Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 51(3); 2017 > Article
-
Original Article
Overexpression of POSTN in Tumor Stroma Is a Poor Prognostic Indicator of Colorectal Cancer - Hyeon Jeong Oh1,2, Jeong Mo Bae2,3, Xian-Yu Wen2, Nam-Yun Cho2, Jung Ho Kim1,2, Gyeong Hoon Kang1,2
-
Journal of Pathology and Translational Medicine 2017;51(3):306-313.
DOI: https://doi.org/10.4132/jptm.2017.01.19
Published online: April 12, 2017
1Department of Pathology, Seoul National University College of Medicine, Seoul, Korea
2Laboratory of Epigenetics, Cancer Research Institute, Seoul National University College of Medicine, Seoul, Korea
3Department of Pathology, SMG-SNU Boramae Medical Center, Seoul, Korea
- Corresponding Author Gyeong Hoon Kang, MD Department of Pathology, Seoul National University College of Medicine, 103 Daehak-ro, Jongno-gu, Seoul 03080, Korea Tel: +82-2-740-8263 Fax: +82-2-765-5600 E-mail: ghkang@snu.ac.kr
© 2017 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Figure & Data
References
Citations

- Exploring Molecular Signature and Prognostic Biomarkers in Ovarian Cancer: Insights From Late‐Stage, Recurrent, and Metastatic Tumors
Vandana Yadav, Aruna Sivaram, Renu Vyas
Biotechnology and Applied Biochemistry.2026;[Epub] CrossRef - Exosomal Dialogue: The Emerging Role of Cancer‐Associated Fibroblast‐Derived Exosomes in Colorectal Cancer Progression and Therapy Resistance
Ahmed Hjazi, Raed Obaid Saleh, Zahraa Abbas Al‐Khafaji, Ali G. Alkhathami, Malathi.H, Mayank Kundlas, Laxmidhar Maharana, Ashish Singh Chauhan, Yasser Fakri Mustafa, Hamza Fadhel Hamzah
Journal of Biochemical and Molecular Toxicology.2026;[Epub] CrossRef - Super‐Enhancer Formation in Scirrhous Gastric CAFs, and the Presence of a Stromal Field in Non‐Cancerous Tissues
Yoshimi Yasukawa, Naoko Hattori, Yu‐Yu Liu, Masayuki Tobo, Genki Yamagishi, Takahiro Irie, Shigeki Sekine, Tohru Kiyono, Satoshi Yamashita, Yukinori Yamagata, Takaki Yoshikawa, Yasuyuki Seto, Toshikazu Ushijima
Cancer Science.2026;[Epub] CrossRef - Unmasking a Recessive Allele by a Rare Interstitial Deletion at 10q26.13q26.2: Prenatal Diagnosis of MMP21 ‐Related Disorder and Further Refine INSYN2A Involvement in the Postnatal Cognitive Phenotype
Jiasun Su, Shujie Zhang, Wei Li, Yuan Wei, Fei Lin, Chaofan Zhou, Xianglian Tang, Yueyun Lan, Minpan Huang, Qiang Zhang, Shang Yi, Qi Yang, Sheng Yi, Xunzhao Zhou, Zailong Qin, Peng Huang
Molecular Genetics & Genomic Medicine.2025;[Epub] CrossRef - Periostin from Tumor Stromal Cells Might Be Associated with Malignant Progression of Colorectal Cancer via Smad2/3
Canfeng Fan, Qiang Wang, Saki Kanei, Kyoka Kawabata, Hinano Nishikubo, Rika Aoyama, Zhonglin Zhu, Daiki Imanishi, Takashi Sakuma, Koji Maruo, Gen Tsujio, Yurie Yamamoto, Tatsunari Fukuoka, Masakazu Yashiro
