Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 54(2); 2020 > Article
-
Original Article
Programmed death-ligand 1 expression and its correlation with clinicopathological parameters in gallbladder cancer -
Ji Hye Kim1
 , Kyungbin Kim1
, Kyungbin Kim1 , Misung Kim1
, Misung Kim1 , Young Min Kim1,2
, Young Min Kim1,2 , Jae Hee Suh1,2
, Jae Hee Suh1,2 , Hee Jeong Cha1,2
, Hee Jeong Cha1,2 , Hye Jeong Choi1,2
, Hye Jeong Choi1,2
-
Journal of Pathology and Translational Medicine 2020;54(2):154-164.
DOI: https://doi.org/10.4132/jptm.2019.11.13
Published online: February 10, 2020
1Department of Pathology, Ulsan University Hospital, Ulsan, Korea
2University of Ulsan College of Medicine, Ulsan, Korea
- Corresponding Author: Hye Jeong Choi, MD, PhD, Department of Pathology, Ulsan University Hospital, University of Ulsan College of Medicine, 877 Bangeojinsunwhando-ro, Dong-gu, Ulsan 05505, Korea Tel: +82-52-250-7264, Fax: +82-52-252-3024, E-mail: thanksg@uuh.ulsan.kr
© 2020 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Figure & Data
References
Citations

- A novel machine learning-based model for precise prediction of postoperative recurrence in gallbladder cancer: development and multicenter validation across four centers
Jiajia He, Weilv Xiong, Hongxia Chen, Qunyan Pan, Weiyue Ji
World Journal of Surgical Oncology.2026;[Epub] CrossRef - PD-L1 Expression in Biliary Tract Cancer: Comparison Across Antibody Clones and Role as a Predictor of Response to Chemoimmunotherapy: A Meta-Analysis
Juan J. Juarez-Vignon Whaley, Soravis Osataphan, Ben Ponvilawan, Nipith Charoenngam, Mary Linton Peters
JCO Precision Oncology.2025;[Epub] CrossRef - An MRI-based model for preoperative prediction of tertiary lymphoid structures in patients with gallbladder cancer
