Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 48(3); 2014 > Article
-
Case Study
Well-Differentiated Papillary Mesothelioma of the Tunica Vaginalis: A Case Study and Review of the Literature - Seyda Erdogan, Arbil Acikalin, Handan Zeren1, Gulfılız Gonlusen, Suzan Zorludemir, Volkan Izol2
-
Korean Journal of Pathology 2014;48(3):225-228.
DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.3.225
Published online: June 26, 2014
Department of Pathology, School of Medicine, Cukurova University, Adana, Turkey.
1Department of Pathology, School of Medicine, Acibadem University, Adana, Turkey.
2Department of Urology, School of Medicine, Cukurova University, Adana, Turkey.
- Corresponding Author: Seyda Erdogan, M.D. Department of Pathology, School of Medicine, Cukurova University, 01330 Adana, Turkey. Tel: +90-322-3386060 (ext. 3158), Fax: +90-322-3386956, seydaer@cu.edu.tr
• Received: May 7, 2012 • Revised: June 21, 2012 • Accepted: July 23, 2012
© 2014 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
- Well-differentiated papillary mesothelioma is an uncommon tumor of the testes that usually presents as a hydrocele. Here, we present the case of one patient who did not have a history of asbestos exposure. The tumor was localized in the tunica vaginalis and was composed of three pedunculated masses macroscopically. Microscopically, branching papillary structures with focal coagulative necrosis were present. In addition to immunohistochemistry, simian virus 40 DNA was also tested by polymerase chain reaction. This report presents one case of this rare entity, its clinical and macroscopic features, and follow-up results.
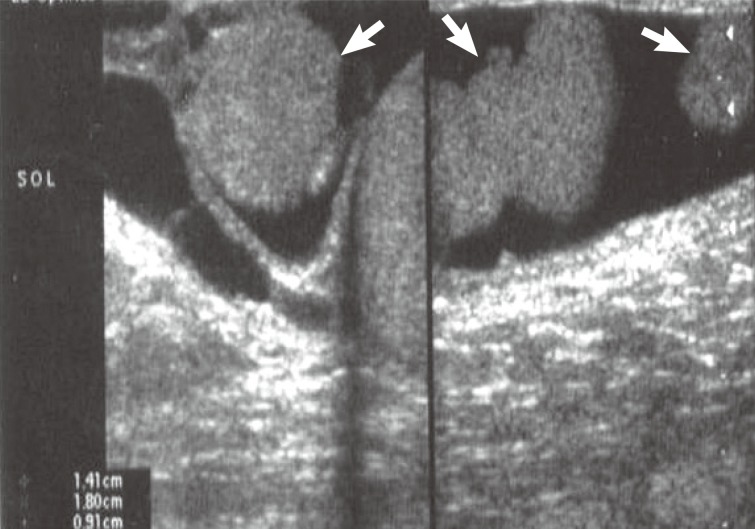
- A 48-year-old man presented with a complaint of scrotal pain and swelling that had been gradually increasing for a period of 6 months. Physical examination revealed an enlarged left hemiscrotum. Testicular ultrasonography showed a left hydrocele consisted of three nodules measuring 2 cm, 1.4 cm, and 0.9 cm (Fig. 1) in the scrotal wall. Magnetic resonance imaging findings also revealed solid intrascrotal, extratesticular lesions. The patient had no history of trauma or asbestos exposure. A left radical orchiectomy was performed. The patient has done well with no signs of residual disease 3 years after surgery.
