Search
- Page Path
- HOME > Search
- PSMA expression in hepatic colorectal cancer metastasis
- Eundong Park, Michel Kmeid, Xin Wang, Haiyan Qiu, Clifton G. Fulmer, Marcello P. Toscano, Nusret Bekir Subasi, Maciej Gracz, Hwajeong Lee
- J Pathol Transl Med. 2026;60(1):107-123. Published online January 14, 2026
- DOI: https://doi.org/10.4132/jptm.2025.10.20
- 1,667 View
- 111 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Prostate-specific membrane antigen (PSMA) is expressed in the neovasculature of various malignancies, such as colorectal cancer (CRC) and hepatocellular carcinoma (HCC). However, PSMA expression in hepatic CRC metastasis has not been studied in detail. Methods: The PSMA expression in primary CRC and corresponding hepatic metastasis was evaluated by immunohistochemistry in a metastatic CRC cohort (n = 56), which was divided into subgroups according to treatment history and timing of metastasis. Demographic and histological characteristics of primary CRC were collected and their relationships with PSMA expression were examined. Additionally, the PSMA expression in resected HCC (n = 76) was compared with that of hepatic CRC metastasis. Results: In primary CRC, PSMA level showed a positive association with tumor size. Lower PSMA expression in hepatic metastasis was associated with higher primary CRC grade, advanced pTNM stage at the time of CRC resection, presence of tumor deposit, and unresectability of metastatic lesion. PSMA expression in primary CRC correlated with that in hepatic metastasis only in concurrent and untreated metastasis subgroup. PSMA expression in primary CRC and hepatic metastasis, regardless of treatment history and timing of metastasis, was not significantly different from that of HCC. Conclusions: Several adverse pathological features of primary CRC were associated with a lower PSMA expression in hepatic metastasis. PSMA expression in hepatic metastasis correlated with that of primary CRC only in concurrent and untreated subgroup. Primary HCC and hepatic CRC metastasis show comparable levels of PSMA expression. -
Citations
Citations to this article as recorded by- Incidental detection of PDAC via 18F-PSMA PET/CT in a patient with recurrent prostate cancer. A case report
Giordano Savelli, Mattia Bonacina, Alberto Soffientini, Elvira Archiati, Claudio Bnà, Alberto Zaniboni
Frontiers in Nuclear Medicine.2026;[Epub] CrossRef
- Incidental detection of PDAC via 18F-PSMA PET/CT in a patient with recurrent prostate cancer. A case report
- Paricalcitol prevents MAPK pathway activation and inflammation in adriamycin-induced kidney injury in rats
- Amanda Lima Deluque, Lucas Ferreira de Almeida, Beatriz Magalhães Oliveira, Cláudia Silva Souza, Ana Lívia Dias Maciel, Heloísa Della Coletta Francescato, Cleonice Giovanini, Roberto Silva Costa, Terezila Machado Coimbra
- J Pathol Transl Med. 2024;58(5):219-228. Published online August 27, 2024
- DOI: https://doi.org/10.4132/jptm.2024.07.12
- 4,156 View
- 222 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Activation of the mitogen-activated protein kinase (MAPK) pathway induces uncontrolled cell proliferation in response to inflammatory stimuli. Adriamycin (ADR)-induced nephropathy (ADRN) in rats triggers MAPK activation and pro-inflammatory mechanisms by increasing cytokine secretion, similar to chronic kidney disease (CKD). Activation of the vitamin D receptor (VDR) plays a crucial role in suppressing the expression of inflammatory markers in the kidney and may contribute to reducing cellular proliferation. This study evaluated the effect of pre-treatment with paricalcitol on ADRN in renal inflammation mechanisms.
Methods
Male Sprague-Dawley rats were implanted with an osmotic minipump containing activated vitamin D (paricalcitol, Zemplar, 6 ng/day) or vehicle (NaCl 0.9%). Two days after implantation, ADR (Fauldoxo, 3.5 mg/kg) or vehicle (NaCl 0.9%) was injected. The rats were divided into four experimental groups: control, n = 6; paricalcitol, n = 6; ADR, n = 7 and, ADR + paricalcitol, n = 7.
Results
VDR activation was demonstrated by increased CYP24A1 in renal tissue. Paricalcitol prevented macrophage infiltration in the glomeruli, cortex, and outer medulla, prevented secretion of tumor necrosis factor-α, and interleukin-1β, increased arginase I and decreased arginase II tissue expressions, effects associated with attenuation of MAPK pathways, increased zonula occludens-1, and reduced cell proliferation associated with proliferating cell nuclear antigen expression. Paricalcitol treatment decreased the stromal cell-derived factor 1α/chemokine C-X-C receptor type 4/β-catenin pathway.
Conclusions
Paricalcitol plays a renoprotective role by modulating renal inflammation and cell proliferation. These results highlight potential targets for treating CKD. -
Citations
Citations to this article as recorded by- Attenuating amiodarone-induced lung toxicity by the vitamin D receptor activator paricalcitol in rats: targeting TLR4/NF-κB/HIF-1α and TGF-β/Smad signaling pathways
Aamal G. El-Waseif, Mahmoud Elshal, Dalia H. El-Kashef, Nashwa M. Abu-Elsaad
Naunyn-Schmiedeberg's Archives of Pharmacology.2026; 399(3): 4067. CrossRef - Perirenal fat differs in patients with chronic kidney disease receiving different vitamin D-based treatments: a preliminary study
Ana Checa-Ros, Antonella Locascio, Owahabanun-Joshua Okojie, Pablo Abellán-Galiana, Luis D’Marco
BMC Nephrology.2025;[Epub] CrossRef
- Attenuating amiodarone-induced lung toxicity by the vitamin D receptor activator paricalcitol in rats: targeting TLR4/NF-κB/HIF-1α and TGF-β/Smad signaling pathways
- Senescent tumor cells in colorectal cancer are characterized by elevated enzymatic activity of complexes 1 and 2 in oxidative phosphorylation
- Jun Sang Shin, Tae-Gyu Kim, Young Hwa Kim, So Yeong Eom, So Hyun Park, Dong Hyun Lee, Tae Jun Park, Soon Sang Park, Jang-Hee Kim
- J Pathol Transl Med. 2023;57(6):305-314. Published online November 7, 2023
- DOI: https://doi.org/10.4132/jptm.2023.10.09
- 7,498 View
- 318 Download
- 3 Web of Science
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Cellular senescence is defined as an irreversible cell cycle arrest caused by various internal and external insults. While the metabolic dysfunction of senescent cells in normal tissue is relatively well-established, there is a lack of information regarding the metabolic features of senescent tumor cells.
Methods
Publicly available single-cell RNA-sequencing data from the GSE166555 and GSE178341 datasets were utilized to investigate the metabolic features of senescent tumor cells. To validate the single-cell RNA-sequencing data, we performed senescence-associated β-galactosidase (SA-β-Gal) staining to identify senescent tumor cells in fresh frozen colorectal cancer tissue. We also evaluated nicotinamide adenine dinucleotide dehydrogenase–tetrazolium reductase (NADH-TR) and succinate dehydrogenase (SDH) activity using enzyme histochemical methods and compared the staining with SA-β-Gal staining. MTT assay was performed to reveal the complex 1 activity of the respiratory chain in in-vitro senescence model.
Results
Single-cell RNA-sequencing data revealed an upregulation in the activity of complexes 1 and 2 in oxidative phosphorylation, despite overall mitochondrial dysfunction in senescent tumor cells. Both SA-β-Gal and enzyme histochemical staining using fresh frozen colorectal cancer tissues indicated a high correlation between SA-β-Gal positivity and NADH-TR/SDH staining positivity. MTT assay showed that senescent colorectal cancer cells exhibit higher absorbance in 600 nm wavelength.
Conclusions
Senescent tumor cells exhibit distinct metabolic features, characterized by upregulation of complexes 1 and 2 in the oxidative phosphorylation pathway. NADH-TR and SDH staining represent efficient methods for detecting senescent tumor cells in colorectal cancer. -
Citations
Citations to this article as recorded by- Multifacet Roles of Cellular Senescence in Cancer: Mechanisms and Therapeutic Implications
Huajie Mao, Wanning Liu, Yuanyuan Su, Yuxuan Ma, Xiaodi Zhao, Yuanyuan Lu
MedComm – Oncology.2026;[Epub] CrossRef - Senescence, Aging and Disease Throughout the Gastrointestinal System
Sofia Ferreira-Gonzalez, Tomonori Matsumoto, Eiji Hara, Stuart J. Forbes
Gastroenterology.2025; 169(7): 1357. CrossRef - Cellular Aging and Senescence in Cancer: A Holistic Review of Cellular Fate Determinants
Muhammad Tufail, Yu-Qi Huang, Jia-Ju Hu, Jie Liang, Cai-Yun He, Wen-Dong Wan, Can-Hua Jiang, Hong Wu, Ning Li
Aging and disease.2024;[Epub] CrossRef - Real-time assessment of relative mitochondrial ATP synthesis response against inhibiting and stimulating substrates (MitoRAISE)
Eun Sol Chang, Kyoung Song, Ji-Young Song, Minjung Sung, Mi-Sook Lee, Jung Han Oh, Ji-Yeon Kim, Yeon Hee Park, Kyungsoo Jung, Yoon-La Choi
Cancer & Metabolism.2024;[Epub] CrossRef
- Multifacet Roles of Cellular Senescence in Cancer: Mechanisms and Therapeutic Implications
- Prognostic significance of viable tumor size measurement in hepatocellular carcinomas after preoperative locoregional treatment
- Yoon Jung Hwang, Youngeun Lee, Hyunjin Park, Yangkyu Lee, Kyoungbun Lee, Haeryoung Kim
- J Pathol Transl Med. 2021;55(5):338-348. Published online September 2, 2021
- DOI: https://doi.org/10.4132/jptm.2021.07.26
- 6,798 View
- 122 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Preoperative locoregional treatment (LRT) for hepatocellular carcinoma (HCC) often induces intratumoral necrosis without affecting the overall tumor size, and residual viable tumor size (VTS) on imaging is an important clinical parameter for assessing post-treatment response. However, for surgical specimens, it is unclear whether the VTS would be more relevant to prognosis compared to total tumor size (TTS).
Methods
A total of 142 surgically resected solitary HCC cases were retrospectively reviewed. The TTS and VTS were assessed by applying the modified Response Evaluation Criteria in Solid Tumors method to the resected specimens, and correlated with the clinicopathological features and survival.
Results
As applying VTS, 13/142 cases (9.2%) were down-staged to ypT1a. Although the survival analysis results for overall survival according to TTS or VTS were similar, VTS was superior to predict disease-free survival (DFS; p = .023) compared to TTS (p = .08). In addition, multivariate analysis demonstrated VTS > 2 cm to be an independent predictive factor for decreased DFS (p = .001). In the subpopulation of patients with LRT (n = 54), DFS in HCCs with TTS or VTS > 2 cm were significantly shorter than those with TTS or VTS ≤ 2 cm (p = .047 and p = .001, respectively). Interestingly, HCCs with TTS > 2 cm but down-staged to VTS ≤ 2 cm after preoperative LRT had similar survival to those with TTS ≤ 2 cm.
Conclusions
Although the prognostic impact of tumor size was similar regardless of whether TTS or VTS was applied, reporting VTS may help to increase the number of candidates for surgery in HCC patients with preoperative LRT. -
Citations
Citations to this article as recorded by- PET-Assessed Metabolic Tumor Volume Across the Spectrum of Solid-Organ Malignancies: A Review of the Literature
Anusha Agarwal, Chase J. Wehrle, Sangeeta Satish, Paresh Mahajan, Suneel Kamath, Shlomo Koyfman, Wen Wee Ma, Maureen Linganna, Jamak Modaresi Esfeh, Charles Miller, David C. H. Kwon, Andrea Schlegel, Federico Aucejo
Biomedicines.2025; 13(1): 123. CrossRef - Measures for response assessment in HCC treatment
Fereshteh Yazdanpanah, Omar Al-Daoud, Moein Moradpour, Stephen Hunt
Hepatoma Research.2024;[Epub] CrossRef - Machine Learning for Dynamic Prognostication of Patients With Hepatocellular Carcinoma Using Time-Series Data: Survival Path Versus Dynamic-DeepHit HCC Model
Lujun Shen, Yiquan Jiang, Tao Zhang, Fei Cao, Liangru Ke, Chen Li, Gulijiayina Nuerhashi, Wang Li, Peihong Wu, Chaofeng Li, Qi Zeng, Weijun Fan
Cancer Informatics.2024;[Epub] CrossRef - Construction and validation of a novel signature based on epithelial-mesenchymal transition–related genes to predict prognosis and immunotherapy response in hepatocellular carcinoma by comprehensive analysis of the tumor microenvironment
Biao Gao, Yafei Wang, Shichun Lu
Functional & Integrative Genomics.2023;[Epub] CrossRef - Cellular senescence affects energy metabolism, immune infiltration and immunotherapeutic response in hepatocellular carcinoma
Biao Gao, Yafei Wang, Shichun Lu
Scientific Reports.2023;[Epub] CrossRef
- PET-Assessed Metabolic Tumor Volume Across the Spectrum of Solid-Organ Malignancies: A Review of the Literature
- Hepatocellular adenomas: recent updates
- Haeryoung Kim, Young Nyun Park
- J Pathol Transl Med. 2021;55(3):171-180. Published online April 7, 2021
- DOI: https://doi.org/10.4132/jptm.2021.02.27
- 12,221 View
- 553 Download
- 9 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF - Hepatocellular adenoma (HCA) is a heterogeneous entity, from both the histomorphological and molecular aspects, and the resultant subclassification has brought a strong translational impact for both pathologists and clinicians. In this review, we provide an overview of the recent updates on HCA from the pathologists’ perspective and discuss several practical issues and pitfalls that may be useful for diagnostic practice.
-
Citations
Citations to this article as recorded by- Preventing false positive imaging diagnosis of HCC: differentiating HCC from mimickers and practical strategies
Ijin Joo
Journal of Liver Cancer.2025; 25(2): 217. CrossRef - Prognostic role of selection criteria for liver transplantation in patients with hepatocellular carcinoma: Review and bibliometric
Pamela Scarlett Espinoza Loyola, Diana Laura Muratalla Bautista, Karen Adela Hernández Bautista, Elizabeth Gil White, José Antonio González Moreno, Daniel Angel Torres del Real, Víctor Manuel Páez Zayas, Carla Escorza-Molina, Fernando Mondragón Rodríguez,
iLIVER.2024; 3(1): 100077. CrossRef - ACG Clinical Guideline: Focal Liver Lesions
Catherine Frenette, Mishal Mendiratta-Lala, Reena Salgia, Robert J. Wong, Bryan G. Sauer, Anjana Pillai
American Journal of Gastroenterology.2024; 119(7): 1235. CrossRef - Hepatocellular adenoma update: diagnosis, molecular classification, and clinical course
Sarah Poetter-Lang, Ahmed Ba-Ssalamah, Nina Bastati, Sami A Ba-Ssalamah, Jacqueline C Hodge, Giuseppe Brancatelli, Valérie Paradis, Valérie Vilgrain
British Journal of Radiology.2024; 97(1163): 1740. CrossRef - Fatal rupture of hepatic adenomatosis: Autopsy case and review of the literature
Sarra Ben Abderrahim, Khouloud Chérif, Zeineb Nfikha, Sarra Gharsallaoui, Imen El Aini, Maher Jedidi, Moncef Mokni, Mohamed Ben Dhiab
Journal of Forensic Sciences.2023; 68(4): 1393. CrossRef - Large Hepatocellular Adenoma Presenting with Iron Deficiency Anemia: A Case Report
Young Kwon Koh, Su Hyun Yoon, Sung Han Kang, Hyery Kim, Ho Joon Im, Suhyeon Ha, Jung-Man Namgoong, Kyung-Nam Koh
Clinical Pediatric Hematology-Oncology.2023; 30(1): 25. CrossRef - A Case Report on a Giant Hepatic Inflammatory Adenoma in a Young Female That Presented as Spontaneous Intrahepatic Hematoma
Andreas Kyvetos, Panagiota Voukelatou, Ioannis Vrettos, Spyridon Pantzios , Ioannis Elefsiniotis
Cureus.2023;[Epub] CrossRef - Advances in Histological and Molecular Classification of Hepatocellular Carcinoma
Joon Hyuk Choi, Swan N. Thung
Biomedicines.2023; 11(9): 2582. CrossRef - Estrobolome and Hepatocellular Adenomas—Connecting the Dots of the Gut Microbial β-Glucuronidase Pathway as a Metabolic Link
Sandica Bucurica, Mihaela Lupanciuc, Florentina Ionita-Radu, Ion Stefan, Alice Elena Munteanu, Daniela Anghel, Mariana Jinga, Elena Laura Gaman
International Journal of Molecular Sciences.2023; 24(22): 16034. CrossRef - Hepatocellular adenoma: what we know, what we do not know, and why it matters
Paulette Bioulac‐Sage, Annette S H Gouw, Charles Balabaud, Christine Sempoux
Histopathology.2022; 80(6): 878. CrossRef
- Preventing false positive imaging diagnosis of HCC: differentiating HCC from mimickers and practical strategies
- Liquid biopsy using extracellular vesicle–derived DNA in lung adenocarcinoma
- In Ae Kim, Jae Young Hur, Hee Joung Kim, Seung Eun Lee, Wan Seop Kim, Kye Young Lee
- J Pathol Transl Med. 2020;54(6):453-461. Published online October 8, 2020
- DOI: https://doi.org/10.4132/jptm.2020.08.13
- 9,536 View
- 177 Download
- 21 Web of Science
- 20 Crossref
-
 Abstract
Abstract
 PDF
PDF - Blood liquid biopsy has emerged as a way of overcoming the clinical limitations of repeat biopsy by testing for the presence of acquired resistance mutations to therapeutic agents. Despite its merits of repeatability and non-invasiveness, this method is currently only used as a supplemental test due to a relatively low sensitivity rate of 50%–60%, and cannot replace tissue biopsy. The circulating tumor DNAs used in blood liquid biopsies are passive products of fragmented DNA with a short half-life released following tumor cell death; the low sensitivity seen with liquid blood biopsy results from this instability, which makes increasing the sensitivity of this test fundamentally difficult. Extracellular vesicles (EVs) are ideal carriers of cancer biomarkers, as cancer cells secret an abundance of EVs, and the contents of tumor cell-originated EVs reflect the molecular and genetic composition of parental cells. In addition, EV-derived DNAs (EV DNAs) consist of large-sized genomic DNAs and tumor-specific oncogenic mutant DNAs. For these reasons, liquid biopsy using EV DNA has the potential to overcome issues arising from tissue shortages associated with small biopsies, which are often seen in lung cancer patients, and the biopsy product can be used in other diagnostic methods, such as epidermal growth factor receptor (EGFR) mutation testing and next-generation sequencing (NGS). A higher sensitivity can be achieved when EV DNAs obtained from bronchoalveolar lavage fluid (BALF) are used rather than those from blood. BALF, when obtained close to the tumor site, is a promising liquid biopsy tool, as it enables the gathering of both cellular and non-cellular fractions of the tumor microenvironment, and provides increased diagnostic sensitivity when compared to blood.