Ying Xu, Zhuo Li, Weihua Zhi, Yi Yang, Jingzhong Ouyang, Yanzhao Zhou, Zeliang Ma, Sicong Wang, Lizhi Xie, Jianming Ying, Jinxue Zhou, Xinming Zhao, Feng Ye
Insights into Imaging.2025;[Epub] CrossRef - Lacking Immunotherapy Biomarkers for Biliary Tract Cancer: A Comprehensive Systematic Literature Review and Meta-Analysis
Giorgio Frega, Fernando P. Cossio, Jesus M. Banales, Vincenzo Cardinale, Rocio I. R. Macias, Chiara Braconi, Angela Lamarca
Cells.2023; 12(16): 2098. CrossRef - Gallbladder carcinomas: review and updates on morphology, immunohistochemistry, and staging
Whayoung Lee, Vishal S. Chandan
Human Pathology.2023; 132: 149. CrossRef - Prognostic Relevance of PDL1 and CA19-9 Expression in Gallbladder Cancer vs. Inflammatory Lesions
Neetu Rawal, Supriya Awasthi, Nihar Ranjan Dash, Sunil Kumar, Prasenjit Das, Amar Ranjan, Anita Chopra, Maroof Ahmad Khan, Sundeep Saluja, Showket Hussain, Pranay Tanwar
Current Oncology.2023; 30(2): 1571. CrossRef - Identification of genes associated with gall bladder cell carcinogenesis: Implications in targeted therapy of gall bladder cancer
Ishita Ghosh, Ruma Dey Ghosh, Soma Mukhopadhyay
World Journal of Gastrointestinal Oncology.2023; 15(12): 2053. CrossRef - CD73 and PD-L1 as Potential Therapeutic Targets in Gallbladder Cancer
Lu Cao, Kim R. Bridle, Ritu Shrestha, Prashanth Prithviraj, Darrell H. G. Crawford, Aparna Jayachandran
International Journal of Molecular Sciences.2022; 23(3): 1565. CrossRef - Evolving Role of Immunotherapy in Advanced Biliary Tract Cancers
Sandra Kang, Bassel F. El-Rayes, Mehmet Akce
Cancers.2022; 14(7): 1748. CrossRef - Novel immune scoring dynamic nomograms based on B7-H3, B7-H4, and HHLA2: Potential prediction in survival and immunotherapeutic efficacy for gallbladder cancer
Chao Lv, Shukun Han, Baokang Wu, Zhiyun Liang, Yang Li, Yizhou Zhang, Qi Lang, Chongli Zhong, Lei Fu, Yang Yu, Feng Xu, Yu Tian