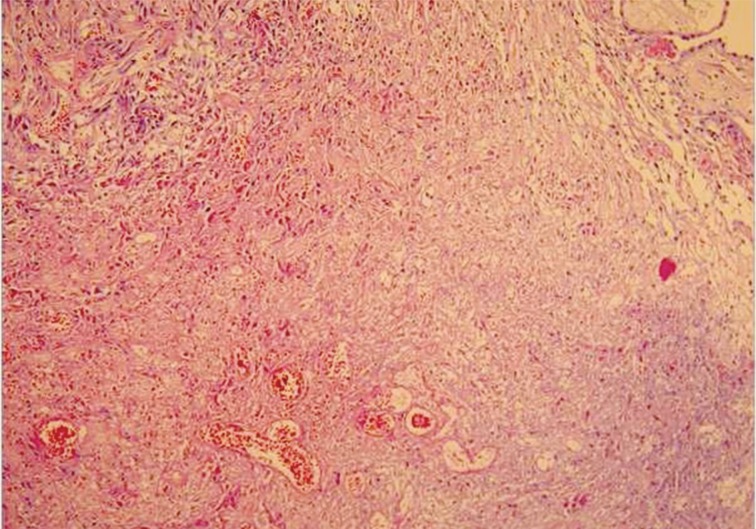
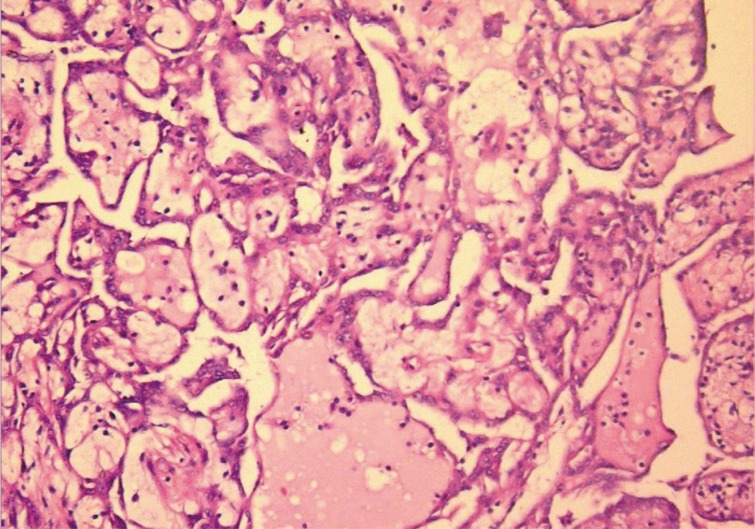
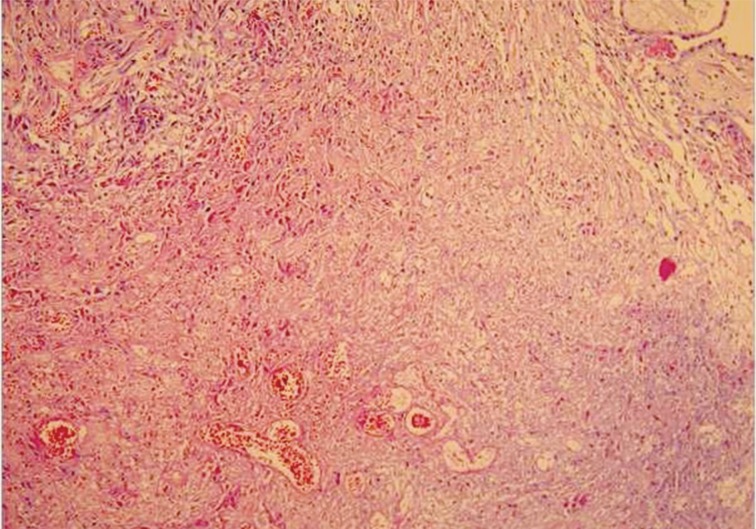
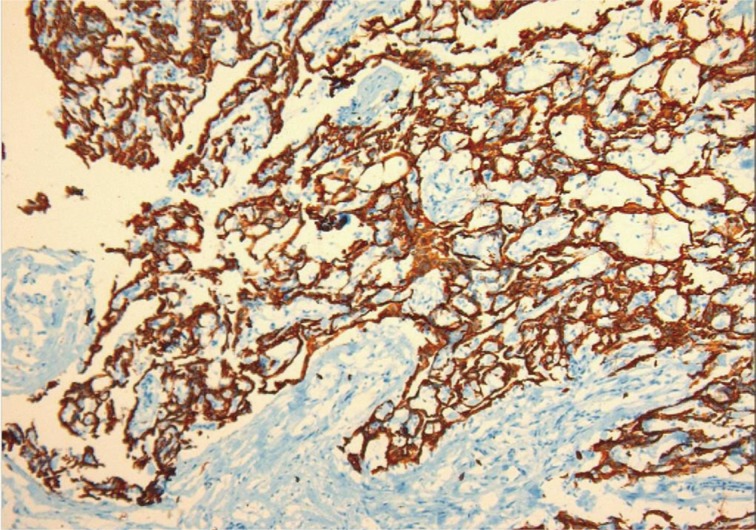
- Macroscopically, the tunica vaginalis had three nodules. These were found to be pedunculated masses with 2 cm, 1.5 cm, and 1 cm in diameter. The testis was normal. Microscopically, the masses were composed of multiple branching, papillary structures with a fibrovascular core (Fig. 2). The papillary structures were lined with a single layer of bland cuboidal cells. The stroma was edematous and myxoid (Fig. 3). Focal areas showed a complex architectural pattern without subepithelial invasion. Focal coagulative necrosis was also seen (Fig. 4). There was no cytologic atypia or atypical mitosis. Immunohistochemical studies were performed. The lining cells were positive for calretinin (Fig. 5), epithelial membrane antigen, HBME-1, and cytokeratin 7. Negative results were found with carcinoembryonic antigen (CEA), cancer antigen 125, and CD10. Additionally, we searched for simian virus 40 (SV40) by polymerase chain reaction (PCR) amplification. DNA was tested using primers specific for the β-globulin gene. Two sets of primers (5'-GAA-TGG-GAG-CAG-TGG-TGG-AAT-GC-3' and 5'-TCT-CTT-CTT-TTT-TGG-AGG-AGT-AGA-3') were used for SV40 detection.12 No SV40 was detected in this case.
CASE REPORT
- Mesotheliomas can arise from the pleura, peritoneum, or paratesticular areas, in decreasing order of frequency. Paratesticular mesothelioma can arise from the tunica vaginalis, formed by an outpouching of the abdominal peritoneum. Only 0.3-5% of cases of mesothelioma occur in the tunica vaginalis. Mesothelial lesions of this area include reactive mesothelial hyperplasia, mesothelial cysts, adenomatoid tumor, WDPM, and MM. WDPM is a rare type of mesothelioma that mostly arises from the peritoneum or pleura.13,14 Barbera and Rubino9 reported the first case of WDPM in 1957. To the best of our knowledge only 18 cases of paratesticular WDPM have been published to date in the English literature. These cases are summarized in Table 1. The majority of these cases have been presented as case reports, except for one series of 8 cases that was published by Brimo et al.8 recently. All reported cases had similar morphology with papillary/tubulopapillary architecture. All cases also had bland appearing cells which lack significant atypia, pleomorphism, and stromal invasion. Only Trpkov et al.6 mentioned a small focus of coagulative necrosis. A minority of cases showed psammoma bodies. One of the cases in the series by Brimo et al.8 showed osteoclast-like giant cells.