Cancers.2025; 17(3): 551. CrossRef - Attributes of HPV associated cancers
Ashi Robert Thobias, Mrugdha Patel, Chirag Vaghela, Prabhudas Shankarbhai Patel
Clinical and Translational Oncology.2025; 27(11): 4131. CrossRef - The association between periostin and tumor microenvironment: a promising cancer prognostic biomarker and therapeutic target to combat tumor progression and chemoresistance
Mohsen Nabi-Afjadi, Farnoosh Farzam, Sina Soltani, Nafiseh Golestani, Shiva Sarani Asl, Fatemeh Aziziyan, Hamidreza Zalpoor, Fatemeh Ghasemi, Bahareh Dabirmanesh, Khosro Khajeh
Cancer Cell International.2025;[Epub] CrossRef - Cancer-associated fibroblasts and their prognostic role in colorectal cancer: review and meta-analysis
Silvia Mihaela Ilie, Laurentia Gales, Ana Maria Musina, Kevin Rouet, Alexandra Elena Stefan, Mara Simona Belceanu, Anda Stefania Trandafir, Constantin Guillaume, Aurélie Bertaut, Ikram Charifi, Adel Cueff, Valentin Derangère, Francois Ghiringhelli
Frontiers in Oncology.2025;[Epub] CrossRef - Electroanalytical Immunotool to Determine Matricellular Protein Periostin, a Stromal Biomarker of Prognosis in Colorectal Cancer
Marina Blázquez‐García, Jennifer Quinchia, Víctor Ruiz‐Valdepeñas Montiel, Rebeca M. Torrente‐Rodríguez, Verónica Serafín, María Garranzo‐Asensio, Ana García‐Romero, Jahir Orozco, Rodrigo Barderas, José M. Pingarrón, Susana Campuzano
ChemElectroChem.2024;[Epub] CrossRef - Simultaneous Expression of CD70 and POSTN in Cancer-Associated Fibroblasts Predicts Worse Survival of Colorectal Cancer Patients
Masayuki Komura, Chengbo Wang, Sunao Ito, Shunsuke Kato, Akane Ueki, Masahide Ebi, Naotaka Ogasawara, Toyonori Tsuzuki, Kenji Kasai, Kunio Kasugai, Shuji Takiguchi, Satoru Takahashi, Shingo Inaguma
International Journal of Molecular Sciences.2024; 25(5): 2537. CrossRef - The combined tumour-based Fascin/Snail and stromal periostin reveals the effective prognosis prediction in colorectal cancer patients
Niphat Jirapongwattana, Suyanee Thongchot, Ananya Pongpaibul, Atthaphorn Trakarnsanga, Jean Quinn, Peti Thuwajit, Chanitra Thuwajit, Joanne Edwards, Peng Zhang
PLOS ONE.2024; 19(6): e0304666. CrossRef - SPOCK1 and POSTN are valuable prognostic biomarkers and correlate with tumor immune infiltrates in colorectal cancer
Caiqin Gan, Mengting Li, Yuanyuan Lu, Ganjing Peng, Wenjie Li, Haizhou Wang, Yanan Peng, Qian Hu, Wanhui Wei, Fan Wang, Lan Liu, Qiu Zhao
BMC Gastroenterology.2023;[Epub] CrossRef - Stromal POSTN Enhances Motility of Both Cancer and Stromal Cells and Predicts Poor Survival in Colorectal Cancer