Frontiers in Immunology.2022;[Epub] CrossRef - PD-1 inhibitors plus nab-paclitaxel-containing chemotherapy for advanced gallbladder cancer in a second-line setting: A retrospective analysis of a case series
Sirui Tan, Jing Yu, Qiyue Huang, Nan Zhou, Hongfeng Gou
Frontiers in Oncology.2022;[Epub] CrossRef - Expression of HER2 and Mismatch Repair Proteins in Surgically Resected Gallbladder Adenocarcinoma
You-Na Sung, Sung Joo Kim, Sun-Young Jun, Changhoon Yoo, Kyu-Pyo Kim, Jae Hoon Lee, Dae Wook Hwang, Shin Hwang, Sang Soo Lee, Seung-Mo Hong
Frontiers in Oncology.2021;[Epub] CrossRef - Programmed Death Ligand-1 (PD-L1) Is an Independent Negative Prognosticator in Western-World Gallbladder Cancer
Thomas Albrecht, Fritz Brinkmann, Michael Albrecht, Anke S. Lonsdorf, Arianeb Mehrabi, Katrin Hoffmann, Yakup Kulu, Alphonse Charbel, Monika N. Vogel, Christian Rupp, Bruno Köhler, Christoph Springfeld, Peter Schirmacher, Stephanie Roessler, Benjamin Goep
Cancers.2021; 13(7): 1682. CrossRef - Immune Microenvironment in Gallbladder Adenocarcinomas
Pallavi A. Patil, Kara Lombardo, Weibiao Cao
Applied Immunohistochemistry & Molecular Morphology.2021; 29(8): 557. CrossRef - Molecular Targets and Emerging Therapies for Advanced Gallbladder Cancer
Matteo Canale, Manlio Monti, Ilario Giovanni Rapposelli, Paola Ulivi, Francesco Giulio Sullo, Giulia Bartolini, Elisa Tiberi, Giovanni Luca Frassineti
Cancers.2021; 13(22): 5671. CrossRef - Overview of current targeted therapy in gallbladder cancer
Xiaoling Song, Yunping Hu, Yongsheng Li, Rong Shao, Fatao Liu, Yingbin Liu
Signal Transduction and Targeted Therapy.2020;[Epub] CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure


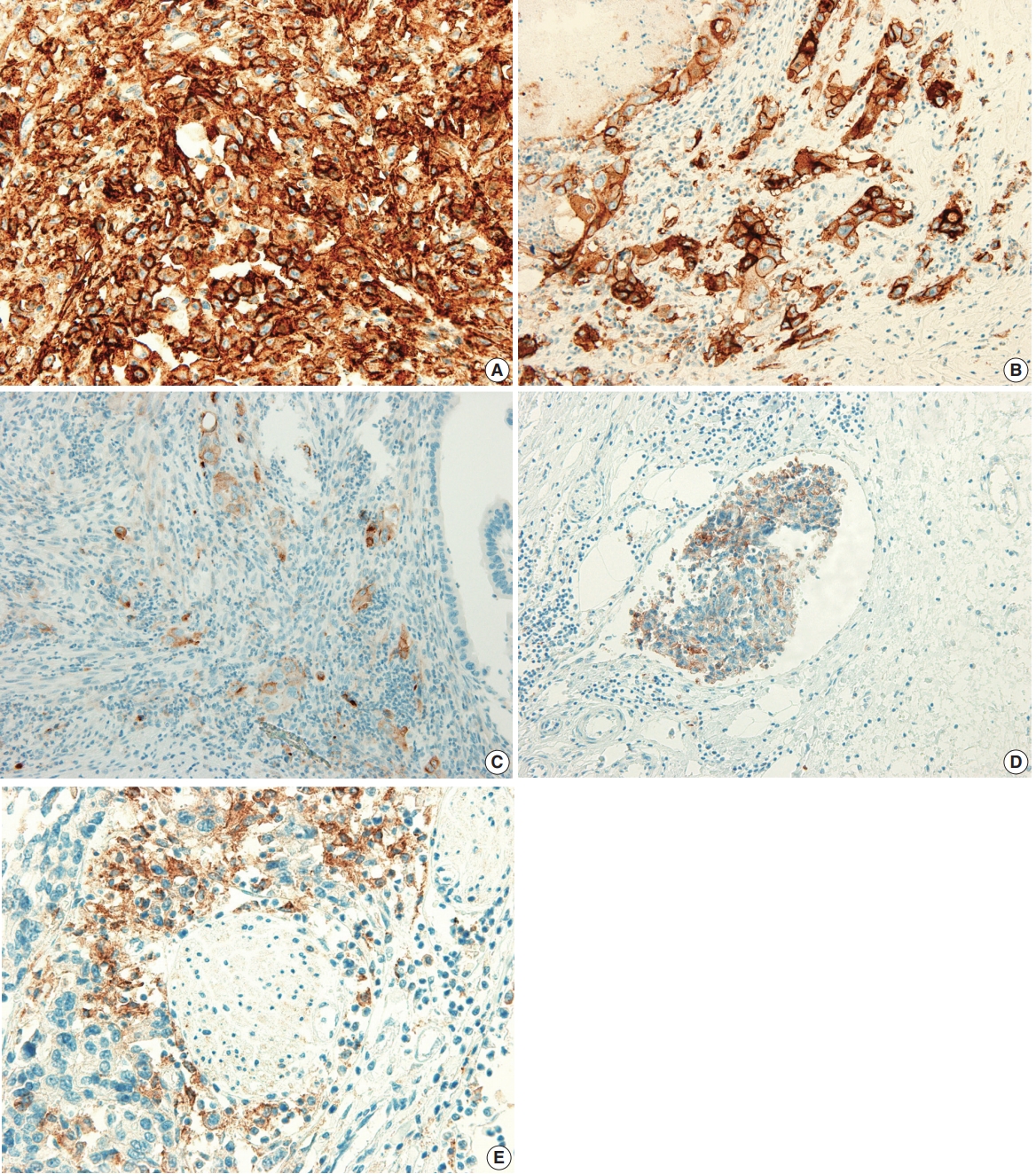
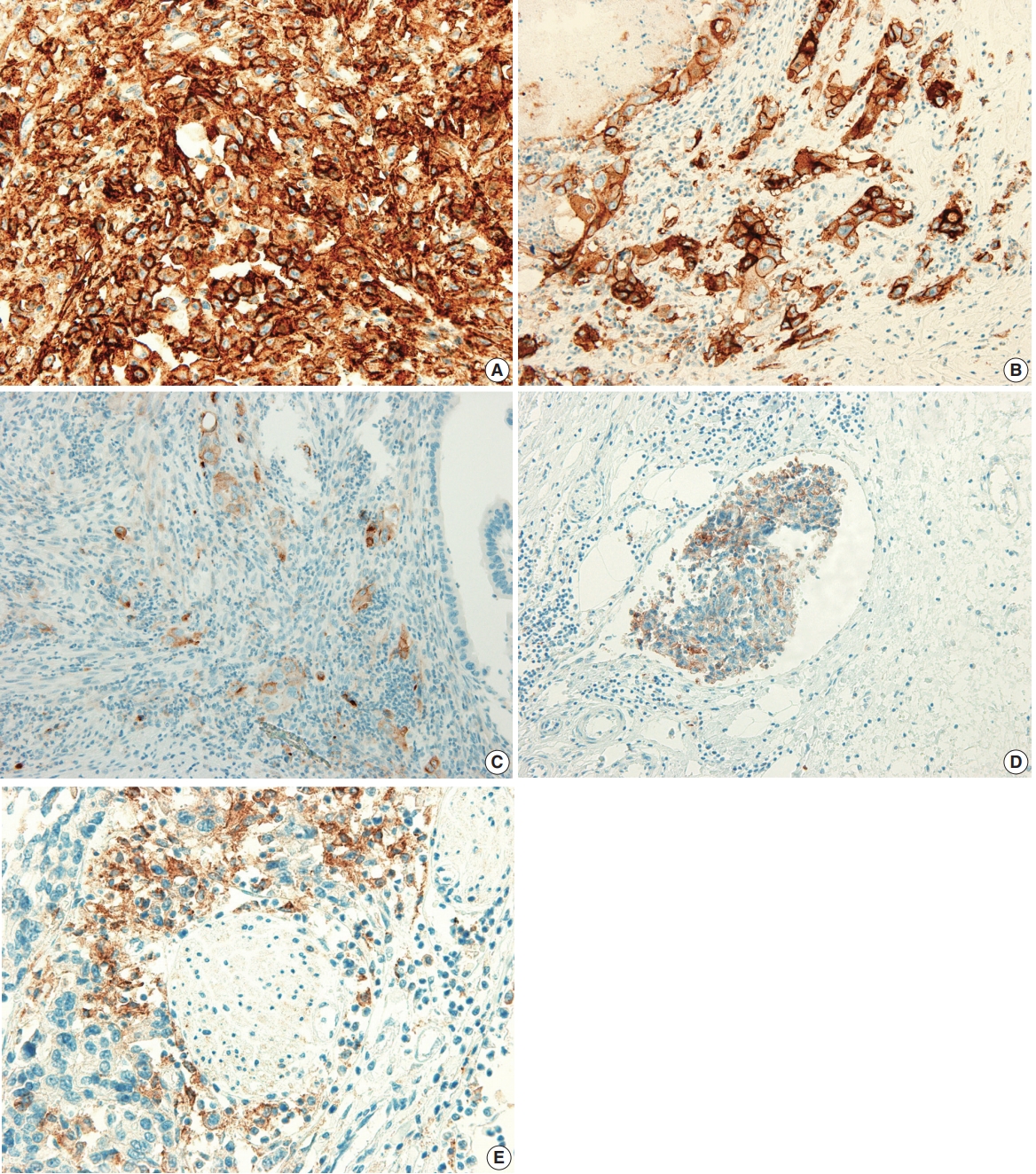
Fig. 1.
