Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 50(1); 2016 > Article
-
Case Study
IgG4-Related Disease Presented as a Mural Mass in the Stomach - Chang Gok Woo1, Jeong Hwan Yook2, Ah Young Kim3,4, Jihun Kim1
-
Journal of Pathology and Translational Medicine 2016;50(1):67-70.
DOI: https://doi.org/10.4132/jptm.2015.07.28
Published online: September 30, 2015
1Department of Pathology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
2Department of Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
3Department of Radiology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
4Research Institute of Radiology, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
- Corresponding Author: Jihun Kim, MD, PhD Department of Pathology, Asan Medical Center, University of Ulsan College of Medicine, 88 Olympic-ro 43-gil, Songpa-gu, Seoul 05505, Korea Tel: +82-2-3010-4556 Fax: +82-2-478-7898 E-mail: jihunkim@amc.seoul.kr
© 2016 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
- Isolated gastric IgG4-related disease (IgG4-RD) is a very rare tumefactive inflammatory condition, with only a few cases reported to date. A 48-year-old woman was incidentally found to have a subepithelial tumor in the stomach. Given a presumptive diagnosis of gastrointestinal stromal tumor or neuroendocrine tumor, she underwent wedge resection. The lesion was vaguely nodular and mainly involved the submucosa and proper muscle layer. Microscopically, all classical features of type I autoimmune pancreatitis including lymphoplasmacytic infiltration, storiform fibrosis, obliterative phlebitis, and numerous IgG4-positive plasma cells were seen. She had no evidence of IgG4-RD in other organs. Although very rare, IgG4-RD should be considered one of the differential diagnoses in the setting of gastric wall thickening or subepithelial mass-like lesion. Deep biopsy with awareness of this entity might avoid unnecessary surgical intervention.
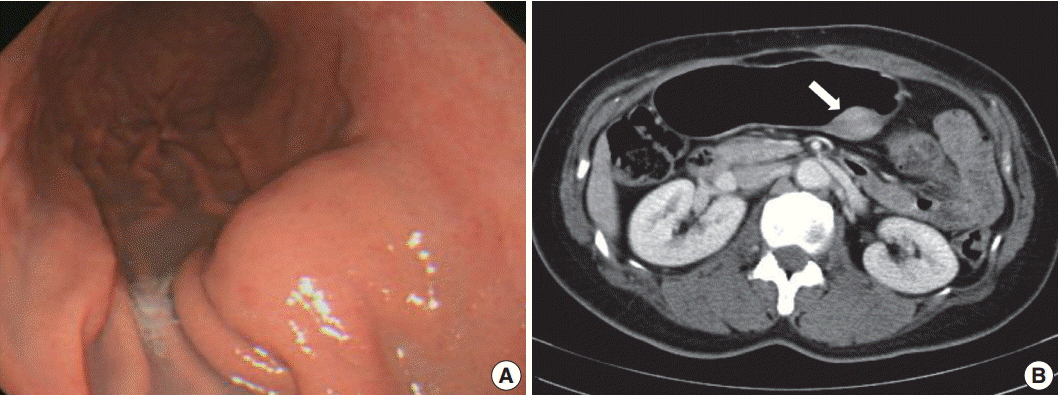
- A 48-year-old, previously healthy woman was found to have a subepithelial tumor during health screening endoscopy (Fig. 1A). Abdominal computed tomography demonstrated a 3.6× 2.2 cm, well-defined, solid, enhancing submucosal mass on the posterior wall of the stomach midbody (Fig. 1B). Radiologic differential diagnoses included GI stromal tumor and neuroendocrine tumor. No remarkable findings were observed in other organs. Seven years ago, she had undergone modified radical mastectomy for breast cancer. There was no further history, symptoms, or signs of systemic disease, and laboratory tests were unremarkable. Serum IgG4 level was not measured preoperatively. Given a presumptive diagnosis of submucosal neoplasm, wedge resection was performed.
