Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 51(1); 2017 > Article
-
Original Article
Aurora Kinase A Is a Prognostic Marker in Colorectal Adenocarcinoma - Hyun Min Koh, Bo Geun Jang, Chang Lim Hyun, Young Sill Kim, Jin Won Hyun1, Weon Young Chang2, Young Hee Maeng
-
Journal of Pathology and Translational Medicine 2017;51(1):32-39.
DOI: https://doi.org/10.4132/jptm.2016.10.17
Published online: December 25, 2016
Department of Pathology, Jeju National University School of Medicine, Jeju, Korea
1Department of Biochemistry, Jeju National University School of Medicine, Jeju, Korea
2Department of Surgery, Jeju National University School of Medicine, Jeju, Korea
- Corresponding Author: Young Hee Maeng, MD, PhD Department of Pathology, Jeju National University School of Medicine, 15 Aran 13-gil, Jeju 63241, Korea Tel: +82-64-717-1410 Fax: +82-64-717-1131 E-mail: yhmaeng@jejunu.ac.kr
© 2017 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
Background
- Aurora kinase A (AURKA), or STK15/BTAK, is a member of the serine/threonine kinase family and plays important roles in mitosis and chromosome stability. This study investigated the clinical significance of AURKA expression in colorectal cancer patients in Korea.
-
Methods
- AURKA protein expression was evaluated by immunohistochemistry in 151 patients with colorectal adenocarcinoma using tissue microarray blocks. We analyzed the relationship between clinicopathological characteristics and AURKA expression. In addition, the prognostic significance of various clinicopathological data for progression-free survival (PFS) was assessed. Also we evaluated copy number variations by array comparative genomic hybridization and AURKA gene amplification using fluorescence in situ hybridization in colorectal carcinoma tissues.
-
Results
- AURKA gene amplification was found more frequently in the 20q13.2–13.33 gain-positive group than the group with no significant gain on the AURKA-containing locus. AURKA protein expression was detected in 45% of the cases (68/151). Positive staining for AURKA was observed more often in male patients (p = .035) and distally located tumors (p = .021). PFS was shorter in patients with AURKA expression compared to those with low-level AURKA expression (p < .001). Univariate analysis revealed that AURKA expression (p = .001), age (p = .034), lymphatic invasion (p = .001), perineural invasion (p = .002), and TNM stage (p = .013) significantly affected PFS. In a multivariate analysis of PFS, a Cox proportional hazard model confirmed that AURKA expression was an independent and significant prognostic factor in colorectal adenocarcinoma (hazard ratio, 3.944; p < .001).
-
Conclusions
- AURKA could serve as an independent factor to predict a poor prognosis in Korean colorectal adenocarcinoma patients.
- Patients and clinicopathological data
- Samples from 151 patients who underwent curative surgical resection for colorectal adenocarcinomas between January 2008 and July 2012 at Jeju National University Hospital (Jeju, Korea) were examined. Patients who did not undergo curative surgical resection and those who had any forms of preoperative chemotherapy and/or radiotherapy at the time of surgical resection were excluded. Staging was performed according to the American Joint Committee on Cancer TNM Classification of Malignant Tumors, seventh edition, while the histologic type and differentiation grade of the tumor were determined using the classification system of the World Health Organization, fourth edition [14]. PFS was measured from the date of CRC surgery until the time of recurrence or last follow-up. Clinical data from the patients were collected through medical record examination. The median age of the patients was 66 years (range, 35 to 88 years). Other clinicopathological information is shown in Table 1. This study was approved by the Institutional Review Board of Jeju National University Hospital (2016-06-004).
- Array comparative genomic hybridization
- DNA from 24 fresh tissue specimens of colorectal adenocarcinomas was analyzed versus reference DNA. Test and reference gDNAs were independently labeled with fluorescent dyes, co-hybridized to a NimbleGen Human CGH 135K Whole-Genome Tiling array (Roche NimbleGen Inc, Madison, WI, USA), and scanned using a 2 µm scanner. Log2-ratio values of the probe signal intensities (Cy3/Cy5) were calculated and plotted versus genomic position using Roche NimbleGen NimbleScan software. Data are displayed in Roche NimbleGen SignalMap software.
- Fluorescent in situ hybridization
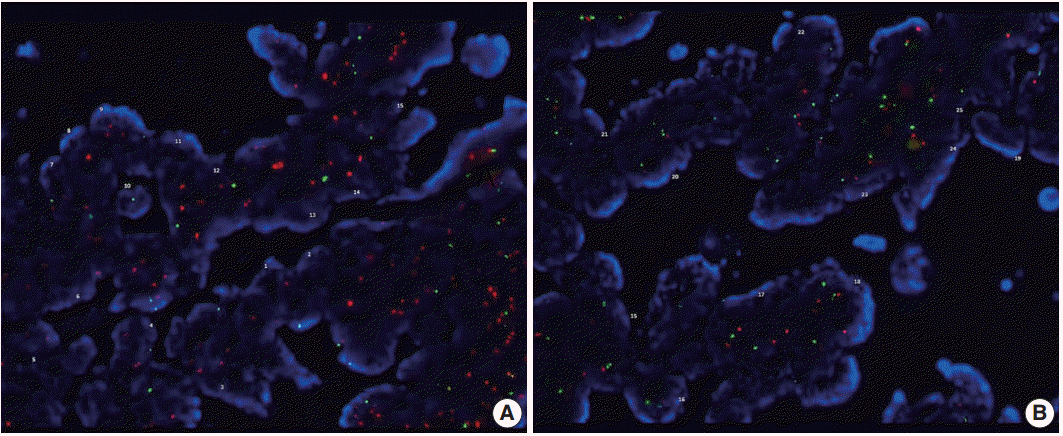
- FISH analysis targeting AURKA on 20q13.2 was done on the same cases used in aCGH. Fifteen cases of formalin-fixed, paraffin-embedded tissue were tested in total; 10 cases with copy number gain on 20q13.2–13.33 and five cases with no copy number gain. The examination was performed according to the manufacturer’s instructions (Empire Genomics, Buffalo, NY, USA). Fluorescence was scored on a minimum of 20 non-overlapping nuclei in the representative tumor areas. The AURKA/CEP20 ratio was calculated by dividing the total number of AURKA signals by the total number of CEP20 signals and the cases with AURKA/CEP20 ratio≥2.0 were interpreted as positive.