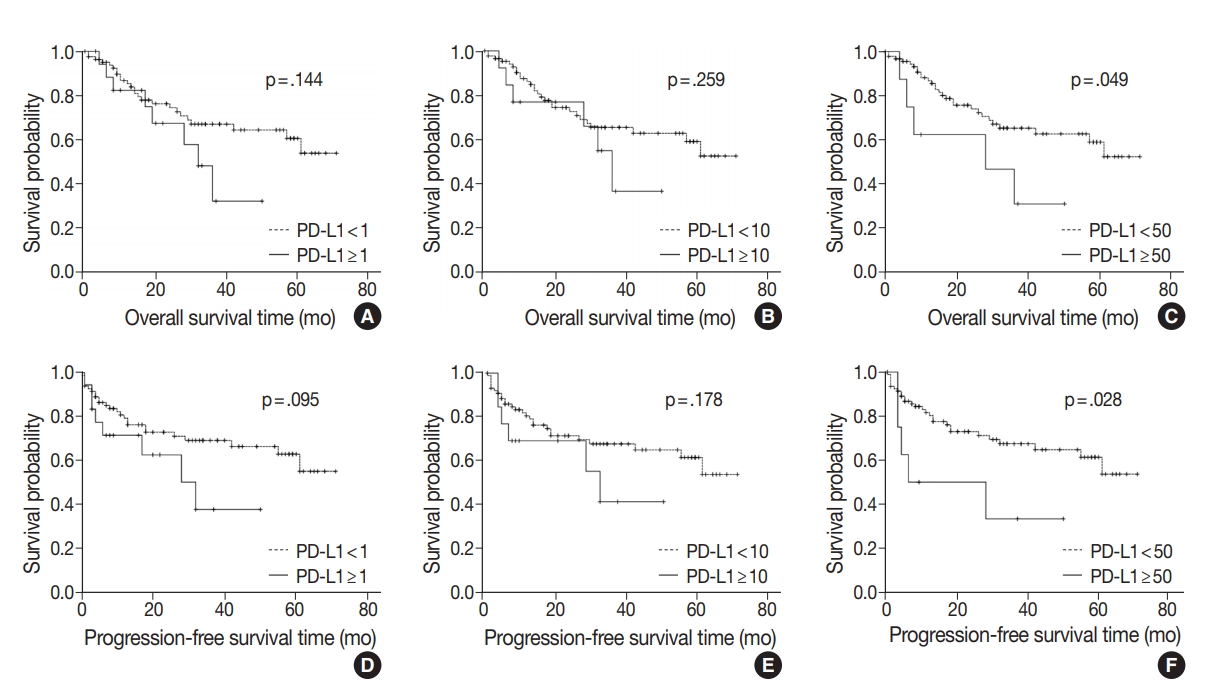
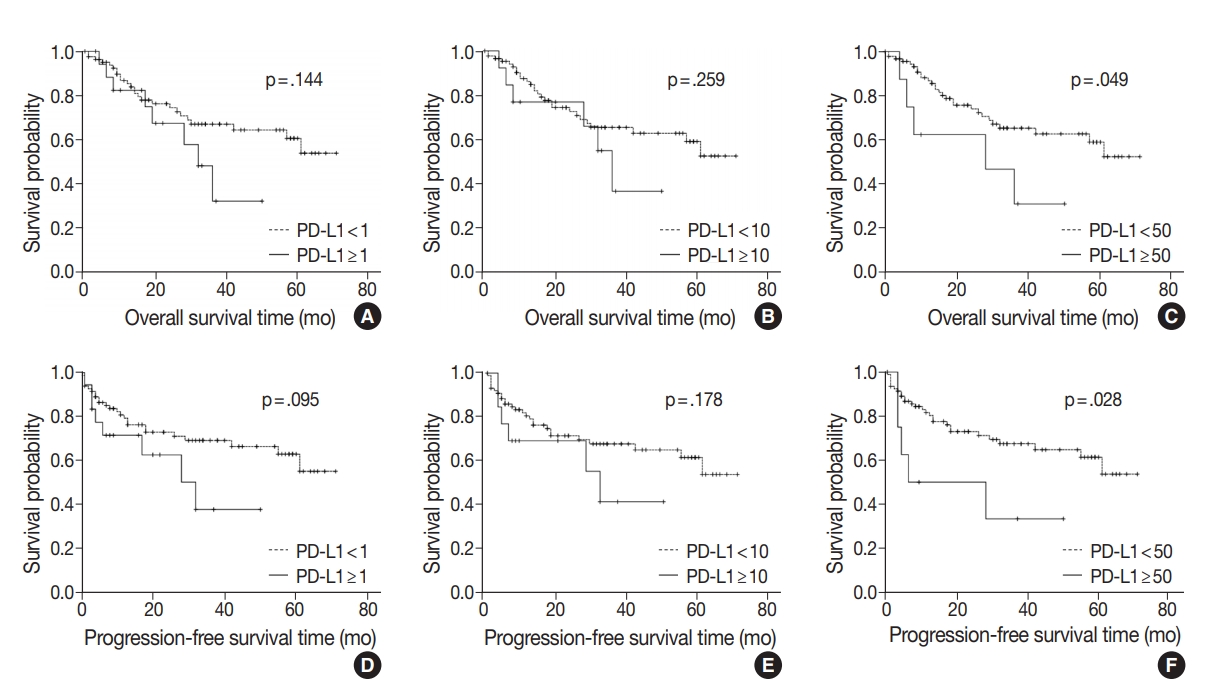
Fig. 2.