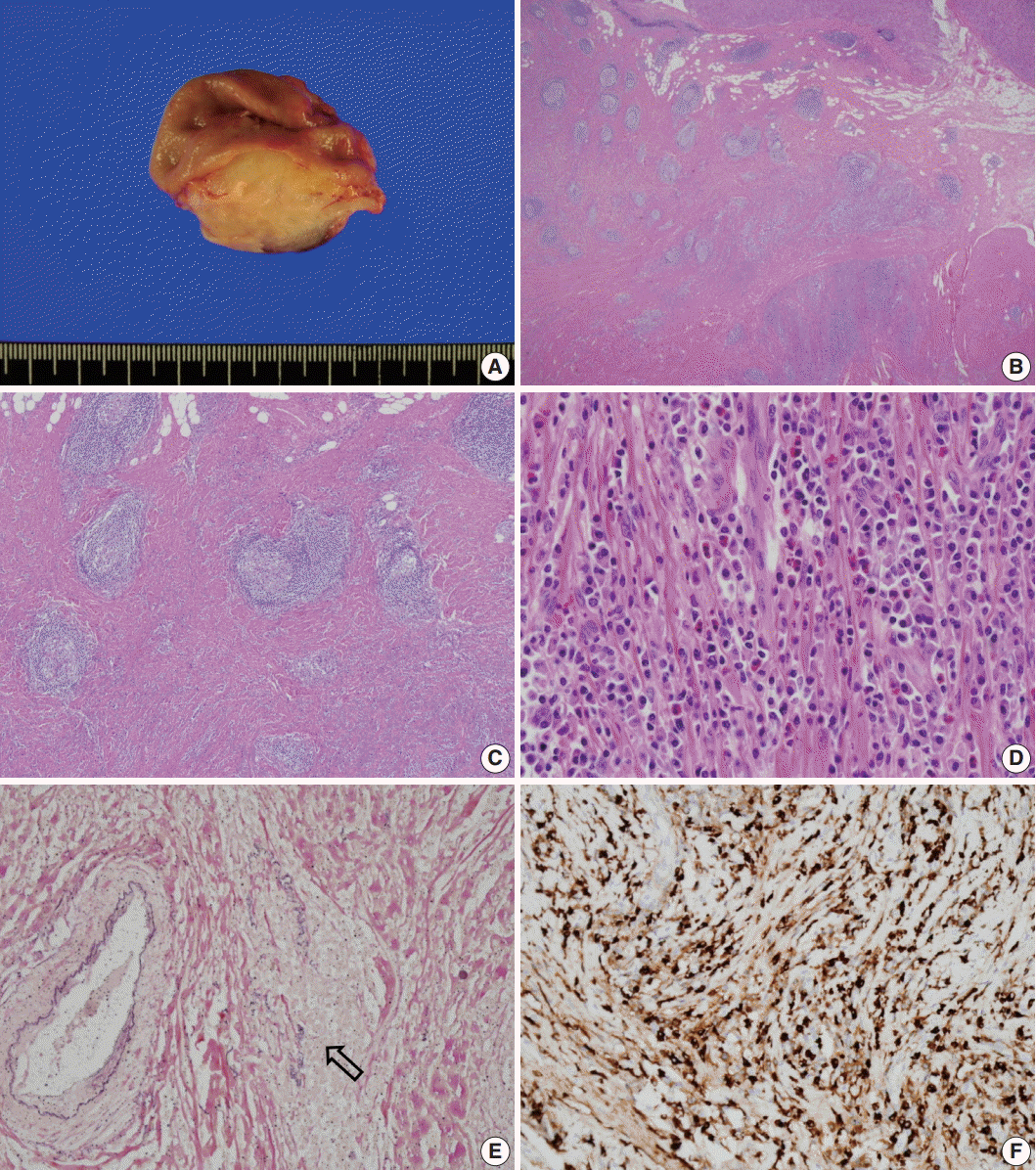
- Grossly, the lesion was a poorly circumscribed, yellowish grey, fusiform mass involving the area from the submucosa to subserosa (Fig. 2A). The overlying mucosa was intact, and there was no ulceration. Microscopically, the mass showed marked fibrosis, often in a storiform pattern of many lymphoid follicles with well-formed germinal centers, and diffuse inflammatory cell infiltration. The infiltrated inflammatory cells were mainly lymphocytes and plasma cells, but some eosinophils were also found (Fig. 2B–D). Obliterative phlebitis was occasionally observed in elastic staining (Fig. 2E). There were numerous IgG4-positive cells throughout the lesion, and the number of IgG4-positive plasma cells was up to 210 per high-power field (Fig. 2F). The IgG4 to IgG-positive cell number ratio was about 85%; however, there were only a few IgG4-positive cells in the mucosa. There was no significant myofibroblastic proliferation or immunostaining for anaplastic lymphoma kinase; therefore, the possibility of inflammatory myofibroblastic tumor was excluded. We concluded that this lesion was IgG4-RD. The patient’s postoperative course was uneventful, and she was discharged without any complications. No recurrence was observed during the 10-month follow-up period.
CASE REPORT
- Here, we described a case of isolated gastric IgG4-RD presenting as a fusiform mural mass mimicking neoplasm, such as GI stromal tumor or neuroendocrine tumor. To the best of our knowledge, this is the ninth case of gastric IgG4-RD. Histologically, this case demonstrated all the important features of IgG4-RD, including dense lymphoplasmacytic infiltration, storiform fibrosis, obliterative phlebitis, and abundant IgG4-positive cells. Although other diagnostic criteria, such as elevated serum IgG4 level or response to steroid therapy, could not be confirmed due to the clinical presentation, typical histopathologic features led us to consider IgG4-RD.