- Tissue microarray construction
- In total, eight tissue microarrays (TMAs) were constructed as described previously [4,9]. Briefly, hematoxylin and eosin (H&E)–stained slides were reviewed and the most representative tumor area was marked. The area was carefully marked on H&E-stained slides as well as formalin-fixed, paraffin-embedded tissue blocks. A core (4 mm in diameter) of the tumor area was obtained from each specimen. One section from each block was stained with H&E for tissue confirmation.
- Immunohistochemistry
- Immunohistochemistry was performed on 4-μm-thick sections from TMA blocks. Tissues were stained with polyclonal anti-AURKA antibodies at a dilution of 1:200 (HPA002636, ATLAS Sigma Life Science, St. Louis, MO, USA) using an automated immunostainer (Benchmark XT, Ventana Medical Systems Inc., Tucson, AZ, USA). The primary antibody was omitted for the negative control, and the adjacent ganglion cells in the nerve bundles within each slide served as an internal reference.
- AURKA protein expression
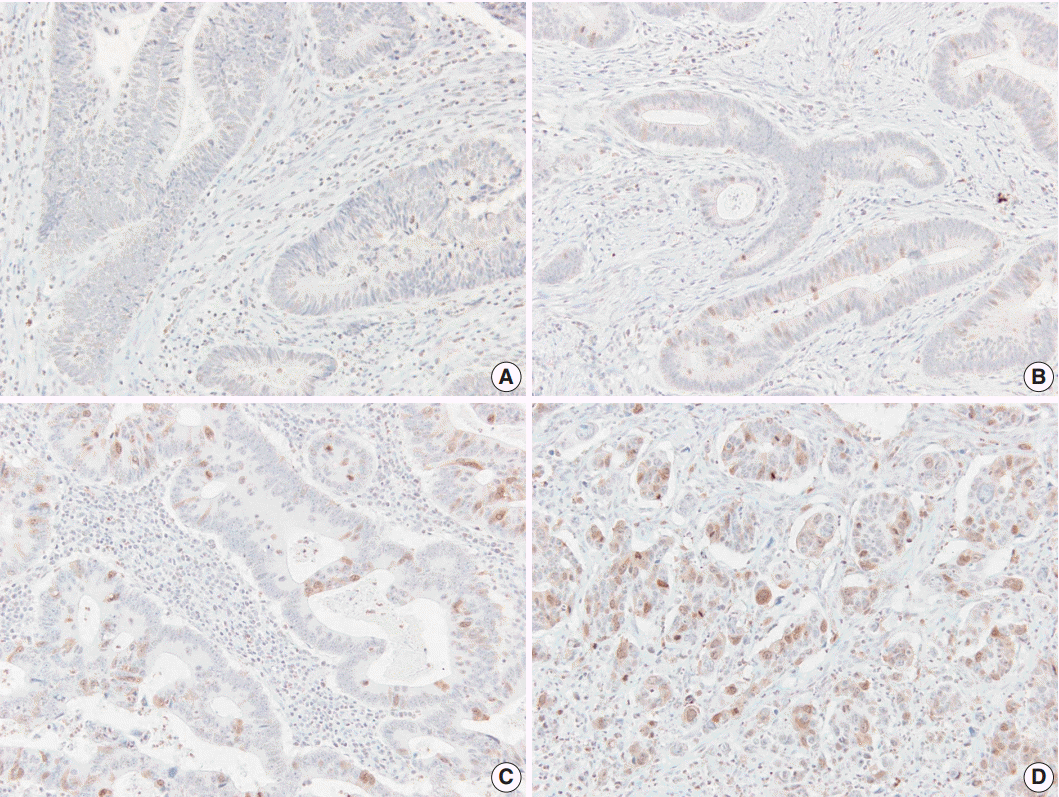
- Immunoreactivity was evaluated in each TMA sample by visual counting of the tumor cells. The extent of positively stained nuclei was scored as follows: 0, positive staining in 0%; 1, <10%; 2, ≥10% and <25%; 3, ≥25% and <50%; and 4, ≥50%. Scores of 2–4 were considered positive, and scores ≤1 were considered negative [4,12,13]. To confirm reproducibility, all samples were scored by two independent observers in a blinded manner. If discrepancies occurred, a consensus score was reached.