-
Citations
Citations to this article as recorded by- Application of extracellular vesicles in tumor liquid biopsy
Shuai Li, Yating Liu, Dayong Yang
Chinese Science Bulletin.2026; 71(2): 421. CrossRef - Liquid biopsy biomarkers for accurate detection of malignant pulmonary nodules: a meta-analytic approach
Alberto Caballero-Vazquez, Marta Garcia-Cerezo, Laura R. Fernandez-Castro, Concepcion Morales-Garcia, Antonio Jesus Lainez Ramos-Bossini, Fabian Vergara-Rubio, Francisco Gabriel Ortega-Sanchez, Jose Manuel Sanchez-Maldonado
Discover Oncology.2026;[Epub] CrossRef - Meta‐Analysis of Non‐Blood Liquid Biopsy Specimens: Diagnostic Performance in Cancer Detection
Kartavya Kumar Verma
Diagnostic Cytopathology.2026; 54(3): 235. CrossRef - Circulating Extracellular Vesicles as Promising Biomarkers for Precession Diagnostics: A Perspective on Lung Cancer
Sunil Vasu, Vinith Johnson, Archana M, K. Anki Reddy, Uday Kumar Sukumar
ACS Biomaterials Science & Engineering.2025; 11(1): 95. CrossRef - Diagnostic performance of metagenomic next-generation sequencing among hematological malignancy patients with bloodstream infections after antimicrobial therapy
Yueyi Xu, Miaoxin Peng, Tong Zhou, Yonggong Yang, Peipei Xu, Ting Xie, Xuefang Cao, Bing Chen, Jian Ouyang
Journal of Infection.2025; 90(2): 106395. CrossRef - Unraveling extracellular vesicle DNA: Biogenesis, functions, and clinical implications
Mehraneh Nouri, Fateme Nasiri, Samaneh Sharif, Mohammad Reza Abbaszadegan
Pathology - Research and Practice.2025; 269: 155937. CrossRef - Nanobiotechnology: A smart platform of the future transform liquid biopsy era
Srijan Goswami, Palas Samanta, Manab Deb Adhikari
The Journal of Liquid Biopsy.2024; 3: 100137. CrossRef - Mesenchymal stem/stromal cells: dedicator to maintain tumor homeostasis
Juncun Yao, Li Sun, Feng Gao, Wei Zhu
Human Cell.2024;[Epub] CrossRef - Extracellular Vesicle-DNA: The Next Liquid Biopsy Biomarker for Early Cancer Diagnosis?
Irène Tatischeff
Cancers.2023; 15(5): 1456. CrossRef - Isolation of extracellular vesicles from human plasma samples: The importance of controls
Migmar Tsamchoe, Stephanie Petrillo, Anthoula Lazaris, Peter Metrakos
Biotechnology Journal.2023;[Epub] CrossRef - The role of extracellular vesicles in non-small-cell lung cancer, the unknowns, and how new approach methodologies can support new knowledge generation in the field
Sive Mullen, Dania Movia
European Journal of Pharmaceutical Sciences.2023; 188: 106516. CrossRef - Silicon microfabrication technologies for biology integrated advance devices and interfaces
Vuslat B. Juska, Graeme Maxwell, Pedro Estrela, Martyn E. Pemble, Alan O'Riordan
Biosensors and Bioelectronics.2023; 237: 115503. CrossRef - Bronchoalveolar Lavage as Potential Diagnostic Specimens to Genetic Testing in Advanced Nonsmall Cell Lung Cancer
Xuwen Lin, Yazhou Cai, Chenyu Zong, Binbin Chen, Di Shao, Hao Cui, Zheng Li, Ping Xu
Technology in Cancer Research & Treatment.2023;[Epub] CrossRef - In-Cell Labeling Coupled to Direct Analysis of Extracellular Vesicles in the Conditioned Medium to Study Extracellular Vesicles Secretion with Minimum Sample Processing and Particle Loss
Anissa Viveiros, Vaibhavi Kadam, John Monyror, Luis Carlos Morales, Desmond Pink, Aja M. Rieger, Simonetta Sipione, Elena Posse de Chaves
Cells.2022; 11(3): 351. CrossRef - Recent advances in liquid biopsy in cancers: Diagnosis, disease state and treatment response monitoring
Zhixian Chen, Judy Wai Ping Yam
Clinical and Translational Discovery.2022;[Epub] CrossRef - Cell-Secreted Vesicles: Novel Opportunities in Cancer Diagnosis, Monitoring and Treatment
Cristina Catoni, Veronica Di Paolo, Elisabetta Rossi, Luigi Quintieri, Rita Zamarchi
Diagnostics.2021; 11(6): 1118. CrossRef - DNA-Loaded Extracellular Vesicles in Liquid Biopsy: Tiny Players With Big Potential?
Susana García-Silva, Miguel Gallardo, Héctor Peinado
Frontiers in Cell and Developmental Biology.2021;[Epub] CrossRef - Characteristics and Clinical Application of Extracellular Vesicle-Derived DNA
Jae Young Hur, Kye Young Lee
Cancers.2021; 13(15): 3827. CrossRef - Bronchoalveolar Lavage as a Potential Diagnostic Specimens to Genetic Testing in Advanced Lung Cancer
Xuwen Lin, Xueying Wang, Yazhou Cai, Chenyu Zong, Dawei Liu, Jiming Yu, Chenxin Zhou, Jing Yao, Zheng Li, ping xu
SSRN Electronic Journal .2021;[Epub] CrossRef - Multi-Omics Data Integration in Extracellular Vesicle Biology—Utopia or Future Reality?
Leona Chitoiu, Alexandra Dobranici, Mihaela Gherghiceanu, Sorina Dinescu, Marieta Costache
International Journal of Molecular Sciences.2020; 21(22): 8550. CrossRef
- Application of extracellular vesicles in tumor liquid biopsy
- Guanabenz Acetate Induces Endoplasmic Reticulum Stress–Related Cell Death in Hepatocellular Carcinoma Cells
- Hyo Jeong Kang, Hyang Sook Seol, Sang Eun Lee, Young-Ah Suh, Jihun Kim, Se Jin Jang, Eunsil Yu
- J Pathol Transl Med. 2019;53(2):94-103. Published online January 16, 2019
- DOI: https://doi.org/10.4132/jptm.2019.01.14
- 9,749 View
- 200 Download
- 13 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Development of chemotherapeutics for the treatment of advanced hepatocellular carcinoma (HCC) has been lagging. Screening of candidate therapeutic agents by using patient-derived preclinical models may facilitate drug discovery for HCC patients.
Methods
Four primary cultured HCC cells from surgically resected tumor tissues and six HCC cell lines were used for high-throughput screening of 252 drugs from the Prestwick Chemical Library. The efficacy and mechanisms of action of the candidate anti-cancer drug were analyzed via cell viability, cell cycle assays, and western blotting.
Results
Guanabenz acetate, which has been used as an antihypertensive drug, was screened as a candidate anti-cancer agent for HCC through a drug sensitivity assay by using the primary cultured HCC cells and HCC cell lines. Guanabenz acetate reduced HCC cell viability through apoptosis and autophagy. This occurred via inhibition of growth arrest and DNA damage-inducible protein 34, increased phosphorylation of eukaryotic initiation factor 2α, increased activating transcription factor 4, and cell cycle arrest.
Conclusions
Guanabenz acetate induces endoplasmic reticulum stress–related cell death in HCC and may be repositioned as an anti-cancer therapeutic agent for HCC patients. -
Citations
Citations to this article as recorded by- ER stress signaling at the interphase between MASH and HCC
Younis Hazari, Eric Chevet, Béatrice Bailly-Maitre, Claudio Hetz
Hepatology.2026; 83(2): 387. CrossRef - The Integrated Stress Response in Cancer: Paradox and Therapeutic Promise
Chenliang Zhang, Ting Zhang, Qiulin Tang, Yu Zeng, Dan Cao
Comprehensive Physiology.2026;[Epub] CrossRef - The Construction of ceRNA Regulatory Network Unraveled Prognostic Biomarkers and Repositioned Drug Candidates for the Management of Pancreatic Ductal Adenocarcinoma
Busra Aydin, Keziban Okutan, Ozge Onluturk Aydogan, Raghu Sinha, Beste Turanli
Current Issues in Molecular Biology.2025; 47(7): 496. CrossRef - Current trends and future prospects of drug repositioning in gastrointestinal oncology
Nayeralsadat Fatemi, Mina Karimpour, Hoda Bahrami, Mohammad Reza Zali, Vahid Chaleshi, Andrea Riccio, Ehsan Nazemalhosseini-Mojarad, Mehdi Totonchi
Frontiers in Pharmacology.2024;[Epub] CrossRef - Small molecules for impairing endoplasmic reticulum in cancer
Tripti Mishra, Navneet Dubey, Sudipta Basu
Organic & Biomolecular Chemistry.2024; 22(44): 8689. CrossRef -
Guanabenz acetate, an antihypertensive drug repurposed as an inhibitor of
Escherichia coli
biofilm
Arakkaveettil Kabeer Farha, Olivier Habimana, Harold Corke, Olaya Rendueles
Microbiology Spectrum.2024;[Epub] CrossRef - The integrated stress response in cancer progression: a force for plasticity and resistance
Caleb L. Lines, Morgan J. McGrath, Tanis Dorwart, Crystal S. Conn
Frontiers in Oncology.2023;[Epub] CrossRef - Endoplasmic reticulum stress: Multiple regulatory roles in hepatocellular carcinoma
Jiacheng Wu, Shan Qiao, Yien Xiang, Menying Cui, Xiaoxiao Yao, Ruixin Lin, Xuewen Zhang
Biomedicine & Pharmacotherapy.2021; 142: 112005. CrossRef - The two faces of the Integrated Stress Response in cancer progression and therapeutic strategies
Eugenia Licari, Luis Sánchez-del-Campo, Paola Falletta
The International Journal of Biochemistry & Cell Biology.2021; 139: 106059. CrossRef - Repurposing of Guanabenz acetate by encapsulation into long-circulating nanopolymersomes for treatment of triple-negative breast cancer
Yusuf A. Haggag, Mohamed Yasser, Murtaza M. Tambuwala, Suleiman S. El Tokhy, Mohammad Isreb, Ahmed A. Donia
International Journal of Pharmaceutics.2021; 600: 120532. CrossRef - Endoplasmic reticulum stress: New insights into the pathogenesis and treatment of retinal degenerative diseases
Marina S. Gorbatyuk, Christopher R. Starr, Oleg S. Gorbatyuk
Progress in Retinal and Eye Research.2020; 79: 100860. CrossRef - Delineating the role of eIF2α in retinal degeneration
Christopher R. Starr, Marina S. Gorbatyuk
Cell Death & Disease.2019;[Epub] CrossRef - Repositioning of Guanabenz in Conjugation with Gold and Silver Nanoparticles against Pathogenic Amoebae Acanthamoeba castellanii and Naegleria fowleri
Areeba Anwar, Mohammad Ridwane Mungroo, Ayaz Anwar, William J. Sullivan, Naveed Ahmed Khan, Ruqaiyyah Siddiqui
ACS Infectious Diseases.2019; 5(12): 2039. CrossRef
- ER stress signaling at the interphase between MASH and HCC
- Quilty Lesions in the Endomyocardial Biopsies after Heart Transplantation
- Haeyon Cho, Jin-Oh Choi, Eun-Seok Jeon, Jung-Sun Kim
- J Pathol Transl Med. 2019;53(1):50-56. Published online December 26, 2018
- DOI: https://doi.org/10.4132/jptm.2018.11.30
- 8,631 View
- 132 Download
- 6 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
The aim of this study was to investigate the clinical significance of Quilty lesions in endomyocardial biopsies (EMBs) of cardiac transplantation patients.
Methods
A total of 1190EMBs from 117 cardiac transplantation patients were evaluated histologically for Quilty lesions,acute cellular rejection, and antibody-mediated rejection. Cardiac allograft vasculopathy wasdiagnosed by computed tomography coronary angiography. Clinical information, including thepatients’ survival was retrieved by a review of medical records.
Results
Eighty-eight patients(75.2%) were diagnosed with Quilty lesions, which were significantly associated with acute cellularrejection, but not with acute cellular rejection ≥ 2R or antibody-mediated rejection. In patientsdiagnosed with both Quilty lesions and acute cellular rejection, the time-to-onset of Quilty lesionsfrom transplantation was longer than that of acute cellular rejections. We found a significant associationbetween Quilty lesions and cardiac allograft vasculopathy. No significant relationship wasfound between Quilty lesions and the patients’ survival.
Conclusions
Quilty lesion may be an indicator of previous acute cellular rejection rather than a predictor for future acute cellular rejection. -
Citations
Citations to this article as recorded by- A molecular reappraisal of quilty lesions: Insights from tissue and circulating biomarkers in heart transplantation
Andrea Fernandez Valledor, Cathrine M. Moeller, Adi Hertz, Daniel Oren, Ilan Richter, Boaz Elad, Julia Baranowska, Salwa Rahman, Carolyn Hennecken, Afsana Rahman, Dor Lotan, David Bae, Adil Yunis, Justin A. Fried, Ersilia M. DeFilippis, David T. Majure, J
The Journal of Heart and Lung Transplantation.2026;[Epub] CrossRef - The roles of tertiary lymphoid structures in orchestrating immune responses in peripheral organs
Keisuke Taniguchi, Takahisa Yoshikawa, Motoko Yanagita
Inflammation and Regeneration.2025;[Epub] CrossRef - The human myocardium harbors a population of naive B-cells with a distinctive gene expression signature conserved across species
Kevin C. Bermea, Nicolas Kostelecky, Sylvie T. Rousseau, Chieh-Yu Lin, Luigi Adamo
Frontiers in Immunology.2022;[Epub] CrossRef - Examination of tracheal allografts after long-term survival in dogs
Tao Lu, Yiwei Huang, Yulei Qiao, Yongxing Zhang, Yu Liu
European Journal of Cardio-Thoracic Surgery.2021; 59(1): 155. CrossRef - Essentials in the diagnosis of postoperative myocardial lesions similar to or unrelated to rejection in heart transplant
Costel Dumitru, Ancuta Zazgyva, Adriana Habor, Ovidiu Cotoi, Horațiu Suciu, Carmen Cotrutz, Bogdan Grecu, Ileana Anca Sin
Revista Romana de Medicina de Laborator.2021; 29(3): 307. CrossRef - Clinical outcome of donor heart with prolonged cold ischemic time: A single‐center study
Fazal Shafiq, Yixuan Wang, Geng Li, Zongtao Liu, Fei Li, Ying Zhou, Li Xu, Xingjian Hu, Nianguo Dong
Journal of Cardiac Surgery.2020; 35(2): 397. CrossRef - The XVth Banff Conference on Allograft Pathology the Banff Workshop Heart Report: Improving the diagnostic yield from endomyocardial biopsies and Quilty effect revisited
Jean-Paul Duong Van Huyen, Marny Fedrigo, Gregory A. Fishbein, Ornella Leone, Desley Neil, Charles Marboe, Eliot Peyster, Jan von der Thüsen, Alexandre Loupy, Michael Mengel, Monica P. Revelo, Benjamin Adam, Patrick Bruneval, Annalisa Angelini, Dylan V. M
American Journal of Transplantation.2020; 20(12): 3308. CrossRef
- A molecular reappraisal of quilty lesions: Insights from tissue and circulating biomarkers in heart transplantation
- C-reactive Protein Overexpression in the Background Liver of Hepatitis B Virus–Associated Hepatocellular Carcinoma Is a Prognostic Biomarker
- Jin Ho Shin, Eunsil Yu, Eun Na Kim, Chong Jai Kim
- J Pathol Transl Med. 2018;52(5):267-274. Published online July 27, 2018
- DOI: https://doi.org/10.4132/jptm.2018.07.14
- 9,240 View
- 181 Download
- 8 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Chronic hepatitis B virus (HBV) infection is a leading cause of hepatocellular carcinoma (HCC). Peripheral blood C-reactive protein (CRP) concentration and CRP overexpression in HCC cells are proven to be prognostic markers for HCC, but the significance of CRP expression in non-neoplastic hepatocytes, which are the primary origin of CRP, has not been studied. This study was conducted to determine the clinicopathologic significance of CRP immunoreactivity in the background liver of HBV-associated HCC.