- Increased IgG4-positive plasma cells can be seen in other organs and in many conditions, including non-specific chronic inflammation, lymphoma, and other malignancies [4,6-8]. However, these lesions lack other characteristic histopathologic findings, such as storiform fibrosis and oblierative phlebitis, as has been described in the consensus statement on the pathology of IgG4-RD [4]. Although abundant IgG4-positive plasma cell infiltration is not uncommon in the GI tract in the setting of autoimmune pancreatitis, the simple presence of IgG4-positive cells does not justify a diagnosis of IgG4-RD in the absence of other gross and microscopic features, such as tumefactive nature, storiform fibrosis, and obliterative phlebitis.
- Including the present case, there have been nine cases of massforming IgG4-RD in the stomach [9-14]. A case of probable IgG4-RD that presented as a gastric ulcer has also been reported [15,16], but we excluded this case from the present review. As is summarized in Table 1, most gastric IgG4-RD was detected in middle age (mean, 58.8 years; range, 45 to 75 years), and men and women were affected equally, although the total number of patients is likely too small to reveal any meaningful data. Seven patients had solitary nodules or masses, whereas two patients had multiple polyps or nodules. The two patients with multiple lesions also had autoimmune pancreatitis and autoimmune polyendocrinopathy, respectively. Four of the seven cases showing a solitary lesion had no sign of multi-organ involvement. Most cases of gastric IgG4-RD (six of nine) involved the submucosal layer of the gastric body. Proper muscle or mucosa was variably involved. Serum IgG4 was increased only in patients with associated autoimmune pancreatitis. Most gastric IgG4-RD patients were treated surgically except for one patient with autoimmune pancreatitis who was treated with steroid.
- Steroid treatment is the first therapeutic option in IgG4-RD [17], but all reported isolated gastric IgG4-RD cases were surgically resected, presumably because they are rare and difficult to diagnose without pathologic examination of a resected specimen. Unnecessary surgery might be avoided if the possibility of IgG4-RD is kept in mind and careful pathologic evaluation including IgG4 immunostaining is performed on a deep biopsy obtained using endoscopic ultrasonography.