- Statistical analysis
- Pearson’s chi-square test was used for categorical variables. PFS was analyzed using the Kaplan-Meier method with the log-rank test assessing differences in survival probability between groups. The prognostic significance of various clinicopathological characteristics for PFS was assessed by the Cox proportional hazard regression method. All values were based on two-sided statistical analyses; significance was set at p<.05. All statistical tests were performed with IBM SPSS ver. 21.0 (IBM Corp., Armonk, NY, USA).
MATERIALS AND METHODS
- CNVs in chromosome 20
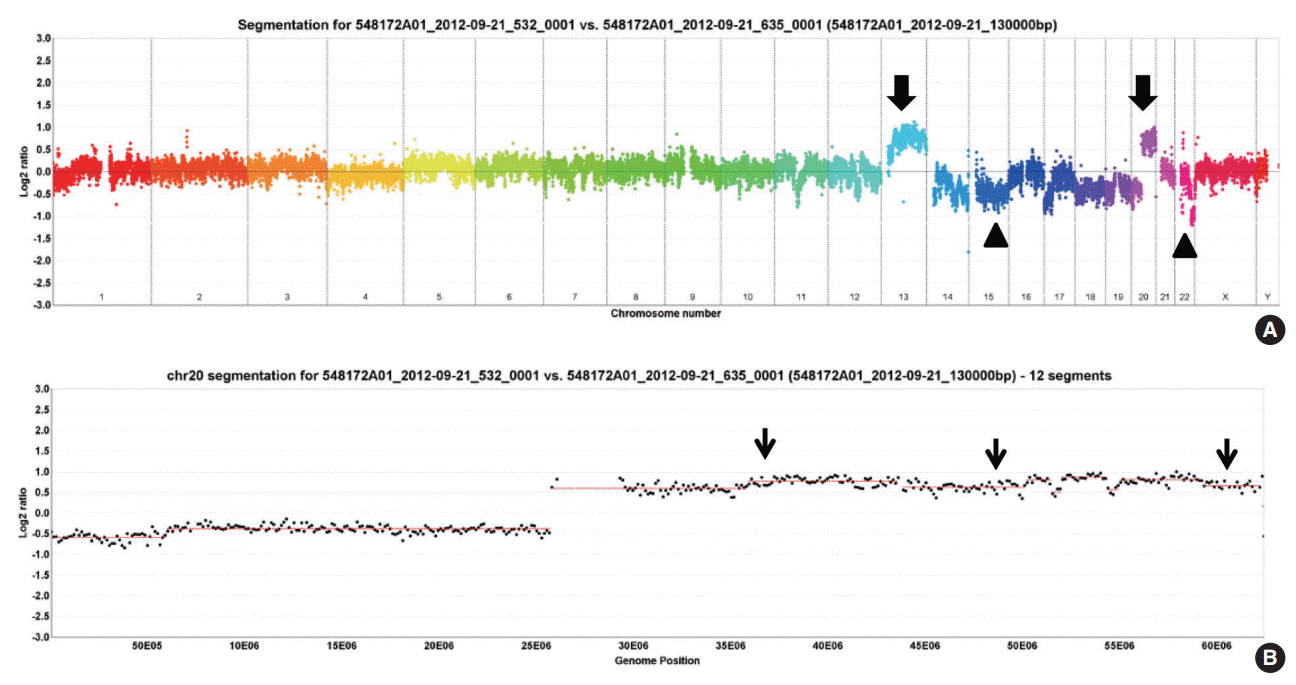
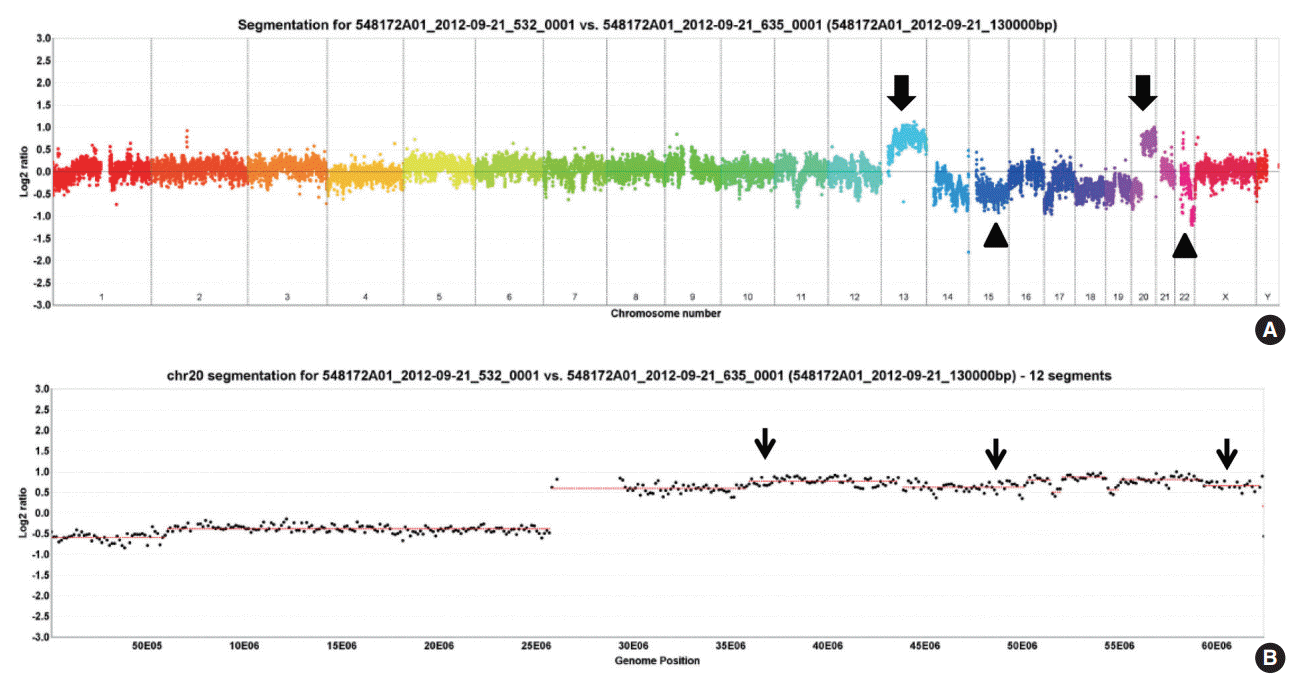
- In twenty-four cases of colorectal carcinomas, total 1,297 CNVs were detected (Fig. 1A). The locus of 20q13.2–13.33 containing AURKA gene were recurrently gained in 13 cases (54%), while only one case showed loss of the area (Fig. 1B).
- AURKA gene amplification status
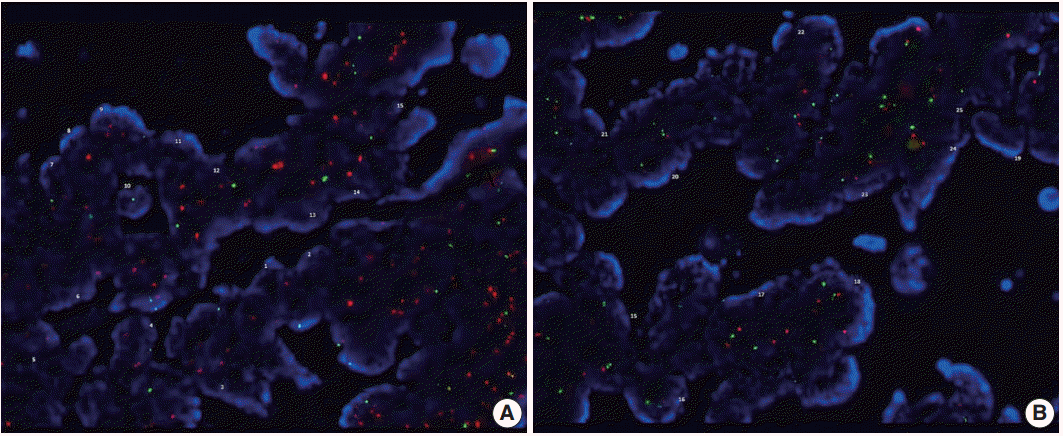
- AURKA amplification was assessed in 15 patients (group with 20q13.2–13.33 copy number gain, n=10; gain-negative group, n=5). One case of 20q13.2–13.33 gain-positive group was failed to express fluorescences. Three out of the remaining nine cases with 20q13.2–13.33 gain showed amplification of AURKA gene but none revealed gene amplification among the gain-negative group (Table 2, Fig. 2).
