Search
- Page Path
- HOME > Search
- A standardized pathology report for gastric cancer: 2nd edition
- Young Soo Park, Myeong-Cherl Kook, Baek-hui Kim, Hye Seung Lee, Dong-Wook Kang, Mi-Jin Gu, Ok Ran Shin, Younghee Choi, Wonae Lee, Hyunki Kim, In Hye Song, Kyoung-Mee Kim, Hee Sung Kim, Guhyun Kang, Do Youn Park, So-Young Jin, Joon Mee Kim, Yoon Jung Choi, Hee Kyung Chang, Soomin Ahn, Mee Soo Chang, Song-Hee Han, Yoonjin Kwak, An Na Seo, Sung Hak Lee, Mee-Yon Cho
- J Pathol Transl Med. 2023;57(1):1-27. Published online January 15, 2023
- DOI: https://doi.org/10.4132/jptm.2022.12.23
- 40,810 View
- 1,595 Download
- 25 Web of Science
- 23 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - The first edition of ‘A Standardized Pathology Report for Gastric Cancer’ was initiated by the Gastrointestinal Pathology Study Group of the Korean Society of Pathologists and published 17 years ago. Since then, significant advances have been made in the pathologic diagnosis, molecular genetics, and management of gastric cancer (GC). To reflect those changes, a committee for publishing a second edition of the report was formed within the Gastrointestinal Pathology Study Group of the Korean Society of Pathologists. This second edition consists of two parts: standard data elements and conditional data elements. The standard data elements contain the basic pathologic findings and items necessary to predict the prognosis of GC patients, and they are adequate for routine surgical pathology service. Other diagnostic and prognostic factors relevant to adjuvant therapy, including molecular biomarkers, are classified as conditional data elements to allow each pathologist to selectively choose items appropriate to the environment in their institution. We trust that the standardized pathology report will be helpful for GC diagnosis and facilitate large-scale multidisciplinary collaborative studies.
-
Citations
Citations to this article as recorded by- GAST-NET: A multi-modal and multi-task deep learning framework for preoperative prediction of perineural invasion and prognostic risk in gastric cancer
Shidi Miao, Hexiang Dong, Jinyang Feng, Yuyang Jiang, Mengzhuo Sun, Zengyao Liu, Qiujun Wang, Xuemei Ding, Ruitao Wang
International Journal of Medical Informatics.2026; 212: 106348. CrossRef - Poorly cohesive carcinoma diffusely involving the whole gastrointestinal tract: a case report
Wei Gao, Yusheng Yang, Xinyi Hu, Yujuan Shi, Kai Liu, Minmin Gu, Jing Wang
Discover Oncology.2026;[Epub] CrossRef - Comprehensive Overview of Gastric Cancer Immunohistochemistry: Key Biomarkers, Advanced Detection Methods, and Perspectives
Bogdan Oprea
Medicina.2026; 62(4): 683. CrossRef - Tumor Budding in Gastric Carcinoma: Beyond Counting Cells at the Invasive Front—A Review of Current Evidence and Biological Perspectives
Catalin-Bogdan Satala, Gabriela Gurau, Alina-Mihaela Gurau, Gabriela Patrichi, Daniela Mihalache
International Journal of Molecular Sciences.2026; 27(9): 3787. CrossRef - Spatial and Temporal Tumor Heterogeneity in Gastric Cancer: Discordance of Predictive Biomarkers
Hye Seung Lee
Journal of Gastric Cancer.2025; 25(1): 192. CrossRef - PD-L1 as a Biomarker in Gastric Cancer Immunotherapy
Yunjoo Cho, Soomin Ahn, Kyoung-Mee Kim
Journal of Gastric Cancer.2025; 25(1): 177. CrossRef - Korean Gastric Cancer Association-Led Nationwide Survey on Surgically Treated Gastric Cancers in 2023
Dong Jin Kim, Jeong Ho Song, Ji-Hyeon Park, Sojung Kim, Sin Hye Park, Cheol Min Shin, Yoonjin Kwak, Kyunghye Bang, Chung-sik Gong, Sung Eun Oh, Yoo Min Kim, Young Suk Park, Jeesun Kim, Ji Eun Jung, Mi Ran Jung, Bang Wool Eom, Ki Bum Park, Jae Hun Chung, S
Journal of Gastric Cancer.2025; 25(1): 115. CrossRef - A Comprehensive and Comparative Review of Global Gastric Cancer Treatment Guidelines: 2024 Update
Sang Soo Eom, Keun Won Ryu, Hye Sook Han, Seong-Ho Kong
Journal of Gastric Cancer.2025; 25(1): 153. CrossRef - Korea, Japan, Europe, and the United States: Why are guidelines for gastric cancer different?
Emily E. Stroobant, Seong-Ho Kong, Maria Bencivenga, Takahiro Kinoshita, Tae-Han Kim, Takeshi Sano, Giovanni de Manzoni, Han-Kwang Yang, Yuko Kitagawa, Vivian E. Strong
Gastric Cancer.2025; 28(4): 559. CrossRef - Can the Japanese guidelines for endoscopic submucosal dissection be safely applied to Korean gastric cancer patients? A multicenter retrospective study based on the Korean Gastric Cancer Association nationwide survey
Hayemin Lee, Mi Ryeong Park, Junhyun Lee
Annals of Surgical Treatment and Research.2025; 109(2): 81. CrossRef - Double optimal transport for differential gene regulatory network inference with unpaired samples
Mengyu Li, Bencong Zhu, Cheng Meng, Xiaodan Fan, Laura Cantini
Bioinformatics.2025;[Epub] CrossRef - A Randomized Controlled Trial to Evaluate the Effect of Fibrin Glue on Bleeding after Gastric Endoscopic Submucosal Dissection
Tae-Se Kim, Tae-Jun Kim, Yang Won Min, Hyuk Lee, Byung-Hoon Min, Jun Haeng Lee, Poong-Lyul Rhee, Jae J. Kim
Gut and Liver.2025; 19(5): 677. CrossRef - Diagnostic accuracy of stereomicroscopy assessment of invasion depth in ex vivo specimens of early gastric cancer
Jing Wang, Lin Chang, Dong-Feng Niu, Yan Yan, Chang-Qi Cao, Shi-Jie Li, Qi Wu
World Journal of Gastroenterology.2025;[Epub] CrossRef - SMMILe enables accurate spatial quantification in digital pathology using multiple-instance learning
Zeyu Gao, Anyu Mao, Yuxing Dong, Hannah Clayton, Jialun Wu, Jiashuai Liu, ChunBao Wang, Kai He, Tieliang Gong, Chen Li, Mireia Crispin-Ortuzar
Nature Cancer.2025; 6(12): 2025. CrossRef - Genomic and Transcriptomic Characterization of Gastric Cancer with Bone Metastasis
Sujin Oh, Soo Kyung Nam, Keun-Wook Lee, Hye Seung Lee, Yujun Park, Yoonjin Kwak, Kyu Sang Lee, Ji-Won Kim, Jin Won Kim, Minsu Kang, Young Suk Park, Sang-Hoon Ahn, Yun-Suhk Suh, Do Joong Park, Hyung Ho Kim
Cancer Research and Treatment.2024; 56(1): 219. CrossRef - Microscopic tumor mapping of post-neoadjuvant therapy pancreatic cancer specimens to predict post-surgical recurrence: A prospective cohort study
Yeshong Park, Yeon Bi Han, Jinju Kim, MeeYoung Kang, Boram Lee, Eun Sung Ahn, Saemi Han, Haeryoung Kim, Hee-Young Na, Ho-Seong Han, Yoo-Seok Yoon
Pancreatology.2024; 24(4): 562. CrossRef - Effect of Neoadjuvant Chemotherapy on Tumor-Infiltrating Lymphocytes in Resectable Gastric Cancer: Analysis from a Western Academic Center
Elliott J. Yee, Danielle Gilbert, Jeffrey Kaplan, Sachin Wani, Sunnie S. Kim, Martin D. McCarter, Camille L. Stewart
Cancers.2024; 16(7): 1428. CrossRef - Interpretation of PD-L1 expression in gastric cancer: summary of a consensus meeting of Korean gastrointestinal pathologists
Soomin Ahn, Yoonjin Kwak, Gui Young Kwon, Kyoung-Mee Kim, Moonsik Kim, Hyunki Kim, Young Soo Park, Hyeon Jeong Oh, Kyoungyul Lee, Sung Hak Lee, Hye Seung Lee
Journal of Pathology and Translational Medicine.2024; 58(3): 103. CrossRef - Expression of claudin 18.2 in poorly cohesive carcinoma and its association with clinicopathologic parameters in East Asian patients
Moonsik Kim, Byung Woog Kang, Jihyun Park, Jin Ho Baek, Jong Gwang Kim
Pathology - Research and Practice.2024; 263: 155628. CrossRef - Clinicopathological analysis of claudin 18.2 focusing on intratumoral heterogeneity and survival in patients with metastatic or unresectable gastric cancer
T.-Y. Kim, Y. Kwak, S.K. Nam, D. Han, D.-Y. Oh, S.-A. Im, H.S. Lee
ESMO Open.2024; 9(12): 104000. CrossRef - Pathological Interpretation of Gastric Tumors in Endoscopic Submucosal Dissection
Jung Yeon Kim
Journal of Digestive Cancer Research.2023; 11(1): 15. CrossRef - Histopathology of Gastric Cancer
Baek-hui Kim, Sung Hak Lee
The Korean Journal of Helicobacter and Upper Gastrointestinal Research.2023; 23(2): 143. CrossRef - Endoscopic submucosal dissection hands-on training with artificial mucosal layer EndoGEL
Tae-Se Kim, Jun Haeng Lee
Journal of Innovative Medical Technology.2023; 1(1): 5. CrossRef
- GAST-NET: A multi-modal and multi-task deep learning framework for preoperative prediction of perineural invasion and prognostic risk in gastric cancer
- Standardization of the pathologic diagnosis of appendiceal mucinous neoplasms
- Dong-Wook Kang, Baek-hui Kim, Joon Mee Kim, Jihun Kim, Hee Jin Chang, Mee Soo Chang, Jin-Hee Sohn, Mee-Yon Cho, So-Young Jin, Hee Kyung Chang, Hye Seung Han, Jung Yeon Kim, Hee Sung Kim, Do Youn Park, Ha Young Park, So Jeong Lee, Wonae Lee, Hye Seung Lee, Yoo Na Kang, Younghee Choi
- J Pathol Transl Med. 2021;55(4):247-264. Published online July 8, 2021
- DOI: https://doi.org/10.4132/jptm.2021.05.28
- 23,185 View
- 1,153 Download
- 19 Web of Science
- 18 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Although the understanding of appendiceal mucinous neoplasms (AMNs) and their relationship with disseminated peritoneal mucinous disease have advanced, the diagnosis, classification, and treatment of AMNs are still confusing for pathologists and clinicians. The Gastrointestinal Pathology Study Group of the Korean Society of Pathologists (GPSG-KSP) proposed a multicenter study and held a workshop for the “Standardization of the Pathologic Diagnosis of the Appendiceal Mucinous Neoplasm” to overcome the controversy and potential conflicts. The present article is focused on the diagnostic criteria, terminologies, tumor grading, pathologic staging, biologic behavior, treatment, and prognosis of AMNs and disseminated peritoneal mucinous disease. In addition, GPSG-KSP proposes a checklist of standard data elements of appendiceal epithelial neoplasms to standardize pathologic diagnosis. We hope the present article will provide pathologists with updated knowledge on how to handle and diagnose AMNs and disseminated peritoneal mucinous disease.