| Clinicopathological variable | No. (%) |
|---|---|
| Age, mean (range, yr) | 68.0 (40–90) |
| Sex | |
| Male | 44 (43.6) |
| Female | 57 (56.4) |
| Histological type | |
| Adenocarcinoma NOS | 82 (81.2) |
| MANEC | 3 (3.0) |
| ICPN with associated invasive carcinoma | 5 (5.0) |
| Adenocarcinoma with undifferentiated carcinoma | 3 (3.0) |
| Adenocarcinoma with squamous differentiation | 3 (3.0) |
| Adenocarcinoma with sarcomatoid differentiation and sarcomatoid carcinoma | 2 (2.0) |
| Adenocarcinoma with signet cell component and signet ring cell carcinoma | 2 (2.0) |
| Mucinous carcinoma | 1 (1.0) |
| Histologic grade | |
| Well differentiated | 45 (44.6) |
| Moderately differentiated | 34 (33.7) |
| Poorly differentiated | 18 (17.8) |
| Undifferentiated | 1 (1.0) |
| Others (SRC, MUC, SARC) | 3 (3.0) |
| T category | |
| pT1a | 15 (14.9) |
| PT1b | 14 (13.9) |
| pT2a | 47 (46.5) |
| pT2b | 8 (7.9) |
| pT3 | 15 (14.9) |
| pT4 | 2 (2.0) |
| N category | |
| Nx | 31 (30.7) |
| N0 | 37 (36.6) |
| N1 | 28 (27.7) |
| N2 | 5 (5.0) |
| M category | |
| M0 | 98 (97.0) |
| M1 | 3 (3.0) |
| Pathologic stage (total=72) | |
| I | 18 (25.0) |
| IIA | 16 (22.2) |
| IIB | 3 (4.2) |
| IIIA | 2 (2.8) |
| IIIB | 26 (36.1) |
| IVA | 1 (1.4) |
| IVB | 6 (8.3) |
| Operation | |
| Simple cholecystectomy | 43 (42.6) |
| Radical cholecystectomy | 55 (54.4) |
| Pylorus resecting pancreatoduodenectomy with hepatectomy | 2 (2.0) |
| Pylorus preserving pancreatoduodenectomy with hepatectomy | 1 (1.0) |
| Complete resection | |
| Yes | 92 (91.1) |
| No | 19 (9.9) |
| Adjuvant chemotherapy | |
| Not received | 71 (70.3) |
| Received | 30 (29.7) |
| Gallstone | |
| No | 72 (71.3) |
| Yes | 29 (28.7) |
| Cholecystitis | |
| No | 9 (9.0) |
| Yes | 92 (91.0) |
| Hypertension | |
| No | 72 (71.3) |
| Yes | 29 (28.7) |
| Diabetes | |
| No | 68 (67.3) |
| Yes | 33 (32.7) |
| Tumor location | |
| Fundus | 36 (35.6) |
| Body | 40 (39.6) |
| Neck, cystic duct | 14 (13.9) |
| More than 2 portions | 11 (10.9) |
| Size, median (range, cm) | 2.7 (0.1–6.9) |
| Growth pattern | |
| Polypoid | 53 (52.5) |
| Nonpolypoid, ulcerative | 48 (47.5) |
| Lymphovascular invasion | |
| Absent | 62 (61.4) |
| Present | 39 (38.6) |
| Perineural invasion | |
| Absent | 65 (64.4) |
| Present | 36 (35.6) |
| PD-L1 expression (%) | |
| < 1 | 82 (81.2) |
| 1–9 | 5 (5.0) |
| 10–49 | 6 (5.9) |
| ≥ 50 | 8 (7.9) |
| Clinicopathological parameter | PD-L1 |
p-value | PD-L1 |
p-value | PD-L1 |
p-value | |||
|---|---|---|---|---|---|---|---|---|---|
| < 1% | ≥ 1% | < 10% | ≥ 10% | < 50% | ≥ 50% | ||||
| Sex | .887 | .270 | > .99 |
||||||
| Male | 36 (43.9) | 8 (42.1) | 36 (41.4) | 8 (57.1) | 41 (44.1) | 3 (37.5) | |||
| Female | 46 (56.1) | 11 (57.9) | 51 (58.6) | 6 (42.9) | 52 (55.9) | 5 (62.5) | |||
| Age (yr) | .259 | .302 | .716 |
||||||
| < 68 | 42 (51.2) | 7 (36.8) | 44 (50.6) | 5 (35.7) | 46 (49.5) | 3 (37.5) | |||
| ≥ 68 | 40 (48.8) | 12 (63.2) | 43 (49.4) | 9 (64.3) | 47 (50.5) | 5 (62.5) | |||
| Histologic type | .132 |
.004 |
.306 |
||||||
| Adenocarcinoma NOS, ICPN with associated invasive carcinoma | 73 (89.0) | 14 (73.7) | 79 (90.8) | 8 (57.1) | 81 (87.1) | 6 (75.0) | |||
| Adenocarcinoma with other component, others | 9 (11.0) | 5 (26.3) | 8 (9.2) | 6 (42.9) | 12 (12.9) | 2 (25.0) | |||
| Histologic grade | .001 | < .001 |
< .001 |
||||||
| Well differentiated | 42 (51.2) | 3 (15.8) | 44 (50.6) | 1 (7.1) | 45 (48.4) | 0 | |||
| Moderately differentiated | 28 (34.1) | 6 (31.6) | 31 (35.6) | 3 (21.4) | 33 (35.5) | 1 (12.5) | |||
| Poorly differentiated, undifferentiated, others | 12 (14.6) | 10 (52.6) | 12 (13.8) | 10 (71.4) | 15 (16.1) | 7 (87.5) | |||
| T category | |||||||||
| pT1 + pT2 | 70 (85.4) | 14 (73.7) | .304 |
76 (87.4) | 8 (57.1) | .012 |