- The main differential diagnosis includes mesothelial hyperplasia and MM. Mesothelial hyperplasia can also be composed of papillary structures, but often do not contain a fibrovascular core like WDPM. The papillary structures are often accompanied by inflammation and reactive changes. One major clinical concern is differentiating WDPM from MM, as they can have overlapping histologic features. The presence of invasion, marked cytologic atypia, atypical mitosis, and a bulky mass are the major features that should be considered in making a diagnosis.15,16
- The etiology of WDPM has not been clearly elucidated. It has been suggested that proliferative lesions might be related to local trauma, herniorrhaphy, or a long-term hydrocele.17 A relationship between asbestos exposure and mesotheliomas of the tunica has been postulated. Only one case of WDPM of the tunica vaginalis in the literature had a history of asbestos exposure7 and one had a history of a household contact with exposure.4 Our case had no asbestos exposure like the rest majority of reported cases. In addition to asbestos, potassium bromate in drinking water has been shown to increase the risk of MM of the tunica vaginalis in an animal model.15 SV40 is a DNA monkey virus that has been associated with MM and has been implicated in mesotheliomas of the pleura. SV40 contaminated polio vaccines produced between 1955 and 1978 are postulated to have been the route of virus transmission from monkeys to humans. Many studies have demonstrated the presence of SV40 in pleural mesotheliomas through the use of various techniques, and animal studies have demonstrated a clear association of up to 60% of developing mesothelioma.15,16,18 However SV40 DNA has not been as well studied in mesotheliomas of the tunica vaginalis as it has been in its pleural counterpart. Xiao et al.1 applied PCR for SV40 DNA in their WDPM case and found it to be negative. We also performed PCR, but did not find SV40 in our case. In taking into consideration all reported cases, hydrocele seems to be the major risk factor for developing WDPM of the tunica vaginalis.