DISCUSSION
| Reference | Sex/Age (yr) | Endoscopic finding | Sites | Invovement | Serum IgG4 | Procedure | Associated condition |
|---|---|---|---|---|---|---|---|
| Baez et al. [10] | M/58 | Nodule, 1.4 cm | Fundus and body | Mucosa | Normal | Steroid | AIP, IgG4-related sialadenitis |
| Kaji et al. [11] | M/74 | Mutiple polyps with erosion and redness | Body | Mucosa | Increased | NA | AIP |
| Chetty et al. [12] | F/45 | Nodule, 1.5 cm | Fundus | Submucosa | Normal | WR | Raynaud’s disease |
| Chetty et al. [12] | M/60 | Multiple nodules, up to 2.2 cm | Antrum | Proper muscle to submucosa | NA | DG | Autoimmune polyendocrinopathy |
| Rollins et al. [13] | F/75 | Polypoid lesion, 5.6 cm | Body | Submucosa | NA | WR | None |
| Na et al. [9] | M/56 | Nodule, 0.8 cm | Low body | Submucosa | NA | ESD | Type 2 diabetes mellitus |
| Kim et al. [14] | F/59 | Mass, 3.3 cm | Midbody | Proper muscle | Normal | WR | None |
| Kim et al. [14] | F/54 | Mass, 2.1 cm | NA | Proper muscle to submucosa | Normal | WR | None |
| Present case | F/48 | Mass, 3.6 cm | Midbody | Submucosa to subserosa | NA | WR | None |
- 1. Hamano H, Kawa S, Horiuchi A, et al. High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med 2001; 344: 732-8. ArticlePubMed
- 2. Kamisawa T, Funata N, Hayashi Y, et al. A new clinicopathological entity of IgG4-related autoimmune disease. J Gastroenterol 2003; 38: 982-4. ArticlePubMedPDF
- 3. Stone JH, Zen Y, Deshpande V. IgG4-related disease. N Engl J Med 2012; 366: 539-51. ArticlePubMed
- 4. Deshpande V, Zen Y, Chan JK, et al. Consensus statement on the pathology of IgG4-related disease. Mod Pathol 2012; 25: 1181-92. PubMed
- 5. Koizumi S, Kamisawa T, Kuruma S, et al. Immunoglobulin G4-related gastrointestinal diseases, are they immunoglobulin G4-related diseases? World J Gastroenterol 2013; 19: 5769-74. ArticlePubMedPMC
- 6. Strehl JD, Hartmann A, Agaimy A. Numerous IgG4-positive plasma cells are ubiquitous in diverse localised non-specific chronic inflammatory conditions and need to be distinguished from IgG4-related systemic disorders. J Clin Pathol 2011; 64: 237-43. ArticlePubMed
- 7. Zhang L, Notohara K, Levy MJ, Chari ST, Smyrk TC. IgG4-positive plasma cell infiltration in the diagnosis of autoimmune pancreatitis. Mod Pathol 2007; 20: 23-8. ArticlePubMedPDF
- 8. Witkiewicz AK, Kennedy EP, Kennyon L, Yeo CJ, Hruban RH. Synchronous autoimmune pancreatitis and infiltrating pancreatic ductal adenocarcinoma: case report and review of the literature. Hum Pathol 2008; 39: 1548-51. ArticlePubMed
- 9. Na KY, Sung JY, Jang JY, et al. Gastric nodular lesion caused by IgG4-related disease. Pathol Int 2012; 62: 716-8. ArticlePubMed
- 10. Baez JC, Hamilton MJ, Bellizzi A, Mortelé KJ. Gastric involvement in autoimmune pancreatitis: MDCT and histopathologic features. JOP 2010; 11: 610-3. PubMed