80 (86.0) | 4 (50.0) | .026 |
| pT3 + pT4 | 12 (14.6) | 5 (26.3) | 11 (12.6) | 6 (42.9) | 13 (14.0) | 4 (50.0) | |||
| N category | .260 | .137 | .093 |
||||||
| N0 | 31 (56.4) | 6 (40.0) | 33 (56.9) | 4 (33.3) | 36 (56.3) | 1 (16.7) | |||
| N1 + N2 | 24 (43.6) | 9 (60.0) | 25 (43.1) | 8 (66.7) | 28 (43.8) | 5 (83.3) | |||
| Pathologic stage | .116 | .045 | .010 |
||||||
| I + II | 32 (56.1) | 5 (33.3) | 34 (56.7) | 3 (25.0) | 37 (56.1) | 0 | |||
| III + IV | 25 (43.9) | 10 (66.7) | 26 (43.3) | 9 (75.0) | 29 (43.9) | 6 (100) | |||
| Growth pattern | .315 | .437 | > .99 |
||||||
| Polypoid | 45 (54.9) | 8 (42.1) | 47 (54.0) | 6 (42.9) | 49 (52.7) | 4 (50.0) | |||
| Nonpolypoid (ulcerative) | 37 (45.1) | 11 (57.9) | 40 (46.0) | 8 (57.1) | 44 (47.3) | 4 (50.0) | |||
| Lymphovascular invasion | .015 | .001 | .005 |
||||||
| No | 55 (67.1) | 7 (36.8) | 59 (67.8) | 3 (21.4) | 61 (65.6) | 1 (12.5) | |||
| Yes | 27 (32.9) | 12 (63.2) | 28 (32.2) | 11 (78.6) | 32 (34.4) | 7 (87.5) | |||
| Perineural invasion | .086 | .032 |
.023 |
||||||
| No | 56 (68.3) | 9 (47.4) | 60 (69.0) | 5 (35.7) | 63 (67.7) | 2 (25.0) | |||
| Yes | 26 (31.7) | 10 (52.6) | 27 (31.0) | 9 (64.3) | 30 (32.3) | 6 (75.0) | |||
| Tumor location | .487 |
.079 |
.060 |
||||||
| Fundus | 30 (36.6) | 6 (31.6) | 31 (35.6) | 5 (35.7) | 35 (37.6) | 1 (12.5) | |||
| Body | 33 (40.2) | 7 (36.8) | 35 (40.2) | 5 (35.7) | 36 (38.7) | 4 (50.0) | |||
| Neck, cystic duct | 12 (14.6) | 2 (10.5) | 14 (16.1) | 0 | 14 (15.1) | 0 | |||
| More than 2 portions | 7 (8.5) | 4 (21.1) | 7 (8.0) | 4 (28.6) | 8 (8.6) | 3 (37.5) | |||
| Tumor size (cm) | .040 | .007 | .062 |
||||||
| < 2.7 | 43 (52.4) | 5 (26.3) | 46 (52.9) | 2 (14.3) | 47 (50.5) | 1 (12.5) | |||
| ≥ 2.7 | 39 (47.6) | 14 (73.7) | 41 (47.1) | 12 (85.7) | 46 (49.5) | 7 (87.5) | |||
| Complete resection | .676 |
> .99 |
.539 |
||||||
| Yes | 75 (91.5) | 17 (89.5) | 79 (90.8) | 13 (92.9) | 85 (91.4) | 7 (87.5) | |||
| No | 7 (8.5) | 2 (10.5) | 8 (9.2) | 1 (7.1) | 8 (8.6) | 1 (12.5) | |||
| Adjuvant chemotherapy | .720 | .344 |
.233 |
||||||
| No or refuse | 57 (69.5) | 14 (73.7) | 63 (72.4) | 8 (57.1) | 67 (72.0) | 4 (50.0) | |||
| Yes | 25 (30.5) | 5 (26.3) | 24 (27.6) | 6 (42.9) | 26 (28.6) | 4 (50.0) | |||
| Gallstone | .798 | .339 |
.433 |
||||||
| No | 58 (70.7) | 14 (73.7) | 60 (69.0) | 12 (85.7) | 65 (69.9) | 7 (87.5) | |||
| Yes | 24 (29.3) | 5 (26.3) | 27 (31.0) | 2 (14.3) | 28 (30.1) | 1 (12.5) | |||
| Cholecystitis | .228 | .727 | > .99 | ||||||
| No | 21 (91.3) | 2 (8.7) | 21 (91.3) | 2 (8.7) | 21 (91.3) | 2 (8.7) | |||
| Yes | 61 (78.2) | 17 (21.8) | 67 (85.9) | 11 (14.1) | 72 (92.3) | 6 (7.7) | |||
| Diabetes | .512 | .137 |
.268 |
||||||
| No | 54 (65.9) | 14 (73.7) | 56 (64.4) | 12 (85.7) | 61 (65.6) | 7 (87.5) | |||
| Yes | 28 (34.1) | 5 (26.3) | 31 (35.6) | 2 (14.3) | 32 (34.4) | 1 (12.5) | |||
| Hypertension | .729 | .346 | .255 |
||||||
| No | 51 (62.2) | 11 (57.9) | 55 (63.2) | 7 (50.0) | 59 (63.4) | 3 (37.5) | |||
| Yes | 31 (37.8) | 8 (42.1) | 32 (36.8) | 7 (50.0) | 34 (36.6) | 5 (62.5) | |||
| Clinicopathological parameter | OS (mo) | p-value | PFS (mo) | p-value |
|---|---|---|---|---|
| Sex | .632 | .694 | ||
| Male | 50.61 ± 4.57 | 49.90 ± 4.82 | ||
| Female | 45.90 ± 3.78 | 45.21 ± 3.97 | ||
| Age (yr) | .044 | .070 | ||
| <68 | 52.37 ± 3.65 | 51.07 ± 3.99 | ||
| ≥68 | 42.52 ± 4.61 | 41.30 ± 4.85 | ||
| Histologic type | .385 | .349 | ||
| Adenocarcinoma NOS, ICPN with associated invasive carcinoma | 49.57 ± 3.27 | 49.04 ± 3.42 | ||
| Adenocarcinoma with other component, others | 38.81 ± 6.30 | 36.73 ± 6.74 | ||
| Histologic grade | .003 | .002 | ||
| Well differentiated | 59.50 ± 3.62 | 59.02 ± 3.79 | ||
| Moderately differentiated | 40.43 ± 4.59 | 39.81 ± 4.87 | ||