- Relationship between AURKA expression and clinicopathological characteristics
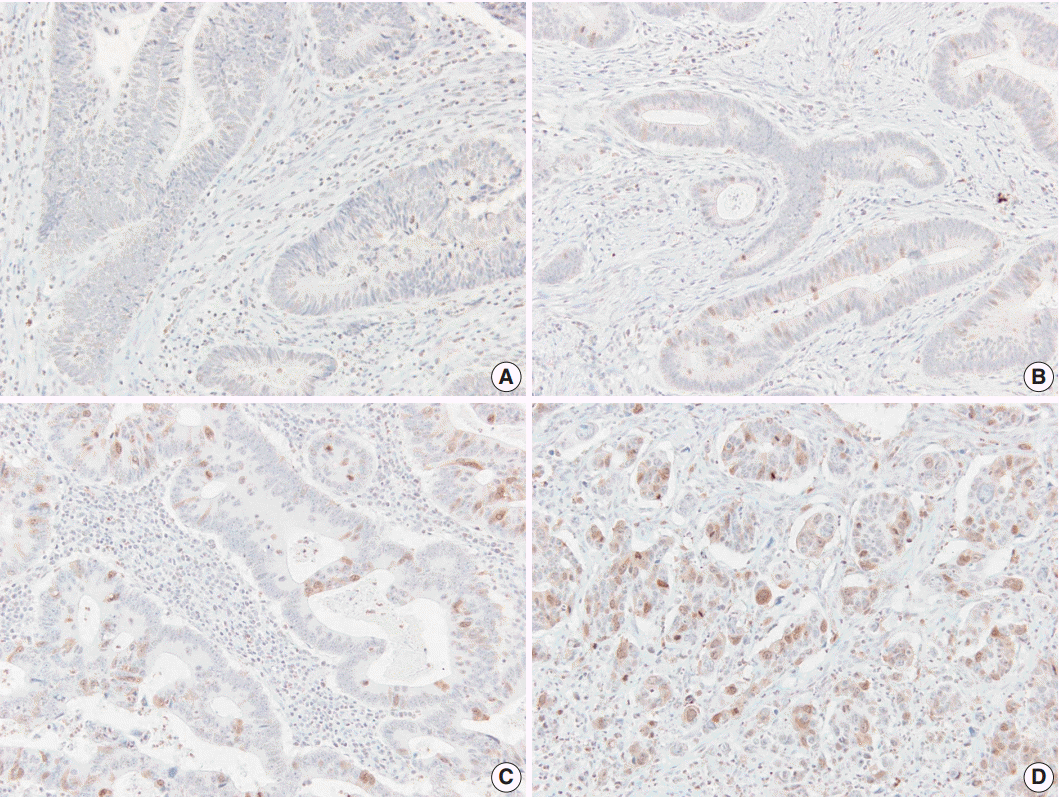
- AURKA protein was expressed in 45% of colorectal adenocarcinoma cases (68/151), while negative to faintly reactive staining was found in normal colorectal epithelial cells. The staining pattern was predominantly nuclear or nuclear and cytoplasmic (Fig. 3). Table 3 shows the relationship between AURKA expression and clinicopathological characteristics. AURKA protein expression was significantly related to patient sex, and positive AURKA staining was detected more often in male patients than in female (51.0% vs 31.9%, p=.035). In addition, AURKA expression was closely associated with tumor location, and it was more frequently found in carcinomas of the rectum, sigmoid colon, and descending colon than in carcinomas of proximal colon (51.4% vs 30.4%, p=.021). AURKA protein expression was not significantly correlated with age; tumor differentiation; vascular, lymphatic, and perineural invasion; or TNM stage.
- AURKA expression and survival analysis
- The mean follow-up time of the patients in this study was 1,269 days (range, 8 to 2,892 days). In total, 23.8% of the patients (n=36) had recurred (AURKA-positive group, n=27; AURKA-negative group, n=9). The recurrence rate was significantly higher in the AURKA-positive group compared to the negative group (39.1% vs 11%, p<.001).
- The mean overall PFS time was 74.6 months (range, 68.6 to 80.7 months). The AURKA-positive patients had a significantly poorer PFS than the AURKA-negative patients (p<.001). A univariate analysis demonstrated that AURKA expression (p=.001) (Fig. 4A), age (p=.034), lymphatic invasion (p=.001) (Fig. 4B), perineural invasion (p=.002) (Fig. 4C), and TNM stage (p=.013) (Fig. 4D) significantly affected PFS. In a multivariate analysis of PFS, a Cox proportional hazard model confirmed that AURKA expression was an independent and significant prognostic factor in colorectal adenocarcinoma (hazard ratio, 3.944; 95% confidence interval [CI], 1.821 to 8.542; p<.001) (Table 4). Perineural invasion was also identified as a significant prognostic factor (hazard ratio, 2.037; 95% CI, 1.017 to 4.079; p=.045) (Table 3).
RESULTS
- CRC is among the most common malignancies [13] and is the leading cause of cancer mortality in the world [20]. The identification of genes correlated with carcinogenesis and the research to silence these genes can improve the patient care by more accurately predicting the prognosis and selecting the most appropriate adjuvant therapy [13,15].
- The role of Aurora kinases in mitosis and tumorigenesis is well documented [12,20,21]. AURKA is required for mitotic entry, chromosome alignment, and cytokinesis, and its abnormal function can result in aberrant cell division and aneuploidy, which in turn increase genomic instability and contribute to carcinogenesis [15,22]. Further, AURKA is an oncogene that contributes to colorectal adenoma to carcinoma progression and is associated with the malignant transformation of colorectal adenomas but not with serrated neoplasia progression [21,22].
- Chromosomal abnormalities in CRC have been studied by multiple groups using either CGH or aCGH. This has led to the discovery of many chromosomal aberrations, including gains and losses. Particularly common findings are gains in 20q, 13q, 7p, and 8q and losses in 17p, 18q, 8p, 4q, and 5q [23]. Orsetti et al. [24] reported that most commonly altered regions (gains or losses in ≥ 35% of the samples) are gains at chromosomes 7p, 7q, 8q, 13q, 20 and losses at 8p, 17p, and 18 in the CRC. In this study, 20q13.2–13.33 copy number gain is recurrently observed in 13 cases (54%), which is consistent with the previous results.
- We also assessed AURKA amplification using FISH in two subgroups. The gene amplification is observed more frequently in the copy number gain group (three cases out of nine), than the group with no significant gain on the AURKA-containing locus. However, the data could not be analyzed statistically, due to a small number of cases. Further large-scale studies are required to assess the differences between the two groups.
- A small number of reseachers have reported FISH result for AURKA gene amplification in various malignancies, such as melanomas and cancers of breast and prostate [25-28]. No reports on FISH for AURKA gene amplification in colorectal carcinoma tissue were found in the English literature in spite of a thorough searching.