- Non-mesothelial tumors of diverse histology must also be kept in mind in the differential diagnosis. This group includes papillary cystadenoma of the epididymis. Features that distinguish papillary mesothelioma from papillary cystadenoma include the absence of clear cells and the presence of calretinin positivity. Papillary serous neoplasms may also be difficult to differentiate from WDPM. However, serous tumors tend to have broader papillae and stratification, budding, and occasional cilia of tumor cells. Psammoma bodies are more numerous than WDPM. Additionally, papillary serous tumors express CEA and Ber-Ep4, both of which are usually negative in WDPM.19,20
- The current case had a focal area of consisting of only superficial, entrapped tubules in the underlying tissue. Given that the stroma exhibited no evidence of hypercellularity, storiform growth or desmoplastic response, we did not consider the tumor to be invasive. Another challenging issue was focal necrosis. Only one previous report mentioned a small focus of coagulative necrosis.6 This area was considered coagulative necrosis in the current case due to torsion or infarct, as mentioned in the previous report. Currently, the main limitation in differentiating WDPM from MM with dominant papillary growth is limited experience, with only 18 known cases in the literature. Although our case had no invasion, cytologic atypia, infiltrative growth, or mitotic activity we recommended close patient follow-up because of the areas of focal necrosis and complexity. This patient has had 4 years of uneventful follow-up. The biologic behavior of paratesticular WDPM is not well-known because of such a limited number of cases. A large series is needed to answer the questions about this enigmatic tumor.
DISCUSSION
- 1. Xiao SY, Rizzo P, Carbone M. Benign papillary mesothelioma of the tunica vaginalis testis. Arch Pathol Lab Med 2000; 124: 143-147. ArticlePubMedPDF
- 2. Tolhurst SR, Lotan T, Rapp DE, et al. Well-differentiated papillary mesothelioma occurring in the tunica vaginalis of the testis with contralateral atypical mesothelial hyperplasia. Urol Oncol 2006; 24: 36-39. ArticlePubMed
- 3. Chetty R. Well differentiated (benign) papillary mesothelioma of the tunica vaginalis. J Clin Pathol 1992; 45: 1029-1030. ArticlePubMedPMC
- 4. Cabay RJ, Siddiqui NH, Alam S. Paratesticular papillary mesothelioma: a case with borderline features. Arch Pathol Lab Med 2006; 130: 90-92. ArticlePubMedPDF
- 5. Fukunaga M. Well-differentiated papillary mesothelioma of the tunica vaginalis: a case report with aspirate cytologic, immunohistochemical, and ultrastructural studies. Pathol Res Pract 2010; 206: 105-109. ArticlePubMed
