martina Jelinkova, Radim Jancalek, Martin Smrcka, Vaclav Vybihal, Jiri Sana
Bratislava Medical Journal.2025; 126(9): 2233. CrossRef - Tumor-associated microenvironment, PD-L1 expression and their relationship with immunotherapy in glioblastoma, IDH-wild type: A comprehensive review with emphasis on the implications for neuropathologists
Giuseppe Broggi, Giuseppe Angelico, Jessica Farina, Giordana Tinnirello, Valeria Barresi, Magda Zanelli, Andrea Palicelli, Francesco Certo, Giuseppe Barbagallo, Gaetano Magro, Rosario Caltabiano
Pathology - Research and Practice.2024; 254: 155144. CrossRef - Treatment advances in high-grade gliomas
Xi Chen, Yi Cui, Liqun Zou
Frontiers in Oncology.2024;[Epub] CrossRef - TRP-2 / gp100 DNA vaccine and PD-1 checkpoint blockade combination for the treatment of intracranial tumors
Joshua R. D. Pearson, Carles Puig-Saenz, Jubini E. Thomas, Lydia D. Hardowar, Murrium Ahmad, Louise C. Wainwright, Adam M. McVicar, Victoria A. Brentville, Chris J. Tinsley, A. Graham Pockley, Lindy G. Durrant, Stephanie E. B. McArdle
Cancer Immunology, Immunotherapy.2024;[Epub] CrossRef - Advanced immunotherapies for glioblastoma: tumor neoantigen vaccines in combination with immunomodulators
Berta Segura-Collar, Sara Hiller-Vallina, Olaya de Dios, Marta Caamaño-Moreno, Lucia Mondejar-Ruescas, Juan M. Sepulveda-Sanchez, Ricardo Gargini
Acta Neuropathologica Communications.2023;[Epub] CrossRef - Immunohistochemical Analysis of PD-1 and FOXP3 in Tumor-Infiltrating Lymphocytes in Human Gliomas
Priyanka Kanagaraj, Archana Balasubramanian, Raveena Suresh, Bhargavi Somasundaram, Sandhya Sundaram, Priyathersini Nagarajan
Cureus.2023;[Epub] CrossRef - Expression, prognostic significance and therapeutic implications of PD‐L1 in gliomas
Gayaththri Vimalathas, Bjarne Winther Kristensen
Neuropathology and Applied Neurobiology.2022;[Epub] CrossRef - PD-L1 tumor expression is associated with poor prognosis and systemic immunosuppression in glioblastoma
Carolina Noronha, Ana Sofia Ribeiro, Ricardo Taipa, Dina Leitão, Fernando Schmitt, Joaquim Reis, Cláudia Faria, Joana Paredes
Journal of Neuro-Oncology.2022; 156(3): 453. CrossRef - Assessment of radiographic and prognostic characteristics of programmed death-ligand 1 expression in high-grade gliomas
Makoto Ohno, Shigehisa Kitano, Kaishi Satomi, Akihiko Yoshida, Yasuji Miyakita, Masamichi Takahashi, Shunsuke Yanagisawa, Yukie Tamura, Koichi Ichimura, Yoshitaka Narita
Journal of Neuro-Oncology.2022; 160(2): 463. CrossRef - The prognostic significance of PD-L1 expression in patients with glioblastoma: A meta-analysis
Xin Guo, Yuelin Zhang, Hengxing Jiao, Xingyu Miao
Frontiers in Oncology.2022;[Epub] CrossRef - LncRNA UCA1 attenuated the killing effect of cytotoxic CD8 + T cells on anaplastic thyroid carcinoma via miR-148a/PD-L1 pathway
Xiaoming Wang, Yan Zhang, Jian Zheng, Cuixian Yao, Xiubo Lu
Cancer Immunology, Immunotherapy.2021; 70(8): 2235. CrossRef - Low tumour-infiltrating lymphocyte density in primary and recurrent glioblastoma
Kelsey Maddison, Moira C. Graves, Nikola A. Bowden, Michael Fay, Ricardo E. Vilain, Sam Faulkner, Paul A. Tooney
Oncotarget.2021; 12(21): 2177. CrossRef - A Systematic Review of the Tumor-Infiltrating CD8+ T-Cells/PD-L1 Axis in High-Grade Glial Tumors: Toward Personalized Immuno-Oncology