Akane Ueki, Masayuki Komura, Akira Koshino, Chengbo Wang, Kazuhiro Nagao, Mai Homochi, Yuki Tsukada, Masahide Ebi, Naotaka Ogasawara, Toyonori Tsuzuki, Kenji Kasai, Kunio Kasugai, Satoru Takahashi, Shingo Inaguma
Cancers.2023; 15(3): 606. CrossRef - POSTN Secretion by Extracellular Matrix Cancer-Associated Fibroblasts (eCAFs) Correlates with Poor ICB Response via Macrophage Chemotaxis Activation of Akt Signaling Pathway in Gastric Cancer
Tingting You, Hui Tang, Wenjing Wu, Jingxi Gao, Xuechun Li, Ningning Li, Xiuxiu Xu, Jiazhang Xing, Hui Ge, Yi Xiao, Junchao Guo, Bin Wu, Xiaoyi Li, Liangrui Zhou, Lin Zhao, Chunmei Bai, Qin Han, Zhao Sun, Robert Chunhua Zhao
Aging and disease.2023; 14(6): 2177. CrossRef - A Pan-cancer Analysis Reveals the Tissue Specificity and Prognostic Impact
of Angiogenesis-associated Genes in Human Cancers
Zhenshen Bao, Minzhen Liao, Wanqi Dong, Yanhao Huo, Xianbin Li, Peng Xu, Wenbin Liu
Current Bioinformatics.2023; 18(8): 670. CrossRef - Cancer‐associated stroma reveals prognostic biomarkers and novel insights into the tumour microenvironment of colorectal cancer and colorectal liver metastases
Kai M. Brown, Aiqun Xue, Ross C. Smith, Jaswinder S. Samra, Anthony J. Gill, Thomas J. Hugh
Cancer Medicine.2022; 11(2): 492. CrossRef - Periostin in Angiogenesis and Inflammation in CRC—A Preliminary Observational Study
Agnieszka Kula, Miriam Dawidowicz, Sylwia Mielcarska, Paweł Kiczmer, Magdalena Chrabańska, Magdalena Rynkiewicz, Elżbieta Świętochowska, Dariusz Waniczek
Medicina.2022; 58(1): 96. CrossRef - Periostin promotes the proliferation and metastasis of osteosarcoma by increasing cell survival and activates the PI3K/Akt pathway
Chaojian Xu, Ziyue Wang, Long Zhang, Yi Feng, Jia Lv, Zhuangzhuang Wu, Rong Yang, Taiyong Wu, Jian Li, Ruhao Zhou, Zhi Tian, Junjun Bai, Huadong Zhang, Yanping Lan, Zhi Lv
Cancer Cell International.2022;[Epub] CrossRef - Periostin in lymph node pre-metastatic niches governs lymphatic endothelial cell functions and metastatic colonization
Lionel Gillot, Alizée Lebeau, Louis Baudin, Charles Pottier, Thomas Louis, Tania Durré, Rémi Longuespée, Gabriel Mazzucchelli, Christophe Nizet, Silvia Blacher, Frédéric Kridelka, Agnès Noël
Cellular and Molecular Life Sciences.2022;[Epub] CrossRef - Prognostic impact of stromal periostin expression in upper urinary tract urothelial carcinoma
Kosuke Miyai, Kazuki Kawamura, Keiichi Ito, Susumu Matsukuma, Hitoshi Tsuda
BMC Cancer.2022;[Epub] CrossRef - Periostin‐ and podoplanin‐positive cancer‐associated fibroblast subtypes cooperate to shape the inflamed tumor microenvironment in aggressive pancreatic adenocarcinoma
Cindy Neuzillet, Rémy Nicolle, Jérôme Raffenne, Annemilaï Tijeras‐Raballand, Alexia Brunel, Lucile Astorgues‐Xerri, Sophie Vacher, Floriane Arbateraz, Marjorie Fanjul, Marc Hilmi, Rémi Samain, Christophe Klein, Aurélie Perraud, Vinciane Rebours, Muriel Ma