Methods
CRP immunostaining was done on tissue microarrays of non-neoplastic liver tissues obtained from surgically resected, treatment-naïve HBV-associated HCCs (n = 156). The relationship between CRP immunoreactivity and other clinicopathologic parameters including cancer-specific survival was analyzed. CRP immunoreactivity was determined using a 4-tier grading system: grades 0, 1, 2, and 3.
Results
CRP was positive in 139 of 156 cases (89.1%) of non-neoplastic liver in patients with HCCs: grade 1 in 83 cases (53.2%); grade 2 in 50 cases (32.1%); and grade 3 in six cases (3.8%). The patients with diffuse CRP immunoreactivity (grade 3) had decreased cancer-specific survival (p = .031) and a tendency for shorter interval before early recurrence (p = .050). The degree of CRP immunoreactivity correlated with serum CRP concentration (p < .001).
Conclusions
CRP immunoreactivity in non-neoplastic liver is a novel biomarker for poor cancer-specific survival of HBV-associated HCC and correlates with serum CRP concentration. -
Citations
Citations to this article as recorded by- Preoperative Inflammatory Markers as Predictors of Post-ERCP Pancreatitis: A Retrospective Cohort Study
Mehmet Fuat Çetin, Mehmet Emin Gönüllü, Erman Yekenkurul, Fatih Gürsoy, Serkan Torun
Digestive Diseases and Sciences.2026;[Epub] CrossRef - Plasma thrombomodulin is a valuable biomarker to predict the severity of hemorrhagic fever with renal syndrome caused by the Hantaan virus
Han-Dong Zhao, Yan Zhang, Xiao-Hong Wang, Hong-Bo Qian, Tong-Bo Yu, Peng Li, Kang-Xiao Ma, Hong-Li Liu
Frontiers in Cellular and Infection Microbiology.2025;[Epub] CrossRef - Multivariate Assessment of Thyroid, Lipid, and Inflammatory Profiles by HBV Status and Viral Load: Age- and Sex-Specific Findings
Hyeokjun Yun, Jong Wan Kim, Jae Kyung Kim
Viruses.2025; 17(9): 1208. CrossRef - Analysis of Inflammatory and Thyroid Hormone Levels Based on Hepatitis A and B Virus Immunity Status: Age and Sex Stratification
Hyeokjun Yun, Jae-Sik Jeon, Jae Kyung Kim
Viruses.2024; 16(8): 1329. CrossRef - Ferritin and procalcitonin serve as discriminative inflammatory biomarkers and can predict the prognosis of severe fever with thrombocytopenia syndrome in its early stages
Keping Chen, Huidi Sun, Yu Geng, Chuankun Yang, Chun Shan, Yuxin Chen
Frontiers in Microbiology.2023;[Epub] CrossRef - Evaluation of Serum Ferritin, Procalcitonin, and C-Reactive Protein for the Prediction of Severity and Mortality in Hemorrhagic Fever With Renal Syndrome
Lihe Che, Zedong Wang, Na Du, Liang Li, Yinghua Zhao, Kaiyu Zhang, Quan Liu
Frontiers in Microbiology.2022;[Epub] CrossRef - Hepatocellular adenomas: recent updates
Haeryoung Kim, Young Nyun Park
Journal of Pathology and Translational Medicine.2021; 55(3): 171. CrossRef - A prospective follow-up study of the relationship between high-sensitivity C-reactive protein and primary liver cancer
Sarah Tan Siyin, Tong Liu, Wenqiang Li, Nan Yao, Guoshuai Xu, Jun Qu, Yajun Chen
BMC Cancer.2020;[Epub] CrossRef - CRP Levels in Viral Hepatitis: A Meta-Analysis Study
Sukhpal Singh, Abhishek Bansal, Pardeep Kumar
International Journal of Infection.2020;[Epub] CrossRef
- Preoperative Inflammatory Markers as Predictors of Post-ERCP Pancreatitis: A Retrospective Cohort Study
- Combined Hepatocellular Carcinoma and Neuroendocrine Carcinoma with Ectopic Secretion of Parathyroid Hormone: A Case Report and Review of the Literature
- Hyun Jung Kwon, Ji-Won Kim, Haeryoung Kim, YoungRok Choi, Soomin Ahn
- J Pathol Transl Med. 2018;52(4):232-237. Published online May 25, 2018
- DOI: https://doi.org/10.4132/jptm.2018.05.17
- 9,057 View
- 159 Download
- 17 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF - Primary combined hepatocellular carcinoma (HCC) and neuroendocrine carcinoma is a rare entity, and so is hypercalcemia due to ectopic parathyroid hormone (PTH) secretion by tumor. A 44-year old man with hepatitis B virus associated chronic liver disease presented with a hepatic mass. Hemihepatectomy discovered the mass as combined HCC and poorly differentiated cholangiocarcinoma. During adjuvant chemoradiation therapy, he presented with nausea, and multiple systemic metastases were found. Laboratory tests revealed hypercalcemia with markedly elevated PTH and neuron specific enolase. Parathyroid scan showed normal uptake in parathyroid glands, suggestive of ectopic PTH secretion. Subsequently, immunohistochemistry of neuroendocrine marker was performed on the primary lesion, and confirmed the neuroendocrine differentiation in non-HCC component. The patient died 71 days after surgery. This report may suggest the possibility of ectopic PTH secretion by neuroendocrine carcinoma of hepatic origin causing hypercalcemia. Caution for neuroendocrine differentiation should be exercised when diagnosing poorly differentiated HCC.
-
Citations
Citations to this article as recorded by- Mixed glandular neuroendocrine carcinoma of the endometrium with hypercalcemic crisis
Mei Luo, Xiaoxia Yu, Zhongpei Chen, Zhenhan Li
The American Journal of the Medical Sciences.2025; 369(2): 281. CrossRef - Combined Neuroendocrine Carcinoma and Hepatocellular Carcinoma of the Liver: Systematic Literature Review Suggests Implementing Biological Characterization to Optimize Therapeutic Strategy
Daniela Sambataro, Sandro Bellavia, Paolo Di Mattia, Danilo Centonze, Carmela Emmanuele, Annalisa Bonasera, Giuseppe Caputo, Andrea Maria Onofrio Quattrocchi, Ernesto Vinci, Vittorio Gebbia, Maria Rosaria Valerio
Cancers.2025; 17(7): 1074. CrossRef - Surgical Resection of Primary Hepatic Mixed Neuroendocrine-Non-Neuroendocrine Neoplasm: A Report of Three Cases
Ryosuke Toyonaka, Osamu Aramaki, Nao Yoshida, Yusuke Mitsuka, Masanori Nakamura, Shu Inagaki, Kaiki Murai, Toshiyuki Ishige, Ryusuke Tsujimura, Sumie Ohni, Shinobu Masuda, Hiroharu Yamashita, Yukiyasu Okamura
The Japanese Journal of Gastroenterological Surgery.2025; 58(6): 331. CrossRef - Case report: mixed large-cell neuroendocrine and hepatocellular carcinoma of the liver
Xin Gao, Heng Wang, Zheyu Niu, Meng Liu, Xiaohan Kong, Hongrui Sun, Chaoqun Ma, Huaqiang Zhu, Jun Lu, Xu Zhou
Frontiers in Oncology.2024;[Epub] CrossRef - Mixed Primary Hepatocellular Carcinoma and Hepatic Neuroendocrine Carcinoma: Case Report and Literature Review
Woo Young Shin, Keon Young Lee, Kyeong Deok Kim
Medicina.2023; 59(2): 418. CrossRef - Comparison of Metastatic Patterns Among Neuroendocrine Tumors, Neuroendocrine Carcinomas, and Nonneuroendocrine Carcinomas of Various Primary Organs
Hyung Kyu Park, Ghee Young Kwon
Journal of Korean Medical Science.2023;[Epub] CrossRef - Immunohistochemical characterization of a steroid-secreting oncocytic adrenal carcinoma responsible for paraneoplastic hyperparathyroidism
Magalie Haissaguerre, Estelle Louiset, Christofer C Juhlin, Adam Stenman, Christophe Laurent, Hélène Trouette, Hervé Lefebvre, Antoine Tabarin
European Journal of Endocrinology.2023; 188(4): K11. CrossRef - Neuroendocrine neoplasms of the biliary tree, liver and pancreas: a pathological approach
Claudio Luchini, Giuseppe Pelosi, Aldo Scarpa, Paola Mattiolo, Deborah Marchiori, Roberta Maragliano, Fausto Sessa, Silvia Uccella
Pathologica.2021; 113(1): 28. CrossRef - Contrast-Enhanced Ultrasound Findings of Hepatocellular Carcinoma With Neuroendocrine Carcinoma: A Case Report
Hong Wang, Dan Yang, Zhenru Wu, Yan Luo, Wenwu Ling
Frontiers in Medicine.2021;[Epub] CrossRef - Combined primary hepatic neuroendocrine carcinoma and hepatocellular carcinoma: case report and literature review
Akira Nakano, Kenichi Hirabayashi, Hiroshi Yamamuro, Taro Mashiko, Yoshihito Masuoka, Seiichiro Yamamoto, Soji Ozawa, Toshio Nakagohri
World Journal of Surgical Oncology.2021;[Epub] CrossRef - Hepatocellular carcinoma in patients with renal dysfunction: Pathophysiology, prognosis, and treatment challenges
Hsuan Yeh, Chung-Cheng Chiang, Tzung-Hai Yen
World Journal of Gastroenterology.2021; 27(26): 4104. CrossRef - Severe hypercalcaemia from ectopic intact parathyroid hormone secretion treated with continuous renal replacement therapy in a patient with two malignancies
Nathaniel Hocker, Maria Story, Alysa Lerud, Sarat Kuppachi
BMJ Case Reports.2021; 14(6): e242172. CrossRef - Parathyroid Carcinoma and Ectopic Secretion of Parathyroid hormone
Filomena Cetani, Elena Pardi, Claudio Marcocci
Endocrinology and Metabolism Clinics of North America.2021; 50(4): 683. CrossRef - Primary hepatic neuroendocrine cancer coexisted with hepatocellular carcinoma: a case report
Chikara Ebisutani, Seitetsu Yoon, Toshiki Hyodo, Takafumi Watanabe, Hirofumi Okada, Yutaka Shirakawa, Yoshio Sakamoto, Shigeya Hirohata
Kanzo.2020; 61(3): 122. CrossRef - Two-in-one: A pooled analysis of primary hepatic neuroendocrine carcinoma combined/collided with hepatocellular carcinoma
Jia-Xi Mao, Fei Teng, Ke-Yan Sun, Cong Liu, Guo-Shan Ding, Wen-Yuan Guo
Hepatobiliary & Pancreatic Diseases International.2020; 19(4): 399. CrossRef - Primary hepatic neuroendocrine carcinoma coexisting with distal cholangiocarcinoma
Qi Xin, Rong Lv, Cheng Lou, Zhe Ma, Gui-Qiu Liu, Qin Zhang, Hai-Bo Yu, Chuan-Shan Zhang
Medicine.2020; 99(26): e20854. CrossRef - Mixed hepatocellular carcinoma-neuroendocrine carcinoma—A diagnostic and therapeutic challenge
Nusrat Jahan, Irfan Warraich, Edwin Onkendi, Sanjay Awasthi
Current Problems in Cancer: Case Reports.2020; 1: 100020. CrossRef
- Mixed glandular neuroendocrine carcinoma of the endometrium with hypercalcemic crisis
- Extracellular Vesicles and the Promise of Continuous Liquid Biopsies
- Don Armstrong, Derek E. Wildman
- J Pathol Transl Med. 2018;52(1):1-8. Published online January 15, 2018
- DOI: https://doi.org/10.4132/jptm.2017.05.21
- 19,366 View
- 339 Download
- 72 Web of Science
- 68 Crossref
-
 Abstract
Abstract
 PDF
PDF - The rapid and accurate diagnosis of patients with minimally invasive procedures was once only found in science fiction. However, the discovery of extracellular vesicles (EVs) and their near ubiquity in body fluids, coupled with the advent of inexpensive next generation sequencing techniques and EV purification protocols, promises to make science fiction a reality. Purifying and sequencing the RNA content of EV from routine blood draws and urine samples are likely to enable pathologists and physicians to diagnose and track the progress of diseases in many inaccessible tissues in the near future. Here we present the evolutionary background of EV, summarize the biology of EV formation and cargo selection, and discuss the current barriers to making continuous liquid biopsies through the use of EV a science reality.
-
Citations
Citations to this article as recorded by-
Blood-derived APLP1
+
extracellular vesicles are potential biomarkers for the early diagnosis of brain diseases
Yuri Choi, Jae Hyun Park, Ala Jo, Chul-Woo Lim, Ji-Min Park, Jin Woo Hwang, Kang Soo Lee, Young-Sang Kim, Hakho Lee, Jisook Moon
Science Advances.2025;[Epub] CrossRef - The Role of Nanotechnology in Understanding the Pathophysiology of Traumatic Brain Injury
Saranya Selvaraj, Laksiri Weerasinghe
Central Nervous System Agents in Medicinal Chemistry.2025; 25(1): 20. CrossRef - Extracellular Vesicles Released From Skeletal Muscle Post‐Chronic Contractile Activity Increase Mitochondrial Biogenesis in Recipient Myoblasts
Patience O. Obi, Tamiris F. G. Souza, Berkay Özerkliğ, Samira Seif, Benjamin Bydak, Nicholas Klassen, Todd A. Duhamel, Adrian R. West, Joseph W. Gordon, Ayesha Saleem
Journal of Extracellular Vesicles.2025;[Epub] CrossRef - The Role of Extracellular Vesicles in Brain‐Peripheral Communication Following Ischemic Stroke: Implications for Neural Repair and Regeneration
Victória Linden de Rezende, Khiany Mathias, Maiara de Aguiar da Costa, Cinara Ludvig Gonçalves, Tatiana Barichello, Fabricia Petronilho
Journal of Neurochemistry.2025;[Epub] CrossRef - Exosomal Non-Coding RNAs as Potential Biomarkers for Alzheimer’s Disease: Advances and Perspectives in Translational Research
Simoneide Souza Titze-de-Almeida, Clara Luna Marina, Milena Vieira Ramos, Letícia Dias dos Santos Silva, Pedro Renato de Paula Brandão, Diógenes Diego de Carvalho Bispo, Felipe Von Glehn, Ricardo Titze-de-Almeida
International Journal of Molecular Sciences.2025; 26(17): 8246. CrossRef - Exploring the Spatial Limits of Extracellular Vesicles‐Mediated Intercellular Communication
Federico Colombo, Kartik Nimkar, Erienne Grace Norton, Francesca Lovat, Emanuele Cocucci
Journal of Extracellular Vesicles.2025;[Epub] CrossRef - Extracellular vesicles decoying across host immunity
Jorge J Canas, Samantha M Enslow, Saloni Bhimani, Mariola J Ferraro
Journal of Leukocyte Biology.2025;[Epub] CrossRef - Extracellular Vesicles as Delivery Vehicles for Non-Coding RNAs: Potential Biomarkers for Chronic Liver Diseases
Arianna Ferro, Gabriele Saccu, Simone Mattivi, Andrea Gaido, Maria Beatriz Herrera Sanchez, Shafiul Haque, Lorenzo Silengo, Fiorella Altruda, Marilena Durazzo, Sharmila Fagoonee
Biomolecules.2024; 14(3): 277. CrossRef - From understanding to action: Exploring molecular connections of Down syndrome to Alzheimer's disease for targeted therapeutic approach
Sonal Sukreet, Michael S. Rafii, Robert A. Rissman
Alzheimer's & Dementia: Diagnosis, Assessment & Disease Monitoring.2024;[Epub] CrossRef - Extracellular vesicles and cancer stem cells: a deadly duo in tumor progression
Akram Tayanloo-Beik, Azin Eslami, Masoumeh Sarvari, Hasan Jalaeikhoo, Mohsen Rajaeinejad, Mohsen Nikandish, Ali Faridfar, Mostafa Rezaei-Tavirani, Ahmad Rezazadeh Mafi, Bagher Larijani, Babak Arjmand
Oncology Reviews.2024;[Epub] CrossRef - Tumor-Derived Extracellular Vesicles as Liquid Biopsy for Diagnosis and Prognosis of Solid Tumors: Their Clinical Utility and Reliability as Tumor Biomarkers
Prerna Dabral, Nobel Bhasin, Manish Ranjan, Maysoon M. Makhlouf, Zakaria Y. Abd Elmageed
Cancers.2024; 16(13): 2462. CrossRef - miR-182, miR-221 and miR-222 are potential urinary extracellular vesicle biomarkers for canine urothelial carcinoma
Jenni Karttunen, Lajos Kalmar, Andrew Grant, Jun Ying, Sarah E. Stewart, Xiaonan Wang, Fiona Karet Frankl, Tim Williams
Scientific Reports.2024;[Epub] CrossRef - Urine Extracellular Vesicles Size Subsets as Lupus Nephritis Biomarkers
Itze C. Navarro-Hernandez, Raúl F. Reyes-Huerta, Mariana Cañez-Hernández, Jiram Torres-Ruiz, Daniel A. Carrillo-Vázquez, Laura P. Whittall-García, David E. Meza-Sánchez, Guillermo Juárez-Vega, Diana Gómez-Martin, José M. Hernández-Hernández, José L. Marav
Diagnostics.2024; 14(20): 2271. CrossRef - Emerging insights in senescence: pathways from preclinical models to therapeutic innovations
Luke Mansfield, Valentina Ramponi, Kavya Gupta, Thomas Stevenson, Abraham Binoy Mathew, Agian Jeffilano Barinda, Florencia Herbstein, Samir Morsli
npj Aging.2024;[Epub] CrossRef - Autologous Platelet and Extracellular Vesicle-Rich Plasma as Therapeutic Fluid: A Review
Kaja Troha, Domen Vozel, Matevž Arko, Apolonija Bedina Zavec, Drago Dolinar, Matej Hočevar, Zala Jan, Matic Kisovec, Boštjan Kocjančič, Ljubiša Pađen, Manca Pajnič, Samo Penič, Anna Romolo, Neža Repar, Vesna Spasovski, Nejc Steiner, Vid Šuštar, Aleš Iglič
International Journal of Molecular Sciences.2023; 24(4): 3420. CrossRef - Liquid Biopsies, Novel Approaches and Future Directions
Athanasios Armakolas, Maria Kotsari, John Koskinas
Cancers.2023; 15(5): 1579. CrossRef - Proteomic Signature of Extracellular Vesicles Associated with Colorectal Cancer
Natalia Soloveva, Svetlana Novikova, Tatiana Farafonova, Olga Tikhonova, Victor Zgoda
Molecules.2023; 28(10): 4227. CrossRef - Engineering extracellular vesicles for Alzheimer's disease: An emerging cell‐free approach for earlier diagnosis and treatment
Sabrina Valentina Lazar, Sirjan Mor, David Wang, Leora Goldbloom‐Helzner, Kaitlin Clark, Dake Hao, Diana Lee Farmer, Aijun Wang
WIREs Mechanisms of Disease.2022;[Epub] CrossRef - Engineered exosomes as a natural nanoplatform for cancer targeted delivery of metal-based drugs
Tao Feng, Johannes Karges, Xinxing Liao, Liangnian Ji, Hui Chao
Coordination Chemistry Reviews.2022; 454: 214325. CrossRef - Storage conditions determine the characteristics of red blood cell derived extracellular vesicles
Tímea Bebesi, Diána Kitka, Anikó Gaál, Imola Csilla Szigyártó, Róbert Deák, Tamás Beke-Somfai, Kitti Koprivanacz, Tünde Juhász, Attila Bóta, Zoltán Varga, Judith Mihály
Scientific Reports.2022;[Epub] CrossRef - Novel Exosome Biomarker Candidates for Alzheimer’s Disease Unravelled Through Mass Spectrometry Analysis
Tânia Soares Martins, Rui Marçalo, Cristóvão B. da Cruz e Silva, Dário Trindade, José Catita, Francisco Amado, Tânia Melo, Ilka Martins Rosa, Jonathan Vogelgsang, Jens Wiltfang, Odete A. B. da Cruz e Silva, Ana Gabriela Henriques
Molecular Neurobiology.2022; 59(5): 2838. CrossRef - Saliva Based Liquid Biopsies in Head and Neck Cancer: How Far Are We From the Clinic?