- Zhang et al. [29] demonstrated an increased AURKA gene copy number in 32.1% of advanced CRCs (43/134), and Casorzo et al. [22] reported AURKA gene overexpression in 85% of adenomas (17/20) containing invasive carcinoma of the colorectum, corresponding to early invasive carcinoma. In a previous study, 69% of metastatic CRC samples (41/59) showed an increased gene copy number [12].
- AURKA protein overexpression and gene amplification are common in CRCs [4,9,12,13,15,19-22,29,30]. In this study, we detected AURKA overexpression in 45% of colorectal adenocarcinoma samples (71/151) using immunohistochemistry. Similarly, Lam et al. [13] reported AURKA protein expression in 48.5% (97/200) of CRC samples. In other studies, 33% (9/20) [12] and 82.5% (33/40) [15] of metastatic CRC samples showed AURKA overexpression.
- In our study, AURKA expression was related to patient sex and tumor location, along with several other clinicopathological parameters. Tumor location, histology, and grade were correlated with AURKA protein expression in the report by Lam et al. [13] Baba et al. [19] reported that AURKA expression was inversely associated with a family history of CRC and not correlated with tumor location, grade, histologic component, or stage. Goktas et al. [15] found a significant relationship between AURKA expression and the histologic grade of the tumor tissue.
- These discrepancies in AURKA expression may not only be caused by the heterogeneity of the study groups (e.g., patient number, patient characteristics, and disease stage), but also by differences in various technical conditions.
- Some authors reported that AURKA expression is correlated with clinicopathological factors in other malignancies. For example, positive AURKA expression was closely correlated with TNM stage in gastric cancer [10] and with initial clinical stage, Ki-67 labeling index, and the recurrence rate in triple-negative breast cancer [14]. Ogawa et al. [11] reported that perimembrane AURKA staining was significantly related to a higher pathologic stage and higher proliferative activity.
- A few previous studies have investigated the prognostic impact of AURKA expression in CRC patients [4,9,15]. Belt et al. [4] suggested that high-level AURKA expression was significantly associated with recurrence in stage II or III colon cancer. Goos et al. [9] revealed that high-level AURKA expression was associated with poor overall survival in CRC patients with liver metastasis. In contrast, Goktas et al. [15] reported that AURKA overexpression may have a positive effect on survival in metastatic CRC. We analyzed the correlation between AURKA expression and survival in patients with CRC. Our data demonstrate that AURKA expression in CRC patients is associated with poor PFS. Moreover, our Cox model analysis indicated that AURKA expression is a prognostic factor for poor PFS in CRC patients. However, overall survival analysis could not be performed due to a short follow-up period.
- Recent studies have shown that AURKA inhibitors have anticancer activity in various preclinical cancer models, and some inhibitors have entered clinical trials [1,8]. Such studies have underlined the incremental therapeutic efficacy of combining AURKA inhibitors with conventional anti-cancer drugs to inhibit tumor progression and restore chemosensitivity [1]. Our results suggest that targeted treatment with AURKA inhibitors can improve PFS and assist in planning the treatment of CRC patients.
- In summary, AURKA expression was significantly associated with patient sex and CRC location, and it was an independent molecular prognostic factor for poor outcome in CRC patients. Thus, AURKA expression may serve as a valuable prognostic marker for CRC.
DISCUSSION
Acknowledgments

| 20q13.2–13.33 copy number gain |
AURKA gene amplification |
||
|---|---|---|---|
| Positive | Negative | Total cases | |
| Positive | 3 | 6 | 9 |
| Negative | 0 | 5 | 5 |
| Total cases | 3 | 11 | 14 |
- 1. D’Assoro AB, Haddad T, Galanis E. Aurora-A kinase as a promising therapeutic target in cancer. Front Oncol 2015; 5: 295.PubMed
- 2. Katsha A, Belkhiri A, Goff L, El-Rifai W. Aurora kinase A in gastrointestinal cancers: time to target. Mol Cancer 2015; 14: 106.ArticlePubMedPMCPDF
- 3. Cammareri P, Scopelliti A, Todaro M, et al. Aurora-a is essential for the tumorigenic capacity and chemoresistance of colorectal cancer stem cells. Cancer Res 2010; 70: 4655-65. ArticlePubMedPDF
- 4. Belt EJ, Brosens RP, Delis-van Diemen PM, et al. Cell cycle proteins predict recurrence in stage II and III colon cancer. Ann Surg Oncol 2012; 19 Suppl 3: S682-92. ArticlePubMed
- 5. Zhang J, Li B, Yang Q, Zhang P, Wang H. Prognostic value of Aurora kinase A (AURKA) expression among solid tumor patients: a systematic review and meta-analysis. Jpn J Clin Oncol 2015; 45: 629-36. ArticlePubMed
- 6. Fu J, Bian M, Jiang Q, Zhang C. Roles of Aurora kinases in mitosis and tumorigenesis. Mol Cancer Res 2007; 5: 1-10. ArticlePubMedPDF
- 7. D’Assoro AB, Liu T, Quatraro C, et al. The mitotic kinase Aurora-A promotes distant metastases by inducing epithelial-to-mesenchymal transition in ERα(+) breast cancer cells. Oncogene 2014; 33: 599-610. ArticlePubMedPDF
- 8. Cervantes A, Elez E, Roda D, et al. Phase I pharmacokinetic/pharmacodynamic study of MLN8237, an investigational, oral, selective aurora a kinase inhibitor, in patients with advanced solid tumors. Clin Cancer Res 2012; 18: 4764-74. ArticlePubMedPDF
- 9. Goos JA, Coupe VM, Diosdado B, et al. Aurora kinase A (AURKA) expression in colorectal cancer liver metastasis is associated with poor prognosis. Br J Cancer 2013; 109: 2445-52. ArticlePubMedPMCPDF
- 10. Wang J, Yang S, Zhang H, et al. Aurora-A as an independent molecular prognostic marker in gastric cancer. Oncol Rep 2011; 26: 23-32. PubMed