-
Citations
Citations to this article as recorded by- The clinical and pathological features of low-grade appendiceal mucinous neoplasm (LAMN)
Omar Hamdy, Gehad A. Saleh, Mona Hany Emile, Ahmed Elhadidy, Ahmed Ibrahim, Ola Elsayed, Ahmed Reda, Yasser Sharaf, Merna M. Hegazi, Osama Bahy, Mahmoud Soliman
Discover Oncology.2026;[Epub] CrossRef - Intrasplenic metastasis of appendiceal low-grade mucinous neoplasm – A case report and review of the literature
P. Meister, J. Rawitzer, M. Reschke, H.A. Baba, U. Neumann, M. Kaths
Current Problems in Cancer: Case Reports.2025; 18: 100364. CrossRef - Complete laparoscopic resection of giant appendiceal mucinous neoplasm, case report, and literature review
Shatha Awad Althobaiti, Rayan Z. Makeen, Abrar J. Filfilan, Ahmed Abdulaziz Hawsawi
Saudi Surgical Journal.2025; 13(1): 35. CrossRef - Survival Outcomes and Prognostic Factors in Metastatic Unresectable Appendiceal Adenocarcinoma Treated with Palliative Systemic Chemotherapy: A 10-Year Retrospective Analysis from Australia
Jirapat Wonglhow, Hui-Li Wong, Michael Michael, Alexander Heriot, Glen Guerra, Catherine Mitchell, Jeanne Tie
Cancers.2025; 17(20): 3297. CrossRef - Lower Gastrointestinal Bleeding Secondary to Appendiceal Mucinous Neoplasm: A Report of Two Cases and a Review of the Literature
Jesús Omar Soto Llanes, Samanta Kin Dosal Limón, Ana Jimena Iberri Jaime, Mario Zambrano Lara, Billy Jiménez Bobadilla
Cureus.2024;[Epub] CrossRef - Predicting Survival in Mucinous Adenocarcinoma of the Appendix: Demographics, Disease Presentation, and Treatment Methodology
Paul H. McClelland, Stephanie N. Gregory, Shirley K. Nah, Jonathan M. Hernandez, Jeremy L. Davis, Andrew M. Blakely
Annals of Surgical Oncology.2024; 31(9): 6237. CrossRef - Histoséminaire biopsies péritonéales tumorales. Néoplasies mucineuses appendiculaires
Peggy Dartigues
Annales de Pathologie.2024; 44(4): 274. CrossRef - Histoséminaire biopsies péritonéales tumorales. Cas no 2
Peggy Dartigues
Annales de Pathologie.2024; 44(4): 245. CrossRef - A Case of Low-Grade Appendiceal Mucinous Neoplasm: The Role of Preoperative Imaging and Surgical Technique in Achieving Favorable Outcomes
Daniel A Meza-Martinez, Yeudiel Suro Santos, Samantha J Andrade-Ordoñez, Julio A Palomino-Payan, Brando J Fematt-Rodriguez
Cureus.2024;[Epub] CrossRef - Incidental Appendiceal Mucinous Neoplasm Found During Appendectomy in a 15-Year-Old Patient: A Case Report
Fernando Aguilar-Ruiz, Kevin Joseph Fuentes-Calvo, Sara Fernanda Arechavala-Lopez, Irving Fuentes-Calvo, Luis F Arias-Ruiz
Cureus.2024;[Epub] CrossRef - Uncovering the Hidden Threat: Ileocolic Intussusception in an Adult With Appendicular Tumor
Mrunal Panchal, Shishir Kumar, Khushboo Jha, Kaushik Saha, Abhijit Kundu
Cureus.2024;[Epub] CrossRef - Low-Grade Appendiceal Mucinous Neoplasm vs. Appendiceal Diverticulum: Distinction with Histomorphologic Features
Cevriye Cansiz Ersöz, Siyar Ersöz, Berna Savas, Arzu Ensari
Gastrointestinal Disorders.2024; 6(4): 905. CrossRef - Appendiceal perforation secondary to endometriosis with intestinal metaplasia: A case report
Minghua Wang, Jing Liu, Boxin Hu, Simin Wang, Ping Xie, Ping Li
Experimental and Therapeutic Medicine.2023;[Epub] CrossRef - Primary and secondary tumors of the peritoneum: key imaging features and differential diagnosis with surgical and pathological correlation
Javier Miguez González, Francesc Calaf Forn, Laura Pelegrí Martínez, Pilar Lozano Arranz, Rafael Oliveira Caiafa, Jordi Català Forteza, Lina Maria Palacio Arteaga, Ferrán Losa Gaspà, Isabel Ramos Bernadó, Pedro Barrios Sánchez, Juan Ramón Ayuso Colella
Insights into Imaging.2023;[Epub] CrossRef - Muzinöse Tumoren des Peritoneums
Anne Kristin Fischer, Andrea Tannapfel, Alexander Quaas
Die Chirurgie.2023; 94(10): 823. CrossRef - Landscape of Genetic Mutations in Appendiceal Cancers
Marian Constantin, Cristina Mătanie, Livia Petrescu, Alexandra Bolocan, Octavian Andronic, Coralia Bleotu, Mihaela Magdalena Mitache, Sorin Tudorache, Corneliu Ovidiu Vrancianu
Cancers.2023; 15(14): 3591. CrossRef - Delivery of an Incidental Appendiceal Mucinous Neoplasm
Madison Bowles, Jessica Y Ng, Hajir Nabi
Cureus.2022;[Epub] CrossRef - Unearthing novel fusions as therapeutic targets in solid tumors using targeted RNA sequencing
Sungbin An, Hyun Hee Koh, Eun Sol Chang, Juyoung Choi, Ji-Young Song, Mi-Sook Lee, Yoon-La Choi
Frontiers in Oncology.2022;[Epub] CrossRef
- The clinical and pathological features of low-grade appendiceal mucinous neoplasm (LAMN)
- Standardized Pathology Report for Colorectal Cancer, 2nd Edition
- Baek-hui Kim, Joon Mee Kim, Gyeong Hoon Kang, Hee Jin Chang, Dong Wook Kang, Jung Ho Kim, Jeong Mo Bae, An Na Seo, Ho Sung Park, Yun Kyung Kang, Kyung-Hwa Lee, Mee Yon Cho, In-Gu Do, Hye Seung Lee, Hee Kyung Chang, Do Youn Park, Hyo Jeong Kang, Jin Hee Sohn, Mee Soo Chang, Eun Sun Jung, So-Young Jin, Eunsil Yu, Hye Seung Han, Youn Wha Kim
- J Pathol Transl Med. 2020;54(1):1-19. Published online November 13, 2019
- DOI: https://doi.org/10.4132/jptm.2019.09.28
- 31,401 View
- 1,339 Download
- 46 Web of Science
- 41 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - The first edition of the ‘Standardized Pathology Report for Colorectal Cancer,’ which was developed by the Gastrointestinal Pathology Study Group (GIP) of the Korean Society of Pathologists, was published 13 years ago. Meanwhile, there have been many changes in the pathologic diagnosis of colorectal cancer (CRC), pathologic findings included in the pathology report, and immunohistochemical and molecular pathology required for the diagnosis and treatment of colorectal cancer. In order to reflect these changes, we (GIP) decided to make the second edition of the report. The purpose of this standardized pathology report is to provide a practical protocol for Korean pathologists, which could help diagnose and treat CRC patients. This report consists of “standard data elements” and “conditional data elements.” Basic pathologic findings and parts necessary for prognostication of CRC patients are classified as “standard data elements,” while other prognostic factors and factors related to adjuvant therapy are classified as “conditional data elements” so that each institution could select the contents according to the characteristics of the institution. The Korean version is also provided separately so that Korean pathologists can easily understand and use this report. We hope that this report will be helpful in the daily practice of CRC diagnosis.
-
Citations
Citations to this article as recorded by- Proteogenomic profiling predicts outcomes of adjuvant chemotherapy in extrahepatic cholangiocarcinoma
Hyehyun Jeong, Ji-Hye Oh, Hee-Sung Ahn, Baek-Yeol Ryoo, Kyu-pyo Kim, Jae Ho Jeong, Inkeun Park, Dae Wook Hwang, Jae Hoon Lee, Ki Byung Song, Woohyung Lee, Ki-Hun Kim, Deog-Bog Moon, Gi Won Song, Dong-Hwan Jung, Seung-Mo Hong, Chae Won Park, In-Pyo Baek, Y
Journal of Hepatology.2026; 84(1): 122. CrossRef - A study on the effect of CBSM-based psychological intervention on self-management ability and quality of life in colorectal cancer patients from the perspective of benefit finding: A quasi-experimental study
Linzhi Jiang, Zhouyuan Peng, Rongrong Liu, Lei Chen, Yang Wu, Xingqun Tan, Fan Wang, Liyuan Sun, Chong-Chi Chiu
PLOS One.2026; 21(1): e0339472. CrossRef - Impact of gross tumor morphology on the clinical outcomes of colon cancer: multicenter retrospective cohort study
So Jung Han, Hyun Seok Lee, Byung Ik Jang, Jae Hyun Kim, Hyun Gun Kim, Il Hyun Baek, Jun Lee, Bun Kim, Dae Bum Kim, Jae Jun Park
International Journal of Colorectal Disease.2026;[Epub] CrossRef - Vitrification-based tissue-to-organoid cryopreservation workflow for colorectal cancer
Juyoung Choi, Hye Kyung Hong, Mi-Sook Lee, Ye Jin Lim, Yurimi Lee, Yong Beom Cho, Yoon-La Choi
New Biotechnology.2026; 93: 341. CrossRef - Diagnostic accuracy and pitfalls of MRI for restaging locally advanced rectal cancer in patients following anti-PD1 therapy plus neoadjuvant chemoradiotherapy: a multicenter study
Lixue Xu, Liting Sun, Yuhuan Fu, Guangyong Chen, Hongwei Yao, Zhenchang Wang, Zhenghan Yang, Jie Zhang
Abdominal Radiology.2025; 51(1): 14. CrossRef - Unraveling the role of perineural invasion in cancer progression across multiple tumor types
Muqtada Shaikh, Sanket Shirodkar, Gaurav Doshi
Medical Oncology.2025;[Epub] CrossRef - MALT lymphoma affecting the oral cavity: a clinical, pathologic and genetic study of MALT1 gene translocation
Juan Manuel Arteaga Legarrea, Mauro Lima dos Santos, Nathalia Gomes Rodrigues, Ricardo Santiago Gomez, Ricardo Alves Mesquita, Silvia Ferreira de Sousa, Cinthia Verónica Bardález López de Cáceres, Hélder Antônio Rebelo Pontes, Pablo Agustin Vargas, Luiz A
Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology.2025; 140(6): 740. CrossRef - Additional staining for lymphovascular invasion is associated with increased estimation of lymph node metastasis in patients with T1 colorectal cancer: Systematic review and meta‐analysis
Jun Watanabe, Katsuro Ichimasa, Yuki Kataoka, Atsushi Miki, Hidehiro Someko, Munenori Honda, Makiko Tahara, Takeshi Yamashina, Khay Guan Yeoh, Shigeo Kawai, Kazuhiko Kotani, Naohiro Sata
Digestive Endoscopy.2024; 36(5): 533. CrossRef - The use of core descriptors from the ENiGMA code study in recent literature: a systematic review
Saher‐Zahra Khan, Andrea Arline, Kate M. Williams, Matthew J. Lee, Emily Steinhagen, Sharon L. Stein
Colorectal Disease.2024; 26(3): 428. CrossRef - Efficacy and safety of PD-1 blockade plus long-course chemoradiotherapy in locally advanced rectal cancer (NECTAR): a multi-center phase 2 study
Zhengyang Yang, Jiale Gao, Jianyong Zheng, Jiagang Han, Ang Li, Gang Liu, Yi Sun, Jie Zhang, Guangyong Chen, Rui Xu, Xiao Zhang, Yishan Liu, Zhigang Bai, Wei Deng, Wei He, Hongwei Yao, Zhongtao Zhang
Signal Transduction and Targeted Therapy.2024;[Epub] CrossRef - Diagnostic Accuracy of Highest-Grade or Predominant Histological Differentiation of T1 Colorectal Cancer in Predicting Lymph Node Metastasis: A Systematic Review and Meta-Analysis
Jun Watanabe, Katsuro Ichimasa, Yuki Kataoka, Shoko Miyahara, Atsushi Miki, Khay Guan Yeoh, Shigeo Kawai, Fernando Martínez de Juan, Isidro Machado, Kazuhiko Kotani, Naohiro Sata
Clinical and Translational Gastroenterology.2024; 15(3): e00673. CrossRef - Comparative evaluation of CT and MRI in the preoperative staging of colon cancer
Effrosyni Bompou, Aikaterini Vassiou, Ioannis Baloyiannis, Konstantinos Perivoliotis, Ioannis Fezoulidis, George Tzovaras
Scientific Reports.2024;[Epub] CrossRef - Pathologic Implications of Magnetic Resonance Imaging-detected Extramural Venous Invasion of Rectal Cancer
Hyun Gu Lee, Chan Wook Kim, Jong Keon Jang, Seong Ho Park, Young Il Kim, Jong Lyul Lee, Yong Sik Yoon, In Ja Park, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Clinical Colorectal Cancer.2023; 22(1): 129. CrossRef - A standardized pathology report for gastric cancer: 2nd edition
Young Soo Park, Myeong-Cherl Kook, Baek-hui Kim, Hye Seung Lee, Dong-Wook Kang, Mi-Jin Gu, Ok Ran Shin, Younghee Choi, Wonae Lee, Hyunki Kim, In Hye Song, Kyoung-Mee Kim, Hee Sung Kim, Guhyun Kang, Do Youn Park, So-Young Jin, Joon Mee Kim, Yoon Jung Choi,
Journal of Pathology and Translational Medicine.2023; 57(1): 1. CrossRef - IGFL2-AS1, a Long Non-Coding RNA, Is Associated with Radioresistance in Colorectal Cancer
Jeeyong Lee, Da Yeon Kim, Younjoo Kim, Ui Sup Shin, Kwang Seok Kim, Eun Ju Kim
International Journal of Molecular Sciences.2023; 24(2): 978. CrossRef - A Standardized Pathology Report for Gastric Cancer: 2nd Edition
Young Soo Park, Myeong-Cherl Kook, Baek-hui Kim, Hye Seung Lee, Dong-Wook Kang, Mi-Jin Gu, Ok Ran Shin, Younghee Choi, Wonae Lee, Hyunki Kim, In Hye Song, Kyoung-Mee Kim, Hee Sung Kim, Guhyun Kang, Do Youn Park, So-Young Jin, Joon Mee Kim, Yoon Jung Choi,
Journal of Gastric Cancer.2023; 23(1): 107. CrossRef - Incremental Detection Rate of Dysplasia and Sessile Serrated Polyps/Adenomas Using Narrow-Band Imaging and Dye Spray Chromoendoscopy in Addition to High-Definition Endoscopy in Patients with Long-Standing Extensive Ulcerative Colitis: Segmental Tandem End
Ji Eun Kim, Chang Wan Choi, Sung Noh Hong, Joo Hye Song, Eun Ran Kim, Dong Kyung Chang, Young-Ho Kim
Diagnostics.2023; 13(3): 516. CrossRef - Prognostic Impact of Extramural Lymphatic, Vascular, and Perineural Invasion in Stage II Colon Cancer: A Comparison With Intramural Invasion
Sang Sik Cho, Ji Won Park, Gyeong Hoon Kang, Jung Ho Kim, Jeong Mo Bae, Sae-Won Han, Tae-You Kim, Min Jung Kim, Seung-Bum Ryoo, Seung-Yong Jeong, Kyu Joo Park
Diseases of the Colon & Rectum.2023; 66(3): 366. CrossRef - Towards targeted colorectal cancer biopsy based on tissue morphology assessment by compression optical coherence elastography
Anton A. Plekhanov, Marina A. Sirotkina, Ekaterina V. Gubarkova, Elena B. Kiseleva, Alexander A. Sovetsky, Maria M. Karabut, Vladimir E. Zagainov, Sergey S. Kuznetsov, Anna V. Maslennikova, Elena V. Zagaynova, Vladimir Y. Zaitsev, Natalia D. Gladkova
Frontiers in Oncology.2023;[Epub] CrossRef - Is High-Grade Tumor Budding an Independent Prognostic Factor in Stage II Colon Cancer?