Aditi Patel, Shanaya Patel, Parina Patel, Vivek Tanavde
Frontiers in Oncology.2022;[Epub] CrossRef - Incidental Detection of Maternal Malignancy by Fetal Cell-Free DNA Screening
Britton D. Rink, Blair K. Stevens, Mary E. Norton
Obstetrics & Gynecology.2022; 140(1): 121. CrossRef - Investigating the consistency of extracellular vesicle production from breast cancer subtypes using CELLine adherent bioreactors
Colin L. Hisey, Anastasiia Artuyants, George Guo, Vanessa Chang, Gabrielle Reshef, Martin Middleditch, Bincy Jacob, Lawrence W. Chamley, Cherie Blenkiron
Journal of Extracellular Biology.2022;[Epub] CrossRef - Diagnostic and therapeutic potential of exosomes in Alzheimer’s disease
Tânia Soares Martins, Dário Trindade, Margarida Vaz, Inês Campelo, Martim Almeida, Guilherme Trigo, Odete A. B. da Cruz e Silva, Ana Gabriela Henriques
Journal of Neurochemistry.2021; 156(2): 162. CrossRef - Composition of the whole transcriptome in the human plasma: Cellular source and modification by aging
Tapio Nevalainen, Arttu Autio, Maija Puhka, Marja Jylhä, Mikko Hurme
Experimental Gerontology.2021; 143: 111119. CrossRef - Extracellular vesicles in cancer diagnostics and therapeutics
Adeeb Shehzad, Salman Ul Islam, Raheem Shahzad, Salman Khan, Young Sup Lee
Pharmacology & Therapeutics.2021; 223: 107806. CrossRef - Elevated complement mediator levels in endothelial-derived plasma exosomes implicate endothelial innate inflammation in diminished brain function of aging humans
Fanny M. Elahi, Danielle Harvey, Marie Altendahl, Nivetha Brathaban, Nicole Fernandes, Kaitlin B. Casaletto, Adam M. Staffaroni, Pauline Maillard, Jason D. Hinman, Bruce L. Miller, Charles DeCarli, Joel H. Kramer, Edward J. Goetzl
Scientific Reports.2021;[Epub] CrossRef - Extracellular Vesicles as Mediators of Cancer Disease and as Nanosystems in Theranostic Applications
Renato Burgos-Ravanal, América Campos, Magda C. Díaz-Vesga, María Fernanda González, Daniela León, Lorena Lobos-González, Lisette Leyton, Marcelo J. Kogan, Andrew F. G. Quest
Cancers.2021; 13(13): 3324. CrossRef - Extracellular Vesicles as Biomarkers and Therapeutic Tools: From Pre-Clinical to Clinical Applications
Maria Chiara Ciferri, Rodolfo Quarto, Roberta Tasso
Biology.2021; 10(5): 359. CrossRef - Unsupervised Machine Learning‐Based Clustering of Nanosized Fluorescent Extracellular Vesicles
Sören Kuypers, Nick Smisdom, Isabel Pintelon, Jean‐Pierre Timmermans, Marcel Ameloot, Luc Michiels, Jelle Hendrix, Baharak Hosseinkhani
Small.2021;[Epub] CrossRef - A multiparametric extraction method for Vn96-isolated plasma extracellular vesicles and cell-free DNA that enables multi-omic profiling
Jeremy W. Roy, Catherine A. Taylor, Annie P. Beauregard, Surendar R. Dhadi, D. Craig Ayre, Sheena Fry, Simi Chacko, Gabriel Wajnberg, Andrew P. Joy, Ngoc-Nu Mai-Thi, Nicolas Crapoulet, David A. Barnett, Anirban Ghosh, Stephen M. Lewis, Rodney J. Ouellette
Scientific Reports.2021;[Epub] CrossRef - The distinct roles of exosomes in tumor-stroma crosstalk within gastric tumor microenvironment
Hanyu Zhang, Min Yang, Xu Wu, Qianxiu Li, Xin Li, Yueshui Zhao, Fukuan Du, Yu Chen, Zhigui Wu, Zhangang Xiao, Jing Shen, Qinglian Wen, Wei Hu, Chi Hin Cho, Meijuan Chen, Yejiang Zhou, Mingxing Li
Pharmacological Research.2021; 171: 105785. CrossRef - Exosomes in Alzheimer’s Disease: From Being Pathological Players to Potential Diagnostics and Therapeutics
Hagar M. Soliman, Ghada A. Ghonaim, Shaza M. Gharib, Hitesh Chopra, Aya K. Farag, Mohamed H. Hassanin, Abdalrazeq Nagah, Mahmoud Emad-Eldin, Nevertary E. Hashem, Galal Yahya, Sherif E. Emam, Abdalla E. A. Hassan, Mohamed S. Attia
International Journal of Molecular Sciences.2021; 22(19): 10794. CrossRef - Mitochondrial Quality Control in Cardiac-Conditioning Strategies against Ischemia-Reperfusion Injury
Wylly Ramsés García-Niño, Cecilia Zazueta, Mabel Buelna-Chontal, Alejandro Silva-Palacios
Life.2021; 11(11): 1123. CrossRef - Proteomic Profiling of Exosomes Derived from Plasma of HIV-Infected Alcohol Drinkers and Cigarette Smokers
Sunitha Kodidela, Yujie Wang, Benjamin J. Patters, Yuqing Gong, Namita Sinha, Sabina Ranjit, Kelli Gerth, Sanjana Haque, Theodore Cory, Carole McArthur, Anil Kumar, Jim Y. Wan, Santosh Kumar
Journal of Neuroimmune Pharmacology.2020; 15(3): 501. CrossRef - Promising Applications of AIEgens in Animal Models
Bairong He, Bo Situ, Zujin Zhao, Lei Zheng
Small Methods.2020;[Epub] CrossRef - Extracellular Vesicles Derived Human-miRNAs Modulate the Immune System in Type 1 Diabetes
Tine Tesovnik, Jernej Kovač, Katka Pohar, Samo Hudoklin, Klemen Dovč, Nataša Bratina, Katarina Trebušak Podkrajšek, Maruša Debeljak, Peter Veranič, Emanuele Bosi, Lorenzo Piemonti, Alojz Ihan, Tadej Battelino
Frontiers in Cell and Developmental Biology.2020;[Epub] CrossRef - The Role of Extracellular Vesicles in the Hallmarks of Cancer and Drug Resistance
Cristina P. R. Xavier, Hugo R. Caires, Mélanie A. G. Barbosa, Rui Bergantim, José E. Guimarães, M. Helena Vasconcelos
Cells.2020; 9(5): 1141. CrossRef - Connexin-46 Contained in Extracellular Vesicles Enhance Malignancy Features in Breast Cancer Cells
Rodrigo A. Acuña, Manuel Varas-Godoy, Viviana M. Berthoud, Ivan E. Alfaro, Mauricio A. Retamal
Biomolecules.2020; 10(5): 676. CrossRef - Mentalexo approach for diagnosis of psychiatric disorders
Ahmet Topuzoğlu, Can Ilgın
Medical Hypotheses.2020; 143: 109823. CrossRef - Reagent-free total protein quantification of intact extracellular vesicles by attenuated total reflection Fourier transform infrared (ATR-FTIR) spectroscopy
Veronika Szentirmai, András Wacha, Csaba Németh, Diána Kitka, Anita Rácz, Károly Héberger, Judith Mihály, Zoltán Varga
Analytical and Bioanalytical Chemistry.2020; 412(19): 4619. CrossRef - Urinary Biomarkers in Bladder Cancer: Where Do We Stand and Potential Role of Extracellular Vesicles
Manuel Castanheira de Oliveira, Hugo R. Caires, Maria J. Oliveira, Avelino Fraga, M. Helena Vasconcelos, Ricardo Ribeiro
Cancers.2020; 12(6): 1400. CrossRef - (Sub)populations of extracellular vesicles released by TNF‐α –triggered human endothelial cells promote vascular inflammation and monocyte migration
Baharak Hosseinkhani, Nynke M.S. van den Akker, Daniel G.M. Molin, Luc Michiels
Journal of Extracellular Vesicles.2020;[Epub] CrossRef - Liquid biopsy using extracellular vesicle–derived DNA in lung adenocarcinoma
In Ae Kim, Jae Young Hur, Hee Joung Kim, Seung Eun Lee, Wan Seop Kim, Kye Young Lee
Journal of Pathology and Translational Medicine.2020; 54(6): 453. CrossRef - Mitochondrial RNA in Alzheimer’s Disease Circulating Extracellular Vesicles
Kyoung Mi Kim, Qiong Meng, Olivia Perez de Acha, Maja Mustapic, Aiwu Cheng, Erden Eren, Gautam Kundu, Yulan Piao, Rachel Munk, William H. Wood, Supriyo De, Ji Heon Noh, Michael Delannoy, Lesley Cheng, Kotb Abdelmohsen, Dimitrios Kapogiannis, Myriam Gorosp
Frontiers in Cell and Developmental Biology.2020;[Epub] CrossRef - Challenges in Biomaterial-Based Drug Delivery Approach for the Treatment of Neurodegenerative Diseases: Opportunities for Extracellular Vesicles
Asit Kumar, Lina Zhou, Kaining Zhi, Babatunde Raji, Shelby Pernell, Erene Tadrous, Sunitha Kodidela, Anantha Nookala, Harry Kochat, Santosh Kumar
International Journal of Molecular Sciences.2020; 22(1): 138. CrossRef - Tumor-specific genetic aberrations in cell-free DNA of gastroesophageal cancer patients
Kristina Magaard Koldby, Michael Bau Mortensen, Sönke Detlefsen, Per Pfeiffer, Mads Thomassen, Torben A. Kruse
Journal of Gastroenterology.2019; 54(2): 108. CrossRef - Raman tweezers microspectroscopy of circa 100 nm extracellular vesicles
Sergei G. Kruglik, Félix Royo, Jean-Michel Guigner, Laura Palomo, Olivier Seksek, Pierre-Yves Turpin, Irène Tatischeff, Juan M. Falcón-Pérez
Nanoscale.2019; 11(4): 1661. CrossRef - Application of Extracellular Vesicles Proteomics to Cardiovascular Disease: Guidelines, Data Analysis, and Future Perspectives
Maria N. Barrachina, Beatriz Calderón‐Cruz, Lucía Fernandez‐Rocca, Ángel García
PROTEOMICS.2019;[Epub] CrossRef - Prognostic Role of S100A8 and S100A9 Protein Expressions in Non-small Cell Carcinoma of the Lung
Hyun Min Koh, Hyo Jung An, Gyung Hyuck Ko, Jeong Hee Lee, Jong Sil Lee, Dong Chul Kim, Jung Wook Yang, Min Hye Kim, Sung Hwan Kim, Kyung Nyeo Jeon, Gyeong-Won Lee, Se Min Jang, Dae Hyun Song
Journal of Pathology and Translational Medicine.2019; 53(1): 13. CrossRef - High-fidelity probing of the structure and heterogeneity of extracellular vesicles by resonance-enhanced atomic force microscopy infrared spectroscopy
Sally Yunsun Kim, Dipesh Khanal, Bill Kalionis, Wojciech Chrzanowski
Nature Protocols.2019; 14(2): 576. CrossRef - Liquid Biopsies in Cancer Diagnosis, Monitoring, and Prognosis
Gabriele De Rubis, Sabna Rajeev Krishnan, Mary Bebawy
Trends in Pharmacological Sciences.2019; 40(3): 172. CrossRef - Intercellular Vesicular Transfer by Exosomes, Microparticles and Oncosomes - Implications for Cancer Biology and Treatments
Ritu Jaiswal, Lisa M. Sedger
Frontiers in Oncology.2019;[Epub] CrossRef - Dictyostelium: A Model for Studying the Extracellular Vesicle Messengers Involved in Human Health and Disease
Irène Tatischeff
Cells.2019; 8(3): 225. CrossRef - Extracellular Vesicles as Diagnostics and Therapeutics for Structural Epilepsies
Jenni Karttunen, Mette Heiskanen, Anssi Lipponen, David Poulsen, Asla Pitkänen
International Journal of Molecular Sciences.2019; 20(6): 1259. CrossRef - Post-translational modification and protein sorting to small extracellular vesicles including exosomes by ubiquitin and UBLs
Hiroshi Ageta, Kunihiro Tsuchida
Cellular and Molecular Life Sciences.2019; 76(24): 4829. CrossRef - Exosome release and cargo in Down syndrome
Eric D. Hamlett, Angela LaRosa, Elliott J. Mufson, Juan Fortea, Aurélie Ledreux, Ann‐Charlotte Granholm
Developmental Neurobiology.2019; 79(7): 639. CrossRef - Exosomes in specific fractions of the boar ejaculate contain CD44: A marker for epididymosomes?