- 11. Kaji R, Okabe Y, Ishida Y, et al. Autoimmune pancreatitis presenting with IgG4-positive multiple gastric polyps. Gastrointest Endosc 2010; 71: 420-2. ArticlePubMed
- 12. Chetty R, Serra S, Gauchotte G, Märkl B, Agaimy A. Sclerosing nodular lesions of the gastrointestinal tract containing large numbers of IgG4 plasma cells. Pathology 2011; 43: 31-5. ArticlePubMed
- 13. Rollins KE, Mehta SP, O’Donovan M, Safranek PM. Gastric IgG4-related autoimmune fibrosclerosing pseudotumour: a novel location. ISRN Gastroenterol 2011; 2011: 873087.ArticlePubMedPDF
- 14. Kim DH, Kim J, Park DH, et al. Immunoglobulin G4-related inflammatory pseudotumor of the stomach. Gastrointest Endosc 2012; 76: 451-2. ArticlePubMed
- 15. Bateman AC, Sommerlad M, Underwood TJ. Chronic gastric ulceration: a novel manifestation of IgG4-related disease? J Clin Pathol 2012; 65: 569-70. ArticlePubMed
- 16. Fujita T, Ando T, Sakakibara M, Hosoda W, Goto H. Refractory gastric ulcer with abundant IgG4-positive plasma cell infiltration: a case report. World J Gastroenterol 2010; 16: 2183-6. ArticlePubMedPMC
- 17. Kamisawa T, Okazaki K, Kawa S, Shimosegawa T, Tanaka M; Research Committee for Intractable Pancreatic Disease and Japan Pancreas Society. Japanese consensus guidelines for management of autoimmune pancreatitis: III. Treatment and prognosis of AIP. J Gastroenterol 2010; 45: 471-7. ArticlePubMedPDF
REFERENCES
Figure & Data
References
Citations

- Compromiso gástrico por enfermedad relacionada con IgG4
Gilberto Jaramillo Trujillo, Oscar Fernando Ruiz, Melissa González Pabón, Maria Andrea Jaramillo Trujillo
Revista Repertorio de Medicina y Cirugía.2024; 33(3): 319. CrossRef - Value of High‐Frequency Ultrasonography in the Qualitative and Semi‐Quantitative Assessment of Immunoglobulin G4‐Related Submandibular Sialadenitis
Lei Chen, Lin Nong, Jumei Liu, Luzeng Chen, Yuhong Shao, Xiuming Sun
Journal of Ultrasound in Medicine.2023; 42(10): 2235. CrossRef - IgG4-related pseudotumours: a series of 12 cases and a review of the literature
Andrea Maccagno, Bianca Grosser, László Füzesi, Björn Konukiewitz, Dmytro Vlasenko, Dorothea Weckermann, Stephan Raab, Johannes Zenk, Abbas Agaimy, Bruno Märkl
Pathology.2022; 54(5): 563. CrossRef - IgG4-Related Disease With Gastrointestinal Involvement: Case Reports and Literature Review
Xinhe Zhang, Xing Jin, Lin Guan, Xuyong Lin, Xuedan Li, Yiling Li
Frontiers in Immunology.2022;[Epub] CrossRef - Clinicopathological characteristics of gastric IgG4‐related disease: Systematic scoping review
Haruki Sawada, Torrey Czech, Krixie Silangcruz, Landon Kozai, Adham Obeidat, Eric Andrew Wien, Midori Filiz Nishimura, Asami Nishikori, Yasuharu Sato, Yoshito Nishimura
Journal of Gastroenterology and Hepatology.2022; 37(10): 1865. CrossRef - Utility of gastric biopsy in diagnosing IgG4‐related gastrointestinal disease
Kaori Uchino, Kenji Notohara, Takeshi Uehara, Yasuhiro Kuraishi, Junya Itakura, Akihiro Matsukawa