| Poorly differentiated, undifferentiated, others | 33.07 ± 5.16 | 30.12 ± 5.63 | ||
| T category | < .001 | < .001 | ||
| pT1 + pT2 | 53.37 ± 3.17 | 52.98 ± 3.28 | ||
| pT3 + pT4 | 25.05 ± 5.41 | 19.64 ± 6.02 | ||
| N category | < .001 | < .001 | ||
| N0 | 62.85 ± 3.28 | 62.31 ± 3.46 | ||
| N1 + N2 | 34.51 ± 5.05 | 32.62 ± 5.75 | ||
| Pathologic stage | < .001 | < .001 | ||
| I + II | 62.53 ± 3.25 | 62.43 ± 3.31 | ||
| III + IV | 34.86 ± 4.92 | 33.03 ± 5.54 | ||
| Lymphovascular invasion | < .001 | < .001 | ||
| No | 58.03 ± 3.26 | 57.79 ± 3.33 | ||
| Yes | 31.38 ± 4.34 | 28.17 ± 4.89 | ||
| Perineural invasion | < .001 | < .001 | ||
| No | 55.46 ± 3.00 | 55.17 ± 3.10 | ||
| Yes | 31.91 ± 5.06 | 29.65 ± 5.59 | ||
| Tumor location | .050 | .094 | ||
| Fundus | 42.46 ± 4.07 | 42.17 ± 4.44 | ||
| Body | 48.36 ± 4.42 | 47.67 ± 4.61 | ||
| Neck, cystic duct | 57.13 ± 6.88 | 55.27 ± 7.91 | ||
| More than 2 portions | 24.73 ± 6.50 | 24.64 ± 6.82 | ||
| Tumor size (cm) | .058 | .042 | ||
| < 2.7 | 54.65 ± 4.14 | 54.16 ± 4.29 | ||
| ≥ 2.7 | 41.27 ± 3.85 | 39.84 ± 4.15 | ||
| Growth pattern | .019 | .015 | ||
| Polypoid | 55.12 ± 3.77 | 54.68 ± 3.90 | ||
| Nonpolypoid, ulcerative | 37.52 ± 3.89 | 35.82 ± 4.35 | ||
| Complete resection | .006 | .005 | ||
| Yes | 25.63 ± 8.72 | 22.98 ± 9.38 | ||
| No | 50.67 ± 3.12 | 49.98 ± 3.28 | ||
| Adjuvant chemotherapy | .488 | .322 | ||
| No | 48.58 ± 3.43 | 48.08 ± 3.54 | ||
| Yes | 45.27 ± 5.46 | 43.02 ± 6.11 | ||
| Gallstone | .066 | .095 | ||
| No | 50.26 ± 3.28 | 49.54 ± 3.47 | ||
| Yes | 38.78 ± 5.63 | 38.31 ± 5.87 | ||
| Cholecystitis | .668 | .694 | ||
| No | 47.70 ± 4.54 | 47.02 ± 4.85 | ||
| Yes | 47.78 ± 3.64 | 47.45 ± 3.78 | ||
| Diabetes | .270 | .222 | ||
| No | 50.89 ± 3.72 | 50.38 ± 3.90 | ||
| Yes | 42.10 ± 4.57 | 40.50 ± 4.86 | ||
| Hypertension | .615 | .619 | ||
| No | 45.93 ± 3.55 | 44.93 ± 3.78 | ||
| Yes | 51.21 ± 4.96 | 51.02 ± 5.07 | ||
| PD-L1 expression | ||||
| PD-L1 < 1% | 50.53 ± 3.29 | .144 | 49.95 ± 3.43 | .095 |
| PD-L1 ≥ 1% | 31.35 ± 4.42 | 28.75 ± 5.17 | ||
| PD-L1 < 10% | 49.80 ± 3.24 | .259 | 49.27 ± 3.38 | .178 |
| PD-L1 ≥ 10% | 32.89 ± 5.03 | 30.31 ± 5.75 | ||
| PD-L1 < 50% | 50.13 ± 3.14 | .049 | 49.48 ± 3.29 | .028 |
| PD-L1 ≥ 50% | 27.88 ± 6.69 | 23.33 ±7.47 |
| Disease | No. | Detection specimen; detection antibody | PD-L1 expression cutoff (%) | Other clinicopathological parameters associated with PD-L1 expression | Survival with PD-L1 expression | Study |
|---|---|---|---|---|---|---|
| Gallbladder cancer | 174 | FFPE tissue; anti–PD-L1 (clone SP263) | 1, 10, 50 | Significant positive association with histologic type (squamous cell carcinoma, adenosquamous cell carcinoma, undifferentiated carcinoma), histologic grade (progressed from WD to PD), nuclear grade, stage 3 and 4, TIL (0 to 3+) | OS was not associated with PD-L1 expression | Neyaz et al. [11] |
| Gallbladder adenocarcinoma | 66 | FFPE tissue; anti–PD-L1 (E1L3N) | 5 | PD-L1 positive alone was not correlated with any clinicopathological or pathological parameters except for CD8+ TIL density and worse median OS | Combination of CD8 high with negative expression of PD-L1 serves as prognostic factor for improved OS and PFS | Lin et al. [12] |
| Gastric adenocarcinoma | 240 | FFPE tissue; anti–PD-L1 (E1L3N) | 10 | Patients with poor tumor differentiation had a higher positive rate of PD-L1 expression on tumor cells | Positive PD-L1 expression on TILs had a shorter OS; However, PD-L1 expression on tumor cells was not associated with OS | Fang et al. [23] |
| Gastric cancer | 107 | FFPE tissue; anti–PDL1 (polyclonal antihuman PD-L1/CD274 antibody) | Not applicable | Positive rate of PD-L1 expression is much higher in depth of invasion, high differentiation, lymph node metastasis, and higher T category | PD-L1–positive gastric cancers were significantly associated with a poor prognosis | Qing et al. [24] |