- 6. Trpkov K, Barr R, Kulaga A, Yilmaz A. Mesothelioma of tunica vaginalis of "uncertain malignant potential": an evolving concept: case report and review of the literature. Diagn Pathol 2011; 6: 78.ArticlePubMedPMCPDF
- 7. Butnor KJ, Sporn TA, Hammar SP, Roggli VL. Well-differentiated papillary mesothelioma. Am J Surg Pathol 2001; 25: 1304-1309. ArticlePubMed
- 8. Brimo F, Illei PB, Epstein JI. Mesothelioma of the tunica vaginalis: a series of eight cases with uncertain malignant potential. Mod Pathol 2010; 23: 1165-1172. ArticlePubMedPDF
- 9. Barbera V, Rubino M. Papillary mesothelioma of the tunica vaginalis. Cancer 1957; 10: 183-189. ArticlePubMed
- 10. Chollet Y, Hauser P, Da Silva T, et al. Well-differentiated papillary mesothelioma of the tunica vaginalis testis: imaging on Tc-99m heat-denatured red blood cell scintigraphy. Clin Nucl Med 2008; 33: 282-284. PubMed
- 11. Fujii Y, Masuda M, Hirokawa M, Matsushita K, Asakura S. A case of benign mesothelioma of the tunica vaginalis testis. Hinyokika Kiyo 1993; 39: 89-92. PubMed
- 12. Carbone M, Pass HI, Rizzo P, et al. Simian virus 40-like DNA sequences in human pleural mesothelioma. Oncogene 1994; 9: 1781-1790. PubMed
- 13. Plas E, Riedl CR, Pflüger H. Malignant mesothelioma of the tunica vaginalis testis: review of the literature and assessment of prognostic parameters. Cancer 1998; 83: 2437-2446. ArticlePubMed
- 14. Churg A. Paratesticular mesothelial proliferations. Semin Diagn Pathol 2003; 20: 272-278. ArticlePubMed
- 15. Chen JL, Hsu YH. Malignant mesothelioma of the tunica vaginalis testis: a case report and literature review. Kaohsiung J Med Sci 2009; 25: 77-81. ArticlePubMed
- 16. Goel A, Agrawal A, Gupta R, Hari S, Dey AB. Malignant mesothelioma of the tunica vaginalis of the testis without exposure to asbestos. Cases J 2008; 1: 310.ArticlePubMedPMCPDF
- 17. Perez-Ordonez B, Srigley JR. Mesothelial lesions of the paratesticular region. Semin Diagn Pathol 2000; 17: 294-306. PubMed
- 18. Winstanley AM, Landon G, Berney D, Minhas S, Fisher C, Parkinson MC. The immunohistochemical profile of malignant mesotheliomas of the tunica vaginalis: a study of 20 cases. Am J Surg Pathol 2006; 30: 1-6. PubMed
- 19. Odrzywolski KJ, Mukhopadhyay S. Papillary cystadenoma of the epididymis. Arch Pathol Lab Med 2010; 134: 630-633. ArticlePubMedPDF
- 20. van der Putte SC, Toonstra J, Sie-Go DM. Mullerian serous cystadenoma of the scrotum following orchiopexy. Adv Urol 2009; 610453.PubMedPMCPDF
REFERENCES
Fig. 1Ultrasonography shows three hypoechoic nodules measuring 2 cm, 1.4 cm, and 0.9 cm in the wall of hydrocele sac (arrows).
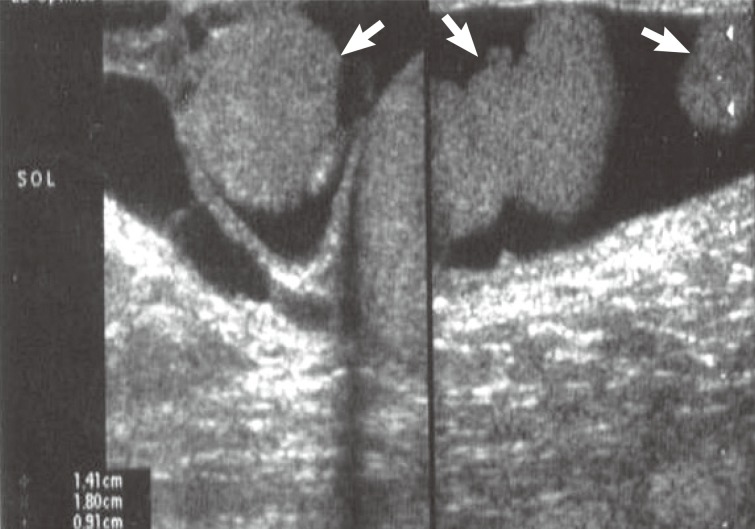

Fig. 2Tumor mass in the tunica vaginalis is composed of multiple branching, papillary structures with a fibrovascular core.