Manuel Alvarez-Rodriguez, Stefan A. Ljunggren, Helen Karlsson, Heriberto Rodriguez-Martinez
Theriogenology.2019; 140: 143. CrossRef - A review on protein markers of exosome from different bio-resources and the antibodies used for characterization
Fengyan Deng, Josh Miller
Journal of Histotechnology.2019; 42(4): 226. CrossRef - Tangential Flow Microfluidics for the Capture and Release of Nanoparticles and Extracellular Vesicles on Conventional and Ultrathin Membranes
Mehdi Dehghani, Kilean Lucas, Jonathan Flax, James McGrath, Thomas Gaborski
Advanced Materials Technologies.2019;[Epub] CrossRef - Lipidomic analysis of urinary exosomes from hereditary α‐tryptasemia patients and healthy volunteers
Sarah C. Glover, Mohammad‐Zaman Nouri, Kubra M. Tuna, Lybil B. Mendoza Alvarez, Lisa K. Ryan, James F. Shirley, Ying Tang, Nancy D. Denslow, Abdel A. Alli
FASEB BioAdvances.2019; 1(10): 624. CrossRef - Novel Epigenetic Biomarkers in Pregnancy-Related Disorders and Cancers
Valentina Karin-Kujundzic, Ida Marija Sola, Nina Predavec, Anamarija Potkonjak, Ema Somen, Pavao Mioc, Alan Serman, Semir Vranic, Ljiljana Serman
Cells.2019; 8(11): 1459. CrossRef - The Potential Clinical Implications of Circulating Tumor Cells and Circulating Tumor Microemboli in Gastric Cancer
Emne A. Abdallah, Alexcia C. Braun, Bianca C.T.C.P. Flores, Laís Senda, Ana Cláudia Urvanegia, Vinicius Calsavara, Victor Hugo Fonseca de Jesus, Maria Fernanda Arruda Almeida, Maria Dirlei Begnami, Felipe J.F. Coimbra, Wilson Luiz da Costa, Diana Noronha
The Oncologist.2019; 24(9): e854. CrossRef - Role of tumor‑derived extracellular vesicles in cancer progression and their clinical applications (Review)
Fuhao Qiao, Peng Pan, Jiaping Yan, Jing Sun, Yan Zong, Zhiyong Wu, Xiaoqin Lu, Na Chen, Rui Mi, Yongbin Ma, Yuan Ji
International Journal of Oncology.2019;[Epub] CrossRef - Circulating tumor DNA – Current state of play and future perspectives
Gabriele De Rubis, Sabna Rajeev Krishnan, Mary Bebawy
Pharmacological Research.2018; 136: 35. CrossRef - “Liquid Biopsy” of White Matter Hyperintensity in Functionally Normal Elders
Fanny M. Elahi, Kaitlin B. Casaletto, Marie Altendahl, Adam M. Staffaroni, Evan Fletcher, Teresa J. Filshtein, Maria M. Glymour, Bruce L. Miller, Jason D. Hinman, Charles DeCarli, Edward J. Goetzl, Joel H. Kramer
Frontiers in Aging Neuroscience.2018;[Epub] CrossRef - The role of exosomal transport of viral agents in persistent HIV pathogenesis
Benjamin J. Patters, Santosh Kumar
Retrovirology.2018;[Epub] CrossRef
-
Blood-derived APLP1
+
extracellular vesicles are potential biomarkers for the early diagnosis of brain diseases
- Hepatocellular Carcinoma Arising in a Huge Hepatocellular Adenoma with Bone Marrow Metaplasia
- Hyo Jeong Kang, Hui Jeong Jeong, So-Woon Kim, Eunsil Yu, Young-Joo Lee, So Yeon Kim, Jihun Kim
- J Pathol Transl Med. 2018;52(4):226-231. Published online December 27, 2017
- DOI: https://doi.org/10.4132/jptm.2017.11.12
- 9,079 View
- 152 Download
- 5 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF - Hepatocellular adenoma (HCA) is the most common type of benign liver tumor, and its major complication is malignant transformation to hepatocellular carcinoma (HCC). Here, we report a case of HCC arising in HCA with bone marrow metaplasia in a 24-year-old Korean woman who presented with abdominal discomfort. A huge liver mass was found on abdominal ultrasonography. She underwent surgical hepatic resection, and the resected specimen was entirely involved by a 20-cm-sized tumor. Histological review revealed a well differentiated HCC arising from inflammatory HCA with β-catenin nuclear positivity and bone marrow metaplasia that contained hematopoietic cells. This case was unique because malignant transformation, inflammatory type HCA, β-catenin nuclear staining, and bone marrow metaplasia were simultaneously observed. Additionally, it should be noted that a large HCA with β-catenin activation can undergo malignant transformation and should be surgically resected in a timely manner.
-
Citations
Citations to this article as recorded by- Adult Hepatocellular Carcinoma Coexisting with Extramedullary Hematopoiesis
Hirotsugu Noguchi, Michiyo Higashi, Ryo Desaki, Takashi Tasaki, Mari Kirishima, Ikumi Kitazono, Kazuhiro Tabata, Akihide Tanimoto
International Journal of Surgical Pathology.2022; 30(3): 339. CrossRef - Spontaneous Occurrence of Various Types of Hepatocellular Adenoma in the Livers of Metabolic Syndrome-Associated Steatohepatitis Model TSOD Mice
Wenhua Shao, Orgil Jargalsaikhan, Mayuko Ichimura-Shimizu, Qinyi Cai, Hirohisa Ogawa, Yuko Miyakami, Kengo Atsumi, Mitsuru Tomita, Mitsuko Sutoh, Shunji Toyohara, Ryoji Hokao, Yasusei Kudo, Takeshi Oya, Koichi Tsuneyama
International Journal of Molecular Sciences.2022; 23(19): 11923. CrossRef - Bilateral Diffuse Nodular Pulmonary Ossification Mimicking Metastatic Disease in a Patient with Fibrolamellar Hepatocellular Carcinoma
Pattamon Sutthatarn, Cara E. Morin, Jessica Gartrell, Wayne L. Furman, Max R. Langham, Teresa Santiago, Andrew J. Murphy
Children.2021; 8(3): 226. CrossRef - Malignant transformation of liver fatty acid binding protein-deficient hepatocellular adenomas: histopathologic spectrum of a rare phenomenon
Juan Putra, Linda D. Ferrell, Annette S.H. Gouw, Valerie Paradis, Arvind Rishi, Christine Sempoux, Charles Balabaud, Swan N. Thung, Paulette Bioulac-Sage
Modern Pathology.2020; 33(4): 665. CrossRef - Hepatocellular carcinoma arising from hepatic adenoma in a young woman
Haythem Yacoub, Hela Kchir, Dhouha Cherif, Hajer Hassine, Slim Haouet, Asma Ayari, Habiba Mizouni, Saber Mannai, Mohamed Tahar Khalfallah, Nadia Maamouri
Clinical Case Reports.2020; 8(9): 1659. CrossRef - Metanephric adenoma with osseous metaplasia and bone marrow elements
Alessandro Pietro Aldera, Jeff John, Dharshnee Chetty, Dhirendra Govender
Human Pathology: Case Reports.2019; 17: 200316. CrossRef
- Adult Hepatocellular Carcinoma Coexisting with Extramedullary Hematopoiesis
- The Clinicopathological and Prognostic Significance of the Gross Classification of Hepatocellular Carcinoma
- Yangkyu Lee, Hyunjin Park, Hyejung Lee, Jai Young Cho, Yoo-Seok Yoon, Young-Rok Choi, Ho-Seong Han, Eun Sun Jang, Jin-Wook Kim, Sook-Hyang Jeong, Soomin Ahn, Haeryoung Kim
- J Pathol Transl Med. 2018;52(2):85-92. Published online November 24, 2017
- DOI: https://doi.org/10.4132/jptm.2017.11.13
- 15,164 View
- 390 Download
- 27 Web of Science
- 24 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
We aimed to determine the clinicopathological significance of the gross classification of hepatocellular carcinoma (HCC) according to the Korean Liver Cancer Association (KLCA) guidelines.
Methods
A retrospective analysis was performed on 242 cases of consecutively resected solitary primary HCC between 2003 and 2012 at Seoul National University Bundang Hospital. The gross classification (vaguely nodular [VN], expanding nodular [EN], multinodular confluent [MC], nodular with perinodular extension [NP], and infiltrative [INF]) was reviewed for all cases, and were correlated with various clinicopathological features and the expression status of “stemness”-related (cytokeratin 19 [CK19], epithelial cell adhesion molecule [EpCAM]), and epithelial-mesenchymal transition (EMT)–related (urokinase plasminogen activator receptor [uPAR] and Ezrin) markers.
Results
Significant differences were seen in overall survival (p=.015) and disease-free survival (p = .034) according to the gross classification; INF type showed the worst prognosis while VN and EN types were more favorable. When the gross types were simplified into two groups, type 2 HCCs (MC/NP/INF) were more frequently larger and poorly differentiated, and showed more frequent microvascular and portal venous invasion, intratumoral fibrous stroma and higher pT stages compared to type 1 HCCs (EN/VN) (p<.05, all). CK19, EpCAM, uPAR, and ezrin expression was more frequently seen in type 2 HCCs (p<.05, all). Gross classification was an independent predictor of both overall and disease-free survival by multivariate analysis (overall survival: p=.030; hazard ratio, 4.118; 95% confidence interval, 1.142 to 14.844; disease-free survival: p=.016; hazard ratio, 1.617; 95% confidence interval, 1.092 to 2.394).
Conclusions
The gross classification of HCC had significant prognostic value and type 2 HCCs were associated with clinicopathological features of aggressive behavior, increased expression of “stemness”- and EMT-related markers, and decreased survival. -
Citations
Citations to this article as recorded by- Long-Term Outcomes of Transarterial Chemoembolization plus Ablation versus Surgical Resection in Patients with Large BCLC Stage A/B HCC
Ying-Wen Hou, Tian-Qi Zhang, Li-Di Ma, Yi-Quan Jiang, Xue Han, Tian Di, Lu Tang, Rong-Ping Guo, Min-Shan Chen, Jin-Xin Zhang, Zhi-Mei Huang, Jin-Hua Huang
Academic Radiology.2025; 32(7): 3960. CrossRef - Membranous Overexpression of Fibronectin Predicts Microvascular Invasion and Poor Survival Outcomes in Patients with Hepatocellular Carcinoma
Yoon Jung Hwang, Hyejung Lee, Suk Kyun Hong, Su Jong Yu, Haeryoung Kim
Gut and Liver.2025; 19(2): 275. CrossRef - Association between tumor morphology and efficacy of atezolizumab plus bevacizumab for advanced hepatocellular carcinoma
Nobuaki Ishihara, Shohei Komatsu, Keitaro Sofue, Eisuke Ueshima, Yoshihiko Yano, Yoshimi Fujishima, Jun Ishida, Masahiro Kido, Hidetoshi Gon, Kenji Fukushima, Takeshi Urade, Hiroaki Yanagimoto, Hirochika Toyama, Yoshihide Ueda, Yuzo Kodama, Takamichi Mura
Hepatology Research.2024; 54(8): 773. CrossRef - Macroscopic Characterization of Hepatocellular Carcinoma: An Underexploited Source of Prognostic Factors
Stéphanie Gonvers, Sebastiao Martins-Filho, André Hirayama, Julien Calderaro, Rebecca Phillips, Emilie Uldry, Nicolas Demartines, Emmanuel Melloul, Young Nyun Park, Valérie Paradis, Swan Thung, Venancio Alves, Christine Sempoux, Ismail Labgaa
Journal of Hepatocellular Carcinoma.2024; Volume 11: 707. CrossRef - Serum Total Superoxide Dismutase Activity as a Predictive Factor in Patients with Hepatocellular Carcinoma
Yanqiu Xu, Bin Liu, Shiqing Cheng, Junguo Zhang, Xiue Cao, Yong Wang, Fang Luan
Hepatitis Monthly.2024;[Epub] CrossRef - Diagnostic value of expressions of cancer stem cell markers for adverse outcomes of hepatocellular carcinoma and their associations with prognosis: A Bayesian network meta‑analysis
Zhengrong Ou, Shoushuo Fu, Jian Yi, Jingxuan Huang, Weidong Zhu
Oncology Letters.2024;[Epub] CrossRef - Recurrence of hepatocellular carcinoma in noncirrhotic patients with nonalcoholic fatty liver disease versus hepatitis B infection
Jungnam Lee, Jong-In Chang, Young-Joo Jin, Jeong-Hoon Lee, Ju Yeon Kim, Dong Hyun Sinn, Soon Sun Kim, Hyun Woong Lee, Sun Hong Yoo, Jung Hwan Yu, Jin-Woo Lee
European Journal of Gastroenterology & Hepatology.2023; 35(4): 431. CrossRef - Comprehensive investigating of MMR gene in hepatocellular carcinoma with chronic hepatitis B virus infection in Han Chinese population
Ning Ma, Ao Jin, Yitong Sun, Yiyao Jin, Yucheng Sun, Qian Xiao, XuanYi Sha, Fengxue Yu, Lei Yang, Wenxuan Liu, Xia Gao, Xiaolin Zhang, Lu Li
Frontiers in Oncology.2023;[Epub] CrossRef - LI-RADS Morphological Type Predicts Prognosis of Patients with Hepatocellular Carcinoma After Radical Resection
Chunhui Zhang, Rui Yang, Xinxin Wang, Yuqing Tao, Shuli Tang, Zhennan Tian, Yang Zhou
Annals of Surgical Oncology.2023; 30(8): 4876. CrossRef - From clinical variables to multiomics analysis: a margin morphology-based gross classification system for hepatocellular carcinoma stratification
Zhongqi Fan, Meishan Jin, Lei Zhang, Nanya Wang, Mingyue Li, Chuanlei Wang, Feng Wei, Ping Zhang, Xiaohong Du, Xiaodong Sun, Wei Qiu, Meng Wang, Hongbin Wang, Xiaoju Shi, Junfeng Ye, Chao Jiang, Jianpeng Zhou, Wengang Chai, Jun Qi, Ting Li, Ruoyan Zhang,
Gut.2023; 72(11): 2149. CrossRef - A clinical and pathological update on hepatocellular carcinoma
Salvatore Lorenzo Renne, Luca Di Tommaso
Journal of Liver Cancer.2022; 22(1): 14. CrossRef - An approach to grossing of hepatectomy specimens
Archana Rastogi
Indian Journal of Pathology and Microbiology.2021; 64(5): 121. CrossRef - Hepatocellular carcinoma: a clinical and pathological overview
Salvatore Lorenzo Renne, Samantha Sarcognato, Diana Sacchi, Maria Guido, Massimo Roncalli, Luigi Terracciano, Luca Di Tommaso
Pathologica.2021; 113(3): 203. CrossRef - The Clinicopathological Significance of YAP/TAZ Expression in Hepatocellular Carcinoma with Relation to Hypoxia and Stemness
Hyunjin Park, Yangkyu Lee, Kiryang Lee, Hyejung Lee, Jeong Eun Yoo, Soomin Ahn, Young Nyun Park, Haeryoung Kim
Pathology and Oncology Research.2021;[Epub] CrossRef - Adjuvant versus Neoadjuvant Immunotherapy for Hepatocellular Carcinoma: Clinical and Immunologic Perspectives
Yung-Yeh Su, Chia-Chen Li, Yih-Jyh Lin, Chiun Hsu
Seminars in Liver Disease.2021; 41(03): 263. CrossRef - Prognostic significance of viable tumor size measurement in hepatocellular carcinomas after preoperative locoregional treatment
Yoon Jung Hwang, Youngeun Lee, Hyunjin Park, Yangkyu Lee, Kyoungbun Lee, Haeryoung Kim
Journal of Pathology and Translational Medicine.2021; 55(5): 338. CrossRef - Survival according to recurrence patterns after resection for transplantable hepatocellular carcinoma in HBV endemic area: Appraisal of liver transplantation strategy
Chung Gyo Seo, Sun Young Yim, Soon Ho Um, Yoo Ra Lee, Yoo Jin Lee, Tae Hyung Kim, Hyun Gil Goh, Young Sun Lee, Sang Jun Suh, Na Yeon Han, Hyuk Soon Choi, Eun Sun Kim, Bora Keum, Yeon Seok Seo, Hyung Joon Yim, Ji Hoon Kim, Dong Sik Kim, Yoon Tae Jeen, Hoon
Clinics and Research in Hepatology and Gastroenterology.2020; 44(4): 532. CrossRef - A radiomics-based biomarker for cytokeratin 19 status of hepatocellular carcinoma with gadoxetic acid–enhanced MRI
Wentao Wang, Dongsheng Gu, Jingwei Wei, Ying Ding, Li Yang, Kai Zhu, Rongkui Luo, Sheng-Xiang Rao, Jie Tian, Mengsu Zeng
European Radiology.2020; 30(5): 3004. CrossRef Paeonol Inhibits Cell Proliferation, Migration and Invasion and Induces Apoptosis in Hepatocellular Carcinoma by Regulating miR-21-5p/KLF6 Axis
Miaoguo Cai, Wei Shao, Huijun Yu, Ye Hong, Lili Shi
Cancer Management and Research.2020; Volume 12: 5931. CrossRef- Update on Hepatocellular Carcinoma: a Brief Review from Pathologist Standpoint
Nese Karadag Soylu
Journal of Gastrointestinal Cancer.2020; 51(4): 1176. CrossRef - Clinico-Radio-Pathological and Molecular Features of Hepatocellular Carcinomas with Keratin 19 Expression
Hyungjin Rhee, Haeryoung Kim, Young Nyun Park
Liver Cancer.2020; 9(6): 663. CrossRef - Histopathological characteristics of needle core biopsy and surgical specimens from patients with solitary hepatocellular carcinoma or intrahepatic cholangiocarcinoma
Ju-Shan Wu, Ji-Liang Feng, Rui-Dong Zhu, San-Guang Liu, Da-Wei Zhao, Ning Li
World Journal of Gastrointestinal Oncology.2019; 11(5): 404. CrossRef - The strengths and weaknesses of gross and histopathological evaluation in hepatocellular carcinoma: a brief review
Sebastião N. Martins-Filho, Venâncio Avancini Ferreira Alves
Surgical and Experimental Pathology.2019;[Epub] CrossRef - Changing role of histopathology in the diagnosis and management of hepatocellular carcinoma
Archana Rastogi
World Journal of Gastroenterology.2018; 24(35): 4000. CrossRef
- Long-Term Outcomes of Transarterial Chemoembolization plus Ablation versus Surgical Resection in Patients with Large BCLC Stage A/B HCC
- Prognosis of Hepatocellular Carcinoma after Liver Transplantation: Comparative Analysis with Partial Hepatectomy
- Kyuho Lee, Kyoung-Bun Lee, Nam-Joon Yi, Kyung-Suk Suh, Ja-June Jang
- J Pathol Transl Med. 2017;51(1):79-86. Published online December 25, 2016
- DOI: https://doi.org/10.4132/jptm.2016.10.13
- 9,612 View
- 150 Download
- 6 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Liver transplantation (LT) is the treatment of choice for hepatocellular carcinoma (HCC). The aim of this study was to investigate the recurrence rate of HCC after LT and prognostic factors for recurrence by comparing LT with non-transplanted resection. Methods: The participants were 338 patients who underwent LT between 1996 and 2012 at Seoul National University Hospital (LT group) and 520 HCC patients who underwent partial hepatectomy between 1995 and 2006 (control group, non-LT group). Results: In the LT group, 68 of 338 patients (19.8%) showed relapse, and the recurrence rate was lower than that in the non-LT group (64.9%, 357/520, p < .001). Stratification analysis by American Joint Committee on Cancer (AJCC) stage showed that the stage I-II LT group had a lower recurrence rate than the non-LT group. Univariate comparative analysis demonstrated that multiplicity of tumor, tumor size, gross type, Edmondson- Steiner (ES) nuclear grade, extent of tumor, angioinvasion, AJCC stage, Milan criteria, University of California at San Francisco criteria on explant pathology (all p < .001), positive expression of cytokeratin 19 (p = .002), and preoperative α-fetoprotein (AFP) (p < .001) were predictors of tumor recurrence. In multivariate analysis, LT, preoperative AFP, multiplicity of tumor, extent of tumor, size of tumor, and ES nuclear grade were independent prognostic factors. Conclusions: LT might have a protective effect against the late recurrence of stage I-II HCC compared to non-LT, and the prognostic factors for recurrence were similar to previously well-known prognostic factors for HCC. -
Citations
Citations to this article as recorded by- Locoregional and Surgical Treatment of Single-Nodule Hepatocellular Carcinoma Recurrence After Liver Transplantation: A Systematic Review and a Meta-Analysis
Marco Maria Pascale, Camilla Marandola, Francesco Frongillo, Erida Nure, Salvatore Agnes
Cancers.2025; 17(9): 1501. CrossRef - Risk Factor Analysis of Death in Patients With Hepatic Cellular Carcinoma After Radical Operation: A Consecutive Cohort of 433 Patients
Zhengyang He, Wenfeng Lu, Dongze Qiu, Weimin She
Health Science Reports.2025;[Epub] CrossRef - Related Factors of Hepatocellular Carcinoma Recurrence Associated With Hyperglycemia After Liver Transplantation
Yujian Zheng, Qing Cai, Lishan Peng, Shibo Sun, Shaoping Wang, Jie Zhou
Transplantation Proceedings.2021; 53(1): 177. CrossRef - Oncological Outcomes of Hepatic Resection vs Transplantation for Localized Hepatocellular Carcinoma
A.T. Akcam, A.G. Saritas, A. Ulku, A. Rencuzogullari
Transplantation Proceedings.2019; 51(4): 1147. CrossRef - Clustering Asian Countries According to the Trend of liver cancer Mortality Rates: an Application of Growth Mixture Models
Maryam Salari, Anoshirvan Kazemnejad, Farid Zayeri
Iranian Red Crescent Medical Journal.2017;[Epub] CrossRef
- Locoregional and Surgical Treatment of Single-Nodule Hepatocellular Carcinoma Recurrence After Liver Transplantation: A Systematic Review and a Meta-Analysis
- SIRT7, H3K18ac, and ELK4 Immunohistochemical Expression in Hepatocellular Carcinoma
- Hye Seung Lee, Wonkyung Jung, Eunjung Lee, Hyeyoon Chang, Jin Hyuk Choi, Han Gyeom Kim, Aeree Kim, Baek-hui Kim
- J Pathol Transl Med. 2016;50(5):337-344. Published online August 5, 2016
- DOI: https://doi.org/10.4132/jptm.2016.05.20
- 12,470 View
- 168 Download
- 27 Web of Science
- 27 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
SIRT7 is one of the histone deacetylases and is NAD-dependent. It forms a complex with ETS-like transcription factor 4 (ELK4), which deacetylates H3K18ac and works as a transcriptional suppressor. Overexpression of SIRT7 and deacetylation of H3K18ac have been shown to be associated with aggressive clinical behavior in some cancers, including hepatocellular carcinoma (HCC). The present study investigated the immunohistochemical expression of SIRT7, H3K18ac, and ELK4 in hepatocellular carcinoma.