Jung Kyong Shin, Yoon Ah Park, Jung Wook Huh, Seong Hyeon Yun, Hee Cheol Kim, Woo Yong Lee, Seok Hyung Kim, Sang Yun Ha, Yong Beom Cho
Diseases of the Colon & Rectum.2023; 66(8): e801. CrossRef - Detection of Human cytomegalovirus UL55 Gene and IE/E Protein Expression in Colorectal Cancer Patients in Egypt
May Raouf, Ahmed A. Sabry, Mahinour A. Ragab, Samar El Achy, Amira Amer
BMC Cancer.2023;[Epub] CrossRef - Polo-like kinase 4 as a potential predictive biomarker of chemoradioresistance in locally advanced rectal cancer
Hyunseung Oh, Soon Gu Kim, Sung Uk Bae, Sang Jun Byun, Shin Kim, Jae-Ho Lee, Ilseon Hwang, Sun Young Kwon, Hye Won Lee
Journal of Pathology and Translational Medicine.2022; 56(1): 40. CrossRef - A Prediction Model for Tumor Recurrence in Stage II–III Colorectal Cancer Patients: From a Machine Learning Model to Genomic Profiling
Po-Chuan Chen, Yu-Min Yeh, Bo-Wen Lin, Ren-Hao Chan, Pei-Fang Su, Yi-Chia Liu, Chung-Ta Lee, Shang-Hung Chen, Peng-Chan Lin
Biomedicines.2022; 10(2): 340. CrossRef - Rationale and design of a prospective, multicenter, phase II clinical trial of safety and efficacy evaluation of long course neoadjuvant chemoradiotherapy plus tislelizumab followed by total mesorectal excision for locally advanced rectal cancer (NCRT-PD1
Zhengyang Yang, Xiao Zhang, Jie Zhang, Jiale Gao, Zhigang Bai, Wei Deng, Guangyong Chen, Yongbo An, Yishan Liu, Qi Wei, Jiagang Han, Ang Li, Gang Liu, Yi Sun, Dalu Kong, Hongwei Yao, Zhongtao Zhang
BMC Cancer.2022;[Epub] CrossRef - Potential of DEK proto‑oncogene as a prognostic biomarker for colorectal cancer: An evidence‑based review
Muhammad Habiburrahman, Muhammad Wardoyo, Stefanus Sutopo, Nur Rahadiani
Molecular and Clinical Oncology.2022;[Epub] CrossRef - Reproducibility and Feasibility of Classification and National Guidelines for Histological Diagnosis of Canine Mammary Gland Tumours: A Multi-Institutional Ring Study
Serenella Papparella, Maria Crescio, Valeria Baldassarre, Barbara Brunetti, Giovanni Burrai, Cristiano Cocumelli, Valeria Grieco, Selina Iussich, Lorella Maniscalco, Francesca Mariotti, Francesca Millanta, Orlando Paciello, Roberta Rasotto, Mariarita Roma
Veterinary Sciences.2022; 9(7): 357. CrossRef - Composite scoring system and optimal tumor budding cut-off number for estimating lymph node metastasis in submucosal colorectal cancer
Jeong-ki Kim, Ye-Young Rhee, Jeong Mo Bae, Jung Ho Kim, Seong-Joon Koh, Hyun Jung Lee, Jong Pil Im, Min Jung Kim, Seung-Bum Ryoo, Seung-Yong Jeong, Kyu Joo Park, Ji Won Park, Gyeong Hoon Kang
BMC Cancer.2022;[Epub] CrossRef - Automated Hybrid Model for Detecting Perineural Invasion in the Histology of Colorectal Cancer
Jiyoon Jung, Eunsu Kim, Hyeseong Lee, Sung Hak Lee, Sangjeong Ahn
Applied Sciences.2022; 12(18): 9159. CrossRef - Clinical Implication of Perineural and Lymphovascular Invasion in Rectal Cancer Patients Who Underwent Surgery After Preoperative Chemoradiotherapy
Young Il Kim, Chan Wook Kim, Jong Hoon Kim, Jihun Kim, Jun-Soo Ro, Jong Lyul Lee, Yong Sik Yoon, In Ja Park, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Diseases of the Colon & Rectum.2022; 65(11): 1325. CrossRef - Molecular Pathology of Gastric Cancer
Moonsik Kim, An Na Seo
Journal of Gastric Cancer.2022; 22(4): 264. CrossRef - Selective approach to arterial ligation in radical sigmoid colon cancer surgery with D3 lymph node dissection: A multicenter comparative study
Sergey Efetov, Albina Zubayraeva, Cüneyt Kayaalp, Alisa Minenkova, Yusuf Bağ, Aftandil Alekberzade, Petr Tsarkov
Turkish Journal of Surgery.2022; 38(4): 382. CrossRef - Evaluation of lncRNA FOXD2-AS1 Expression as a Diagnostic Biomarker in Colorectal Cancer
Hooman Shalmashi, Sahar Safaei, Dariush Shanehbandi, Milad Asadi, Soghra Bornehdeli, Abdolreza Mehdi Navaz
Reports of Biochemistry and Molecular Biology.2022; 11(3): 471. CrossRef - Improvement in the Assessment of Response to Preoperative Chemoradiotherapy for Rectal Cancer Using Magnetic Resonance Imaging and a Multigene Biomarker
Eunhae Cho, Sung Woo Jung, In Ja Park, Jong Keon Jang, Seong Ho Park, Seung-Mo Hong, Jong Lyul Lee, Chan Wook Kim, Yong Sik Yoon, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Cancers.2021; 13(14): 3480. CrossRef - Addition of V-Stage to Conventional TNM Staging to Create the TNVM Staging System for Accurate Prediction of Prognosis in Colon Cancer: A Multi-Institutional Retrospective Cohort Study
Jung Hoon Bae, Ji Hoon Kim, Jaeim Lee, Bong-Hyeon Kye, Sang Chul Lee, In Kyu Lee, Won Kyung Kang, Hyeon-Min Cho, Yoon Suk Lee
Biomedicines.2021; 9(8): 888. CrossRef - Gene Expression Profiles Associated with Radio-Responsiveness in Locally Advanced Rectal Cancer
Jeeyong Lee, Junhye Kwon, DaYeon Kim, Misun Park, KwangSeok Kim, InHwa Bae, Hyunkyung Kim, JoonSeog Kong, Younjoo Kim, UiSup Shin, EunJu Kim
Biology.2021; 10(6): 500. CrossRef - A Patient-Derived Organoid-Based Radiosensitivity Model for the Prediction of Radiation Responses in Patients with Rectal Cancer
Misun Park, Junhye Kwon, Joonseog Kong, Sun Mi Moon, Sangsik Cho, Ki Young Yang, Won Il Jang, Mi Sook Kim, Younjoo Kim, Ui Sup Shin
Cancers.2021; 13(15): 3760. CrossRef - Comparison between Local Excision and Radical Resection for the Treatment of Rectal Cancer in ypT0-1 Patients: An Analysis of the Clinicopathological Factors and Survival Rates
Soo Young Oh, In Ja Park, Young IL Kim, Jong-Lyul Lee, Chan Wook Kim, Yong Sik Yoon, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Cancers.2021; 13(19): 4823. CrossRef - Comparison of Vascular Invasion With Lymph Node Metastasis as a Prognostic Factor in Stage I-III Colon Cancer: An Observational Cohort Study
Jung Hoon Bae, Ji Hoon Kim, Bong-Hyeon Kye, Abdullah Al-Sawat, Chul Seung Lee, Seung-Rim Han, In Kyu Lee, Sung Hak Lee, Yoon Suk Lee
Frontiers in Surgery.2021;[Epub] CrossRef - Clinicopathological significance of Ki67 expression in colorectal cancer
Jing Li, Zhi-ye Liu, Hai-bo Yu, Qing Xue, Wen-jie He, Hai-tao Yu
Medicine.2020; 99(20): e20136. CrossRef - Lateral lymph node and its association with distant recurrence in rectal cancer: A clue of systemic disease
Young Il Kim, Jong Keon Jang, In Ja Park, Seong Ho Park, Jong Beom Kim, Jin-Hong Park, Tae Won Kim, Jun-Soo Ro, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Surgical Oncology.2020; 35: 174. CrossRef - Transformation of Pathology Reports Into the Common Data Model With Oncology Module: Use Case for Colon Cancer
Borim Ryu, Eunsil Yoon, Seok Kim, Sejoon Lee, Hyunyoung Baek, Soyoung Yi, Hee Young Na, Ji-Won Kim, Rong-Min Baek, Hee Hwang, Sooyoung Yoo
Journal of Medical Internet Research.2020; 22(12): e18526. CrossRef
- Proteogenomic profiling predicts outcomes of adjuvant chemotherapy in extrahepatic cholangiocarcinoma
- Gastric Langerhans Cell Histiocytosis: Case Report and Review of the Literature
- So Jung Lee, Chung Su Hwang, Gi Young Huh, Chang Hun Lee, Do Youn Park
- J Pathol Transl Med. 2015;49(5):421-423. Published online June 9, 2015
- DOI: https://doi.org/10.4132/jptm.2015.05.19
- 11,917 View
- 73 Download
- 9 Web of Science
- 11 Crossref
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Gastric Langerhans Cell Histiocytosis is Easily Ignored or Misdiagnosed in Stomach Biopsy and Indicates a Poor Outcome in Multisystem Langerhans Cell Histiocytosis
Yue Fan, Yang Liu, Haimin Xu, Lei Zhang, Fei Yuan, Hongmei Yi, Chaofu Wang
International Journal of Surgical Pathology.2026; 34(3): 640. CrossRef - Clinicopathological features of gastric Langerhans cell histiocytosis and a literature review
Xue Chen, Yunjin Wu, Xueli Wang, Muye Yang, Xiaoxiang Gao, Suxia Zhang, Huihui Sun, Yunhui Zhang, Hongmei Yi, Yu Zeng
Journal of Clinical and Experimental Hematopathology.2026; 66(1): 11. CrossRef - Isolated Adult Gastrointestinal Tract Langerhans Cell Histiocytosis—Report of Two Rare Patients with Review of Literature
Ekta Jain, Eric Ollila, Fatme Ghandour, Abrar Alghamdi, Samuel Borak, Sameer Al Diffalha
International Journal of Surgical Pathology.2025; 33(7): 1679. CrossRef - Isolated Langerhans cell histiocytosis in the stomach of adults: four-case series and literature review
Jianmin Zhao, Yanlei Li, Yanlin Zhang, Xue Mei, Wei Liu, Yinghong Li
Journal of Hematopathology.2024; 17(2): 63. CrossRef - Clinical Characteristics and Outcomes in Patients With Localized Gastric Langerhans Cell Histiocytosis: A Case Series
Tae-Se Kim, Soomin Ahn, Yang Won Min, Hyuk Lee, Jun Haeng Lee, Poong-Lyul Rhee, Jae J. Kim, Byung-Hoon Min
The Korean Journal of Helicobacter and Upper Gastrointestinal Research.2024; 24(2): 175. CrossRef - Isolated Langerhans cell histiocytosis of the stomach in adults: An analysis of clinicopathologic characteristics and molecular genetics
Ruinuan Wu, Yali Zhao, Xikang Wu, Huihui Gui, Xia Liu, Zhaohui Liu
Medicine.2024; 103(51): e40950. CrossRef - Unifocal Gastric Langerhans Cell Histiocytosis in a Child—A Unique Case to Remember
Bhaswati C. Acharyya, Mandira Roy, Hema Chakraborty
JPGN Reports.2022;[Epub] CrossRef - Langerhans Cell Histiocytosis with the Synchronous Invasion of Stomach and Colon in an Adult Patient: A Case Report
Seong Je Kim, Se In Hah, Ji Yoon Kwak, Jung Woo Choi, Hyun Chin Cho, Chang Yoon Ha, Woon Tae Jung, Ok Jae Lee, Chang Min Lee
The Korean Journal of Gastroenterology.2022; 80(3): 149. CrossRef - Gastrointestinal Langerhans cell histiocytosis with unifocal, single‐system involvement in adults: Cases report and literature review
Li Wang, Fang Yang, Yong Ding, Lixia Lu, Haili Li, Yangyang Cui, Lu Lu, Xiaohan Shen, Rong Ge
Journal of Clinical Laboratory Analysis.2022;[Epub] CrossRef - Upper Gastrointestinal Langerhans Cell Histiocytosis: A Report of 2 Adult Cases and a Literature Review
Yui Matsuoka, Yoshiki Iemura, Masakazu Fujimoto, Shinsuke Shibuya, Atsushi Yamada, Shigehiko Fujii, Toshihiro Kusaka, Takero Shindo, Sachiko Minamiguchi, Hironori Haga
International Journal of Surgical Pathology.2021; 29(5): 550. CrossRef - Langerhans cell histiocytosis of the gastrointestinal tract
Aoife J. McCarthy, Madiha Emran Soofi, Imaad Mujeeb, Runjan Chetty
Diagnostic Histopathology.2018; 24(4): 154. CrossRef
- Gastric Langerhans Cell Histiocytosis is Easily Ignored or Misdiagnosed in Stomach Biopsy and Indicates a Poor Outcome in Multisystem Langerhans Cell Histiocytosis
- A Ciliated Cyst with Müllerian Differentiation Arising in the Posterior Mediastinum
- So Jung Lee, Chung Su Hwang, Do Youn Park, Gi Young Huh, Chang Hun Lee
- Korean J Pathol. 2014;48(5):401-404. Published online October 27, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.5.401
- 10,091 View
- 80 Download
- 11 Crossref
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Rare Posterior Mediastinal Müllerian Cyst Resected by VATS: Case Report and Literature Review
Małgorzata Edyta Wojtyś, Wiktoria Skórka, Miłosz Podsiadło, Konrad Ptaszyński, Katarzyna Rodak, Dominik Jakubowski, Tomasz Grodzki
Journal of Clinical Medicine.2026; 15(7): 2773. CrossRef - Cyst of Hattori: literature review and case presentation
R. B. Berdnikov, K. A. Andryuschenko, N. S. Zavarov, E. M. Petrunina, A. V. Bazhenov, A. S. Romakhin
PULMONOLOGIYA.2025; 35(4): 553. CrossRef - Cyst of Hattori: A Rare Cyst in the Posterior Mediastinum
Matthew D. Turner, Elicia Goodale, Barry C. Gibney, Maria Cecilia D. Reyes
International Journal of Surgical Pathology.2023; 31(4): 431. CrossRef - A large retroperitoneal Mullerian cyst: case report and review of the literature
Elena Parmentier, Jody Valk, Paul Willemsen, Caroline Mattelaer
Acta Chirurgica Belgica.2021; 121(4): 278. CrossRef - A case of resected Mullerian cyst in posterior mediastinum
Yoshiyuki Susaki, Noriyoshi Sawabata
The Journal of the Japanese Association for Chest Surgery.2020; 34(2): 137. CrossRef - Serosal Inclusion Cysts and Arteriovenous Fistulas in Paraprostatic Area of a Dog
Daisuke KOJIMA, Kyoko KOJIMA, Kazumi OTA, Yoshihiko KOJIMA
Journal of the Japan Veterinary Medical Association.2020; 73(9): 511. CrossRef - A surgical case of Mullerian cyst in the posterior mediastinum
Yusuke Kita, Yoshimasa Tokunaga, Taku Okamoto
The Journal of the Japanese Association for Chest Surgery.2019; 33(1): 68. CrossRef - CT and MRI characteristics for differentiating mediastinal Müllerian cysts from bronchogenic cysts
M. Kawaguchi, H. Kato, A. Hara, N. Suzui, H. Tomita, T. Miyazaki, H. Iwata, M. Matsuo
Clinical Radiology.2019; 74(12): 976.e19. CrossRef - A case of Mullerian cyst arising in the posterior mediastinum
Masahiro Adachi, Isao Sano, Shintaro Hashimoto, Ryoichiro Doi, Hideki Taniguchi, Kazuto Shigematsu
The Journal of the Japanese Association for Chest Surgery.2018; 32(6): 713. CrossRef - Two resected cases of Mullerian cyst in the posterior mediastinum
Shotaro Hashimoto, Masato Hisano, Masato Morimoto
The Journal of the Japanese Association for Chest Surgery.2018; 32(7): 818. CrossRef - Posterior mediastinal Müllerian cyst: a rare cause of pain in a young woman
Rebecca Weedle, Keith Conway, Igor Saftic, Alan Soo
Asian Cardiovascular and Thoracic Annals.2017; 25(6): 466. CrossRef
- Rare Posterior Mediastinal Müllerian Cyst Resected by VATS: Case Report and Literature Review
- Nodular Fasciitis of the Parotid Gland, Masquerading as Pleomorphic Adenoma
- Chung Su Hwang, Chang Hun Lee, Ahrong Kim, Nari Shin, Won Young Park, Min Gyoung Park, Do Youn Park
- Korean J Pathol. 2014;48(5):366-370. Published online October 27, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.5.366
- 9,556 View
- 56 Download
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF - It is difficult to distinguish nodular fasciitis (NF) from other neoplasm of the parotid gland, especially pleomorphic adenoma (PA) by fine needle aspiration cytology. A 39-year-old female noticed a mass in the parotid region. The aspirate material showed cohesive parts composed of the cells that had oval or spindle-shaped nuclei and relatively abundant cytoplasm and some cells with plasmacytoid features. The background substance was fibromyxoid. PA was diagnosed based on the cytologic findings. Subsequently, parotidectomy was performed and NF was diagnosed based on histologic and immunohistochemical findings. NF in the parotid region is rare and may be misdiagnosed as other benign or malignant tumors of the parotid gland. The clinical history of rapid growth and the presence of mitoses and inflammatory cells help to distinguish NF from PA. In addition, immunohistochemical stains for smooth muscle actin and CD68 are useful to confirm the diagnosis of NF.