Table 1.The review of paratesticular WDPM cases in the literature
| Author | Age (yr) | Presentation | Location | Focality | Size | Follow-up | Asbestosis | SV40 |
|---|---|---|---|---|---|---|---|---|
| Chetty [3] | 18 | Hydrocele | NA | Multifocal | 1 cm | 1 yr | - | NA |
| Fujii et al. [11] | 56 | Hydrocele | Left | Solitary | 15 mm | 10 yr | - | NA |
| Xiao et al. [1] | 69 | Hydrocele | Right | Solitary | 1.5 cm | 3 yr | - | - |
| Butnor et al. [7] | 32 | Hydrocele | NA | NA | NA | 2 yr | Family contact | NA |
| Tolhurst et al. [2] | 35 | Hydrocele | Right | Multifocal | 9 mm | NA | NA | NA |
| Cabay et al. [4] | 52 | Hydrocele | Right | Solitary | 2 cm | 3 mo | + | NA |
| Fukunaga [5] | 70 | Hydrocele | Right | Solitary | 1.2 cm | 18 mo | - | NA |
| Chollet et al. [10] | 18 | Hydrocele | Left | Solitary | NA | 18 mo | NA | NA |
| Brimo et al. [8] (8 cases) | 52.5 (mean) | 7/8 hydrocele | NA | 6/8 solitary | Mean 1 cm | 3 yr | NA | NA |
| 1/8 mass | 1/8 multifocal | 3 yr | ||||||
| 1/8 plaque | 1.5 yr | |||||||
| 1.5 yr | ||||||||
| 2 mo | ||||||||
| Trpkov et al. [6] | 57 | Hydrocele | NA | Multifocal | 1.5 cm | 6 yr | _ | NA |
| Present case | 48 | Hydrocele | Left | Multifocal | 2 cm | 3 yr | - | - |
Figure & Data
References
Citations
Citations to this article as recorded by 

- Testicular/paratesticular mesothelial tumours: Uncommon histopathologic entities in a very complex anatomical site
Francesca Pagliuca, Stefano Lucà, Marco De Sio, Davide Arcaniolo, Gaetano Facchini, Marco De Martino, Francesco Esposito, Ferdinando DE Vita, Paolo Chieffi, Renato Franco
Pathology - Research and Practice.2024; 253: 155069. CrossRef - Well-differentiated Papillary Mesothelial Tumour of the Tunica Vaginalis Testis – A Rare Lesion, but one Pathologists Should Know About Two Patient Reports and a Review of the Literature
Johannes Kläger, Felicitas Oberndorfer, Cristophe Brunel, Julian Veser, Eva Compérat
International Journal of Surgical Pathology.2023; 31(6): 1126. CrossRef - A diagnostic approach to paratesticular lesions with tubulopapillary architecture: a series of 16 serous borderline tumors/low-grade serous carcinoma and 14 well-differentiated papillary mesothelial tumors and mesothelioma
Rabia Zafar, Lacey J. Schrader, John C. Cheville, J. Kenneth Schoolmeester, Anja C. Roden, Marie-Christine Aubry, Eunhee S. Yi, Aditya Raghunathan, Loren Herrera-Hernandez, R. Houston Thompson, Stephen A. Boorjian, Bradley C. Leibovich, Gary L. Keeney, Ra
Human Pathology.2022; 128: 31. CrossRef - Mesothelioma subtypes of the tunica vaginalis: a rare case report and review of histological criteria
Cutts Rebecca, Martin J Connor, Luxi Sun, Thomas Johnston, Rachel Gooch, John McLoughlin
Journal of Surgical Case Reports.2019;[Epub] CrossRef - Well‐differentiated papillary mesothelioma of tunica vaginalis testis of unknown malignant potential: Sonographic appearance
K.W.S. Ko, K.S. Tse, K.W. Shek, M.N. Hau, S.H. Ting
Journal of Clinical Ultrasound.2018; 46(5): 364. CrossRef - Tunica Vaginalis Thickening, Hemorrhagic Infiltration and Inflammatory Changes in 8 Children with Primary Hydrocele; Reactive Mesothelial Hyperplasia? A Prospective Clinical Study
Ioannis Patoulias, Evangelia Rachmani, Maria Kalogirou, Kyriakos Chatzopoulos, Dimitrios Patoulias
Acta Medica (Hradec Kralove, Czech Republic).2018; 61(2): 41. CrossRef - A 45-year-old man presenting with chest pain
Sheetu Singh, Arpita Jindal
Lung India.2018; 35(2): 171. CrossRef - Two Case Reports of Benign Testicular Mesothelioma and Review of the Literature