The Journal of Pathology.2022; 258(4): 408. CrossRef - Periostin: biology and function in cancer
Shima Dorafshan, Mahdieh Razmi, Sadegh Safaei, Erica Gentilin, Zahra Madjd, Roya Ghods
Cancer Cell International.2022;[Epub] CrossRef - Periostin as a key molecule defining desmoplastic environment in colorectal cancer
Takahiro Sueyama, Yoshiki Kajiwara, Satsuki Mochizuki, Hideyuki Shimazaki, Eiji Shinto, Kazuo Hase, Hideki Ueno
Virchows Archiv.2021; 478(5): 865. CrossRef - Expression Patterns of Microenvironmental Factors and Tenascin-C at the Invasive Front of Stage II and III Colorectal Cancer: Novel Tumor Prognostic Markers
Mai Hashimoto, Noriyuki Uesugi, Mitsumasa Osakabe, Naoki Yanagawa, Koki Otsuka, Yoshiki Kajiwara, Hideki Ueno, Akira Sasaki, Tamotsu Sugai
Frontiers in Oncology.2021;[Epub] CrossRef - Deregulation of extracellular matrix modeling with molecular prognostic markers revealed by transcriptome sequencing and validations in Oral Tongue squamous cell carcinoma
Soundara Viveka Thangaraj, Vidyarani Shyamsundar, Arvind Krishnamurthy, Vijayalakshmi Ramshankar
Scientific Reports.2021;[Epub] CrossRef - Inhibition of Postn Rescues Myogenesis Defects in Myotonic Dystrophy Type 1 Myoblast Model
Xiaopeng Shen, Zhongxian Liu, Chunguang Wang, Feng Xu, Jingyi Zhang, Meng Li, Yang Lei, Ao Wang, Chao Bi, Guoping Zhu
Frontiers in Cell and Developmental Biology.2021;[Epub] CrossRef - Radiographical assessment of tumour stroma and treatment outcomes using deep learning: a retrospective, multicohort study
Yuming Jiang, Xiaokun Liang, Zhen Han, Wei Wang, Sujuan Xi, Tuanjie Li, Chuanli Chen, Qingyu Yuan, Na Li, Jiang Yu, Yaoqin Xie, Yikai Xu, Zhiwei Zhou, George A Poultsides, Guoxin Li, Ruijiang Li
The Lancet Digital Health.2021; 3(6): e371. CrossRef - Periostin expression and its supposed roles in benign and malignant thyroid nodules: an immunohistochemical study of 105 cases
Kimihide Kusafuka, Masaru Yamashita, Tomohiro Iwasaki, Chinatsu Tsuchiya, Aki Kubota, Kazuki Hirata, Akinori Murakami, Aya Muramatsu, Kazumori Arai, Makoto Suzuki
Diagnostic Pathology.2021;[Epub] CrossRef - Cancer-associated fibroblasts in colorectal cancer
S. Kamali Zonouzi, P. S. Pezeshki, S. Razi, N. Rezaei
Clinical and Translational Oncology.2021; 24(5): 757. CrossRef - Prognostic value of periostin in multiple solid cancers: A systematic review with meta‐analysis
Tao Yang, Zhengdong Deng, Zhongya Pan, Yawei Qian, Wei Yao, Jianming Wang
Journal of Cellular Physiology.2020; 235(3): 2800. CrossRef - Serum periostin is associated with cancer mortality but not cancer risk in older home-dwelling men: A 8-year prospective analysis of the STRAMBO study