-
Citations
Citations to this article as recorded by- A case report of nodular fasciitis of the parotid gland: An entity of concern
Andrea Varazzani, Laura Tognin, Silvia Eleonora Gazzani, Luigi Corcione, Tito Poli
Journal of Oral and Maxillofacial Surgery, Medicine, and Pathology.2024; 36(3): 422. CrossRef - Cytologic findings of nodular fasciitis in the parotid region
Yoshihiro KATO, Keiko TSUCHIDO, Makoto YAMADA, Yasuhiro AKAZAWA, Shogo MIZUNO, Yoshiro OTSUKI, Shin-ichi SHIMIZU, Hiroshi KOBAYASHI
The Journal of the Japanese Society of Clinical Cytology.2024; 63(3): 129. CrossRef - A Case of Parotid Nodular Fasciitis in Children and Literature Review
豆豆 屈
Advances in Clinical Medicine.2024; 14(10): 854. CrossRef - A Rare Case of Parotid Nodular Fasciitis in a Six-Month-Old Female
Mazin Merdad, Linah Qasim, Mohammed Nujoom, Hani Z Marzouki, Abdulaziz Neazy
Cureus.2023;[Epub] CrossRef - A rare case of nodular fasciitis presenting as a parotid tumor: Clues to cytodiagnosis
Seetu Palo, Chitrawati Bal Gargade
Journal of Laboratory Physicians.2023; 16: 124. CrossRef - Condylar Reshape in Orthognathic Surgery: Morphovolumetric and Densitometric Analysis Based on 3D Imaging and Digital Workflow
Vincenzo Abbate, Giovanni Audino, Giovanni Dell’Aversana Orabona, Marco Friscia, Paola Bonavolontà, Carmelo Lo Faro, Umberto Committeri, Carlos Navarro Cuéllar, Giorgio Iaconetta, Luigi Califano
Journal of Maxillofacial and Oral Surgery.2022; 21(2): 501. CrossRef - Nodular fasciitis of the submandibular gland
Ting Suen Wong, Richard Wei Chern Gan, Laszlo Karsai, Bun Yin Winson Wong
BMJ Case Reports.2022; 15(4): e245584. CrossRef - Nodular fasciitis in cervicofacial region: a rare case description and literature review
Vincenzo Abbate, Giovanni Dell’Aversana Orabona, Giovanni Audino, Antonio Romano, Paola Bonavolontà, Daniela Russo, Silvia Varricchio, Roberto Ferrigno, Giorgio Iaconetta, Luigi Califano
Oral Surgery.2022; 15(4): 550. CrossRef - Nodular fasciitis of the parotid gland engulfing the facial nerve: a conservative approach
Stephen Bennett, Kristian Hutson, Olakunle Ajayi, Andreas Hilger
BMJ Case Reports.2019; 12(10): e231203. CrossRef
- A case report of nodular fasciitis of the parotid gland: An entity of concern
- Mediastinal Thymolipoma with Striated Myoid Cells: Report of a Peculiar Case
- Young Keum Kim, Nari Shin, Won Young Park, Do Youn Park, Gi Young Huh, Chang Hun Lee
- Korean J Pathol. 2013;47(6):596-598. Published online December 24, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.6.596
- 9,274 View
- 46 Download
- 3 Crossref
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Thymoangiolipoma: A rare case of mediastinal tumor with a brief review of literature
Shahin Hameed, Shehla Basheer Kollathodi, Jaseela Beevirakath Puthiyapuryil, Bindu Rajkumar
Indian Journal of Pathology and Microbiology.2025; 68(4): 877. CrossRef - Thymoangiolipoma: A rare histologic variant of thymolipoma in a patient with myasthenia gravis
Mohammad Hossein Anbardar, Fatemeh Amirmoezi, Armin Amirian
Rare Tumors.2020;[Epub] CrossRef - Thymic epithelial neoplasms with rhabdomyomatous component: a clinicopathological and immunohistochemical study of 7 cases
Neda Kalhor, Cesar A. Moran
Human Pathology.2019; 83: 100. CrossRef
- Thymoangiolipoma: A rare case of mediastinal tumor with a brief review of literature
- Microsatellite Instability Status in Gastric Cancer: A Reappraisal of Its Clinical Significance and Relationship with Mucin Phenotypes
- Joo-Yeun Kim, Na Ri Shin, Ahrong Kim, Hyun-Jeong Lee, Won-young Park, Jee-Yeon Kim, Chang-Hun Lee, Gi-Young Huh, Do Youn Park
- Korean J Pathol. 2013;47(1):28-35. Published online February 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.1.28
- 13,498 View
- 128 Download
- 77 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Gastric cancers with microsatellite instabilities (MSI) have been reported to be associated with favorable prognosis. However, the significance of the effect of MSI on the clinicopathological features, as well as its association with mucin phenotype, remains unclear.
Methods MSI status was assessed in 414 cases of gastric cancer using polymerase chain reaction analysis of five microsatellite loci, as recommended by National Cancer Institution criteria. The expression of mucins (MUC5AC, MUC6, MUC2, and CD10) was assessed.
Results Out of 414 total cases of gastric cancer, 380 (91.7%), 11 (2.7%), and 23 (5.6%) were microsatellite stable (MSS), low-level MSI (MSI-L), and high-level MSI (MSI-H), respectively. Compared to MSS/MSI-L, MSI-H gastric cancers were associated with older age (p=0.010), tumor size (p=0.014), excavated gross (p=0.042), intestinal type (p=0.028), aggressive behaviors (increase of T stage [p=0.009]), perineural invasion [p=0.022], and lymphovascular emboli [p=0.027]). MSI-H gastric cancers were associated with tumor necrosis (p=0.041), tumor-infiltrating lymphocytes (≥2/high power field, p<0.001), expanding growth patterns (p=0.038), gastric predominant mucin phenotypes (p=0.028), and MUC6 expression (p=0.016). Tumor necrosis (≥10% of mass, p=0.031), tumor-infiltrating lymphocytes (p<0.001), intestinal type (p=0.014), and gastric mucin phenotypes (p=0.020) could represent independent features associated with MSI-H gastric cancers. MSI-H intestinal type gastric cancers had a tendency for poor prognosis in univariate analysis (p=0.054) but no association in Cox multivariate analysis (p=0.197).
Conclusions Our data suggest that MSI-H gastric cancers exhibit distinct aggressive biologic behaviors and a gastric mucin phenotype. This contradicts previous reports that describe MSI-H gastric cancer as being associated with favorable prognosis.
-
Citations
Citations to this article as recorded by- DNA Methylation in Gastric Cancer and Preneoplastic Lesions: Emerging Insights and Future Directions
Carlotta Ceccon, Giulia Maddalena, Valentina Angerilli, Floriana Nappo, Jessica Gasparello, Marianna Sabbadin, Luisa Toffolatti, Francesca Bergamo, Matteo Fassan, Sara Lonardi
Cancers.2026; 18(7): 1075. CrossRef - Intestinal Subtype as a Biomarker of Response to Neoadjuvant Immunochemotherapy in Locally Advanced Gastric Adenocarcinoma: Insights from a Prospective Phase II Trial
Lei Wang, Mengting Sun, Jinyang Li, Linghong Wan, Yuting Tan, Shuoran Tian, Yongying Hou, Linyu Wu, Ziyi Peng, Xiao Hu, Qihua Zhang, Zening Huang, Mengyi Han, Shiyin Peng, Yuwei Pan, Yuanfeng Ren, Mengsi Zhang, Dongfeng Chen, Qin Liu, Xianfeng Li, Zhong-y
Clinical Cancer Research.2025; 31(1): 74. CrossRef - How do I treat dMMR/MSI gastro-oesophageal adenocarcinoma in 2025? A position paper from the EORTC-GITCG gastro-esophageal task force
Christelle de la Fouchardière, Antonella Cammarota, Magali Svrcek, Maria Alsina, Tania Fleitas-Kanonnikoff, Radka Lordick Obermannová, Anna Dorothea Wagner, Dominic Yap Wei Ting, Diana Enea, Angelica Petrillo, Elizabeth C. Smyth
Cancer Treatment Reviews.2025; 134: 102890. CrossRef - T-bet+CD8+ T cells govern anti-PD-1 responses in microsatellite-stable gastric cancers
Shiying Tang, Xiaofang Che, Jinyan Wang, Ce Li, Xin He, Kezuo Hou, Xiaojie Zhang, Jia Guo, Bowen Yang, Danni Li, Lili Cao, Xiujuan Qu, Zhenning Wang, Yunpeng Liu
Nature Communications.2025;[Epub] CrossRef - Prediction of a Panel of Programmed Cell Death Protein-1 (PD-1) Inhibitor–Sensitive Biomarkers Using Multiphase Computed Tomography Imaging Textural Features: Retrospective Cohort Analysis
Shiqi Wang, Na Chai, Jingji Xu, Pengfei Yu, Luguang Huang, Quan Wang, Zhifeng Zhao, Bin Yang, Jiangpeng Wei, Xiangjie Wang, Gang Ji, Minwen Zheng
JMIR Cancer.2025; 11: e67379. CrossRef - Isolated tumor cell clusters (ITC) in lymph nodes and PD-L1 expression on tumor-associated immune cells are prognostic factors for microsatellite instable-high gastric cancers
Menghan Cui, Yangli Zhou, Yin Han, Nannan Chen, Min Zhao, Yan Wang, Fengxia He
Translational Oncology.2025; 59: 102465. CrossRef - Microsatellite Instability and BAT-26 Marker Expression in a Mexican Prostate Cancer Population with Different Gleason Scores
Ana K. Flores-Islas, Manuel A. Rico-Méndez, Marisol Godínez-Rubí, Martha Arisbeth Villanueva-Pérez, Erick Sierra-Díaz, Ana Laura Pereira-Suárez, Saul A. Beltrán-Ontiveros, Perla Y. Gutiérrez-Arzapalo, José M. Moreno-Ortiz, Adrián Ramírez-de-Arellano
Diseases.2025; 13(7): 202. CrossRef - Prognostic implications of ERBB2 amplification and mismatch repair in gastric adenocarcinoma: a single-center study
Han Xia, Zekang Li, Minyi Wang, Dachuan Zhang, Xiao Zheng, Jun Wu, Chen Wu
Gastrointestinal Tumors.2025;[Epub] CrossRef - Microsatellite Instability in Chronic Gastritis Associated with Gastric Cancer
A. V. Kononov, V. A. Rubtsov, E. V. Demidova, M. N. Parygina, A. G. Shimanskaya, S. I. Mozgovoi, E. G. Pomorgailo, М. V. Markelova
Russian Journal of Gastroenterology, Hepatology, Coloproctology.2025; 35(4): 48. CrossRef - Non–Pure Intestinal Phenotype as an Indicator of Progression in Sporadic Nonampullary Duodenal Adenomas: A Multicenter Retrospective Cohort Study
Ryotaro Uema, Yoshito Hayashi, Masato Komori, Narihiro Shibukawa, Noriko Hayashi, Masayoshi Horimoto, Takuya Yamada, Masashi Yamamoto, Satoshi Hiyama, Kazuo Kinoshita, Hideharu Ogiyama, Shinjiro Yamaguchi, Satoshi Egawa, Takashi Kanesaka, Minoru Kato, Shu
Clinical and Translational Gastroenterology.2024; 15(1): e00649. CrossRef - Intratumoral and peritumoral CT-based radiomics for predicting the microsatellite instability in gastric cancer
Xingchi Chen, Zijian Zhuang, Lin Pen, Jing Xue, Haitao Zhu, Lirong Zhang, Dongqing Wang
Abdominal Radiology.2024; 49(5): 1363. CrossRef - The tumor immune composition of mismatch repair deficient and Epstein-Barr virus-positive gastric cancer: A systematic review
J. Bos, T.S. Groen-van Schooten, C.P. Brugman, F.S. Jamaludin, H.W.M. van Laarhoven, S. Derks
Cancer Treatment Reviews.2024; 127: 102737. CrossRef - Potent therapeutic strategy in gastric cancer with microsatellite instability-high and/or deficient mismatch repair
Akira Ooki, Hiroki Osumi, Koichiro Yoshino, Kensei Yamaguchi
Gastric Cancer.2024; 27(5): 907. CrossRef - The mechanism of RGS5 regulating gastric cancer mismatch repair protein
Zhenwei Yang, Ranran Zhang, Jialong Liu, Sufang Tian, Hailin Zhang, Lingxiu Zeng, Yangyang Zhang, Liping Gao, Meng Wang, Wenqing Shan, Jing Liu
Molecular Carcinogenesis.2024; 63(9): 1750. CrossRef - Prognostic significance of microsatellite instability in patients with resectable gastric cancer
Marina Alessandra Pereira, Marcus Fernando Kodama Pertille Ramos, Leonardo Cardili, André Roncon Dias, Venancio Avancini Ferreira Alves, Evandro Sobroza de Mello, Ulysses Ribeiro
Journal of Gastrointestinal Surgery.2024; 28(10): 1687. CrossRef - Access to radiotherapy in improving gastric cancer care quality and equality
Minmin Wang, Kepei Huang, Xiaohan Fan, Jia Wang, Yinzi Jin, Zhi-Jie Zheng
Communications Medicine.2024;[Epub] CrossRef - Deep learning captures selective features for discrimination of microsatellite instability from pathologic tissue slides of gastric cancer
Sung Hak Lee, Yujin Lee, Hyun‐Jong Jang
International Journal of Cancer.2023; 152(2): 298. CrossRef - Novel Biomarkers of Gastric Cancer: Current Research and Future Perspectives
Yasushi Sato, Koichi Okamoto, Yutaka Kawano, Akinari Kasai, Tomoyuki Kawaguchi, Tamotsu Sagawa, Masahiro Sogabe, Hiroshi Miyamoto, Tetsuji Takayama
Journal of Clinical Medicine.2023; 12(14): 4646. CrossRef - The results of treatment for resectable gastric cancer with microsatellite instability
H. Sun, S. N. Nered, A. A. Tryakin, E. V. Artamonova, A. E. Kalinin, V. E. Bugaev, A. M. Stroganova, N. S. Besova, P. P. Arkhiri, V. I. Marshall, R. Sh. Abdulaeva, I. S. Stilidi
Surgery and Oncology.2023; 13(2): 17. CrossRef - Heterogeneity and Adjuvant Therapeutic Approaches in MSI-H/dMMR Resectable Gastric Cancer: Emerging Trends in Immunotherapy
Hui Wu, Wenyuan Ma, Congfa Jiang, Ning Li, Xin Xu, Yongfeng Ding, Haiping Jiang
Annals of Surgical Oncology.2023; 30(13): 8572. CrossRef - Dual-layer spectral-detector CT for predicting microsatellite instability status and prognosis in locally advanced gastric cancer