Cristobal Ramirez Sevilla, Carme Admella Salvador, Josep Feliu Canaleta, Juan Llopis Manzanera, Miguel Angel Barranco Sanz, Juan Antoni Romero Martin, Sergi Bernal Salguero
Case Reports in Oncological Medicine.2017; 2017: 1. CrossRef - Well-differentiated Papillary Mesothelioma of the Tunica Vaginalis
Wei Keith Tan, Mae-Yen Tan, Hui Meng Tan, Rajadurai Pathmanathan, Wei Phin Tan
Urology.2016; 90: e7. CrossRef - Well-Differentiated Papillary Mesothelioma of the Tunica Vaginalis: Case Report and Systematic Review of Literature
Wei Keith Tan, Mae-Yen Tan, Wei Shen Tan, Soon Ching Gan, Rajadurai Pathmanathan, Hui Meng Tan, Wei Phin Tan
Clinical Genitourinary Cancer.2016; 14(4): e435. CrossRef - The legacy of the F344 rat as a cancer bioassay model (a retrospective summary of three common F344 rat neoplasms)
Robert R. Maronpot, Abraham Nyska, Jennifer E. Foreman, Yuval Ramot
Critical Reviews in Toxicology.2016; 46(8): 641. CrossRef - Malignant Mesothelioma of the Tunica Vaginalis: A Rare Neoplasm—Case Report and Literature Review
Manuel Segura-González, Jorge Urias-Rocha, Jorge Castelán-Pedraza
Clinical Genitourinary Cancer.2015; 13(6): e401. CrossRef - In vivo Optical Coherence Tomography Imaging of the Mesothelium Using Developed Window Models
Yeh-Chan Ahn, Yu-Gyeong Chae, Sang Seok Hwang, Bong-Kwon Chun, Maan Hong Jung, Sung Jin Nam, Hae-Young Lee, Jae Min Chung, Chulho Oak, Eun-Kee Park
Journal of the Optical Society of Korea.2015; 19(1): 69. CrossRef
Well-Differentiated Papillary Mesothelioma of the Tunica Vaginalis: A Case Study and Review of the Literature





Fig. 1 Ultrasonography shows three hypoechoic nodules measuring 2 cm, 1.4 cm, and 0.9 cm in the wall of hydrocele sac (arrows).
Fig. 2 Tumor mass in the tunica vaginalis is composed of multiple branching, papillary structures with a fibrovascular core.
Fig. 3 Papillary structures are lined by bland-looking cuboidal epithelium.
Fig. 4 A focal area of coagulative necrosis is present in the tumor.
Fig. 5 Mesothelial cells show diffuse calretinin positivity in the tumor.
Fig. 1
Fig. 2
Fig. 3
Fig. 4
Fig. 5
Well-Differentiated Papillary Mesothelioma of the Tunica Vaginalis: A Case Study and Review of the Literature
| Author | Age (yr) | Presentation | Location | Focality | Size | Follow-up | Asbestosis | SV40 |
|---|---|---|---|---|---|---|---|---|
| Chetty [3] | 18 | Hydrocele | NA | Multifocal | 1 cm | 1 yr | - | NA |
| Fujii et al. [11] | 56 | Hydrocele | Left | Solitary | 15 mm | 10 yr | - | NA |
| Xiao et al. [1] | 69 | Hydrocele | Right | Solitary | 1.5 cm | 3 yr | - | - |
| Butnor et al. [7] | 32 | Hydrocele | NA | NA | NA | 2 yr | Family contact | NA |
| Tolhurst et al. [2] | 35 | Hydrocele | Right | Multifocal | 9 mm | NA | NA | NA |
| Cabay et al. [4] | 52 | Hydrocele | Right | Solitary | 2 cm | 3 mo | + | NA |
| Fukunaga [5] | 70 | Hydrocele | Right | Solitary | 1.2 cm | 18 mo | - | NA |
| Chollet et al. [10] | 18 | Hydrocele | Left | Solitary | NA | 18 mo | NA | NA |
| Brimo et al. [8] (8 cases) | 52.5 (mean) | 7/8 hydrocele | NA | 6/8 solitary | Mean 1 cm | 3 yr | NA | NA |
| 1/8 mass | 1/8 multifocal | 3 yr | ||||||
| 1/8 plaque | 1.5 yr | |||||||
| 1.5 yr | ||||||||
| 2 mo | ||||||||
| Trpkov et al. [6] | 57 | Hydrocele | NA | Multifocal | 1.5 cm | 6 yr | _ | NA |
| Present case | 48 | Hydrocele | Left | Multifocal | 2 cm | 3 yr | - | - |
Table 1. The review of paratesticular WDPM cases in the literature
WDPM, well-differentiated papillary mesothelioma; SV40, simian virus 40; NA, not available.

 E-submission
E-submission
 PubReader
PubReader Cite this Article
Cite this Article