- 11. Ogawa E, Takenaka K, Katakura H, et al. Perimembrane Aurora-A expression is a significant prognostic factor in correlation with proliferative activity in non-small-cell lung cancer (NSCLC). Ann Surg Oncol 2008; 15: 547-54. ArticlePubMedPDF
- 12. Dotan E, Meropol NJ, Zhu F, et al. Relationship of increased aurora kinase A gene copy number, prognosis and response to chemotherapy in patients with metastatic colorectal cancer. Br J Cancer 2012; 106: 748-55. ArticlePubMedPMCPDF
- 13. Lam AK, Ong K, Ho YH. Aurora kinase expression in colorectal adenocarcinoma: correlations with clinicopathological features, p16 expression, and telomerase activity. Hum Pathol 2008; 39: 599-604. ArticlePubMed
- 14. Xu J, Wu X, Zhou WH, et al. Aurora-A identifies early recurrence and poor prognosis and promises a potential therapeutic target in triple negative breast cancer. PLoS One 2013; 8: e56919.ArticlePubMedPMC
- 15. Goktas S, Yildirim M, Suren D, et al. Prognostic role of Aurora-A expression in metastatic colorectal cancer patients. J BUON 2014; 19: 686-91. PubMed
- 16. Li D, Zhu J, Firozi PF, et al. Overexpression of oncogenic STK15/BTAK/Aurora A kinase in human pancreatic cancer. Clin Cancer Res 2003; 9: 991-7. PubMed
- 17. Park HS, Park WS, Bondaruk J, et al. Quantitation of Aurora kinase A gene copy number in urine sediments and bladder cancer detection. J Natl Cancer Inst 2008; 100: 1401-11. ArticlePubMedPMC
- 18. Jeng YM, Peng SY, Lin CY, Hsu HC. Overexpression and amplification of Aurora-A in hepatocellular carcinoma. Clin Cancer Res 2004; 10: 2065-71. ArticlePubMedPDF
- 19. Baba Y, Nosho K, Shima K, et al. Aurora-A expression is independently associated with chromosomal instability in colorectal cancer. Neoplasia 2009; 11: 418-25. ArticlePubMedPMC
- 20. Sillars-Hardebol AH, Carvalho B, de Wit M, et al. Identification of key genes for carcinogenic pathways associated with colorectal adenoma-to-carcinoma progression. Tumour Biol 2010; 31: 89-96. ArticlePubMedPMC
- 21. Carvalho B, Postma C, Mongera S, et al. Multiple putative oncogenes at the chromosome 20q amplicon contribute to colorectal adenoma to carcinoma progression. Gut 2009; 58: 79-89. ArticlePubMed
- 22. Casorzo L, Dell’Aglio C, Sarotto I, Risio M. Aurora kinase A gene copy number is associated with the malignant transformation of colorectal adenomas but not with the serrated neoplasia progression. Hum Pathol 2015; 46: 411-8. ArticlePubMed
- 23. Jasmine F, Rahaman R, Dodsworth C, et al. A genome-wide study of cytogenetic changes in colorectal cancer using SNP microarrays: opportunities for future personalized treatment. PLoS One 2012; 7: e31968.ArticlePubMedPMC
- 24. Orsetti B, Selves J, Bascoul-Mollevi C, et al. Impact of chromosomal instability on colorectal cancer progression and outcome. BMC Cancer 2014; 14: 121.ArticlePubMedPMCPDF
- 25. Park K, Chen Z, MacDonald TY, et al. Prostate cancer with Paneth cell-like neuroendocrine differentiation has recognizable histomorphology and harbors AURKA gene amplification. Hum Pathol 2014; 45: 2136-43. ArticlePubMedPMC
- 26. Mosquera JM, Beltran H, Park K, et al. Concurrent AURKA and MYCN gene amplifications are harbingers of lethal treatment-related neuroendocrine prostate cancer. Neoplasia 2013; 15: 1-10. ArticlePubMedPMC
- 27. Letessier A, Sircoulomb F, Ginestier C, et al. Frequency, prognostic impact, and subtype association of 8p12, 8q24, 11q13, 12p13, 17q12, and 20q13 amplifications in breast cancers. BMC Cancer 2006; 6: 245.ArticlePubMedPMCPDF
- 28. Diaz A, Puig-Butillé JA, Valera A, et al. TERT and AURKA gene copy number gains enhance the detection of acral lentiginous melanomas by fluorescence in situ hybridization. J Mol Diagn 2014; 16: 198-206. ArticlePubMed
- 29. Zhang C, Fang Z, Xiong Y, et al. Copy number increase of aurora kinase A in colorectal cancers: a correlation with tumor progression. Acta Biochim Biophys Sin (Shanghai) 2010; 42: 834-8. ArticlePubMedPDF
- 30. Lassmann S, Danciu M, Müller M, et al. Aurora A is differentially expressed and regulated in chromosomal and microsatellite instable sporadic colorectal cancers. Mod Pathol 2009; 22: 1385-97. ArticlePubMedPDF
REFERENCES
Figure & Data
References
Citations

- Exploring pyrimidine scaffolds for cancer therapy: A triad of synthetic chemistry, computational studies, and in-vitro biological testing
Pooja Kumari, Anandkumar Tengli
Journal of Molecular Structure.2026; 1350: 144013. CrossRef - The Role of Aurora Kinase A in HBV-Associated Hepatocellular Carcinomas: A Molecular and Immunohistochemical Study
Mustafa Huz, Nese Karadag Soylu, Ahmet Koc, Zeynep Kucukakcali, Nefsun Danis, Onural Ozhan
Diagnostics.2026; 16(1): 160. CrossRef - First-in-class dual inhibitors of MASTL and Aurora A kinase: Discovery of selective cyclohexa[b]thiophenes with potent anticancer activity
Somaya A. Abdel-Rahman, Hossam Nada, Moustafa T. Gabr
European Journal of Medicinal Chemistry.2025; 293: 117729. CrossRef - RNAi delivery mediated by milk extracellular vesicles in colon cancer
Jessie Santoro, Silvia Nuzzo, Andrea Soricelli, Marco Salvatore, Anna Maria Grimaldi
Molecular Therapy Nucleic Acids.2025; 36(3): 102644. CrossRef - Potential Signature Therapeutic Biomarkers TOP2A, MAD2L1, and CDK1 in Colorectal Cancer: A Systems Biomedicine-Based Approach
P. Priyamvada, Sudha Ramaiah
Biochemical Genetics.2024; 62(3): 2166. CrossRef - Neutralizing IL-16 enhances the efficacy of targeting Aurora-A therapy in colorectal cancer with high lymphocyte infiltration through restoring anti-tumor immunity
Shiang-Jie Yang, Sheng-Tsung Chang, Kung-Chao Chang, Bo-Wen Lin, Kwang-Yu Chang, Yao-Wen Liu, Ming-Derg Lai, Liang-Yi Hung
Cell Death & Disease.2024;[Epub] CrossRef - Development and validation of epigenetic modification-related signals for the diagnosis and prognosis of colorectal cancer