Yongjian Zhu, Peng Wang, Bingzhi Wang, Zhichao Jiang, Ying Li, Jun Jiang, Yuxin Zhong, Liyan Xue, Liming Jiang
Insights into Imaging.2023;[Epub] CrossRef - Concordance between microsatellite instability testing and immunohistochemistry for mismatch repair proteins and efficient screening of mismatch repair deficient gastric cancer
Gou Yamamoto, Tetsuya Ito, Okihide Suzuki, Nao Kamae, Miho Kakuta, Akemi Takahashi, Katsuya Iuchi, Tomio Arai, Hideyuki Ishida, Kiwamu Akagi
Oncology Letters.2023;[Epub] CrossRef - Low incidence of microsatellite instability in gastric cancers and its association with the clinicopathological characteristics: a comparative study
Fateme Fooladi Talari, Ali Bozorg, Sirous Zeinali, Mohammadreza Zali, Zhale Mohsenifar, Hamid Asadzadeh Aghdaei, Kaveh Baghaei
Scientific Reports.2023;[Epub] CrossRef - Mutational separation and clinical outcomes of TP53 and CDH1 in gastric cancer
He-Li Liu, Huan Peng, Chang-Hao Huang, Hai-Yan Zhou, Jie Ge
World Journal of Gastrointestinal Surgery.2023; 15(12): 2855. CrossRef - Genomic and Immunologic Markers of Intrinsic Resistance to Pembrolizumab Monotherapy in Microsatellite Instability-High Gastric Cancer: Observations from a Prospective Phase II Study
Haibo Qiu
Global Medical Genetics.2022; 09(02): 060. CrossRef - Clinicopathological features of PD-L1 protein expression, EBV positivity, and MSI status in patients with advanced gastric and esophagogastric junction adenocarcinoma in Japan
Tsutomu Yoshida, Go Ogura, Mikiko Tanabe, Takuo Hayashi, Chiho Ohbayashi, Mizutomo Azuma, Chikara Kunisaki, Yoichi Akazawa, Soji Ozawa, Sohei Matsumoto, Takayoshi Suzuki, Akira Mitoro, Tetsu Fukunaga, Akiko Shimizu, Go Fujimoto, Takashi Yao
Cancer Biology & Therapy.2022; 23(1): 191. CrossRef - Development of Tissue-Agnostic Treatments for Patients with Cancer
Steven Lemery, Lola Fashoyin-Aje, Leigh Marcus, Sandra Casak, Julie Schneider, Marc Theoret, Paul Kluetz, Richard Pazdur, Julia A. Beaver
Annual Review of Cancer Biology.2022; 6(1): 147. CrossRef - A multicenter study on the preoperative prediction of gastric cancer microsatellite instability status based on computed tomography radiomics
Xiuqun Liang, Yinbo Wu, Ying Liu, Danping Yu, Chencui Huang, Zhi Li
Abdominal Radiology.2022; 47(6): 2036. CrossRef - Combination of AKT1 and CDH1 mutations predicts primary resistance to immunotherapy in dMMR/MSI-H gastrointestinal cancer
Zhenghang Wang, Qi Zhang, Changsong Qi, Yuezong Bai, Feilong Zhao, Hui Chen, Zhongwu Li, Xicheng Wang, Mifen Chen, Jifang Gong, Zhi Peng, Xiaotian Zhang, Jinping Cai, Shiqing Chen, Xiaochen Zhao, Lin Shen, Jian Li
Journal for ImmunoTherapy of Cancer.2022; 10(6): e004703. CrossRef - Eldest gastric cancer patient with high microsatellite instability responding to pembrolizumab
Akinobu Wakasugi, Akinori Sasaki, Risa Okamoto, Yasuaki Motomura
International Cancer Conference Journal.2022; 12(1): 59. CrossRef - Baseline lesion number as an efficacy predictive and independent prognostic factor and its joint utility with TMB for PD-1 inhibitor treatment in advanced gastric cancer
Xiao-Li Wei, Jian-Ying Xu, De-Shen Wang, Dong-Liang Chen, Chao Ren, Jia-Ning Li, Feng Wang, Feng-Hua Wang, Rui-Hua Xu
Therapeutic Advances in Medical Oncology.2021;[Epub] CrossRef - Clinical and morphological portrait of tumors with microsatellite instability
A. A. Musaelyan, V. D. Nazarov, A. S. Budnikova, S. V. Lapin, S. L. Vorobyev, V. L. Emanuel, A. A. Zakharenko, S. V. Orlov
Advances in Molecular Oncology.2021; 8(2): 52. CrossRef - How to Best Exploit Immunotherapeutics in Advanced Gastric Cancer: Between Biomarkers and Novel Cell-Based Approaches
Michele Ghidini, Angelica Petrillo, Andrea Botticelli, Dario Trapani, Alessandro Parisi, Anna La Salvia, Elham Sajjadi, Roberto Piciotti, Nicola Fusco, Shelize Khakoo
Journal of Clinical Medicine.2021; 10(7): 1412. CrossRef - Microsatellite instability in Gastric Cancer: Between lights and shadows
Elisabetta Puliga, Simona Corso, Filippo Pietrantonio, Silvia Giordano
Cancer Treatment Reviews.2021; 95: 102175. CrossRef - Impact of microsatellite status on negative lymph node count and prognostic relevance after curative gastrectomy
Zhenghao Cai, Junjun Ma, Shuchun Li, Abe Fingerhut, Jing Sun, Lu Zang, Chao Yan, Wentao Liu, Zhenggang Zhu, Minhua Zheng
Journal of Surgical Oncology.2021;[Epub] CrossRef - A greater lymph node yield is required during pathological examination in microsatellite instability-high gastric cancer
Zhenghao Cai, Haiqin Song, Abe Fingerhut, Jing Sun, Junjun Ma, Luyang Zhang, Shuchun Li, Chaoran Yu, Minhua Zheng, Lu Zang
BMC Cancer.2021;[Epub] CrossRef - Determinants of Response and Intrinsic Resistance to PD-1 Blockade in Microsatellite Instability–High Gastric Cancer
Minsuk Kwon, Minae An, Samuel J. Klempner, Hyuk Lee, Kyoung-Mee Kim, Jason K. Sa, Hee Jin Cho, Jung Yong Hong, Taehyang Lee, Yang Won Min, Tae Jun Kim, Byung-Hoon Min, Woong-Yang Park, Won Ki Kang, Kyu-Tae Kim, Seung Tae Kim, Jeeyun Lee
Cancer Discovery.2021; 11(9): 2168. CrossRef - Advanced Gastric Cancer: Current Treatment Landscape and a Future Outlook for Sequential and Personalized Guide: Swiss Expert Statement Article
Alexander R. Siebenhüner, Sara De Dosso, Daniel Helbling, Christoforos Astaras, Petr Szturz, Peter Moosmann, Stefanie Pederiva, Thomas Winder, Philippe Von Burg, Markus Borner
Oncology Research and Treatment.2021; 44(9): 485. CrossRef - High homogeneity of mismatch repair deficiency in advanced prostate cancer
Christoph Fraune, Ronald Simon, Doris Höflmayer, Katharina Möller, David Dum, Franziska Büscheck, Claudia Hube-Magg, Georgia Makrypidi-Fraune, Martina Kluth, Andrea Hinsch, Eike Burandt, Till Sebastian Clauditz, Waldemar Wilczak, Guido Sauter, Stefan Steu
Virchows Archiv.2020; 476(5): 745. CrossRef - High homogeneity of MMR deficiency in ovarian cancer
Christoph Fraune, Janina Rosebrock, Ronald Simon, Claudia Hube-Magg, Georgia Makrypidi-Fraune, Martina Kluth, Franziska Büscheck, Doris Höflmayer, Barbara Schmalfeldt, Volkmar Müller, Linn Wölber, Isabell Witzel, Peter Paluchowski, Christian Wilke, Uwe He
Gynecologic Oncology.2020; 156(3): 669. CrossRef - Molecular Classification of Gastric Cancer among Alaska Native People
Holly Martinson, Dominic Mallari, Christine Richter, Tsung-Teh Wu, James Tiesinga, Steven Alberts, Matthew Olnes
Cancers.2020; 12(1): 198. CrossRef - Tumor immune response and immunotherapy in gastric cancer
Yoonjin Kwak, An Na Seo, Hee Eun Lee, Hye Seung Lee
Journal of Pathology and Translational Medicine.2020; 54(1): 20. CrossRef - MMR deficiency in urothelial carcinoma of the bladder presents with temporal and spatial homogeneity throughout the tumor mass
Christoph Fraune, Ronald Simon, Claudia Hube-Magg, Georgia Makrypidi-Fraune, Christian Kähler, Martina Kluth, Doris Höflmayer, Franziska Büscheck, David Dum, Andreas M. Luebke, Eike Burandt, Till Sebastian Clauditz, Waldemar Wilczak, Guido Sauter, Stefan
Urologic Oncology: Seminars and Original Investigations.2020; 38(5): 488. CrossRef - MMR Deficiency is Homogeneous in Pancreatic Carcinoma and Associated with High Density of Cd8-Positive Lymphocytes
Christoph Fraune, Eike Burandt, Ronald Simon, Claudia Hube-Magg, Georgia Makrypidi-Fraune, Martina Kluth, Franziska Büscheck, Doris Höflmayer, Niclas Ch. Blessin, Tim Mandelkow, Wenchao Li, Daniel Perez, Jakob R. Izbicki, Waldemar Wilczak, Guido Sauter, J
Annals of Surgical Oncology.2020; 27(10): 3997. CrossRef - CD73's Potential as an Immunotherapy Target in Gastrointestinal Cancers
Jerry B. Harvey, Luan H. Phan, Oscar E. Villarreal, Jessica L. Bowser
Frontiers in Immunology.2020;[Epub] CrossRef - Tumor copy-number alterations predict response to immune-checkpoint-blockade in gastrointestinal cancer
Zhihao Lu, Huan Chen, Shuang Li, Jifang Gong, Jian Li, Jianling Zou, Lihong Wu, Jianing Yu, Wenbo Han, Huaibo Sun, Xi Jiao, Xiaotian Zhang, Zhi Peng, Ming Lu, Zhenghang Wang, Henghui Zhang, Lin Shen
Journal for ImmunoTherapy of Cancer.2020; 8(2): e000374. CrossRef - Protein expression-based classification of gastric cancer by immunohistochemistry of tissue microarray
Chong Zhao, Zhiqiang Feng, Hongzhen He, Dan Zang, Hong Du, Hongli Huang, Yanlei Du, Jie He, Yongjian Zhou, Yuqiang Nie, Girijesh Kumar Patel
PLOS ONE.2020; 15(10): e0238836. CrossRef - Clinicopathologic Characteristics and Long-Term Outcome of Gastric Cancer Patients with Family History: Seven-Year Follow-Up Study for Korean Health Check-Up Subjects
Jooyoung Lee, Su Jin Chung, Ji Min Choi, Yoo Min Han, Joo Sung Kim, Greger Lindberg
Gastroenterology Research and Practice.2020; 2020: 1. CrossRef - Implication of expression of MMR proteins and clinicopathological characteristics in gastric cancer
Renu Verma, Puja Sakhuja, Ritu Srivastava, Prakash Chand Sharma
Asia-Pacific Journal of Oncology.2020; : 1. CrossRef - Prognostic significance of microsatellite‐instability in gastric and gastroesophageal junction cancer patients undergoing neoadjuvant chemotherapy
Georg Martin Haag, Elena Czink, Aysel Ahadova, Thomas Schmidt, Leila Sisic, Susanne Blank, Ulrike Heger, Leonidas Apostolidis, Anne Katrin Berger, Christoph Springfeld, Felix Lasitschka, Dirk Jäger, Magnus von Knebel Doeberitz, Matthias Kloor
International Journal of Cancer.2019; 144(7): 1697. CrossRef - Serological Markers Associated With Response to Immune Checkpoint Blockade in Metastatic Gastrointestinal Tract Cancer
Zhihao Lu, Jianling Zou, Ying Hu, Shuang Li, Tao Zhou, Jifang Gong, Jian Li, Xiaotian Zhang, Jun Zhou, Ming Lu, Xicheng Wang, Zhi Peng, Changsong Qi, Yanyan Li, Jie Li, Yan Li, Jianyin Zou, Xiao Du, Henghui Zhang, Lin Shen
JAMA Network Open.2019; 2(7): e197621. CrossRef - Assessing molecular subtypes of gastric cancer: microsatellite unstable and Epstein-Barr virus subtypes. Methods for detection and clinical and pathological implications
Carolina Martinez-Ciarpaglini, Tania Fleitas-Kanonnikoff, Valentina Gambardella, Marta Llorca, Cristina Mongort, Regina Mengual, Gema Nieto, Lara Navarro, Marisol Huerta, Susana Rosello, Desamparados Roda, Noelia Tarazona, Samuel Navarro, Gloria Ribas, An
ESMO Open.2019; 4(3): e000470. CrossRef - The role of pembrolizumab in the treatment of PD-L1 expressing gastric and gastroesophageal junction adenocarcinoma
Gagandeep Brar, Manish A. Shah
Therapeutic Advances in Gastroenterology.2019;[Epub] CrossRef - Novel Biomarkers for Prediction of Response to Preoperative Systemic Therapies in Gastric Cancer
Alessandro Cavaliere, Valeria Merz, Simona Casalino, Camilla Zecchetto, Francesca Simionato, Hayley Louise Salt, Serena Contarelli, Raffaela Santoro, Davide Melisi
Journal of Gastric Cancer.2019; 19(4): 375. CrossRef - MICROSATELLITE INSTABILITY AND GASTRIC CARCINOMA. REVIEW OF THELITERATURE
D. L. Rotin, O. V. Paklina, I. O. Tin’kova, D. N. Grekov
Russian Journal of Biotherapy.2019; 18(4): 17. CrossRef - Meta-analysis of microsatellite instability in relation to clinicopathological characteristics and overall survival in gastric cancer
K Polom, L Marano, D Marrelli, R De Luca, G Roviello, V Savelli, P Tan, F Roviello
Journal of British Surgery.2018; 105(3): 159. CrossRef - Gastric poorly cohesive carcinoma: a correlative study of mutational signatures and prognostic significance based on histopathological subtypes
Chae H Kwon, Young K Kim, Sojeong Lee, Ahrong Kim, Hye J Park, Yuri Choi, Yeo J Won, Do Y Park, Gregory Y Lauwers
Histopathology.2018; 72(4): 556. CrossRef - Microsatellite instability in gastric cancer: molecular bases, clinical perspectives, and new treatment approaches
Margherita Ratti, Andrea Lampis, Jens C. Hahne, Rodolfo Passalacqua, Nicola Valeri
Cellular and Molecular Life Sciences.2018; 75(22): 4151. CrossRef - High-throughput Protein and mRNA Expression–based Classification of Gastric Cancers Can Identify Clinically Distinct Subtypes, Concordant With Recent Molecular Classifications
Sangjeong Ahn, So-Jeong Lee, Yonugkeum Kim, Ahrong Kim, Nari Shin, Kyung Un Choi, Chang-Hun Lee, Gi Yeong Huh, Kyong-Mee Kim, Namrata Setia, Gregory Y. Lauwers, Do Youn Park