Mahdi Abdoli Shadbad, Zahra Asadzadeh, Negar Hosseinkhani, Afshin Derakhshani, Nazila Alizadeh, Oronzo Brunetti, Nicola Silvestris, Behzad Baradaran
Frontiers in Immunology.2021;[Epub] CrossRef - Prognostic value of programmed death ligand 1 (PD-L1) in glioblastoma: a systematic review, meta-analysis and validation based on dataset
Huan Wang, Youchao Xiao, Xingguang Ren, Dahai Wan
Bioengineered.2021; 12(2): 10366. CrossRef - Expression of Programmed Cell Death Ligand 1 and Associated Lymphocyte Infiltration in Olfactory Neuroblastoma
Nyall R. London, Lisa M. Rooper, Justin A. Bishop, Haiying Xu, Lydia J. Bernhardt, Masaru Ishii, Christine L. Hann, Janis M. Taube, Evgeny Izumchenko, Daria A. Gaykalova, Gary L. Gallia
World Neurosurgery.2020; 135: e187. CrossRef - CCR2 inhibition reduces tumor myeloid cells and unmasks a checkpoint inhibitor effect to slow progression of resistant murine gliomas
Joseph A. Flores-Toro, Defang Luo, Adithya Gopinath, Matthew R. Sarkisian, James J. Campbell, Israel F. Charo, Rajinder Singh, Thomas J. Schall, Meenal Datta, Rakesh K. Jain, Duane A. Mitchell, Jeffrey K. Harrison
Proceedings of the National Academy of Sciences.2020; 117(2): 1129. CrossRef - Treatment Results for Recurrent Glioblastoma and Alteration of Programmed Death-Ligand 1 Expression After Recurrence
Kyoung Su Sung, Tae Hoon Roh, Ju Hyung Moon, Eui Hyun Kim, Seok-Gu Kang, Se Hoon Kim, Jong Hee Chang
World Neurosurgery.2020; 135: e459. CrossRef - Current advances in PD-1/PD-L1 axis-related tumour-infiltrating immune cells and therapeutic regimens in glioblastoma
Chang Shu, Qingguo Li
Critical Reviews in Oncology/Hematology.2020; 151: 102965. CrossRef - PD-L1 Expression in Glioblastoma, the Clinical and Prognostic Significance: A Systematic Literature Review and Meta-Analysis
Chengcheng Hao, Gang Chen, Huishan Zhao, Yan Li, Jianxin Chen, Hongmei Zhang, Shan Li, Yuze Zhao, Feng Chen, Wenbin Li, Wen G. Jiang
Frontiers in Oncology.2020;[Epub] CrossRef - Checkpoint inhibitor immunotherapy for glioblastoma: current progress, challenges and future outlook
Patrick C. Gedeon, Cosette D. Champion, Kristen E. Rhodin, Karolina Woroniecka, Hanna R. Kemeny, Alexa N. Bramall, Joshua D. Bernstock, Bryan D. Choi, John H. Sampson
Expert Review of Clinical Pharmacology.2020; 13(10): 1147. CrossRef - Current clinical management of elderly patients with glioma
Alessia Pellerino, Francesco Bruno, Valeria Internò, Roberta Rudà, Riccardo Soffietti
Expert Review of Anticancer Therapy.2020; 20(12): 1037. CrossRef - The Prognostic and Therapeutic Value of PD-L1 in Glioma
Ruo Qiao Chen, Feng Liu, Xin Yao Qiu, Xiao Qian Chen
Frontiers in Pharmacology.2019;[Epub] CrossRef - Challenges and potential of PD-1/PD-L1 checkpoint blockade immunotherapy for glioblastoma
Xin Wang, Gaochao Guo, Hui Guan, Yang Yu, Jie Lu, Jinming Yu
Journal of Experimental & Clinical Cancer Research.2019;[Epub] CrossRef - Association Between Programmed Death-Ligand 1 Expression and Clinicopathological Characteristics, Structural Recurrence, and Biochemical Recurrence/Persistent Disease in Medullary Thyroid Carcinoma
Xiao Shi, Peng-Cheng Yu, Bo-Wen Lei, Cui-Wei Li, Yan Zhang, Li-Cheng Tan, Rong-Liang Shi, Jie Wang, Ben Ma, Wei-Bo Xu, Xiao Wang, Jia-Qian Hu, Nai-Si Huang, Wen-Jun Wei, Yu Wang, Tong-Zhen Chen, Yu-Long Wang, Qing-Hai Ji