Jean-Charles Rousseau, Cindy Bertholon, Roland Chapurlat, Pawel Szulc
Bone.2020; 132: 115184. CrossRef - Systematic prediction of key genes for ovarian cancer by co‐expression network analysis
Mingyuan Wang, Jinjin Wang, Jinglan Liu, Lili Zhu, Heng Ma, Jiang Zou, Wei Wu, Kangkai Wang
Journal of Cellular and Molecular Medicine.2020; 24(11): 6298. CrossRef - Upregulation of adipocyte enhancer‐binding protein 1 in endothelial cells promotes tumor angiogenesis in colorectal cancer
Akira Yorozu, Eiichiro Yamamoto, Takeshi Niinuma, Akihiro Tsuyada, Reo Maruyama, Hiroshi Kitajima, Yuto Numata, Masahiro Kai, Gota Sudo, Toshiyuki Kubo, Toshihiko Nishidate, Kenji Okita, Ichiro Takemasa, Hiroshi Nakase, Tamotsu Sugai, Kenichi Takano, Hiro
Cancer Science.2020; 111(5): 1631. CrossRef - Periostin aggravates NLRP3 inflammasome-mediated pyroptosis in myocardial ischemia-reperfusion injury
Lei Yao, Jie Song, Xiao wen Meng, Jian yun Ge, Bo xiang Du, Jun Yu, Fu hai Ji
Molecular and Cellular Probes.2020; 53: 101596. CrossRef - Vitamin K and Kidney Transplantation
Maria Fusaro, Laura Cosmai, Pieter Evenepoel, Thomas L. Nickolas, Angela M. Cheung, Andrea Aghi, Giovanni Tripepi, Mario Plebani, Giorgio Iervasi, Roberto Vettor, Martina Zaninotto, Maura Ravera, Marina Foramitti, Sandro Giannini, Stefania Sella, Maurizio
Nutrients.2020; 12(9): 2717. CrossRef - Periostin regulates autophagy through integrin α5β1 or α6β4 and an AKT‐dependent pathway in colorectal cancer cell migration
Suyanee Thongchot, Ekapot Singsuksawat, Nuttavut Sumransub, Ananya Pongpaibul, Attaporn Trakarnsanga, Peti Thuwajit, Chanitra Thuwajit
Journal of Cellular and Molecular Medicine.2020; 24(21): 12421. CrossRef - Genomic, transcriptomic, and viral integration profiles associated with recurrent/metastatic progression in high‐risk human papillomavirus cervical carcinomas
Jing Jing Liu, Jung Yoon Ho, Jung Eum Lee, Soo Young Hur, Jinseon Yoo, Kyu Ryung Kim, Daeun Ryu, Tae Min Kim, Youn Jin Choi
Cancer Medicine.2020; 9(21): 8243. CrossRef - Periostin Secreted by Carcinoma-Associated Fibroblasts Promotes Ovarian Cancer Cell Platinum Resistance Through the PI3K/Akt Signaling Pathway
Lei Chu, Fangce Wang, Wenjun Zhang, Huai-fang Li, Jun Xu, Xiao-wen Tong
Technology in Cancer Research & Treatment.2020;[Epub] CrossRef - Overexpression of periostin is positively associated with gastric cancer metastasis through promoting tumor metastasis and invasion
Hai Zhong, Xiang Li, Junhua Zhang, Xu Wu
Journal of Cellular Biochemistry.2019; 120(6): 9927. CrossRef - Genes associated with bowel metastases in ovarian cancer