American Journal of Surgical Pathology.2017; 41(1): 106. CrossRef - Molecular Testing for Gastrointestinal Cancer
Hye Seung Lee, Woo Ho Kim, Yoonjin Kwak, Jiwon Koh, Jeong Mo Bae, Kyoung-Mee Kim, Mee Soo Chang, Hye Seung Han, Joon Mee Kim, Hwal Woong Kim, Hee Kyung Chang, Young Hee Choi, Ji Y. Park, Mi Jin Gu, Min Jin Lhee, Jung Yeon Kim, Hee Sung Kim, Mee-Yon Cho
Journal of Pathology and Translational Medicine.2017; 51(2): 103. CrossRef - Molecular testing of gastrointestinal tumours
Matthew Evans, Matthew Smith, Brendan O'Sullivan, Philippe Taniere
Diagnostic Histopathology.2017; 23(10): 442. CrossRef - Gastric Carcinomas With Lymphoid Stroma
Raul S Gonzalez, Justin M M Cates, Frank Revetta, Loralee A McMahon, Kay Washington
American Journal of Clinical Pathology.2017; 148(6): 477. CrossRef - Meta-Analysis of Prognostic Role of Ki-67 Labeling Index in Gastric Carcinoma
Jung-Soo Pyo, Nae Yu Kim
The International Journal of Biological Markers.2017; 32(4): 447. CrossRef - Tissue-Agnostic Drug Development
Keith T. Flaherty, Dung T. Le, Steven Lemery
American Society of Clinical Oncology Educational Book.2017; (37): 222. CrossRef - Programmed death ligand-1 and MET co-expression is a poor prognostic factor in gastric cancers after resection
Mi Jung Kwon, Kab-Choong Kim, Eun Sook Nam, Seong Jin Cho, Hye-Rim Park, Soo Kee Min, Jinwon Seo, Ji-Young Choe, Hye Kyung Lee, Ho Suk Kang, Kyueng-Whan Min
Oncotarget.2017; 8(47): 82399. CrossRef - Hypermutation and microsatellite instability in gastrointestinal cancers
Kizuki Yuza, Masayuki Nagahashi, Satoshi Watanabe, Kazuaki Takabe, Toshifumi Wakai
Oncotarget.2017; 8(67): 112103. CrossRef - The Emerging Role of Immunotherapy in Gastric and Esophageal Adenocarcinoma
Bruno Bockorny, Eirini Pectasides
Future Oncology.2016; 12(15): 1833. CrossRef - Expression of Mismatch Repair Proteins in Early and Advanced Gastric Cancer in Poland
Katarzyna Karpińska-Kaczmarczyk, Magdalena Lewandowska, Małgorzata Ławniczak, Andrzej Białek, Elżbieta Urasińska
Medical Science Monitor.2016; 22: 2886. CrossRef - Immunotherapy for Gastroesophageal Cancer
Emily Goode, Elizabeth Smyth
Journal of Clinical Medicine.2016; 5(10): 84. CrossRef - Lauren classification and individualized chemotherapy in gastric cancer
JUNLI MA, HONG SHEN, LINDA KAPESA, SHAN ZENG
Oncology Letters.2016; 11(5): 2959. CrossRef - High-risk and low-risk gastric cancer areas in Italy and its association with microsatellite instability
Karol Polom, Daniele Marrelli, Valeria Pascale, Giandomenico Roviello, Costantino Voglino, Henry Rho, Carla Vindigni, Mario Marini, Raffaele Macchiarelli, Franco Roviello
Journal of Cancer Research and Clinical Oncology.2016; 142(8): 1817. CrossRef - MUC2 Expression Is Correlated with Tumor Differentiation and Inhibits Tumor Invasion in Gastric Carcinomas: A Systematic Review and Meta-analysis
Jung-Soo Pyo, Jin Hee Sohn, Guhyun Kang, Dong-Hoon Kim, Kyungeun Kim, In-Gu Do, Dong Hyun Kim
Journal of Pathology and Translational Medicine.2015; 49(3): 249. CrossRef - Correlation between microsatellite instability-high phenotype and occult lymph node metastasis in gastric carcinoma
Jiwoon Choi, Soo Kyung Nam, Do Joong Park, Hwal Woong Kim, Hyung-Ho Kim, Woo Ho Kim, Hye Seung Lee
APMIS.2015; 123(3): 215. CrossRef - Clinicopathologic and molecular features associated with patient age in gastric cancer
Ji Yeon Seo, Eun Hyo Jin, Hyun Jin Jo, Hyuk Yoon, Cheol Min Shin, Young Soo Park, Nayoung Kim, Hyun Chae Jung, Dong Ho Lee
World Journal of Gastroenterology.2015; 21(22): 6905. CrossRef - Molecular classification of gastric cancer: Towards a pathway-driven targeted therapy
Ismael Riquelme, Kathleen Saavedra, Jaime A. Espinoza, Helga Weber, Patricia García, Bruno Nervi, Marcelo Garrido, Alejandro H. Corvalán, Juan Carlos Roa, Carolina Bizama
Oncotarget.2015; 6(28): 24750. CrossRef - A phylogenetic model for understanding the effect of gene duplication on cancer progression
Qin Ma, Jaxk H. Reeves, David A. Liberles, Lili Yu, Zheng Chang, Jing Zhao, Juan Cui, Ying Xu, Liang Liu
Nucleic Acids Research.2014; 42(5): 2870. CrossRef - The analysis of microsatellite instability in extracolonic gastrointestinal malignancy
Andrew S. Williams, Weei-Yuarn Huang
Pathology.2013; 45(6): 540. CrossRef
- DNA Methylation in Gastric Cancer and Preneoplastic Lesions: Emerging Insights and Future Directions
- Prognostic Relevance of the Expression of CA IX, GLUT-1, and VEGF in Ovarian Epithelial Cancers
- Kyungbin Kim, Won Young Park, Jee Yeon Kim, Mee Young Sol, Dong Hun Shin, Do Youn Park, Chang Hun Lee, Jeong Hee Lee, Kyung Un Choi
- Korean J Pathol. 2012;46(6):532-540. Published online December 26, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.6.532
- 11,147 View
- 42 Download
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Tumor hypoxia is associated with malignant progression and treatment resistance. Hypoxia-related factors, such as carbonic anhydrase IX (CA IX), glucose transporter-1 (GLUT-1), and vascular endothelial growth factor (VEGF) permit tumor cell adaptation to hypoxia. We attempted to elucidate the correlation of these markers with variable clinicopathological factors and overall prognosis.
Methods Immunohistochemistry for CA IX, GLUT-1, and VEGF was performed on formalin-fixed, paraffin-embedded tissues from 125 cases of ovarian epithelial cancer (OEC).
Results CA IX expression was significantly associated with an endometrioid and mucinous histology, nuclear grade, tumor necrosis, and mitosis. GLUT-1 expression was associated with tumor necrosis and mitosis. VEGF expression was correlated only with disease recurrence. Expression of each marker was not significant in terms of overall survival in OECs; however, there was a significant correlation between poor overall survival rate and high coexpression of these markers.
Conclusions The present study suggests that it is questionable whether CA IX, GLUT-1, or VEGF can be used alone as independent prognostic factors in OECs. Using at least two markers helps to predict patient outcomes in total OECs. Moreover, the inhibition of two target gene combinations might prove to be a novel anticancer therapy.
-
Citations
Citations to this article as recorded by- Glucose-transporter 1 (GLUT1) as a prognostic biomarker: evidence from 14,966 human tumors across 134 cancer types
Seyma Büyücek, Katharina Möller, Florian Viehweger, Ria Schlichter, Anne Menz, Andreas M Luebke, Viktor Reiswich, Martina Kluth, Claudia Hube-Magg, Andrea Hinsch, Florian Lutz, Sören Weidemann, Frank Jacobsen, Maximilian Lennartz, David Dum, Christian Ber
BMC Cancer.2026;[Epub] CrossRef - Role of Carbonic Anhydrase IX Expression in Triple-negative Breast Cancer
Hemali B Kotadiya, Nupur A Patel, Hemangini H Vora
Gujarat Cancer Society Research Journal.2026; 27(2): 31. CrossRef - Evaluation of the effect of Endogenous and Exogenous Antioxidants on Hypoxia Induced Breast Adenocarcinoma Cell Invasion and Migration:
In vitro
Subarnarekha Maitra, Poulami Sen, Dibya Sinha, Tathagata Roy
Research Journal of Pharmacy and Technology.2025; : 3153. CrossRef - Effect of Ultrasound Therapy at the ST11 on Sympathetic Nervous System Change: A Prospective Randomized Controlled Study
Shinwoo Kang, Dongho Keum
Journal of Korean Medicine Rehabilitation.2023; 33(4): 167. CrossRef - A systematic review verified by bioinformatic analysis based on TCGA reveals week prognosis power of CAIX in renal cancer
Zikuan Zhang, Bo Wu, Yuan Shao, Yongquan Chen, Dongwen Wang, Lucia Magnelli
PLOS ONE.2022; 17(12): e0278556. CrossRef - Effect of Acupuncture at the Field of the Auricular Branch of the Vagus Nerve on Autonomic Nervous System Change
Sunjoo An, Dongho Keum
Journal of Korean Medicine Rehabilitation.2021; 31(2): 81. CrossRef - Responses of Autonomic Nervous System and Gastrointestinal Function to Acupuncture at Abdominal Anterior Cutaneous Nerve : A Pilot Study
Seohyun Park, Hojun Kim, Dongho Keum
Journal of Korean Medicine.2019; 40(1): 99. CrossRef - Omega-3 polyunsaturated fatty acid docosahexaenoic acid and its role in exhaustive-exercise-induced changes in female rat ovulatory cycle
Abeer F. Mostafa, Shereen M. Samir, R.M. Nagib
Canadian Journal of Physiology and Pharmacology.2018; 96(4): 395. CrossRef - Clear cell carcinomas of the ovary and kidney: clarity through genomics
Jennifer X Ji, Yi Kan Wang, Dawn R Cochrane, David G Huntsman
The Journal of Pathology.2018; 244(5): 550. CrossRef - Prognostic Significance of Carbonic Anhydrase IX Expression in Cancer Patients: A Meta-Analysis
Simon J. A. van Kuijk, Ala Yaromina, Ruud Houben, Raymon Niemans, Philippe Lambin, Ludwig J. Dubois
Frontiers in Oncology.2016;[Epub] CrossRef - Review of Research Topics on Abdominal Examination
Jihye Kim, Jeong Hwan Park, Keun Ho Kim
Journal of Korean Medicine.2016; 37(3): 1. CrossRef - Expression of hypoxic markers and their prognostic significance in soft tissue sarcoma
JEUNG IL KIM, KYUNG UN CHOI, IN SOOK LEE, YOUNG JIN CHOI, WON TACK KIM, DONG HOON SHIN, KYUNGBIN KIM, JEONG HEE LEE, JEE YEON KIM, MEE YOUNG SOL
Oncology Letters.2015; 9(4): 1699. CrossRef - Evaluation of a Hypoxia Regulated Gene Panel in Ovarian Cancer
Amanda F. Baker, Scott W. Malm, Ritu Pandey, Cindy Laughren, Haiyan Cui, Denise Roe, Setsuko K. Chambers
Cancer Microenvironment.2015; 8(1): 45. CrossRef - Sulforaphane reduces molecular response to hypoxia in ovarian tumor cells independently of their resistance to chemotherapy
MICHAL PASTOREK, VERONIKA SIMKO, MARTINA TAKACOVA, MONIKA BARATHOVA, MARIA BARTOSOVA, LUBA HUNAKOVA, OLGA SEDLAKOVA, SONA HUDECOVA, OLGA KRIZANOVA, FRANCK DEQUIEDT, SILVIA PASTOREKOVA, JAN SEDLAK
International Journal of Oncology.2015; 47(1): 51. CrossRef - Overexpression of Glucose Transporter-1 (GLUT-1) Predicts Poor Prognosis in Epithelial Ovarian Cancer
Hanbyoul Cho, You Sun Lee, Julie Kim, Joon-Yong Chung, Jae-Hoon Kim
Cancer Investigation.2013; 31(9): 607. CrossRef - Towards Lipidomics of Low-Abundant Species for Exploring Tumor Heterogeneity Guided by High-Resolution Mass Spectrometry Imaging
Jonathan Cimino, David Calligaris, Johann Far, Delphine Debois, Silvia Blacher, Nor Sounni, Agnès Noel, Edwin De Pauw
International Journal of Molecular Sciences.2013; 14(12): 24560. CrossRef
- Glucose-transporter 1 (GLUT1) as a prognostic biomarker: evidence from 14,966 human tumors across 134 cancer types
- Molecular Biological Characteristics of Differentiated Early Gastric Cancer on the Basis of Mucin Expression.
- Nari Shin, Hye Yeon Kim, Woo Kyung Kim, Min Gyung Park, Kyung Bin Kim, Dong Hoon Shin, Kyung Un Choi, Jee Yeon Kim, Chang Hun Lee, Gi Young Huh, Mee Young Sol, Do Youn Park
- Korean J Pathol. 2011;45(1):69-78.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.1.69
- 4,992 View
- 24 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
It is clear that the biologic characteristics of gastric cancer are different on the basis of mucin phenotypes. However, there are unabated controversies on the exact biologic differences of mucin expression in gastric cancer.
METHODS
We analyzed various protein expressions and microsatellite instability (MSI) status based on mucin expression in 130 differentiated early gastric adenocarcinoma cases. Furthermore, we evaluated the genomic alternation in 10 selected differentiated early gastric adenocarcinoma cases using array based comparative genomic hybridization (aCGH).
RESULTS
Intestinal mucin predominant subtype showed significantly elevated p53 protein and caudal-related homeobox 2 expression, and delocalization of beta catenin expressions compared to the gastric mucin predominant subtype. On MSI status, the gastric mucin predominant subtype more frequently showed unstable status than the intestinal mucin predominant subtype. CGH study showed more frequent chromosomal gain and loss in the intestinal mucin predominant subtype than the gastric mucin predominant subtype, albeit without statistical significance. Interestingly, there were significant differences in chromosomal alternation between four mucin phenotypes.