Xia Li, Jingjing Li, Jie Li, Nannan Liu, Liwei Zhuang
BMC Genomics.2024;[Epub] CrossRef - Recent Updates on Oncogenic Signaling of Aurora Kinases in
Chemosensitive, Chemoresistant Cancers: Novel Medicinal Chemistry
Approaches for Targeting Aurora Kinases
Pooja Kumari, Narasimha Murthy Beeraka, Anandkumar Tengli, Gurupadayya Bannimath, Ramandeep Kaur Baath, Mayuri Patil
Current Medicinal Chemistry.2024; 31(23): 3502. CrossRef - Identification of Aurora A kinase allosteric inhibitors: A comprehensive virtual screening through fingerprint-based similarity search, molecular docking, machine learning and molecular dynamics simulation
Mahima Sudhir Kolpe, Surbhi Pravin Pawar, Vikramsinh Sardarsinh Suryawanshi, Heba Taha M. Abdelghani, Pritee Chunarkar Patil, Shovonlal Bhowmick
Journal of Molecular Liquids.2024; 414: 126115. CrossRef - Exploring Core Genes by Comparative Transcriptomics Analysis for Early Diagnosis, Prognosis, and Therapies of Colorectal Cancer
Md. Ariful Islam, Md. Bayazid Hossen, Md. Abu Horaira, Md. Alim Hossen, Md. Kaderi Kibria, Md. Selim Reza, Khanis Farhana Tuly, Md. Omar Faruqe, Firoz Kabir, Rashidul Alam Mahumud, Md. Nurul Haque Mollah
Cancers.2023; 15(5): 1369. CrossRef - The Oncology Biomarker Discovery framework reveals cetuximab and bevacizumab response patterns in metastatic colorectal cancer
Alexander J. Ohnmacht, Arndt Stahler, Sebastian Stintzing, Dominik P. Modest, Julian W. Holch, C. Benedikt Westphalen, Linus Hölzel, Marisa K. Schübel, Ana Galhoz, Ali Farnoud, Minhaz Ud-Dean, Ursula Vehling-Kaiser, Thomas Decker, Markus Moehler, Matthias
Nature Communications.2023;[Epub] CrossRef - Disease Modeling on Tumor Organoids Implicates AURKA as a Therapeutic Target in Liver Metastatic Colorectal Cancer
Sophie L. Boos, Leon P. Loevenich, Sebastian Vosberg, Thomas Engleitner, Rupert Öllinger, Jörg Kumbrink, Matjaz Rokavec, Marlies Michl, Philipp A. Greif, Andreas Jung, Heiko Hermeking, Jens Neumann, Thomas Kirchner, Roland Rad, Peter Jung
Cellular and Molecular Gastroenterology and Hepatology.2022; 13(2): 517. CrossRef - Colorectal cancer on a dish: exploring the 3D-sphere culture of primary colorectal cancer cells from an Indonesian perspective
Murdani Abdullah, DR Noor, Amanda Pitarini Utari, Virly Nanda Muzellina, Nur Rahadiani, Radiana Dhewayani Antarianto
F1000Research.2022; 11: 182. CrossRef - Mitotic protein kinase-driven crosstalk of machineries for mitosis and metastasis
Chang-Hyeon Kim, Da-Eun Kim, Dae-Hoon Kim, Ga-Hong Min, Jung-Won Park, Yeo-Bin Kim, Chang K. Sung, Hyungshin Yim
Experimental & Molecular Medicine.2022; 54(4): 414. CrossRef - AURKA is a prognostic biomarker for good overall survival in stage II colorectal cancer patients
Peter Jung, David Horst, Thomas Kirchner, Frederick Klauschen, Jens Neumann
Pathology - Research and Practice.2022; 235: 153936. CrossRef - Therapeutic Potential of Mitotic Kinases’ Inhibitors in Cancers of the Gastrointestinal System
Aadil Javed, Gianluca Malagraba, Mahdieh Yarmohammadi, Catalina M. Perelló-Reus, Carles Barceló, Teresa Rubio-Tomás
Future Pharmacology.2022; 2(3): 214. CrossRef - Bioinformatics Analysis of RNA-seq Data Reveals Genes Related to Cancer Stem Cells in Colorectal Cancerogenesis
Kristian Urh, Nina Zidar, Emanuela Boštjančič
International Journal of Molecular Sciences.2022; 23(21): 13252. CrossRef - Unweaving the mitotic spindle: A focus on Aurora kinase inhibitors in lung cancer
Alessio Stefani, Geny Piro, Francesco Schietroma, Alessandro Strusi, Emanuele Vita, Simone Fiorani, Diletta Barone, Federico Monaca, Ileana Sparagna, Giustina Valente, Miriam Grazia Ferrara, Ettore D’Argento, Mariantonietta Di Salvatore, Carmine Carbone,
Frontiers in Oncology.2022;[Epub] CrossRef - Increased expression levels of AURKA and KIFC1 are promising predictors of progression and poor survival associated with gastric cancer
Jiyoon Jung, Hoiseon Jeong, Jung-Woo Choi, Hye-Sun Kim, Hwa Eun Oh, Eung Seok Lee, Young-Sik Kim, Ju-Han Lee
Pathology - Research and Practice.2021; 224: 153524. CrossRef - SALL Proteins; Common and Antagonistic Roles in Cancer
Claudia Álvarez, Aracelly Quiroz, Diego Benítez-Riquelme, Elizabeth Riffo, Ariel F. Castro, Roxana Pincheira
Cancers.2021; 13(24): 6292. CrossRef - AURKA gene polymorphisms and central nervous system tumor susceptibility in Chinese children
Yong-Ping Chen, Li Yuan, Hui-Ran Lin, Xiao-Kai Huang, Ji-Chen Ruan, Zhen-Jian Zhuo
Discover Oncology.2021;[Epub] CrossRef - Palmatine induces G2/M phase arrest and mitochondrial-associated pathway apoptosis in colon cancer cells by targeting AURKA
Xiaojiang Liu, Yaru Zhang, Siqi Wu, Minmin Xu, Youfeng Shen, Min Yu, Jinhua Fan, Sijia Wei, Chaohang Xu, Lu Huang, Han Zhao, Xuegang Li, Xiaoli Ye
Biochemical Pharmacology.2020; 175: 113933. CrossRef - New landscapes and horizons in hepatocellular carcinoma therapy
Melchiorre Cervello, Maria R. Emma, Giuseppa Augello, Antonella Cusimano, Lydia Giannitrapani, Maurizio Soresi, Shaw M. Akula, Stephen L. Abrams, Linda S. Steelman, Alessandro Gulino, Beatrice Belmonte, Giuseppe Montalto, James A. McCubrey
Aging.2020; 12(3): 3053. CrossRef - The New Paradigm of Network Medicine to Analyze Breast Cancer Phenotypes
Anna Maria Grimaldi, Federica Conte, Katia Pane, Giulia Fiscon, Peppino Mirabelli, Simona Baselice, Rosa Giannatiempo, Francesco Messina, Monica Franzese, Marco Salvatore, Paola Paci, Mariarosaria Incoronato
International Journal of Molecular Sciences.2020; 21(18): 6690. CrossRef - The GTEx Consortium atlas of genetic regulatory effects across human tissues
François Aguet, Shankara Anand, Kristin G. Ardlie, Stacey Gabriel, Gad A. Getz, Aaron Graubert, Kane Hadley, Robert E. Handsaker, Katherine H. Huang, Seva Kashin, Xiao Li, Daniel G. MacArthur, Samuel R. Meier, Jared L. Nedzel, Duyen T. Nguyen, Ayellet V.