Andrea Mariani, Chen Wang, Ann L. Oberg, Shaun M. Riska, Michelle Torres, Joseph Kumka, Francesco Multinu, Gunisha Sagar, Debarshi Roy, Deok–Beom Jung, Qing Zhang, Tommaso Grassi, Daniel W. Visscher, Vatsal P. Patel, Ling Jin, Julie K. Staub, William A. C
Gynecologic Oncology.2019; 154(3): 495. CrossRef - Periostin: A Matricellular Protein With Multiple Functions in Cancer Development and Progression
Laura González-González, Javier Alonso
Frontiers in Oncology.2018;[Epub] CrossRef - Upregulation of Periostin expression in the pathogenesis of ameloblastoma
Yuanyuan Kang, Jie Liu, Ying Zhang, Yan Sun, Junting Wang, Biying Huang, Ming Zhong
Pathology - Research and Practice.2018; 214(12): 1959. CrossRef - Periostin expression in neoplastic and non-neoplastic diseases of bone and joint
Jennifer M. Brown, Akiro Mantoku, Afsie Sabokbar, Udo Oppermann, A. Bass Hassan, Akiro Kudo, Nick Athanasou
Clinical Sarcoma Research.2018;[Epub] CrossRef - Molecular patterns of cancer colonisation in lymph nodes of breast cancer patients
Gaurav Chatterjee, Trupti Pai, Thomas Hardiman, Kelly Avery-Kiejda, Rodney J. Scott, Jo Spencer, Sarah E. Pinder, Anita Grigoriadis
Breast Cancer Research.2018;[Epub] CrossRef - Multiplicity of Advanced T Category–Tumors Is a Risk Factor for Survival in Patients with Colorectal Carcinoma
Hye Eun Park, Seungyeon Yoo, Jeong Mo Bae, Seorin Jeong, Nam-Yun Cho, Gyeong Hoon Kang
Journal of Pathology and Translational Medicine.2018; 52(6): 386. CrossRef - Periostin attenuates tumor growth by inducing apoptosis in colitis-related colorectal cancer
Yusuke Shimoyama, Keiichi Tamai, Rie Shibuya, Mao Nakamura, Mai Mochizuki, Kazunori Yamaguchi, Yoichi Kakuta, Yoshitaka Kinouchi, Ikuro Sato, Akira Kudo, Tooru Shimosegawa, Kennichi Satoh
Oncotarget.2018; 9(28): 20008. CrossRef - Periostin serves an important role in the pathogenesis of oral squamous cell carcinoma
Yuanyuan Kang, Xue Wang, Ying Zhang, Yan Sun
Oncology Letters.2018;[Epub] CrossRef - The prognostic significance of cancer-associated fibroblasts in pancreatic ductal adenocarcinoma
Hyunjin Park, Yangkyu Lee, Hyejung Lee, Jin-Won Kim, Jin-Hyeok Hwang, Jaihwan Kim, Yoo-Seok Yoon, Ho-Seong Han, Haeryoung Kim
Tumor Biology.2017; 39(10): 101042831771840. CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure


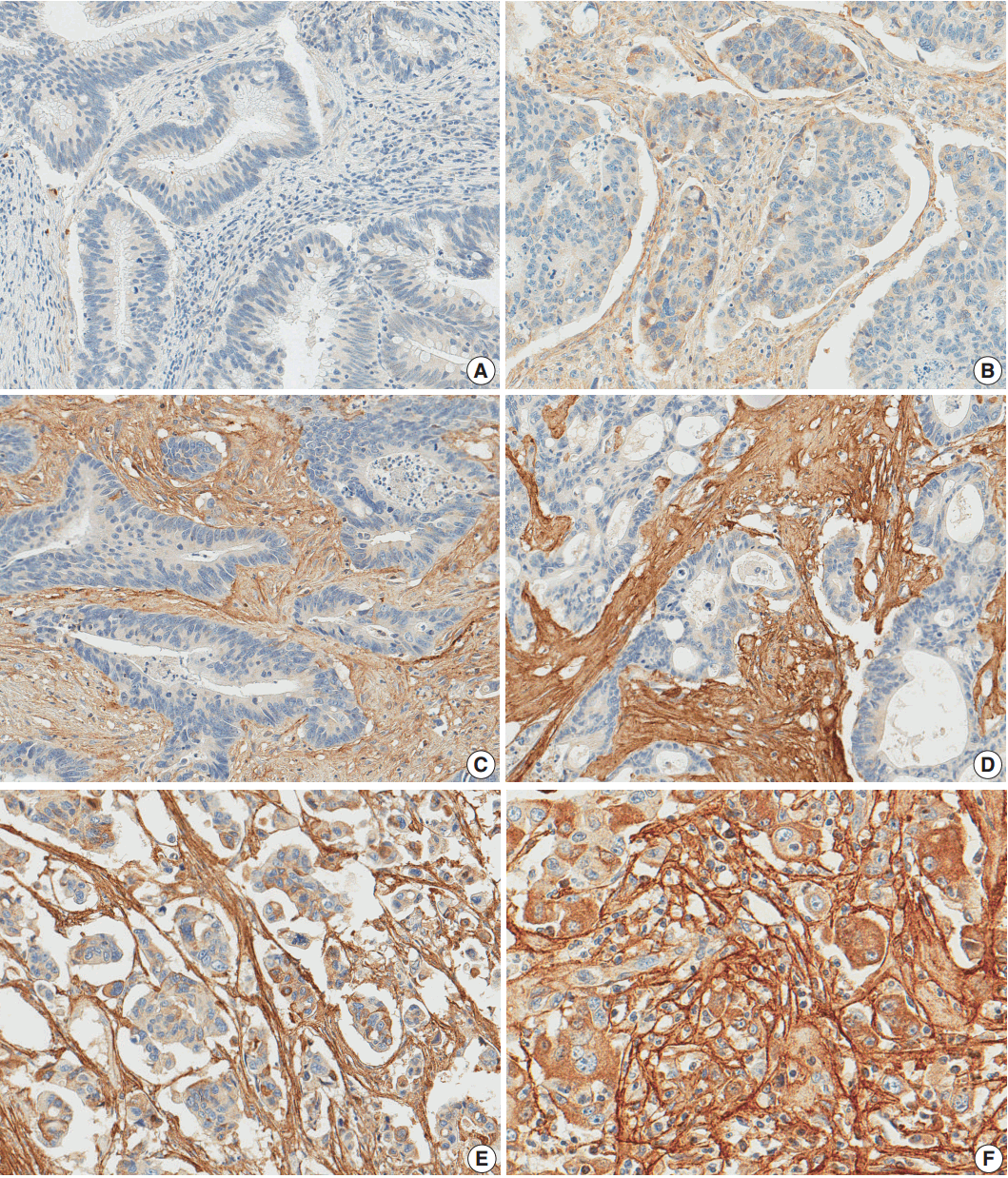
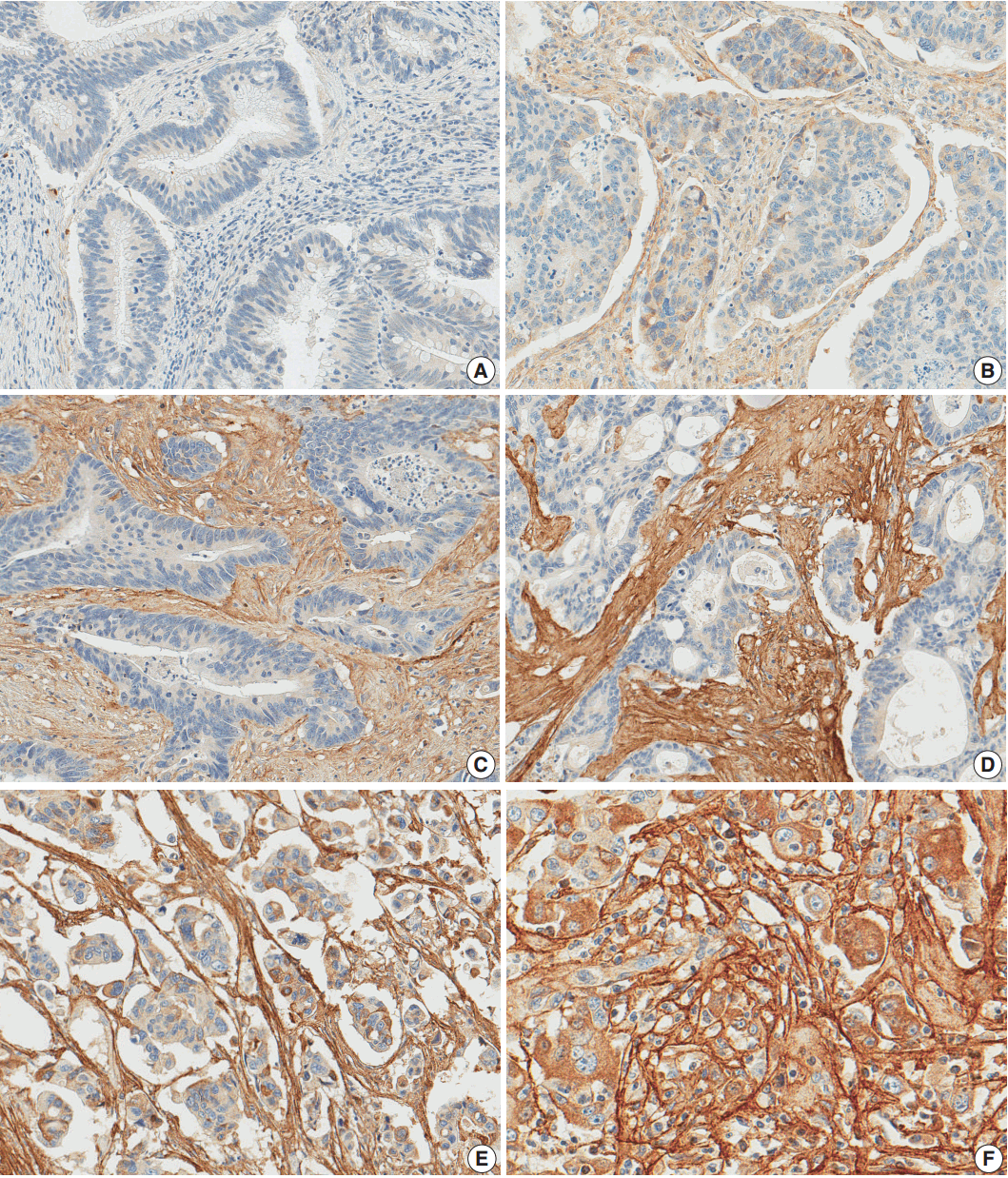
Fig. 1.
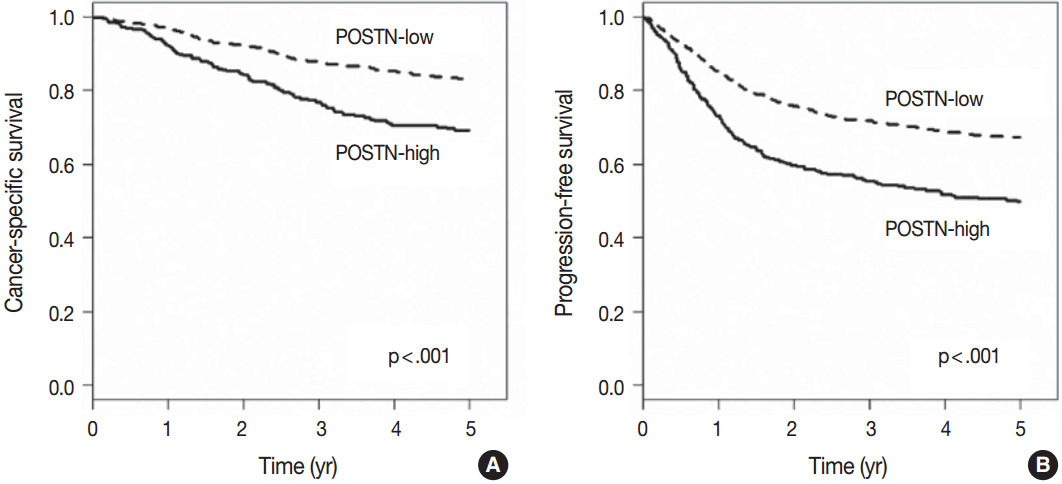
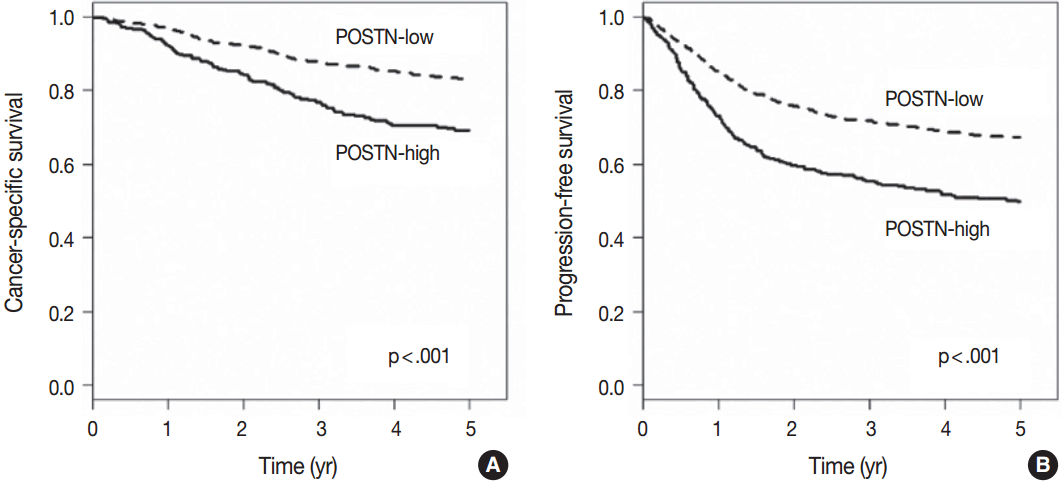
Fig. 2.
| Variable | POSTN-low (n = 821, 73.0%) | POSTN-high (n = 304, 27.0%) | p-value | |
|---|---|---|---|---|
| Age (yr) | 62 (20–87) | 62 (29–90) | .932 | |
| Sex | Male | 500 (60.9) | 173 (56.9) | .225 |
| Female | 321 (39.1) | 131 (43.1) | ||