CONCLUSIONS
Study results suggest possible different points of biologic behaviors in early differentiated gastric adenocarcinomas by mucin expression type. -
Citations
Citations to this article as recorded by- Mucin Expression in Gastric Cancer: Reappraisal of Its Clinicopathologic and Prognostic Significance
Dae Hwan Kim, Nari Shin, Gwang Ha Kim, Geum Am Song, Tae-Yong Jeon, Dong-Heon Kim, Gregory Y. Lauwers, Do Youn Park
Archives of Pathology & Laboratory Medicine.2013; 137(8): 1047. CrossRef - Microsatellite Instability Status in Gastric Cancer: A Reappraisal of Its Clinical Significance and Relationship with Mucin Phenotypes
Joo-Yeun Kim, Na Ri Shin, Ahrong Kim, Hyun-Jeong Lee, Won-young Park, Jee-Yeon Kim, Chang-Hun Lee, Gi-Young Huh, Do Youn Park
Korean Journal of Pathology.2013; 47(1): 28. CrossRef
- Mucin Expression in Gastric Cancer: Reappraisal of Its Clinicopathologic and Prognostic Significance
- Expression of p63 and its Isoform, deltaNp63, in Non-Small Cell Lung Carcinoma.
- Ick Doo Kim, Dong Hoon Shin, Kyung Un Choi, Do Youn Park, Gi Yeong Huh, Mee Young Sol, Min Ki Lee, Young Dae Kim, Chang Hun Lee
- Korean J Pathol. 2009;43(4):321-328.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.4.321
- 4,301 View
- 58 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Several studies have been conducted on the role of the p63 gene family in non-small cell lung carcinoma (NSCLC). Nevertheless, the role of these genes in the development and progression of NSCLC remains controversial. This study was designed to examine the expression and clinicopathologic significance of the p63 family in NSCLC.
METHODS
Immunohistochemical staining was performed on 92 cases of NSCLC (47 squamous cell carcinomas [SqCCs] and 45 adenocarcinomas [ACs]) using tissue microarray blocks. The results were analyzed and correlated with clinicopathologic data. RESULTS: The expression of delta Np63 (Delta Np63) was elevated in SqCC (39/47), but not in AC (2/45; p<0.01). Both p63 and Delta Np63 had high expression in 39 SqCCs; p63 and Delta Np63 also had a similar geomorphologic distribution in most positive tumors. The expression of Delta Np63 was correlated with histologic type, gender, pT stage, p53 expression, and p63 expression. pT and pN stages were independent factors in survival (p<0.05, respectively).
CONCLUSIONS
The major p63 isoform in NSCLC, Delta Np63, had a strong correlation with p53 and p63, and was exclusively expressed in SqCC. However, our findings suggest that Delta Np63 was not an independent prognostic factor for NSCLC.
- Primary Extragastrointestinal Stromal Tumor (EGIST) of the Greater Omentum.
- Kyung Un Choi, Jee Yeun Kim, Do Youn Park, Chang Hun Lee, Mee Young Sol, Kang Suek Suh, Jun Woo Lee
- Korean J Pathol. 2001;35(4):347-350.
- 4,071 View
- 34 Download
-
 Abstract
Abstract
 PDF
PDF - Gastrointestinal stromal tumors (GISTs) were recently defined as spindle cell, epithelioid, or occasionally, pleomorphic mesenchymal tumors of the gastrointestinal tract that express the CD117 (proto-oncogene c-kit protein, stem cell factor receptor), as detected using immunohistochemistry. And they show a new tendency to include the CD117-positive mesenchymal spindle cell or epithelioid neoplasms primary in the omentum and mesentery, and is so termed extragastrointestinal stromal tumors (EGISTs). Omental EGISTs are very rare and similar to their gastrointestinal counterpart. We present a case of primary EGIST of the greater omentum in a 58-year-old man. The resected tumor mass measured 20X15X5 cm and weighed 1,150 g. The cut surface displayed a central cystic change and partial mural nodules. Microscopically, most parts of the tumor were composed of round or polygonal cells, with many of them containing perinuclear vacuoles. The mitotic count was less than one per 50 high-power-fields. Immunohistochemically, the tumor cells were diffusely positive for CD117 and vimentin, and focally for smooth muscle actin and CD34. Ultrastructurally, partially smooth muscle differentiation was confirmed in this case.
- Expression of Fas/Fas Ligand and Its Relationship with Apoptosis in Chemically Induced Preneoplastic Lesions in Rat Liver.
- Hye Jin Lee, Do Youn Park, Kyung Un Choi, Jee Yeon Kim, Chang Hun Lee, Mee Young Sol, Kang Suek Suh
- Korean J Pathol. 2001;35(5):383-390.
- 2,196 View
- 15 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Apoptosis of hepatocytes plays a major role in experimental hepatocarcinogenesis of rats. But sequential change and localization of Fas and Fas ligand (FasL) in preneoplastic lesions and the relationship with apoptosis are not clearly elucidated.
METHODS
We investigated sequential change and localization of Fas/FasL and its relationship to apoptosis in preneoplastic lesions of chemical hepatocarcinogenesis in rats using northern blot analysis, immunohistochemistry and terminal deoxynucleotidyl transferase end labeling (TUNEL) assay.
RESULTS
We found that mRNA of Fas and Fas ligand increased for up to 42 days and 14 days after partial hepatectomy, respectively, and thereafter decreased with time. Fas protein was localized on the cytoplasm of hepatocytes of preneoplastic lesions, as well as on the cytoplasmic membrane of the adjacent liver parenchyme. Fas negative preneoplastic lesions were evident at 42 days after partial hepatectomy. FasL protein was found only in the cytoplasm of hepatocytes of preneoplastic lesions, instead of in the adjacent liver parenchyme. FasL-positive hepatocytes increased with time for up to 14 days after partial hepatectomy and therafter decreased. Also, TUNEL-positive apoptotic cells increased with time and were more numerous in the adjacent liver parenchyme than in the preneoplastic lesions.
CONCLUSIONS
It was suggested that Fas/FasL-mediated apoptosis might be one of the major mechanisms for controlling apoptotic cell death in the promotion stage of chemical hepatocarcinogenesis.
- Immunohistochemical Study on the Expression of p53 and Bcl-2 Proteins in Non-Small Cell Lung Carcinomas.
- Ok Ju Lee, Do Youn Park, Kang Suek Suh
- Korean J Pathol. 1997;31(9):823-831.
- 2,084 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - To address the possible prognostic value of p53 and Bcl-2 proteins in non-small cell lung carcinomas (NSCLCs), the authors studied 43 cases of NSCLCs diagnosed between the years 1990 to 1995 at Pusan National University Hospital. The patients were treated either by pneumonectomy or lobectomy of the lung. The expression of p53 and Bcl-2 proteins was semiquantitatively analyzed in paraffin sections by immunohistochemical method and correlated with clinicopathologic prognostic parameters of NSCLCs. Overexpression of the p53 protein was found in 31 cases (72.1%) of the 43 NSCLCs. Overexpression of the p53 protein was significantly correlated with the decreasing degree of histologic differentiation, increasing tumor stage, and cigarette smoking. Bcl-2 expression was found in 19 cases (44.2%) of the 43 NSCLCs. Increased expression of the Bcl-2 protein was significantly correlated only with decreasing tumor stage. An inverse relationship was found between p53 and Bcl-2 proteins, but it was not statistically significant. Thus p53 and Bcl-2 proteins, as demonstrated immunohistochemically in routine paraffin sections, could be of value in prediction of the aggressiveness and prognosis of NSCLCs, in agreement with the central role of p53 and Bcl-2 proteins in the evolution of NSCLCs associated with cigarette smoking.
- Cytologic Features of Fine Needle Aspirates of Hyalinizing Trabecular Adenoma with Occult Papillary Carcinoma of the Thyroid.
- Kyung Un Choi, Jee Yeon Kim, Jin Sook Lee, Do Youn Park, Chang Hoon Lee, Mee Young So, Kang Suek Suh
- J Pathol Transl Med. 2003;14(1):7-11.
- 2,143 View
- 12 Download
-
 Abstract
Abstract
 PDF
PDF - Hyalinizing trabecular adenoma of the thyroid gland is a rare benign neoplasm predominantly diagnosed in middle-aged women. Carney et al. first described this entity that may mimic paraganglioma, medullary carcinoma and papillary carcinoma in 1987. We describe cytologic and histopathologic features of a case of hyalinizing trabecular adenoma combined with occult papillary carcinoma in the opposite lobe. A 55-year-old woman presented with nontender palpable mass of the right neck for 6 months. The aspirate was cellular and contained small clusters and sheets of epithelial cells with abundant filamentous, vacuolated, and ill-defined cytoplasm. The nuclei were slightly pleomorphic and showed nuclear overlapping, nuclear grooves, and intranuclear cytoplasmic inclusions. Histologic examination showed hyalinizing trabecular adenoma in the right lobe and occult papillary carcinoma in the left lobe.
- Cellular Distribution of TGF-beta1 Peptide in Dimethylnitrosamine Induced Fibrosis of Rat Liver.
- Sook Nyo Lee, Do Youn Park, Sun Kyung Lee
- Korean J Pathol. 1997;31(11):1157-1165.
- 2,048 View
- 11 Download
-
 Abstract
Abstract
- Recently attention has been focused on the biology of transforming growth factor-beta1 (TGF-beta1). TGF-beta1, a potent regulator of cell proliferation, stimulates the proliferation of many cell types of mesenchymal origin and inhibits the growth of many epithelial cells. But its cellular distribution and temporal expression remain unknown. The aim of this study was to investigate immunohistochemically the cellular distribution and temporal expression of TGF-beta1 during rat hepatic fibrosis induced by dimethylnitrosamine (DMN). At an early stage of liver fibrosis, there was evidence of multiple centrilobular hemorrhagic necrosis with parenchymal lobular collapse, and at a late stage, there was septal fibrosis with micronodule formation of the parenchyme. TGF-beta1 peptide was first expressed in centrilobular clusters of macrophage which were surrounded by many TGF-beta1 negative fat-storing cells (FSCs). Along with the progression of fibrosis, the TGF-beta1 peptide was expressed in the alpha-smooth muscle actin positive FSCs and also in some peripherally located hepatocytes of micronodules. Serum IFN-gamma was detected in the serum 2 weeks after an initial administration of DMN had reached the peak level at the 4th week and then markedly decreased at the 5th week. We think that TGF-beta1 peptide is produced by macrophages influenced by soluble IFN-gamma, and is expressed in the -smooth muscle actin positive mesenchymal cells and regenerating hepatocytes, and that this cytokine may have an important role in the synthesis of the extracellular matrix and in the regulation of hepatocytic regeneration.
- "Chordoid" Meningioma with Systemic Manifestations of Castleman Syndrome: A case report.
- Hwa Sun Lee, Hweon Ok Kim, Do Youn Park, Mee Yeong Sol, Kang Suek Suh, Sun Kyung Lee
- Korean J Pathol. 1996;30(3):255-260.
- 2,835 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - Chordoid meningioma is a recently established meningeal tumor and is characterized by a chordoma like histologic appearance, peritumoral lymphoplasma cell infiltrates causing systemic manifestations similar to Castleman syndrome and having a good prognosis. We experienced a case of chordoid meningioma in a 25 year-old woman. The patient preoperatively manifested iron-resistant hypochromic microcytic anemia, polyclonal gammopathy with beta-gamma bridging and detected a huge mass in the right temporo-parietal convexity of the brain. Microscopically, the mass was composed of nests and cords of cuboid, partly vacuolated cells in a mucoid matrix, simulating chordoma. The tumor was surrounded by masses of lymphoplasma cells around vessels, many of the plasma cells contained Russell bodies. Ultrastructural findings showed intranuclear cytoplasmic invaginations, microvilli protruding from cytoplasmic surfaces and well formed desmosomes. Some portions of tumor cell surface were covered by stretches of basal lamina.
- Primary MALT(mucosa-associated lymphoid tissue) Type Lymphoma of the Liver.
- Do Youn Park, Jee Yeon Kim, Hyo Jeong Chae, Jin Sook Lee, Chang Hun Lee, Mee Young Sol, Kang Suek Suh, Sun Kyung Lee
- Korean J Pathol. 1997;31(12):1317-1319.
- 2,239 View
- 13 Download
-
 Abstract
Abstract
 PDF
PDF - Primary non-Hodgkin' lymphomas of the liver, an organ normally devoid of a native lymphoid tissue, are very rare. We recently experienced a case of a primary low-grade hepatic B-cell lymphoma of mucosa-associated lymphoid tissue (MALT) type in a 36-year-old woman. The ultrasonography revealed a 5 cm sized mass in the right lobe of the liver. A right segmentectomy of the liver was done and showed a relatively well-circumscribed brownish yellow lobulated homogenous mass, measuring 5.5x4.5 cm in size. Histologic sections of liver mass revealed large lymphoid follicles with reactive germinal centers, follicular colonization by centrocyte-like cells (CCL cells), and lymphoepithelial lesions. The CCL cells were positive for B-cell (CD20), LCA (CD45RA), Bcl-2 oncoprotein, and lambda light chain.
- Altered Expression of DNA Topoisomerase IIalpha, Ki-67, p53 and p27 in Non-Hodgkin's Lymphoma.
- Kyeong Min Lee, Mee Young Sol, Hyun Jeong Kang, Dong Hoon Shin, Kyung Un Choi, Hwal Woong Kim, Jee Yeon Kim, Do Youn Park, Chang Hun Lee
- Korean J Pathol. 2005;39(5):332-337.
- 2,498 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Topoisomerase II (TOPO II) is an enzyme that separates intertwined chromosomes during DNA synthesis by transiently breaking and joining DNA strands. The level of TOP II is one of the determinants of cellular sensitivity to anti-tumor drugs in non-Hodgkin's lymphoma patients. The alpha form of TOPO II has been recently used as a marker of cellular proliferation. High levels of TOPO IIalpha are expressed in aggressive and proliferative tumors.
METHODS
This study was designed to evaluate the relationship between TOPO IIalpha expression and clinicopathological parameters including age, gender, the serum LDH level, the serum beta2-microglobulin level and stage, or expressions, of Ki-67, p53 and p27, in non-Hodgkin's lymphoma. We analyzed forty-one biopsied tissue specimens from patients with non-Hodgkin's lymphoma.
RESULTS
The expression of TOPO IIalpha increased with the clinical stage and it was correlated with Ki-67 and p53 expressions. However, TOPO IIalpha expression did not have any significant correlation with age, gender, the serum LDH level, the serum 2-microglobulin level and the p27 expression.
CONCLUSIONS
TOPO IIalpha expression is a useful marker of cellular proliferation and it may serve as a prognostic factor of a tumor's progression and aggressiveness in non-Hodgkin's lymphomas.
- Cytologic Features of Pseudoangiomatous Stromal Hyperplasia of the Breast: A Case Report with Review of Literature.