Thyroid®.2019; 29(9): 1269. CrossRef - The Binding of PD-L1 and Akt Facilitates Glioma Cell Invasion Upon Starvation via Akt/Autophagy/F-Actin Signaling
Ruo Qiao Chen, Xiao Hong Xu, Feng Liu, Chun Yang Li, Yuan Jun Li, Xiang Rui Li, Guo Yong Jiang, Feng Hu, Di Liu, Feng Pan, Xin Yao Qiu, Xiao Qian Chen
Frontiers in Oncology.2019;[Epub] CrossRef - Analysis of PD-L1 expression in salivary duct carcinoma with its efficacy as a tumor marker
Yong Ju Lee, Yoon Woo Koh, Sun Och Yoon, Hyang Joo Ryu, Hye Ryun Kim, Hyang Ae Shin
Korean Society for Head and Neck Oncology.2019; 35(1): 13. CrossRef - Prognostic relevance of programmed cell death ligand 1 expression in glioblastoma
Kyu Sang Lee, Kyoungyul Lee, Sumi Yun, Seyoung Moon, Yujun Park, Jung Ho Han, Chae-Yong Kim, Hye Seung Lee, Gheeyoung Choe
Journal of Neuro-Oncology.2018; 136(3): 453. CrossRef - Programmed Death-Ligand 1 Expression and Its Correlation with Lymph Node Metastasis in Papillary Thyroid Carcinoma
Hyo Jung An, Gyung Hyuck Ko, Jeong-Hee Lee, Jong Sil Lee, Dong Chul Kim, Jung Wook Yang, Min Hye Kim, Jin Pyeong Kim, Eun Jung Jung, Dae Hyun Song
Journal of Pathology and Translational Medicine.2018; 52(1): 9. CrossRef - Radiological evaluation of response to immunotherapy in brain tumors: Where are we now and where are we going?
Michele Porcu, Cinzia Solinas, Paolo Garofalo, Evandro de Azambuja, Mario Scartozzi, Karen Willard-Gallo, Matthias Preusser, Luca Saba
Critical Reviews in Oncology/Hematology.2018; 126: 135. CrossRef - The expression of programed death ligand‐1 could be related with unfavorable prognosis in salivary duct carcinoma
Fumihiko Sato, Jun Akiba, Akihiko Kawahara, Yoshiki Naito, Takeharu Ono, Yorihiko Takase, Kazuya Murata, Hideyuki Abe, Tomohiko Yamaguchi, Hiroaki Miyoshi, Yushi Abe, Yutaro Mihara, Masahiko Tanikawa, Momoko Akashi, Hirofumi Kurose, Hirohito Umeno, Hirohi
Journal of Oral Pathology & Medicine.2018; 47(7): 683. CrossRef - Expression Patterns, Prognostic Value, and Intratumoral Heterogeneity of PD-L1 and PD-1 in Thymoma and Thymic Carcinoma
Dwight Owen, Benjamin Chu, Amy M. Lehman, Lakshmanan Annamalai, Jennifer H. Yearley, Konstantin Shilo, Gregory A. Otterson
Journal of Thoracic Oncology.2018; 13(8): 1204. CrossRef - PD-L1 and immune escape: insights from melanoma and other lineage-unrelated malignancies
Noah Frydenlund, Meera Mahalingam
Human Pathology.2017; 66: 13. CrossRef - Clinical Trials Investigating Immune Checkpoint Blockade in Glioblastoma
Russell Maxwell, Christopher M. Jackson, Michael Lim
Current Treatment Options in Oncology.2017;[Epub] CrossRef - Topotecan Decreases the Expression of Programmed Death-Ligand 1 in Glioblastoma Cell Lines; Implications for Immunotherapy
Joshua Bernstock, Daniel Ye, Florian Gessler, Luca Peruzzotti-Jametti, Mark Gilbert, Yves Pommier, Stefano Pluchino, Ichiro Nakano, John Hallenbeck
Matters.2017;[Epub] CrossRef - Relationship between expression of PD-L1 and tumor angiogenesis, proliferation, and invasion in glioma
Song Xue, Man Hu, Peifeng Li, Ji Ma, Li Xie, Feifei Teng, Yufang Zhu, Bingjie Fan, Dianbin Mu, Jinming Yu
Oncotarget.2017; 8(30): 49702. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure



Fig. 1.