| Location | Proximal | 170 (20.7) | 107 (35.2) | < .001 |
| Distal | 336 (40.9) | 102 (33.5) | ||
| Rectum | 315 (38.4) | 95 (31.3) | ||
| Growth pattern | Fungating | 569 (69.3) | 168 (55.3) | < .001 |
| Fungating | 252 (30.7) | 136 (44.7) | ||
| T category | T1,2 | 192 (23.4) | 18 (5.9) | < .001 |
| T3,4 | 629 (76.6) | 286 (94.1) | ||
| N category | N0 | 454 (55.3) | 117 (38.5) | < .001 |
| N1,2 | 367 (44.7) | 187 (61.5) | ||
| M category | 0 | 712 (86.7) | 222 (73.0) | < .001 |
| 1 | 109 (13.3) | 82 (27.0) | ||
| Stage | I, II | 432 (52.6) | 104 (34.2) | < .001 |
| III, IV | 109 (13.3) | 200 (65.8) | ||
| Differentiation | Differentiated | 802 (97.7) | 284 (93.4) | .001 |
| Undifferentiated | 19 (2.3) | 20 (6.6) | ||
| Tumor budding | Absent | 261 (31.8) | 58 (19.1) | < .001 |
| Present | 560 (68.2) | 246 (80.9) | ||
| Dirty necrosis | Absent | 85 (10.4) | 17 (5.6) | .014 |
| Present | 736 (89.6) | 287 (94.4) | ||
| Crohn-like reaction | Absent | 703 (85.6) | 251 (82.6) | .204 |
| Present | 118 (14.4) | 53 (17.4) | ||
| Tumor-infiltrating lymphocytes | High (≥ 8/HPF) | 599 (73.0) | 233 (76.6) | .211 |
| Low (< 8/HPF) | 222 (27.0) | 71 (23.4) | ||
| Serration | Absent | 793 (96.6) | 288 (94.7) | .155 |
| Present | 28 (3.4) | 16 (5.3) | ||
| Mucin production | Absent | 727 (88.5) | 265 (87.2) | .525 |
| Present | 94 (11.5) | 39 (12.8) | ||
| CIMP | CIMP-0 | 387 (47.1) | 123 (40.5) | .030 |
| CIMP-low | 396 (48.2) | 157 (51.6) | ||
| CIMP-high | 38 (4.6) | 24 (7.9) | ||
| MSI | MSS | 702 (85.5) | 262 (86.2) | .959 |
| MSI-low | 54 (6.6) | 19 (6.2) | ||
| MSI-high | 65 (7.9) | 23 (7.6) | ||
| KRAS mutation | Wild type | 602 (73.3) | 210 (69.1) | .158 |
| Mutant | 219 (26.7) | 94 (30.9) | ||
| BRAF mutation (n = 1,124) | Wild type | 791 (96.5) | 285 (93.7) | .046 |
| Mutant | 29 (3.5) | 19 (6.3) |
| Variable | Univariate |
Multivariate |
||
|---|---|---|---|---|
| HR | p-value | HR | p-value | |
| Gross (infiltrative/fungating) | 1.87 (1.32–2.66) | < .001 | 1.64 (1.24–2.18) | .001 |
| Stage (III, IV/I, II) | 4.52 (3.26–6.26) | < .001 | 6.30 (4.27–9.29) | < .001 |
| Differentiation (PD/WD, MD) | 3.41 (2.05–5.67) | < .001 | 2.15 (1.27–3.62) | .013 |
| BRAF (mutant/wild type) | 1.92 (1.15–3.19) | .012 | 1.92 (1.11–3.34) | .041 |
| Chemotherapy (treated/not-treated) | 0.94 (0.71–1.25) | .655 | 0.38 (0.28–0.52) | < .001 |
| POSTN (high/low) | 2.00 (1.52–2.64) | < .001 | 1.50 (1.13–2.00) | .006 |
| Tumor location (right/left) | 1.56 (1.19–2.06) | .002 | 1.46 (1.09–1.96) | .011 |
| Tumor-infiltrating lymphocytes (high/low) | 0.69 (0.49–0.97) | .032 | - | .051 |
| Budding (present/absent) | 1.90 (1.36–2.66) | < .001 | - | .129 |
| Crohn-like reaction (present/absent) | 0.71 (0.48–1.06) | .095 | - | .305 |