Pathology International.2021; 71(2): 124. CrossRef - A reappraisal of sclerosing nodular and/or polypoid lesions of the gastrointestinal tract rich in IgG4‐positive plasma cells
Runjan Chetty
Histopathology.2020; 76(6): 832. CrossRef - Gastric IgG4-related disease presenting as a mass lesion and masquerading as a gastrointestinal stromal tumor
Banumathi Ramakrishna, Rohan Yewale, Kavita Vijayakumar, Patta Radhakrishna, Balakrishnan Siddartha Ramakrishna
Journal of Pathology and Translational Medicine.2020; 54(3): 258. CrossRef - IgG4-related Sclerosing Disease Forming a Gastric Submucosal Tumor Diagnosed after Laparoscopic Endoscopic Cooperative Surgery—Report of a Case—
Tatsuki ISHIKAWA, Katsunori NAKANO, Masafumi OSAKA, Yayoi KADOTANI, Kaori OKUGAWA, Kiyokazu AKIOKA, Kenta SHIGEMORI, Yohei HOSOKAWA
Nihon Rinsho Geka Gakkai Zasshi (Journal of Japan Surgical Association).2020; 81(2): 254. CrossRef - Calcifying fibrous tumor of the gastrointestinal tract: A clinicopathologic review and update
Donald Turbiville, Xu-Chen Zhang
World Journal of Gastroenterology.2020; 26(37): 5597. CrossRef - A Suspected Case of IgG4-Related Appendiceal Pseudotumor
Yudai Hojo, Yoshiharu Shirakata, Ai Izumi, Jun Matsui, Tokuyuki Yamashita, Hikaru Aoki, Makoto Kurimoto, Masaaki Hirata, Naoki Goda, Hiroaki Ito, Jun Tamura
The Japanese Journal of Gastroenterological Surgery.2020; 53(12): 976. CrossRef - Immunoglobulin G4-related gastric pseudotumor – An impostor
Manuel Santiago Mosquera, Andrea Suarez Gómez, Hugo Herrera, Karen Moreno-Medina, Alejandro González-Orozco, Carlos J-Perez Rivera
International Journal of Surgery Case Reports.2020; 75(C): 333. CrossRef - Imaging and pathological features of gastric lesion of immunoglobulin G4-related disease: A case report and review of the recent literature
Dai Inoue, Norihide Yoneda, Kotaro Yoshida, Hiromi Nuka, Jun Kinoshita, Sachio Fushida, Fumihito Toshima, Tetsuya Minami, Masayuki Takahira, Shoko Hamaoka, Hiroko Ikeda, Toshifumi Gabata, Mitsuhiro Kawano
Modern Rheumatology.2019; 29(2): 377. CrossRef - Immunoglobulin G4-Related Gastric Ulcer Mimicking Advanced Stomach Cancer in a Patient with Type I Autoimmune Pancreatitis
Joung Ha Park, Jin Hee Noh, Jang ho Lee, Goeun Lee, Seung-Mo Hong, Kwang Bum Cho, Myung-Hwan Kim
The Korean Journal of Medicine.2019; 94(3): 287. CrossRef - Review of IgG4-related disease
Raquel Sánchez-Oro, Elsa María Alonso-Muñoz, Lidia Martí Romero
Gastroenterología y Hepatología (English Edition).2019; 42(10): 638. CrossRef - Revisión de la enfermedad relacionada con la IgG4
Raquel Sánchez-Oro, Elsa María Alonso-Muñoz, Lidia Martí Romero
Gastroenterología y Hepatología.2019; 42(10): 638. CrossRef - Gastrointestinal manifestation of immunoglobulin G4-related disease: clarification through a multicenter survey
Kenji Notohara, Terumi Kamisawa, Kazushige Uchida, Yoh Zen, Mitsuhiro Kawano, Satomi Kasashima, Yasuharu Sato, Masahiro Shiokawa, Takeshi Uehara, Hajime Yoshifuji, Hiroko Hayashi, Koichi Inoue, Keisuke Iwasaki, Hiroo Kawano, Hiroyuki Matsubayashi, Yukitos