Methods
A total of 278 HCC patients were enrolled in this study. Tissue microarray blocks were made from existing paraffin-embedded blocks. Immunohistochemical expressions of SIRT7, H3K18ac and ELK4 were scored and analyzed.
Results
High SIRT7 (p = .034), high H3K18ac (p = .001), and low ELK4 (p = .021) groups were associated with poor outcomes. Age < 65 years (p = .028), tumor size ≥ 5 cm (p = .001), presence of vascular emboli (p = .003), involvement of surgical margin (p = .001), and high American Joint Committee on Cancer stage (III&V) (p < .001) were correlated with worse prognoses. In multivariate analysis, H3K18ac (p = .001) and ELK4 (p = .015) were the significant independent prognostic factors.
Conclusions
High SIRT7 expression with poor overall survival implies that deacetylation of H3K18ac contributes to progression of HCC. High H3K18ac expression with poor prognosis is predicted due to a compensation mechanism. In addition, high ELK4 expression with good prognosis suggests another role of ELK4 as a tumor suppressor beyond SIRT7’s helper. In conclusion, we could assume that the H3K18ac deacetylation pathway is influenced by many other factors. -
Citations
Citations to this article as recorded by- Combined single-cell RNA sequencing and mendelian randomization to identify biomarkers associated with necrotic apoptosis in intervertebral disc degeneration
Yi Ye, Lun Wan, Jiang Hu, Xiaoxue Li, Kun Zhang
The Spine Journal.2025; 25(1): 165. CrossRef - ETS-1 in tumor immunology: implications for novel anti-cancer strategies
SiYu Wang, Lei Wan, XiaoJun Zhang, HaoXiang Fang, MengYu Zhang, Feng Li, DaWei Yan
Frontiers in Immunology.2025;[Epub] CrossRef - Role of SIRT7 in Prostate Cancer Progression: New Insight Into Potential Therapeutic Target
Jiale Zhang, Chenxin Liu, Wenting Luo, Baoqing Sun
Cancer Medicine.2025;[Epub] CrossRef - SIRT7: the seventh key to unlocking the mystery of aging
Umar Raza, Xiaolong Tang, Zuojun Liu, Baohua Liu
Physiological Reviews.2024; 104(1): 253. CrossRef - The Significance of Modified Histone H3 in Epithelial Dysplasia and Oral Cancer
Woraphaluck Tachaveeraphong, Ekarat Phattarataratip
International Dental Journal.2024; 74(4): 769. CrossRef - Analysis of the Expression and Prognostic Value of SIRTs in Hepatocellular Carcinoma
Chuang Qin, Xiaofei Ye, Hongliang Luo, Hu Jin, Qiang Liu, Jiangfa Li
International Journal of General Medicine.2024; Volume 17: 2655. CrossRef - Role of Sirtuins in the Pathogenesis of Rheumatoid Arthritis
Agata Poniewierska-Baran, Oliwia Bochniak, Paulina Warias, Andrzej Pawlik
International Journal of Molecular Sciences.2023; 24(2): 1532. CrossRef - Role of sirtuins in hepatocellular carcinoma progression and multidrug resistance: Mechanistical and pharmacological perspectives
María Paula Ceballos, Ariel Darío Quiroga, Nicolás Francisco Palma
Biochemical Pharmacology.2023; 212: 115573. CrossRef - Substrates and Cyclic Peptide Inhibitors of the Oligonucleotide‐Activated Sirtuin 7**
Julie E. Bolding, Alexander L. Nielsen, Iben Jensen, Tobias N. Hansen, Line A. Ryberg, Samuel T. Jameson, Pernille Harris, Günther H. J. Peters, John M. Denu, Joseph M. Rogers, Christian A. Olsen
Angewandte Chemie International Edition.2023;[Epub] CrossRef - Substrates and Cyclic Peptide Inhibitors of the Oligonucleotide‐Activated Sirtuin 7**
Julie E. Bolding, Alexander L. Nielsen, Iben Jensen, Tobias N. Hansen, Line A. Ryberg, Samuel T. Jameson, Pernille Harris, Günther H. J. Peters, John M. Denu, Joseph M. Rogers, Christian A. Olsen
Angewandte Chemie.2023;[Epub] CrossRef - Epigenomic interplay in tumor heterogeneity: Potential of epidrugs as adjunct therapy
Suvasmita Rath, Diptesh Chakraborty, Jyotsnarani Pradhan, Mohammad Imran Khan, Jagneshwar Dandapat
Cytokine.2022; 157: 155967. CrossRef - Distinct histone H3 modification profiles correlate with aggressive characteristics of salivary gland neoplasms
Aroonwan Lam-Ubol, Ekarat Phattarataratip
Scientific Reports.2022;[Epub] CrossRef - Acetyl-CoA: An interplay between metabolism and epigenetics in cancer
Yang Hao, Qin Yi, Xu XiaoWu, Chen WeiBo, Zu GuangChen, Chen XueMin
Frontiers in Molecular Medicine.2022;[Epub] CrossRef - Sirtuins (SIRTs) As a Novel Target in Gastric Cancer
Agata Poniewierska-Baran, Paulina Warias, Katarzyna Zgutka
International Journal of Molecular Sciences.2022; 23(23): 15119. CrossRef - Novel oncogenes and tumor suppressor genes in hepatocellular carcinoma
Fang Wang, Peter Breslin S J, Wei Qiu
Liver Research.2021; 5(4): 195. CrossRef - Acute high folic acid treatment in SH-SY5Y cells with and without MTHFR function leads to gene expression changes in epigenetic modifying enzymes, changes in epigenetic marks, and changes in dendritic spine densities
Daniel F. Clark, Rachael Schmelz, Nicole Rogers, Nuri E. Smith, Kimberly R. Shorter, Lorenzo Chiariotti
PLOS ONE.2021; 16(1): e0245005. CrossRef - The E-Twenty-Six Family in Hepatocellular Carcinoma: Moving into the Spotlight
Tongyue Zhang, Danfei Liu, Yijun Wang, Mengyu Sun, Limin Xia
Frontiers in Oncology.2021;[Epub] CrossRef - Upregulation of histone acetylation reverses organic anion transporter 2 repression and enhances 5-fluorouracil sensitivity in hepatocellular carcinoma
Yingying Wang, Qianying Zhu, Haihong Hu, Hong Zhu, Bo Yang, Qiaojun He, Lushan Yu, Su Zeng
Biochemical Pharmacology.2021; 188: 114546. CrossRef - HCG11 up-regulation induced by ELK4 suppressed proliferation in vestibular schwannoma by targeting miR-620/ELK4
Ruiqing Long, Zhuohui Liu, Jinghui Li, Yuan Zhang, Hualin Yu
Cancer Cell International.2021;[Epub] CrossRef - Downregulation of circular RNA circPVT1 restricts cell growth of hepatocellular carcinoma through downregulation of Sirtuin 7 via microRNA‐3666
Yong Li, Haitao Shi, Jia Yuan, Lu Qiao, Lei Dong, Yan Wang
Clinical and Experimental Pharmacology and Physiology.2020; 47(7): 1291. CrossRef - Clinicopathological and molecular analysis of SIRT7 in hepatocellular carcinoma
Masae Yanai, Morito Kurata, Yutaka Muto, Hiroto Iha, Toshinori Kanao, Anna Tatsuzawa, Sachiko Ishibashi, Masumi Ikeda, Masanobu Kitagawa, Kouhei Yamamoto
Pathology.2020; 52(5): 529. CrossRef - MicroRNA‐148b Inhibits the Malignant Biological Behavior of Melanoma by Reducing Sirtuin 7 Expression Levels
Rui Sun, Meiliang Guo, Xiaojing Fan, Qinqin Meng, Dingfen Yuan, Xinrong Yang, Kexiang Yan, Hui Deng, Fengjie Sun
BioMed Research International.2020;[Epub] CrossRef - H3K18Ac as a Marker of Cancer Progression and Potential Target of Anti-Cancer Therapy
Marta Hałasa, Anna Wawruszak, Alicja Przybyszewska, Anna Jaruga, Małgorzata Guz, Joanna Kałafut, Andrzej Stepulak, Marek Cybulski
Cells.2019; 8(5): 485. CrossRef - Sirtuin7 has an oncogenic potential via promoting the growth of cholangiocarcinoma cells
Wenzhi Li, Zhe Sun, Chen Chen, Lin Wang, Zhimin Geng, Jie Tao
Biomedicine & Pharmacotherapy.2018; 100: 257. CrossRef - Identification of cancer‐related potential biomarkers based on lncRNA–pseudogene–mRNA competitive networks
Cheng Wu, Yunzhen Wei, Yinling Zhu, Kun Li, Yanjiao Zhu, Yichuan Zhao, Zhiqiang Chang, Yan Xu
FEBS Letters.2018; 592(6): 973. CrossRef - SIRT7 suppresses the epithelial-to-mesenchymal transition in oral squamous cell carcinoma metastasis by promoting SMAD4 deacetylation
Wenlu Li, Dandan Zhu, Shuaihua Qin
Journal of Experimental & Clinical Cancer Research.2018;[Epub] CrossRef - Sirtuin 7: a new marker of aggressiveness in prostate cancer
Romain Haider, Fabienne Massa, Lisa Kaminski, Stephan Clavel, Zied Djabari, Guillaume Robert, Kathiane Laurent, Jean-François Michiels, Matthieu Durand, Jean-Ehrland Ricci, Jean-François Tanti, Frédéric Bost, Damien Ambrosetti
Oncotarget.2017; 8(44): 77309. CrossRef
- Combined single-cell RNA sequencing and mendelian randomization to identify biomarkers associated with necrotic apoptosis in intervertebral disc degeneration
- Nuclear Expression of Hepatitis B Virus X Protein Is Associated with Recurrence of Early-Stage Hepatocellular Carcinomas: Role of Viral Protein in Tumor Recurrence
- Jing Jin, Hae Yoen Jung, KyuHo Lee, Nam-Joon Yi, Kyung-Suk Suh, Ja-June Jang, Kyoung-Bun Lee
- J Pathol Transl Med. 2016;50(3):181-189. Published online April 17, 2016
- DOI: https://doi.org/10.4132/jptm.2016.03.18
- 19,982 View
- 103 Download
- 11 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Hepatitis B virus (HBV) plays well-known roles in tumorigenesis of hepatocellular carcinoma (HCC) in infected patients. However, HBV-associated protein status in tumor tissues and the relevance to tumor behavior has not been reported. Our study aimed to examine the expression of HBV-associated proteins in HCC and adjacent nontumorous tissue and their clinicopathologic implication in HCC patients.
Methods
HBV surface antigen (HBsAg), HBV core antigen (HBcAg), and HBV X protein (HBx) were assessed in 328 HBV-associated HCCs and in 155 matched nontumorous tissues by immunohistochemistry staining.
Results
The positive rates of HBsAg and cytoplasmic HBx staining in tumor tissue were lower than those in nontumorous tissue (7.3% vs. 57.4%, p < .001; 43.4% vs. 81.3%, p < .001). Conversely, nuclear HBx was detected more frequently in tumors than in nontumorous tissue (52.1% vs. 30.3%, p < .001). HCCs expressing HBsAg, HBcAg, or cytoplasmic HBx had smaller size; lower Edmondson-Steiner (ES) nuclear grade, pT stage, and serum alpha-fetoprotein, and less angioinvasion than HCCs not expressing HBV-associated proteins. Exceptionally, nuclear HBx-positive HCCs showed higher ES nuclear grade and more frequent large-vessel invasion than did nuclear HBx-negative HCCs. In survival analysis, only nuclear HBx-positive HCCs had shorter disease-free survival than nuclear HBx-negative HCCs in pT1 and ES nuclear grade 1–2 HCC subgroup (median, 126 months vs. 35 months; p = .015).