- Jin Sook Lee, Jee Yeon Kim, Dong Hoon Shin, Do Youn Park, Kyung Un Choi, Chang Hoon Lee, Mee Young Sol
- J Pathol Transl Med. 2005;16(1):25-30.
- 2,492 View
- 41 Download
-
 Abstract
Abstract
 PDF
PDF - Pseudoangiomatous stromal hyperplasia(PASH) was initially described by Vuitch et al. as a benign breast lesion, consisting of mammary stromal proliferations which simulate vascular lesions, and which might be mistaken for a low-grade angiosarcoma. This condition occasionally presents as a palpable mass in postmenopausal women, but is more frequently encountered as an incidental component in premenopausal women. Clinical, radiological, and fine-needle aspiration(FNA) findings associated with this condition can mimic those observed in conjunction with a phyllodes tumor or a fibroadenoma. The cytological features of PASH are generally nonspecific, and its diagnosis by FNA cytology is fairly difficult. In this study, we report a case of PASH, manifesting as a palpable mass
- Smad4 Expression in Gastric Adenocarcinoma.
- Hyeon Ok Kim, Do Youn Park, Kang Suek Suh
- Korean J Pathol. 2003;37(2):93-99.
- 2,461 View
- 31 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The role of Smad4 in carcinogenesis is important, because of its function as a central mediator of TGF-beta signaling. In the present study we analyzed the expressions of Smad4 mRNA and protein in human gastric cancer cell lines and tissues and we also analyzed their clinicopathological significance.
METHODS
We used semi-quantitative RT-PCR for Smad4 mRNA expression in 13 cases of fresh gastric cancer tissues and two gastric cancer cell lines (MKN-28, SNU-1). We also used immunohistochemistry for Smad4 protein expression in 88 cases of formalin fixed gastric cancers tissues.
RESULTS
The mRNA level of Smad4 was higher in MKN-28 cell line (intestinal type) than in the SNU-1 cell line (diffuse type). Fresh frozen gastric cancer tissues showed that the intestinal type of gastric cancer had higher Smad4 mRNA expressions than the diffuse type of gastric cancer (p<0.05). Immunohistochemical staining for Smad4 revealed that cytoplasmic and nuclear expressions of Smad4 were significantly correlated with histologic types of gastric cancer (p<0.05). That is, the intestinal type of gastric cancer showed more cytoplasmic and nuclear smad4 expressions than did the diffuse type of gastric cancer. Reduced cytoplasmic expressions and positive nuclear expressions of Smad4 were more prominent in the advanced gastric cancer than in the early gastric cancer.
CONCLUSION
Taken together, we suggest that loss of Smad4 expression might be associated with the intestinal type of gastric cancer. Also reduced cytoplasmic Smad4 expressions and increased nuclear Smad4 expressions may be associated with the advanced stage of gastric cancer.
- Expression of TGF-beta1 and TGF-betatype II Receptor in Chemically Induced Hepatocarcinogenesis of the Rat.
- Do Youn Park, Kang Woo Park, Kang Suek Suh
- Korean J Pathol. 2003;37(2):121-128.
- 1,992 View
- 12 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Transforming growth factor (TGF)-beta1 inhibits hepatocyte proliferation by inducing apoptosis. Expression of TGF-beta1 is tightly associated with the TGF-betatype II receptor (TGR2) expression level, and has been regarded as an important change of TGF-beta1 and TGR2 during hepatocarcinogenesis. We investigated the gene expressions and protein localizations of TGF-beta1 and TGR2 in chemical hepatocarcinogenesis.
METHODS
Solt and Farber's method was used as the chemical hepatocarcinogenesis model of the rat. Northern blot analyses and immunohistochemistry for TGF-beta1 and TGR2 were performed to investigate the gene expressions and protein localizations, respectively.
RESULTS
The Northern blot analyses showed a slight increase of TGF-beta1 transcripts one month after partial hepatectomy, which is more than in sham operated control liver, and a decrease of transcripts for TGR2 two months after partial hepatectomy. The number of TGF-beta-positive preneoplastic hepatocytes was increased and correlated with the increase of the number of TGR2 negative hepatocytes or reduction of expressions of TGR2 in preneoplastic lesions. HCC tissues showed an increase of TGF-beta1 protein expressions and a decrease of TGR2 compared to the adjacent liver parenchyme.
CONCLUSION
Our data suggest that down regulation of TGR2 in preneoplastic lesions and HCC might contribute to the resistance to the growth inhibitory effects of TGF-beta.
- Experimental Liver Disease Models of Rats: Morphological Characteristics.
- Do Youn Park, Kang Suek Suh
- Korean J Pathol. 2003;37(3):151-158.
- 2,071 View
- 24 Download
-
 Abstract
Abstract
 PDF
PDF - Experimental liver disease models of rats have many similarities with those of humans, especially in morphological characteristics. Rat liver disease models can be categorized as models of hepatic fibrosis, hepatic stem cell and hepatocarcinogenesis. The purpose of this article is to review experimental liver disease models, with a major emphasis on morphologic features, including routine morphological, immunohistochemical, and electron microscopic features.
- Overexpression of Insulin-like Growth Factor Binding Protein 3 in Colorectal Carcinoma Identified by cDNA Microarray and Immunohistochemical Analysis.
- Kyung Un Choi, Do Youn Park, Jee Yeon Kim, Jin Sook Lee, Mee Young Sol
- Korean J Pathol. 2003;37(3):166-173.
- 1,972 View
- 12 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Insulin-like growth factor binding protein 3 (IGFBP3), a member of six proteins with a high affinity for insulin-like growth factors (IGFs), seems to modulate the effects of IGFs on cells and to regulate cell proliferation through the IGF-independent pathway. We assessed the role of IGFBP3 in the colorectal carcinoma detected by cDNA microarray.
METHODS
To identify molecular alterations in the colorectal carcinoma, we analyzed gene expression profiles of the colorectal adenocarcinoma by means of a cDNA microarray representing 7,500 genes. Of the differentially expressed genes, the author assessed the insulin-like growth factor binding protein 3 (IGFBP3) gene at the protein level using immunohistochemistry.
RESULTS
The expressions of 21 and 16 genes were noted to have more than fivefold increases or decreases in the colonic adenocarcinoma tissue compared with the noncancerous colonic mucosal tissue. The differentially expressed genes include those associated with cell proliferation/apoptosis, signal transduction/transcription, metabolizing enzymes, cytoskeleton, angiogenesis, ion channel, extracellular matrix and others. Of the total 68 cases of colorectal adenocarcinomas observed, 34 cases (50%) showed positive immunohistochemical stainings for IGFBP3.
CONCLUSIONS
In this study, it is suggested that IGFBP3 plays a role in colorectal carcinogenesis. And combining an immunohistochemistry with a cDNA microarray can facillitate the rapid characterization of a candidate novel molecular target.
- Epstein-Barr Viral RNA(EBERs) Expression in Conventional Malignant Lymphoma and Polymorphic Reticulosis of Upper Aerodigestive Tract.
- Do Youn Park, Kang Suek Suh, Sun Kyung Lee
- Korean J Pathol. 1996;30(10):893-902.
- 2,076 View
- 12 Download
-
 Abstract
Abstract
 PDF
PDF - The author examined the immunophenotype and expression of Epstem-Barr virus RNA (EBERs) used in the situ hybridization technique in 20 cases of conventional malignant lymphoma and 28 cases of polymorphic reticulosis and malignant lymphoma with features of polymorphic reticulosis occured in the upper aerodigestive tract including the upper digestive tract(palatine tonsil), and upper respiratory tract(nasal cavity, paranasal sinus, nasopharynx). The results obtained were summarized as followings; 1. The favorable site of malignant lymphoma that occured in the upper aerodigestive tract was in the palatine tonsil(11 out of 20 cases, 55%), those of polymorphic reticulosis and malignant lymphoma with features of polymorphic reticulosis were nasal cavity and nasopharynx(19 out of 28 cases, 78%). 2. The immunophentype of malignant lymphoma that occured in the upper aerodigestive tract was mostly B-cell phenotype (15 out of 20 cases, 75%), and that of polymorphic reticulosis and malignant lymphoma with features of polymorphic reticulosis was predominantly T-cell phenotype(22 out of 28 cases, 79%). 3. The EBERs positivity of malignant lymphoma that occured in the upper aerodigestive tract was 25%(5 out of 20 cases), but that of polymorphic reticulosis and malignant lymphoma with features of polymorphic reticulosis was 57%(16 out of 28 cases). 4. The positive cases for EBERs revealed angiocentricity with necrosis(16 out of 21 cases, 76%), predominantly T-cell phenotype(19 out of 21 cases, 90%), and favorably involved the nasal cavity and nasopharynx(16 out of 21 cases, 76%). Based on the above results, it was concluded that polymorphic reticulosis and malignant lymphoma with features of polymorphic reticulosis that occurred in the upper respiratory tract was an EBV-positive angiocentric T-cell lymphoma favorably involving the nasal cavity and nasopharynx.
- Assessment of Apoptosis by M30 Immunoreactivity and the Relationship with the MSI status and the Clinicopathological Characteristics of Colorectal Carcinomas.
- Hyun Jeong Kang, Mee Young Sol, Do Youn Park, Soo Han Lee, Dong Hun Shin, Jee Yeon Kim, Kyung Un Choi, Hwal Woong Kim, Chang Hun Lee, Gi Young Huh
- Korean J Pathol. 2006;40(5):319-325.
- 2,398 View
- 22 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The monoclonal antibody M30 recognizes a neoepitope of cytokeratin 18 that's produced during the process of apoptosis, and it is reactive in formalin-fixed, paraffin-embedded tissue. The detailed nature of apoptosis in colorectal cancer is unclear, especially in regard to the MSI status and the clinicopathologic factors. The purpose of this study was to elucidate the apoptosis assessed by M30 immunoreactivity in colorectal cancer and its relationship with the MSI status and the various clinicopathologic factors of colorectal cancers.
METHODS
101 colorectal cancers were classified according to levels of MSI as 12 MSI-H, 4 MSI-L and 85 MSS. Apoptosis was quantified by immunohistochemistry with using M30 CytoDEATH anti-body.
RESULTS
The apoptotic index assessed by M30 was significantly increased in the MSI-H and MSI-L colorectal cancer compared to that in the MSS colorectal cancer. Right sided colon cancer showed a significant higher apoptotic index than did the left sided colon cancer. There was also a tendency for decreased apoptosis in metastatic colorectal cancers (Duke's stage D). There was somewhat of an increase of apoptosis in colorectal cancers with mucinous carcinoma and medullary carcinoma, and also in the colorectal cancers with an increased TIL count, but this was not statistically significant.
CONCLUSION
M30 immunoreactivity is a valuable method to detect apoptosis in formalin-fixed, paraffin-embedded tissue and it might explain that MSI-H colorectal cancer shows better clinical behavior than MSS colorectal cancer in regard to the increased apoptosis.
- Analysis of Gene Expression in Renal Cell Carcinomas Using cDNA Microarray: Reduced Expression of Decorin in Renal Cell Carcinomas.
- Jin Sook Lee, Kang Suek Suh, Kyung Un Choi, Jee Yeun Kim, Do Youn Park
- Korean J Pathol. 2003;37(4):232-238.
- 2,002 View
- 14 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Identification of the genes expressed differentially in renal cell carcinoma (RCC)but not in the non-cancerous kidney is important for understanding the molecular basis ofrenal cell carcinoma and for defining possible prognostic value and therapeutic intervention.We investigated the changes in gene expression accompanying the development and progression of kidney cancer by cDNA microarrays.
METHODS
To identify molecular alterations in renal cell carcinoma, we measured expression profiles for paired neoplastic and noncancerouskidney samples from an individual by means of a cDNA microarry representing 7, 500genes. Of the differentially expressed genes, we assessed the decorin gene at the proteinlevel using immunohistochemistry.
RESULTS
The 60 genes were noted to have more than a fivefold change in expression (either increased or decreased) in RCC compared to the noncancerouskidney. The changed genes are those associated with signal transduction, metabolizingenzymes, the cytoskeleton, cell adhesion, cell cycle control, modulation of transcription, the tumor suppressor gene and tumor antigens. Under immunohistochemistry, the expressionof decorin was significantly decreased in the tumor than in the non-cancerous kidney.The expression rate of decorin was not associated with the patient's sex, age, histologic type, Fuhrmann nuclear grade and T stage.
CONCLUSION
The author predicted that these geneexpression profiling experiments will lead to improvements in the basic understanding of renaltumor pathogenesis and will promote the discovery of novel molecular markers for renal tumordiagnosis and therapy.
- Recurred Angiomyofibroblastoma of the Vulva: Report of a case.
- Do Youn Park, Ji Yeon Kim, OK Hyeon Kim, Hwa Sun Lee, Mee Young Sol, Kang Suek Suh, Sun Kyung Lee
- Korean J Pathol. 1996;30(10):947-950.
- 2,431 View
- 30 Download
-
 Abstract
Abstract
 PDF
PDF - Angiomyofibroblastoma is a rare, benign mesenchymal tumor of the vulva. Since it was described in 1992 by Fletcher, 15 cases have been reported in literature. We recently experienced a recurred angiomyofibroblastoma of the vulva. A 45-year-old woman was presented initially in 1991 with a mass of labium major and local excision of tumor mass had been performed. A histologic diagnosis was made of angiomyxoma, but this diagnosis was revised to angiomyofibroblastoma by the authors. The recurred mass was well circumscribed, measuring 2.5x1.6x1.5cm in dimensions. Microscopically the tumor was characterized by high cellularity, numerous blood vessels(which lack prominent hyalinization), and plump stromal cells. Immunohistochemically, the stromal cells were reactive for vimentin and desmin, but not alpha-smooth muscle actin, or S-100 protein. We thought that this case was a recurred angiomyofibrblastoma of the vulva due to incomplete surgical excision.

 E-submission
E-submission


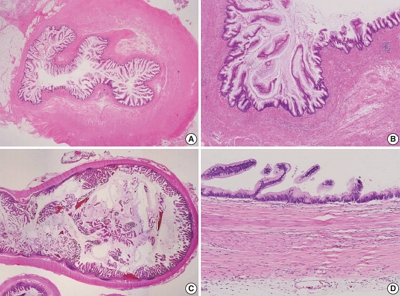
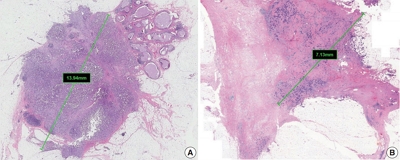
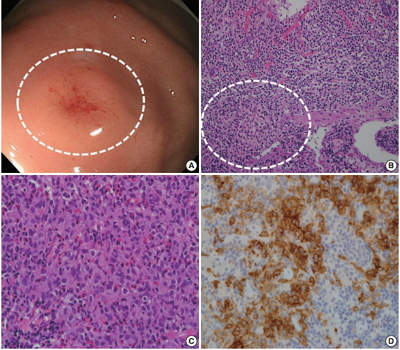
 First
First Prev
Prev