Journal of Gastroenterology.2018; 53(7): 845. CrossRef - IgG4-Related Disease Mimicking Crohn’s Disease: A Case Report and Review of Literature
Fabiana Ciccone, Antonio Ciccone, Mirko Di Ruscio, Filippo Vernia, Gianluca Cipolloni, Gino Coletti, Giuseppe Calvisi, Giuseppe Frieri, Giovanni Latella
Digestive Diseases and Sciences.2018; 63(4): 1072. CrossRef - IgG4-related Disease in the Stomach which Was Confused with Gastrointestinal Stromal Tumor (GIST): Two Case Reports and Review of the Literature
Ho Seok Seo, Yoon Ju Jung, Cho Hyun Park, Kyo Young Song, Eun Sun Jung
Journal of Gastric Cancer.2018; 18(1): 99. CrossRef - Multivisceral IgG4-related disease presenting as recurrent massive gastrointestinal bleeding: a case report and literature review
Xuexue Deng, Ronghua Fang, Jianshu Zhang, Rongqiong Li
BMC Gastroenterology.2018;[Epub] CrossRef - IgG4-Related Sclerosing Disease Presenting as a Gastric Submucosal Tumor
Takashi Masuda, Toshifumi Matsumoto, Yushi Kaishakuji, Hirotada Tajiri, Akinori Egashira, Hirofumi Kawanaka
The Japanese Journal of Gastroenterological Surgery.2018; 51(10): 599. CrossRef - A rare case of IgG4-related disease: a gastric mass, associated with regional lymphadenopathy
Dimitar Bulanov, Elena Arabadzhieva, Sasho Bonev, Atanas Yonkov, Diana Kyoseva, Tihomir Dikov, Violeta Dimitrova
BMC Surgery.2016;[Epub] CrossRef
 PubReader
PubReader ePub Link
ePub Link-
 Cite this Article
Cite this Article
- Cite this Article
-
- Close
- Download Citation
- Close
- Figure


Fig. 1.
Fig. 2.
| Reference | Sex/Age (yr) | Endoscopic finding | Sites | Invovement | Serum IgG4 | Procedure | Associated condition |
|---|---|---|---|---|---|---|---|
| Baez et al. [10] | M/58 | Nodule, 1.4 cm | Fundus and body | Mucosa | Normal | Steroid | AIP, IgG4-related sialadenitis |
| Kaji et al. [11] | M/74 | Mutiple polyps with erosion and redness | Body | Mucosa | Increased | NA | AIP |
| Chetty et al. [12] | F/45 | Nodule, 1.5 cm | Fundus | Submucosa | Normal | WR | Raynaud’s disease |
| Chetty et al. [12] | M/60 | Multiple nodules, up to 2.2 cm | Antrum | Proper muscle to submucosa | NA | DG | Autoimmune polyendocrinopathy |
| Rollins et al. [13] | F/75 | Polypoid lesion, 5.6 cm | Body | Submucosa | NA | WR | None |
| Na et al. [9] | M/56 | Nodule, 0.8 cm | Low body | Submucosa | NA | ESD | Type 2 diabetes mellitus |
| Kim et al. [14] | F/59 | Mass, 3.3 cm | Midbody | Proper muscle | Normal | WR | None |
| Kim et al. [14] | F/54 | Mass, 2.1 cm | NA | Proper muscle to submucosa | Normal | WR | None |
| Present case | F/48 | Mass, 3.6 cm | Midbody | Submucosa to subserosa | NA | WR | None |
M, male; AIP, autoimmune pancreatitis; NA, not available; F, female; WR, wedge resection; DG, distal gastrectomy; ESD, endoscopic submucosal dissection.

 E-submission
E-submission