Fig. 2.
Fig. 3.
| Characteristic | No. (%) |
|---|---|
| Gender | |
| Male | 26 (48.1) |
| Female | 28 (51.9) |
| Primary/Secondary | |
| Primary | 43 (79.6) |
| Secondary | 11 (20.4) |
| Surgical treatment | |
| Total resection | 40 (74.1) |
| Subtotal resection | 11 (20.4) |
| Biopsy and others | 3 (5.6) |
| Adjuvant treatment | |
| CCRT | 43 (79.6) |
| CTx or RTx alone | 9 (16.7) |
| No treatment | 2 (3.7) |
| No. of lesions | |
| Single | 32 (59.3) |
| Multiple (multifocal, multicentric) | 22 (40.7) |
| Alive at last follow-up | |
| Yes | 36 (66.7) |
| No | 18 (33.3) |
| Progress/Recurrence | |
| Yes | 40 (74.1) |
| No | 14 (25.9) |
| Overall survival time, mean (range, mo) | 17.57 (1.0–51.0) |
| Disease free survival, mean (range, mo) | 12.13 (1.0–43.0) |
| All cases (n=54) | PD-L1 |
PD-1+TIMC |
|||||
|---|---|---|---|---|---|---|---|
| Negative | Positive | p-value | Low | High | p-value | ||
| All cases | 37 (68.5) | 17 (31.5) | 27 (50) | 27 (50) | |||
| Gender | .914 | .586 | |||||
| Male | 26 | 18 (69.2) | 8 (30.8) | 14 (53.8) | 12 (46.2) | ||
| Female | 28 | 19 (67.9) | 9 (32.1) | 13 (48.1) | 15 (55.6) | ||
| Age at diagnosis (yr) Mean (min-max) | 57.62 (31–85) | 56.18 (36–78) | .814 | 54.26 (32–77) | 60.07 (31–85) | .115 | |
| Primary/Secondary | .47 | .311 | |||||
| Primary | 43 | 28 (65.1) | 15 (34.9) | 23 (53.5) | 20 (46.5) | ||
| Secondary | 11 | 9 (81.8) | 2 (18.2) | 4 (36.4) | 7 (63.6) | ||
| Surgical treatment | .672 | .804 | |||||
| Total resection | 40 | 26 (65.0) | 14 (35.0) | 19 (47.5) | 21 (52.5) | ||
| Subtotal resection | 11 | 9 (81.8) | 2 (18.2) | 6 (54.5) | 5 (45.5) | ||
| Biopsy and others | 3 | 2 (66.7) | 1 (33.3) | 2 (66.7) | 1 (33.3) | ||
| Adjuvant treatment | .257 | .082 | |||||
| CCRT | 43 | 27 (62.8) | 16 (37.2) | 23 (53.5) | 20 (46.5) | ||
| CTx or RTx alone | 9 | 8 (88.9) | 1 (11.1) | 2 (22.2) | 7 (77.8) | ||
| No treatment | 2 | 2 (100) | 0 | 2 (100) | 0 | ||
| No. of lesions | .713 | .78 | |||||
| Single | 33 | 22 (66.7) | 11 (33.3) | 16 (48.5) | 17 (51.5) | ||
| Multiple | 21 | 15 (71.4) | 6 (28.6) | 11 (52.4) | 10 (47.6) | ||
| Alive at last follow-up | .038 | .248 | |||||
| Yes | 36 | 28 (77.8) | 8 (22.2) | 16 (44.4) | 20 (55.6) | ||
| No | 18 | 9 (50.0) | 9 (50.0) | 11 (61.1) | 7 (38.9) | ||
| Progress/Recurrence | 1 | .214 | |||||
| Yes | 40 | 27 (67.5) | 13 (32.5) | 22 (55.0) | 18 (45.0) | ||
| No | 14 | 10 (71.4) | 4 (28.6) | 5 (35.7) | 9 (64.3) | ||
| Variable | OS |
DFS |
||||||
|---|---|---|---|---|---|---|---|---|
| Univariate |
Multivariate |
Univariate |
Multivariate |
|||||
| HR (95% CI) | p-value | HR (95% CI) | p-value | Hazard ratio (95% CI) | p-value | HR (95% CI) | p-value | |
| PD-L1 expression | ||||||||
| Positive | 3.058 (1.160–8.060) | .024 | 4.958 (1.557–15.79) | .007 | 1.651 (0.821–3.319) | .16 | ||