| Esophageal cancer | 41 | Frozen tissue; anti–PD-L1 (MIH1, mouse IgG1) | 10 | Effect of PD-L1 status was more distinct in the advanced stage of tumor with lymph node metastasis and distinct metastasis | Overall survival of patients with tumors positive for both PD-L1 and PD-L2 was significantly worse than that with tumors negative for both | Ohigashi et al. [25] |
| Colorectal cancer | 143 | FFPE tissue; anti–PD-L1 (Abcam, ab58810) | Strong and moderate immunostaining intensity | PD-L1 was significantly associated with cell differentiation status and TNM stage | Positive PD-L1 expression showed a trend shorter survival time; as an independent predictor of prognosis | Shi et al. [26] |
| Lung adenocarcinoma | 163 | FFPE tissue; anti–PD-L1 (Proteintech Group Inc., Chicago, IL, USA) | 5 | PD-L1 had higher positive results in tumors with higher grade differentiation and vascular invasion | PD-L1 expression correlated with better RFS | Yang et al. [27] |
| Lung non-small cell carcinoma | 819 | FFPE tissue; anti–PD-L1 (22C3) | 50 | Lower PD-L1 positivity correlated with lower stage and squamous cell carcinoma than adenocarcinoma | Not assessed | Skov et al. [28] |
| Extrahepatic cholangiocarcinoma | 69 | FFPE tissue; anti–PD-L1 (E1L3N) | Not applicable | Significant correlations of PD-L1 expression with venous invasion and poor differentiation of the tumor were observed | PD-L1 expression was not correlated with patient OS, but combined high PDL1 expression on tumor cells and low infiltration of CD3+ TILs showed poor OS | Walter D et al. [29] |
| Hepatocellular carcinoma | 240 + additional 125 | FFPE tissue; anti–PD-L1 (eBioscience) | High vs. low | PD-L1 expression was an independent prognostic factor for tumor vascular invasion, encapsulation, and TNM stage | PD-L1–positive (high expression) patients had significantly poorer DFS and OS | Gao et al. [30] |
| Hepatocellular carcinoma | 448 | FFPE tissue; anti–PD-L1 (E1L3N) | 1, 5 | No significant difference in PD-L1 expression was detected | Survival analysis showed that 5% PD-L1 expression was significantly correlated with improved rates of OS and RFS | Chen et al. [31] |
| Uveal melanoma | 67 | FFPE tissue; anti–PD-L1 (E1L3N) | 5 | Significant association of PD-L1 expression to a decreased number of TIL | PD-L1 expression is associated with metastasis-free survival | Zoroquiain et al. [32] |
Values are presented as number (%). NOS, not otherwise specified; MANEC, mixed adenoneuroendocrine carcinoma; ICPN, intracholecystic papillary neoplasm; SRC, signet ring cell carcinoma; MUC, mucinous carcinoma; SARC, sarcomatoid carcinoma; PDL1, programmed death-ligand 1.
Values are presented as number (%). Statistical analysis method: Pearson chi-square test. PD-L1, programmed death-ligand 1; GBC, gallbladder cancer; NOS, not otherwise specified; ICPN, intracholecystic papillary neoplasm; Others, mixed adenoneuroendocrine carcinoma, signet ring cell carcinoma, mucinous carcinoma, sarcomatoid carcinoma. Fisher exact test.
Values are presented as mean ± standard error. Statistical analysis method: survival analysis by Kaplan-Meier method and log-rank test. OS, overall survival; PFS, progression-free survival; GBC, gallbladder cancer; NOS, not otherwise specified; ICPN, intracholecystic papillary neoplasm; others, mixed adenoneuroendocrine carcinoma, signet ring cell carcinoma, mucinous carcinoma,sarcomatoid carcinoma; PD-L1, programmed death-ligand 1.
PD-L1, programmed death-ligand 1; FFPE, formalin-fixed, paraffin-embedded; WD, well-differentiated; PD, poorly differentiated; TIL, tumor-infiltrating lymphocyte; OS, overall survival; PFS, progression-free survival.

 E-submission
E-submission