Conclusions
Our data confirmed that expression of normal HBV-associated proteins generally decreases in tumor cells in comparison to nontumorous hepatocytes, with the exception of nuclear HBx, which suggests that nuclear HBx plays a role in recurrence of well-differentiated and early-stage HCCs. -
Citations
Citations to this article as recorded by- Triphasic CT Radiomics Model for Preoperative Prediction of Hepatocellular Carcinoma Pathological Grading
Haibo Huang, Xianpan Pan, Yingdan Zhang, Jie Yang, Lei Chen, Qinping Zhao, Lifeng Huang, Wei Lu, Yaohong Deng, Yingying Huang, Ke Ding
Journal of Hepatocellular Carcinoma.2025; Volume 12: 1725. CrossRef - Upregulation of Keratin 19 Expression by Hepatitis B Virus X Protein Promotes Hepatocellular Carcinoma Invasion, Metastasis, and Postoperative Recurrence
Jingyao Shen, Jie Zhang, Weimin Sun
Hepatitis Monthly.2025;[Epub] CrossRef - Relevance of HBx for Hepatitis B Virus-Associated Pathogenesis
Anja Schollmeier, Mirco Glitscher, Eberhard Hildt
International Journal of Molecular Sciences.2023; 24(5): 4964. CrossRef - Nomogram to predict the prognosis of patients with AFP-negative hepatocellular carcinoma undergoing chemotherapy: A SEER based study
Lei Wang, Jin-Lin Peng, Ji-Zhou Wu
Medicine.2023; 102(13): e33319. CrossRef - Tertiary Prevention of HCC in Chronic Hepatitis B or C Infected Patients
Wei Teng, Yen-Chun Liu, Wen-Juei Jeng, Chien-Wei Su
Cancers.2021; 13(7): 1729. CrossRef - Suppression of hepatitis b virus by a combined activity of CRISPR/Cas9 and HBx proteins
S. A. Brezgin, A. P. Kostyusheva, V. N. Simirsky, E. V. Volchkova, D. S. Chistyakov, D. S. Kostyushev, V. P. Chulanov
Russian Journal of Infection and Immunity.2019; 9(3-4): 476. CrossRef - Hepatitis B virus surface gene pre‐S2 mutant as a high‐risk serum marker for hepatoma recurrence after curative hepatic resection
Chia‐Jui Yen, Yu‐Lin Ai, Hung‐Wen Tsai, Shih‐Huang Chan, Chia‐Sheng Yen, Kuang‐Hsiung Cheng, Yun‐Ping Lee, Chia‐Wei Kao, Yu‐Chun Wang, Yi‐Lin Chen, Cheng‐Han Lin, Tsunglin Liu, Huey‐Pin Tsai, Jen‐Ren Wang, Ih‐Jen Su, Wenya Huang
Hepatology.2018; 68(3): 815. CrossRef - Integrin α6 as an invasiveness marker for hepatitis B viral X-driven hepatocellular carcinoma
Yi Rang Kim, Mi Ran Byun, Jin Woo Choi
Cancer Biomarkers.2018; 23(1): 135. CrossRef - Clinical Implications of Hepatitis B Virus RNA and Covalently Closed Circular DNA in Monitoring Patients with Chronic Hepatitis B Today with a Gaze into the Future: The Field Is Unprepared for a Sterilizing Cure
Anastasiya Kostyusheva, Dmitry Kostyushev, Sergey Brezgin, Elena Volchkova, Vladimir Chulanov
Genes.2018; 9(10): 483. CrossRef
- Triphasic CT Radiomics Model for Preoperative Prediction of Hepatocellular Carcinoma Pathological Grading
- Immunohistochemical Expression and Clinical Significance of Suggested Stem Cell Markers in Hepatocellular Carcinoma
- Jong Jin Sung, Sang Jae Noh, Jun Sang Bae, Ho Sung Park, Kyu Yun Jang, Myoung Ja Chung, Woo Sung Moon
- J Pathol Transl Med. 2016;50(1):52-57. Published online November 18, 2015
- DOI: https://doi.org/10.4132/jptm.2015.10.09
- 12,081 View
- 78 Download
- 21 Web of Science
- 18 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Increasing evidence has shown that tumor initiation and growth are nourished by a small subpopulation of cancer stem cells (CSCs) within the tumor mass. CSCs are posited to be responsible for tumor maintenance, growth, distant metastasis, and relapse after curative operation. We examined the expression of CSC markers in paraffin-embedded tissue sections of hepatocellular carcinoma (HCC) and correlated the results with clinicopathologic characteristics. Methods: Immunohistochemical staining for the markers believed to be expressed in the CSCs, including epithelial cell adhesion molecule (EpCAM), keratin 19 (K19), CD133, and CD56, was performed in 82 HCC specimens. Results: EpCAM expression was observed in 56% of the HCCs (46/82) and K19 in 6% (5/82). EpCAM expression in HCC significantly correlated with elevated α-fetoprotein level, microvessel invasion of tumor cells, and high histologic grade. In addition, Ep- CAM expression significantly correlated with K19 expression. The overall survival and relapsefree survival rates in patients with EpCAM-expressing HCC were relatively lower than those in patients with EpCAM-negative HCC. All but two of the 82 HCCs were negative for CD133 and CD56, respectively. Conclusions: Our results suggest that HCCs expressing EpCAM are associated with unfavorable prognostic factors and have a more aggressive clinical course than those not expressing EpCAM. Further, the expression of either CD133 or CD56 in paraffin-embedded HCC tissues appears to be rare. -
Citations
Citations to this article as recorded by- Spatial immune scoring system predicts hepatocellular carcinoma recurrence
Gengjie Jia, Peiqi He, Tianli Dai, Denise Goh, Jiabei Wang, Mengyuan Sun, Felicia Wee, Fuling Li, Jeffrey Chun Tatt Lim, Shuxia Hao, Yao Liu, Tony Kiat Hon Lim, Nye-Thane Ngo, Qingping Tao, Wei Wang, Ahitsham Umar, Björn Nashan, Yongchang Zhang, Chen Ding
Nature.2025; 640(8060): 1031. CrossRef - Evolving Landscape of Systemic Therapy for Hepatocellular Carcinoma in 2025
Karan Kumar, Vivek A. Saraswat
Journal of Clinical and Experimental Hepatology.2025; 15(5): 102547. CrossRef - Recent Progress in Systemic Therapy for Advanced Hepatocellular Carcinoma
Narayanan Sadagopan, Aiwu Ruth He
International Journal of Molecular Sciences.2024; 25(2): 1259. CrossRef - Diagnostic value of expressions of cancer stem cell markers for adverse outcomes of hepatocellular carcinoma and their associations with prognosis: A Bayesian network meta‑analysis
Zhengrong Ou, Shoushuo Fu, Jian Yi, Jingxuan Huang, Weidong Zhu
Oncology Letters.2024;[Epub] CrossRef - Clinicopathological and prognostic value of epithelial cell adhesion molecule in solid tumours: a meta-analysis
Peiwen Ding, Panyu Chen, Jiqi Ouyang, Qiang Li, Shijie Li
Frontiers in Oncology.2023;[Epub] CrossRef - PD-L1 Downregulation and DNA Methylation Inhibition for Molecular Therapy against Cancer Stem Cells in Hepatocellular Carcinoma
Caecilia Sukowati, Loraine Kay D. Cabral, Beatrice Anfuso, Francesco Dituri, Roberto Negro, Gianluigi Giannelli, Claudio Tiribelli
International Journal of Molecular Sciences.2023; 24(17): 13357. CrossRef - EpCAM, Ki67, and ESM1 Predict Hepatocellular Carcinoma Recurrence After Liver Transplantation
Aiat Shaban Hemida, Doha Maher Taie, Moshira Mohamed Abd El-Wahed, Mohammed Ibrahim Shabaan, Mona Saeed Tantawy, Nermine Ahmed Ehsan
Applied Immunohistochemistry & Molecular Morphology.2023; 31(9): 596. CrossRef - The clinical, prognostic and therapeutic significance of liver cancer stem cells and their markers
Izabela Zarębska, Arkadiusz Gzil, Justyna Durślewicz, Damian Jaworski, Paulina Antosik, Navid Ahmadi, Marta Smolińska-Świtała, Dariusz Grzanka, Łukasz Szylberg
Clinics and Research in Hepatology and Gastroenterology.2021; 45(3): 101664. CrossRef - Detection of oncogenic mutations in paired circulating tumor DNA and circulating tumor cells in patients with hepatocellular carcinoma
Zhouhong Ge, Jean C.A. Helmijr, Maurice P.H.M. Jansen, Patrick P.C. Boor, Lisanne Noordam, Maikel Peppelenbosch, Jaap Kwekkeboom, Jaco Kraan, Dave Sprengers
Translational Oncology.2021; 14(7): 101073. CrossRef - Hepatocellular Carcinoma Score and Subclassification Into Aggressive Subtypes Using Immunohistochemical Expression of p53, β-Catenin, CD133, and Ki-67
Asmaa G. Abdou, Nanis S. Holah, Dina S. Elazab, Walaa G. El-Gendy, Mohammed T. Badr, Dalia R. Al-Sharaky
Applied Immunohistochemistry & Molecular Morphology.2021; 29(1): 20. CrossRef - The prognostic significance of neuroendocrine markers and somatostatin receptor 2 in hepatocellular carcinoma
Keigo Murakami, Hiroyuki Kumata, Shigehito Miyagi, Takashi Kamei, Hironobu Sasano
Pathology International.2021; 71(10): 682. CrossRef - Predictors of recurrence and survival of hepatocellular carcinoma: A prospective study including transient elastography and cancer stem cell markers
Hend Ibrahim Shousha, Rabab Fouad, Tamer Mahmoud Elbaz, Dina Sabry, Mohamed Mahmoud Nabeel, Ahmed Hosni Abdelmaksoud, Aisha Mahmoud Elsharkawy, Zeinab Abdellatif Soliman, Ghada Habib, Ashraf Omar Abdelaziz
Arab Journal of Gastroenterology.2020; 21(2): 95. CrossRef - Napabucasin Reduces Cancer Stem Cell Characteristics in Hepatocellular Carcinoma
Ya Li, Qiuju Han, Huajun Zhao, Quanjuan Guo, Jian Zhang
Frontiers in Pharmacology.2020;[Epub] CrossRef - The mRNA Distribution of Cancer Stem Cell Marker CD90/Thy-1 Is Comparable in Hepatocellular Carcinoma of Eastern and Western Populations
An B. Luong, Huy Q. Do, Paola Tarchi, Deborah Bonazza, Cristina Bottin, Loraine Kay D. Cabral, Long D. C. Tran, Thao P. T. Doan, Lory S. Crocè, Hoa L. T. Pham, Claudio Tiribelli, Caecilia H. C. Sukowati
Cells.2020; 9(12): 2672. CrossRef - Histological architectural classification determines recurrence pattern and prognosis after curative hepatectomy in patients with hepatocellular carcinoma
Hirohisa Okabe, Tomoharu Yoshizumi, Yo-ichi Yamashita, Katsunori Imai, Hiromitsu Hayashi, Shigeki Nakagawa, Shinji Itoh, Norifumi Harimoto, Toru Ikegami, Hideaki Uchiyama, Toru Beppu, Shinichi Aishima, Ken Shirabe, Hideo Baba, Yoshihiko Maehara, Motoyuki
PLOS ONE.2018; 13(9): e0203856. CrossRef - Overexpression of epithelial cell adhesion molecule as a predictor of poor outcome in patients with hepatocellular carcinoma
Chih‑Jan Ko, Chia‑Jung Li, Meng‑Yu Wu, Pei‑Yi Chu
Experimental and Therapeutic Medicine.2018;[Epub] CrossRef - Clinicopathologic Significance of Survivin Expression in Relation to CD133 Expression in Surgically Resected Stage II or III Colorectal Cancer
Wanlu Li, Mi-Ra Lee, EunHee Choi, Mee-Yon Cho
Journal of Pathology and Translational Medicine.2017; 51(1): 17. CrossRef - PIN1 in hepatocellular carcinoma is associated with TP53 gene status
Jun Sang Bae, Sang Jae Noh, Kyoung Min Kim, Kyu Yun Jang, Ho Sung Park, Myoung Ja Chung, Byung-Hyun Park, Woo Sung Moon
Oncology Reports.2016; 36(4): 2405. CrossRef
- Spatial immune scoring system predicts hepatocellular carcinoma recurrence
- SALL4 Expression in Hepatocellular Carcinomas Is Associated with EpCAM-Positivity and a Poor Prognosis
- Hyunjin Park, Hyejung Lee, An Na Seo, Jai Young Cho, Young Rok Choi, Yoo-Seok Yoon, Ho-Seong Han, Young Nyun Park, Haeryoung Kim
- J Pathol Transl Med. 2015;49(5):373-381. Published online August 10, 2015
- DOI: https://doi.org/10.4132/jptm.2015.07.09
- 13,063 View
- 98 Download
- 24 Web of Science
- 23 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
There is increasing interest in hepatocellular carcinomas (HCC) expressing “stemness”-related markers, as they have been associated with aggressive behavior and poor prognosis. In this study, we investigated the usefulness of Sal-like protein 4 (SALL4), a recently proposed candidate marker of “stemness.” Methods: Immunohistochemical stains were performed for SALL4, K19, and epithelial cellular adhesion molecule (EpCAM) on tissue microarrays constructed from 190 surgically resected HCCs, and the results were correlated with the clinicopathological features and patient survival data. Results: Nuclear SALL4 expression was observed in 39/190 HCCs (20.5%), while K19 and EpCAM were expressed in 30 (15.9%) and 92 (48.7%) HCCs, respectively. The nuclear expression was generally weak, punctate or clumped. SALL4 expression was significantly associated with a poor overall survival compared to SALL4-negative HCCs (p = .014) compared to SALL4-negative HCCs. On multivariate analysis adjusted for tumor size, multiplicity, vascular invasion, and pathological tumor stage, SALL4 remained as a significant independent predictor of decreased overall survival (p= .004). SALL4 expression was positively correlated with EpCAM expression (p = .013) but not with K19 expression. HCCs that expressed both SALL4 and EpCAM were associated with significantly decreased overall survival, compared to those cases which were negative for both of these markers (p = .031). Conclusions: Although SALL4 expression was not significantly correlated with other clinicopathological parameters suggestive of tumor aggressiveness, SALL4 expression was an independent predictor of poor overall survival in human HCCs, and was also positively correlated with EpCAM expression. -
Citations
Citations to this article as recorded by- A Clinical Guidance for the Management of Patients With Hepatoid Adenocarcinoma and A Case Series
Christina Liava, Sudhakar Venkatesh, Michael S. Torbenson, Patrick S. Kamath, Moira Hilscher
Cancer Medicine.2026;[Epub] CrossRef - Cytoplasmic SALL4-A isoform expression as a diagnostic marker of less aggressive tumor behavior in gastric cancer
Saeed Rahmani, Amirhesam Babajani, Maryam Abolhasani, Roya Ghods, Elham Kalantari, Zahra Madjd
World Journal of Surgical Oncology.2025;[Epub] CrossRef - Cancer stem cells in hepatocellular carcinoma: therapy resistance and emerging treatments
Dipesh Kumar Yadav, Rajesh Kumar Yadav, Alina Singh, Yi Huang, Dandan Bao, Zhangwei Yang, Hanzhang Huang, Yin Jiang, Pengwei Wang, Sisi Lin, Yongfei Hua, Yiren Hu
Frontiers in Immunology.2025;[Epub] CrossRef - Stemness markers in hepatocellular carcinoma of Eastern vs. Western population: Etiology matters?