| Negative | Reference | Reference | Reference | |||||
| PD-1+TIMC | ||||||||
| High | 0.726 (0.280–1.879) | .509 | 0.842 (0.445–1.593) | .597 | ||||
| Low | Reference | Reference | ||||||
| Age (continuous) | 0.989 (0.953–1.026) | .541 | 0.997 (0.973–1.002) | .825 | ||||
| Gender | ||||||||
| Male | 2.000 (0.747–5.360) | .168 | 4.053 (1.230–13.35) | .021 | 1.806 (0.940–3.472) | .076 | 2.142 (1.077–4.260) | .03 |
| Female | Reference | Reference | Reference | Reference | ||||
| Primary vs secondary | ||||||||
| Primary | 1.830 (0.418–8.007) | .423 | 1.023 (0.447–2.340) | .957 | ||||
| Secondary | Reference | Reference | ||||||
| Numver of lesions | ||||||||
| Single | Reference | .133 | Reference | .078 | Reference | .278 | Reference | .092 |
| Multiple | 2.103 (0.797–5.547) | 2.715 (0.893–8.253) | 1.438 (0.746–2.772) | 1.814 (0.907–3.629) | ||||
| Surgical treatment | ||||||||
| Total resection | Reference | Reference | ||||||
| Subtotal resection | 1.134 (0.365–3.528) | .828 | 1.099 (0.497–2.433) | .815 | ||||
| Biopsy and others | 1.453 (0.186–11.34) | .721 | 2.807 (0.838–9.405) | .094 | ||||
| Adjuvant treatment | ||||||||
| CCRT | Reference | Reference | Reference | |||||
| CTx or RTx alone | 1.309 (0.369–4.640) | .677 | 2.369 (0.562–9.989) | .024 | 0.706 (0.245–2.030) | .518 | ||
| No treatment | 7.717 (0.880–67.674) | .065 | 5.760 (2.089–317.6) | .011 | 1.346 (0.181–10.011) | .771 | ||
| Recurrence or progression | 2.238 (0.511–9.795) | .285 | ||||||
| Variable | Group 1 | Group 2 | Group 3 | Group 4 |
|---|---|---|---|---|
| (PD-L1+/high PD-1+TIMC) | (PD-L1+/low PD-1+TIMC) | (PD-L1-/high PD-1+TIMC) | (PD-L1-/low PD-1+TIMC) | |
| No. of patients (%) | 10 (18.5) | 7 (13) | 17 (31.5) | 20 (37) |
| Age, mean (range, yr) | 59.6 (40–70) | 51.3 (36–69) | 60.3 (31–85) | 55.3 (32–68) |
| Ki-67 index, mean (range, %) | 28.3 (10–60) | 41.4 (5–80) | 29.9 (6–55) | 32.3 (4–95) |
| Tumor cellularity | Moderate–marked | Marked | Mild–moderate | Mild–moderate |
| TIMC density | High | Low | High | Low~high |
CCRT, concurrent chemoradiotherapy; CTx, chemotherapy; RTx, radiotherapy.
Values are presented as number (%) unless otherwise indicated. PD-L1, programmed death ligand 1; PD-1, programmed cell death 1; TIMC, tumor infiltrating mononuclear cell; GBM, glioblastoma; CCRT, concurrent chemoradiotheraphy; CTx, chemotherapy; RTx, radiation therapy.
OS, overall survival; DFS, disease free survival; HR, hazard ratio; CI, confidence interval; PD-L1, programmed death ligand 1; PD-1, programmed cell death 1; TIMC, tumor infiltrating mononuclear cell; CCRT, concurrent chemoradiation therapy; CTx, chemotherapy; RTx, radiation therapy.
PD-L1, programmed death ligand 1; PD-1, programmed cell death 1; TIMC, tumor infiltrating mononuclear cell.

 E-submission
E-submission