| Age (≥ 65 yr/< 65 yr) | 1.49 (1.15–1.93) | .003 | - | .053 |
| CIMP (CIMP-H/CIMP-0, L) | 1.91 (1.21–3.02) | .006 | - | .632 |
| Sex (male/female) | 1.04 (0.80–1.36) | .762 | - | - |
| Necrosis (present/absent) | 1.11 (0.70–1.78) | .652 | - | - |
| Serration (present/absent) | 1.42 (0.80–2.54) | .235 | - | - |
| Mucin (present/absent) | 1.32 (0.92–1.90) | .136 | - | - |
| MSI (MSI-H/MSS, MSI-L) | 0.82 (0.48–1.41) | .476 | - | - |
| KRAS (mutant/wild type) | 1.12 (0.84–1.49) | .440 | - | - |
| Variable | Univariate |
Multivariate |
||
|---|---|---|---|---|
| HR (95% CI) | p-value | HR (95% CI) | p-value | |
| Gross (infiltrative/fungating) | 1.96 (1.61–2.39) | < .001 | 1.43 (1.17–1.76) | .001 |
| Stage (III, IV/I, II) | 4.72 (3.71–6.02) | < .001 | 4.75 (3.63–6.23) | < .001 |
| Differentiation (PD/WD, MD) | 3.32 (2.28–4.85) | < .001 | 1.85 (1.26–2.71) | .002 |
| BRAF (mutant/wild type) | 1.61 (1.06–2.45) | .027 | 1.72 (1.12–2.63) | .013 |
| Chemotherapy (treated/not-treated) | 1.40 (1.11–1.76) | .004 | 0.59 (0.46–0.76) | < .001 |
| POSTN (high/low) | 1.80 (1.47–2.20) | < .001 | 1.40 (1.08–1.83) | .012 |
| Budding (present/absent) | 2.15 (1.66–2.79) | < .001 | 1.51 (1.15–1.97) | .003 |
| Crohn-like reaction (present/absent) | 0.72 (0.53–0.98) | .034 | - | .302 |
| Tumor-infiltrating lymphocytes (high/low) | 0.70 (0.55–0.89) | .004 | - | .089 |
| Tumor location (right/left) | 1.22 (0.98–1.51) | .080 | - | .773 |
| Age (≥ 6 yr/< 65 yr) | 1.22 (1.00–1.49) | .046 | - | .098 |
| CIMP (CIMP-H/CIMP-0, L) | 1.44 (0.98–2.12) | .061 | - | .277 |
| Sex (male/female) | 0.94 (0.77–1.14) | .514 | - | - |
| Necrosis (present/absent) | 1.14 (0.80–1.62) | .463 | - | - |
| Serration (present/absent) | 1.32 (0.83–2.08) | .244 | - | - |
| Mucin (present/absent) | 1.12 (0.84–1.50) | .448 | - | - |
| MSI (MSI-H/MSS, MSI-L) | 0.80 (0.54–1.20) | .285 | - | - |
| KRAS (mutant/wild type) | 1.05 (0.85–1.31) | .633 | - | - |
Values are presented as median (range) or number (%). POSTN, periostin; HPF, high-power field; CIMP, CpG island methylator phenotype; MSI, microsatellite instability.
HR, hazard ratio; PD, poorly differentiated; WD, well differentiated; MD, moderately differentiated; POSTN, periostin; CIMP, CpG island methylator phenotype; CIMP-H, CIMP-high; CIMP-L, CIMP-low; MSI, microsatellite instability; MSI-H, MSI-high; MSS, microsatellite stable; MSI-L, MSI-low.
HR, hazard ratio; CI, confidence interval; PD, poorly differentiated; WD, well differentiated; MD, moderately differentiated; POSTN, periostin; CIMP, CpG island methylator phenotype; CIMP-H, CIMP-high; MSI, microsatellite instability; MSI-H, MSI-high; MSS, microsatellite stable; MSI-L, MSI-low.

 E-submission
E-submission