Science.2020; 369(6509): 1318. CrossRef - Upregulation of aurora kinase A promotes vascular smooth muscle cell proliferation and migration by activating the GSK-3β/β-catenin pathway in aortic-dissecting aneurysms
Jia Meng, He-Liang Liu, Dong Ma, Hong-Yan Wang, Yue Peng, Hong-Li Wang
Life Sciences.2020; 262: 118491. CrossRef - Inhibition of AURKA Reduces Proliferation and Survival of Gastrointestinal Cancer Cells With Activated KRAS by Preventing Activation of RPS6KB1
Lihong Wang-Bishop, Zheng Chen, Ahmed Gomaa, Albert Craig Lockhart, Safia Salaria, Jialiang Wang, Keeli B. Lewis, Jeffrey Ecsedy, Kay Washington, Robert Daniel Beauchamp, Wael El-Rifai
Gastroenterology.2019; 156(3): 662. CrossRef - Discovery and Validation of Novel Biomarkers for Detection of Epithelial Ovarian Cancer
Hagen Kulbe, Raik Otto, Silvia Darb-Esfahani, Hedwig Lammert, Salem Abobaker, Gabriele Welsch, Radoslav Chekerov, Reinhold Schäfer, Duska Dragun, Michael Hummel, Ulf Leser, Jalid Sehouli, Elena Ioana Braicu
Cells.2019; 8(7): 713. CrossRef - Epigenetic regulation of AURKA by miR-4715-3p in upper gastrointestinal cancers
Ahmed Gomaa, Dunfa Peng, Zheng Chen, Mohammed Soutto, Khaled Abouelezz, Alejandro Corvalan, Wael El-Rifai
Scientific Reports.2019;[Epub] CrossRef - The functional diversity of Aurora kinases: a comprehensive review
Estelle Willems, Matthias Dedobbeleer, Marina Digregorio, Arnaud Lombard, Paul Noel Lumapat, Bernard Rogister
Cell Division.2018;[Epub] CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure




Fig. 1.
Fig. 2.
Fig. 3.
Fig. 4.
| Characteristic | No. (%) (n = 151) |
|---|---|
| Age (yr) | |
| < 65 | 60 (39.7) |
| ≥ 65 | 91 (60.3) |
| Sex | |
| Male | 104 (68.9) |
| Female | 47 (31.1) |
| Tumor location | |
| Proximal | 46 (30.5) |
| Distal | 105 (69.5) |
| Tumor differentiation | |
| Well | 18 (11.9) |
| Moderate | 122 (80.8) |
| Poor | 9 (6.0) |
| Mucinous | 2 (1.3) |
| Vascular invasion | |
| Absent | 140 (92.7) |
| Present | 11 (7.3) |
| Lymphatic invasion | |
| Absent | 82 (54.3) |
| Present | 69 (45.7) |
| Perineural invasion | |
| Absent | 105 (69.5) |
| Present | 46 (30.5) |
| TNM stage | |
| I | 22 (14.6) |
| II | 61 (40.4) |
| III | 68 (45) |
| 20q13.2–13.33 copy number gain | AURKA gene amplification |
||
|---|---|---|---|
| Positive | Negative | Total cases | |
| Positive | 3 | 6 | 9 |
| Negative | 0 | 5 | 5 |
| Total cases | 3 | 11 | 14 |
| Characteristic | Aurora kinase A expression |
p-value | |
|---|---|---|---|
| Positive | Negative | ||
| Age (yr) | .616 | ||
| <65 | 29 (48.3) | 31 (51.7) | |
| ≥65 | 39 (42.9) | 52 (57.1) | |
| Sex | .035 | ||
| Male | 53 (51.0) | 51 (49.0) | |
| Female | 15 (31.9) | 32 (68.1) | |
| Tumor location | .021 | ||
| Proximal | 14 (30.4) | 32 (69.6) | |
| Distal | 54 (51.4) | 51 (48.6) | |
| Tumor differentiation | .517 | ||
| Well | 8 (44.4) | 10 (55.6) | |
| Moderate | 57 (46.7) | 65 (53.3) | |
| Poor | 3 (33.3) | 6 (66.7) | |
| Mucinous | 0 | 2 (100) | |
| Vascular invasion | .755 | ||
| Absent | 64 (45.7) | 76 (54.3) | |
| Present | 4 (36.4) | 7 (63.6) | |
| Lymphatic invasion | .139 | ||
| Absent | 32 (39.0) | 50 (61.0) | |
| Present | 36 (52.2) | 33 (47.8) | |
| Perineural invasion | .288 | ||
| Absent | 44 (41.9) | 61 (58.1) | |
| Present | 24 (52.2) | 22 (47.8) | |
| TNM stage | .692 | ||
| I | 11 (50.0) | 11 (50.0) | |
| II | 25 (41.0) | 36 (59.0) | |
| III | 32 (47.1) | 36 (52.9) | |
| Factors | Hazard ratio (95% CI) | p-value |
|---|---|---|
| AURKA expression (positive vs negative) | 3.944 (1.821–8.542) | <.001 |
| Age (< 65 yr vs ≥ 65 yr) | 1.453 (0.726–2.907) | .291 |
| Lymphatic invasion (present vs absent) | 1.654 (0.707–3.867) | .246 |
| Perineural invasion (present vs absent) | 2.037 (1.017–4.079) | .045 |
| TNM stage (III vs I or II) | 1.489 (0.688–3.224) | .312 |
TNM, tumor-node-metastasis.
Values are presented as numbers (%). TNM, tumor-node-metastasis.
CI, confidence interval; AURKA, Aurora kinase A; TNM, tumor-node-metastasis.

 E-submission
E-submission