Caecilia HC Sukowati, Korri El-Khobar, Chyntia Olivia Maurine Jasirwan, Juferdy Kurniawan, Rino Alvani Gani
Annals of Hepatology.2024; 29(1): 101153. CrossRef - Research progress and prospects of AFP-positive gastric cancer
Long Zhao, Changjiang Yang, Yilin Lin, Shan Wang, Yingjiang Ye, Zhanlong Shen
Foregut Surgery.2022; 2(1): 29. CrossRef - SALL4 and microRNA: The Role of Let-7
Jun Liu, Madeline A. Sauer, Shaza G. Hussein, Junyu Yang, Daniel G. Tenen, Li Chai
Genes.2021; 12(9): 1301. CrossRef - Hepatoid Teratoma, Hepatoid Yolk Sac Tumor, and Hepatocellular Carcinoma
Khaleel I. Al-Obaidy, Sean R. Williamson, Nathan Shelman, Muhammad T. Idrees, Thomas M. Ulbright
American Journal of Surgical Pathology.2021; 45(1): 127. CrossRef - Targeting an Inducible SALL4-Mediated Cancer Vulnerability with Sequential Therapy
Junyu Yang, Chong Gao, Miao Liu, Yao-Chung Liu, Junsu Kwon, Jun Qi, Xi Tian, Alicia Stein, Yanjing V. Liu, Nikki R. Kong, Yue Wu, Shenyi Yin, Jianzhong Xi, Zhiyuan Chen, Kalpana Kumari, Hannan Wong, Hongbo Luo, Leslie E. Silberstein, Julie A.I. Thoms, Ash
Cancer Research.2021; 81(23): 6018. CrossRef - Lipoprotein‐Like Nanoparticle Carrying Small Interfering RNA Against Spalt‐Like Transcription Factor 4 Effectively Targets Hepatocellular Carcinoma Cells and Decreases Tumor Burden
William Cruz, Huang Huang, Brian Barber, Elisa Pasini, Lili Ding, Gang Zheng, Juan Chen, Mamatha Bhat
Hepatology Communications.2020; 4(5): 769. CrossRef - Hepatoid adenocarcinoma of the stomach: a unique subgroup with distinct clinicopathological and molecular features
Yakun Wang, Li Sun, Zhongwu Li, Jing Gao, Sai Ge, Cheng Zhang, Jiajia Yuan, Xicheng Wang, Jian Li, Zhihao Lu, Jifang Gong, Ming Lu, Jun Zhou, Zhi Peng, Lin Shen, Xiaotian Zhang
Gastric Cancer.2019; 22(6): 1183. CrossRef - Gynecologic Serous Carcinoma: An Immunohistochemical Analysis of Malignant Body Fluid Specimens
Shuyue Ren, William Klump
Archives of Pathology & Laboratory Medicine.2019; 143(6): 677. CrossRef - The Pluripotency Network in Colorectal Cancer Pathogenesis and Prognosis: an Update
Ioannis A Voutsadakis
Biomarkers in Medicine.2018; 12(6): 653. CrossRef - Cancer stem cells in hepatocellular carcinoma: an overview and promising therapeutic strategies
Nuozhou Wang, Shanshan Wang, Ming-Yue Li, Bao-guang Hu, Li-ping Liu, Sheng-li Yang, Shucai Yang, Zhongqin Gong, Paul B. S. Lai, George G. Chen
Therapeutic Advances in Medical Oncology.2018;[Epub] CrossRef - DNA demethylation induces SALL4 gene re-expression in subgroups of hepatocellular carcinoma associated with Hepatitis B or C virus infection
H Fan, Z Cui, H Zhang, S K Mani, A Diab, L Lefrancois, N Fares, P Merle, O Andrisani
Oncogene.2017; 36(17): 2435. CrossRef - Higher expression of SALL4 predicts poor cancer prognosis: A meta-analysis
Hongyu Shen, Liangpeng Li, Dandan Wang, Sujin Yang, Xiu Chen, Siying Zhou, Shanliang Zhong, Jianhua Zhao, Jinhai Tang
Cancer Biomarkers.2017; 19(4): 365. CrossRef - SALL4 suppresses PTEN expression to promote glioma cell proliferation via PI3K/AKT signaling pathway
Chuanjin Liu, Haibin Wu, Yanyan Li, Liang Shen, Renchun Yu, Hongwei Yin, Ting Sun, Chunming Sun, Youxin Zhou, Ziwei Du
Journal of Neuro-Oncology.2017; 135(2): 263. CrossRef - Liver Cancer: Molecular Characterization, Clonal Evolution and Cancer Stem Cells
Germana Castelli, Elvira Pelosi, Ugo Testa
Cancers.2017; 9(9): 127. CrossRef - Oncofetal gene SALL4 and prognosis in cancer: A systematic review with meta-analysis
Lorenzo Nicolè, Tiziana Sanavia, Nicola Veronese, Rocco Cappellesso, Claudio Luchini, Paolo Dabrilli, Ambrogio Fassina
Oncotarget.2017; 8(14): 22968. CrossRef - SALL4, the missing link between stem cells, development and cancer
Hiro Tatetsu, Nikki R. Kong, Gao Chong, Giovanni Amabile, Daniel G. Tenen, Li Chai
Gene.2016; 584(2): 111. CrossRef - A New Cell Block Method for Multiple Immunohistochemical Analysis of Circulating Tumor Cells in Patients with Liver Cancer
Soo Jeong Nam, Hyun Yang Yeo, Hee Jin Chang, Bo Hyun Kim, Eun Kyung Hong, Joong-Won Park
Cancer Research and Treatment.2016; 48(4): 1229. CrossRef - Functional and clinical significance of SALL4 in breast cancer
Ebubekir Dirican, Mustafa Akkiprik
Tumor Biology.2016; 37(9): 11701. CrossRef - MicroRNA-33b suppresses the proliferation and metastasis of hepatocellular carcinoma cells through the inhibition of Sal-like protein 4 expression
Qinggang Tian, Yao Xiao, Yanting Wu, Yun Liu, Zhiqing Song, Wenfeng Gao, Jing Zhang, Jingling Yang, Yuguo Zhang, Tuankui Guo, Furong Dai, Zhigang Sun
International Journal of Molecular Medicine.2016; 38(5): 1587. CrossRef - Oncogenic protein SALL4 and ZNF217 as prognostic indicators in solid cancers: a meta-analysis of individual studies
Ji Cheng, Jinbo Gao, Xiaoming Shuai, Kaixiong Tao
Oncotarget.2016; 7(17): 24314. CrossRef
- A Clinical Guidance for the Management of Patients With Hepatoid Adenocarcinoma and A Case Series
- Pathology-MRI Correlation of Hepatocarcinogenesis: Recent Update
- Jimi Huh, Kyung Won Kim, Jihun Kim, Eunsil Yu
- J Pathol Transl Med. 2015;49(3):218-229. Published online May 15, 2015
- DOI: https://doi.org/10.4132/jptm.2015.04.15
- 26,794 View
- 334 Download
- 13 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF - Understanding the important alterations during hepatocarcinogenesis as well as the characteristic magnetic resonance imaging (MRI) and histopathological features will be helpful for managing patients with chronic liver disease and hepatocellular carcinoma. Recent advances in MRI techniques, such as fat/iron quantification, diffusion-weighted images, and gadoxetic acid-enhanced MRI, have greatly enhanced our understanding of hepatocarcinogenesis.
-
Citations
Citations to this article as recorded by- Update on Hepatocellular Carcinoma Imaging Features Associated With Histology, Subtype, and Prognosis Along With Changes to LI-RADS in 2024
Sergio P. Klimkowski, Ann Shi, Omar Altabbakh, Janio Szklaruk, AnuradhaS. Shenoy-Bhangle, Gauruv S. Likhari, Khaled M. Elsayes
Seminars in Roentgenology.2025; 60(1): 6. CrossRef - Advances in the Diagnosis, Treatment, and Management of Liver Nodules: A Comprehensive Review
Chang Gao, Dongyang Chen, Youpeng Chen
Portal Hypertension & Cirrhosis.2025; 4(4): 232. CrossRef - Gadoxetic acid in hepatocellular carcinoma and liver metastases: pearls and pitfalls
H.M. Kwok, C.M. Chau, H.C.H. Lee, T. Wong, H.F. Chan, W.H. Luk, W.T.A. Yung, L.F. Cheng, K.F.J. Ma
Clinical Radiology.2023; 78(10): 715. CrossRef - Multi-phasic magnetic resonance imaging of hemodynamic interchanges in hepatocarcinogenesis
Ahmed Mahmoud Elzeneini, Mohsen Ahmed Abdelmohsen, Mohamed Ibrahim Yousef
Egyptian Journal of Radiology and Nuclear Medicine.2023;[Epub] CrossRef - Risk Factors for Hypervascularization in Hepatobiliary Phase Hypointense Nodules without Arterial Phase Hyperenhancement: A Systematic Review and Meta-analysis
Tae-Hyung Kim, Sungmin Woo, Sangwon Han, Chong Hyun Suh, Richard Kinh Gian Do, Jeong Min Lee
Academic Radiology.2022; 29(2): 198. CrossRef - Comparison of IDEAL-IQ and IVIM-DWI for Differentiating between Alpha Fetoprotein-Negative Hepatocellular Carcinoma and Focal Nodular Hyperplasia
Shaopeng Li, Peng Wang, Jun Qiu, Yiju Xie, Dawei Yin, Kexue Deng
Oncologie.2022; 24(3): 527. CrossRef - Hepatocarcinogenesis
Alice Fung, Krishna P. Shanbhogue, Myles T. Taffel, Brian T. Brinkerhoff, Neil D. Theise
Magnetic Resonance Imaging Clinics of North America.2021; 29(3): 359. CrossRef - Pathologic, Molecular, and Prognostic Radiologic Features of Hepatocellular Carcinoma
Kathryn J. Fowler, Adam Burgoyne, Tyler J. Fraum, Mojgan Hosseini, Shintaro Ichikawa, Sooah Kim, Azusa Kitao, Jeong Min Lee, Valérie Paradis, Bachir Taouli, Neil D. Theise, Valérie Vilgrain, Jin Wang, Claude B. Sirlin, Victoria Chernyak
RadioGraphics.2021; 41(6): 1611. CrossRef - Update on Hepatocellular Carcinoma: a Brief Review from Pathologist Standpoint
Nese Karadag Soylu
Journal of Gastrointestinal Cancer.2020; 51(4): 1176. CrossRef - Gadoxetate-enhanced dynamic contrast-enhanced MRI for evaluation of liver function and liver fibrosis in preclinical trials
Jimi Huh, Su Jung Ham, Young Chul Cho, Bumwoo Park, Bohyun Kim, Chul-Woong Woo, Yoonseok Choi, Dong-Cheol Woo, Kyung Won Kim
BMC Medical Imaging.2019;[Epub] CrossRef - Non-Hypervascular Hypointense Nodules at Gadoxetic Acid MRI: Hepatocellular Carcinoma Risk Assessment with Emphasis on the Role of Diffusion-Weighted Imaging
Chiara Briani, Marco Di Pietropaolo, Massimo Marignani, Francesco Carbonetti, Paola Begini, Vincenzo David, Elsa Iannicelli
Journal of Gastrointestinal Cancer.2018; 49(3): 302. CrossRef
- Update on Hepatocellular Carcinoma Imaging Features Associated With Histology, Subtype, and Prognosis Along With Changes to LI-RADS in 2024
- Overexpression of C-reactive Protein as a Poor Prognostic Marker of Resectable Hepatocellular Carcinomas
- Jin Ho Shin, Chong Jai Kim, Eun Jeong Jeon, Chang Ohk Sung, Hwa Jeong Shin, Jene Choi, Eunsil Yu
- J Pathol Transl Med. 2015;49(2):105-111. Published online March 12, 2015
- DOI: https://doi.org/10.4132/jptm.2015.01.19
- 13,499 View
- 83 Download
- 22 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
C-reactive protein (CRP) is an acute phase reactant synthesized in the liver. CRP immunoreactivity is a feature of inflammatory hepatocellular adenomas with a higher risk of malignant transformation. A high serum CRP level denotes poor prognosis in hepatocellular carcinoma (HCC) patients. This study was conducted to determine whether CRP is produced in HCC and to assess the clinicopathologic significance of CRP expression in cancer cells. Methods: CRP immunoreactivity was examined in treatment-naïve HCCs (n=224) using tissue microarrays and was correlated with clinicopathologic parameters. The expression of CRP mRNA and protein was also assessed in 12 HCC cases by quantitative real-time polymerase chain reaction and immunoblotting. Hep3B and SNU-449 HCC cell lines were used for the analysis of CRP mRNA regulation by interleukin 6 (IL-6). Results: CRP was expressed in 133 of 224 HCCs (59.4%) with a variable degree of immunoreactivity (grade 1 in 25.9%; grade 2 in 20.1%; grade 3 in 13.4%). There was an inverse relationship between grade 3 CRP immunoreactivity and cancer-specific survival (p=.0047), while no associations were found with other parameters, including recurrence-free survival. The CRP mRNA expression level was significantly higher in CRP immunopositive cases than in immunonegative cases (p<.05). CRP mRNA expression was increased in Hep3B cells, but was not detected in SNU-449 cells even after IL-6 treatment. Conclusions: We report the expression of CRP in HCC for the first time. CRP expression was associated with poor cancer-specific survival in patients with resectable HCC. -
Citations
Citations to this article as recorded by- Influencing Factors for Postembolization Fever in Patients Undergoing Transarterial Chemoembolization Based on Machine Learning
Won-Du Chang, Myoung Soo Kim
CIN: Computers, Informatics, Nursing.2026;[Epub] CrossRef - Diagnostic and prognostic relevance of inflammatory markers in surgically treated thymic epithelial tumors: An international multicenter study
Evelyn Megyesfalvi, Aron Ghimessy, Jonas Bauer, Orsolya Pipek, Kevin Saghi, Aron Gellert, Janos Fillinger, Ozlem Okumus, Vivien Teglas, Erna Ganofszky, Krisztina Bogos, Ferenc Renyi-Vamos, Zsolt Megyesfalvi, Clemens Aigner, Balazs Hegedus, Balazs Dome, Be
Lung Cancer.2025; 200: 108111. CrossRef - The Role of IL‐6, IL‐10 and CRP in Gastrointestinal Cancers
Reyhaneh Yarmohammadi, Kazem Najafi, Mina Noroozbeygi, Kimia Didehvar, Aria Rastin, Faezeh Ataei, Mohammad Reza Atashzar, Sahar Shomeil Shushtari
Cell Biology International.2025; 49(9): 1061. CrossRef - Peritumoral portal enhancement during transarterial chemoembolization: a potential prognostic factor for patients with hepatocellular carcinoma
Sofi Sennefelt Nyman, Angeliki Dimopoulou Creusen, Ulf Johnsson, Fredrik Rorsman, Johan Vessby, Charlotte Ebeling Barbier
Acta Radiologica.2022; 63(10): 1323. CrossRef - The quest for precision oncology with immune checkpoint inhibitors for hepatocellular carcinoma
Giuseppe Cabibbo, Amit G. Singal
Journal of Hepatology.2022; 76(2): 262. CrossRef - HNF-1β is a More Sensitive and Specific Marker Than C-Reactive Protein for Identifying Biliary Differentiation in Primary Hepatic Carcinomas
Pallavi A. Patil, Tamar Taddei, Dhanpat Jain, Xuchen Zhang
Archives of Pathology & Laboratory Medicine.2022; 146(2): 220. CrossRef - Malignant transformation of hepatocellular adenoma
Céline Julien, Brigitte Le Bail, Laurence Chiche, Charles Balabaud, Paulette Bioulac-Sage
JHEP Reports.2022; 4(3): 100430. CrossRef - Effect of Treatment with Colchicine after Acute Coronary Syndrome on Major Cardiovascular Events: A Systematic Review and Meta-Analysis of Clinical Trials
Erfan Razavi, Akam Ramezani, Asma Kazemi, Armin Attar, Baohui Xu
Cardiovascular Therapeutics.2022; 2022: 1. CrossRef - Steatotic and Steatohepatitic Hepatocellular Carcinomas
Umut Aykutlu, Asuman Argon, Mehmet Orman, Sezgin Ulukaya, Murat Zeytunlu, Zeki Karasu, Fulya Günşar, Deniz Nart, Ulus Akarca, Funda Yilmaz
American Journal of Surgical Pathology.2021; 45(9): 1252. CrossRef - Cytochrome P450 4A11 expression in tumor cells: A favorable prognostic factor for hepatocellular carcinoma patients
Hyuk Soo Eun, Sang Yeon Cho, Byung Seok Lee, Sup Kim, In‐Sang Song, Kwangsik Chun, Cheong‐Hae Oh, Min‐Kyung Yeo, Seok Hyun Kim, Kyung‐Hee Kim
Journal of Gastroenterology and Hepatology.2019; 34(1): 224. CrossRef - Investigating Trk Protein Expression between Oropharyngeal and Non-oropharyngeal Squamous Cell Carcinoma: Clinical Implications and Possible Roles of Human Papillomavirus Infection
Yoon Ah Cho, Ji Myung Chung, Hyunmi Ryu, Eun Kyung Kim, Byoung Chul Cho, Sun Och Yoon
Cancer Research and Treatment.2019; 51(3): 1052. CrossRef - Increased systemic zonula occludens 1 associated with inflammation and independent biomarker in patients with hepatocellular carcinoma
Amit Kumar Ram, Biju Pottakat, Balasubramaniyan Vairappan
BMC Cancer.2018;[Epub] CrossRef - C-reactive Protein Overexpression in the Background Liver of Hepatitis B Virus–Associated Hepatocellular Carcinoma Is a Prognostic Biomarker
Jin Ho Shin, Eunsil Yu, Eun Na Kim, Chong Jai Kim
Journal of Pathology and Translational Medicine.2018; 52(5): 267. CrossRef - Efficacy of vasopressin V2 receptor antagonist tolvaptan in treatment of hepatic edema
Yasunari Hiramine, Hirofumi Uto, Yasushi Imamura, Takuya Hiwaki, Takeshi Kure, Sho Ijuin, Kohei Oda, Seiichi Mawatari, Kotaro Kumagai, Koki Tokunaga, Hirofumi Higashi, Ichiro Kanetsuki, Osamu Kubozono, Shigeho Maenohara, Akio Ido
Hepatology Research.2017; 47(6): 542. CrossRef - Elevated CRP levels predict poor outcome and tumor recurrence in patients with thymic epithelial tumors: A pro- and retrospective analysis
Stefan Janik, Christine Bekos, Philipp Hacker, Thomas Raunegger, Bahil Ghanim, Elisa Einwallner, Lucian Beer, Walter Klepetko, Leonhard Müllauer, Hendrik J. Ankersmit, Bernhard Moser
Oncotarget.2017; 8(29): 47090. CrossRef - Pretreatment neutrophil-to-lymphocyte ratio predicts prognosis in patients with metastatic renal cell carcinoma receiving targeted therapy
Gui-Ming Zhang, Yao Zhu, Wei-Jie Gu, Hai-Liang Zhang, Guo-Hai Shi, Ding-Wei Ye
International Journal of Clinical Oncology.2016; 21(2): 373. CrossRef - Current Proceedings in the Molecular Dissection of Hepatocellular Adenomas: Review and Hands-on Guide for Diagnosis
Diane Goltz, Hans-Peter Fischer
International Journal of Molecular Sciences.2015; 16(9): 20994. CrossRef
- Influencing Factors for Postembolization Fever in Patients Undergoing Transarterial Chemoembolization Based on Machine Learning
- Periductal Stromal Tumor of Breast: A Case Report and A Review of Literature
- Salma L. Abbasi, Kate McNamara, Mohammed S. Absar, Alison Darlington, Francene Clucas, Sami Titi
- Korean J Pathol. 2014;48(6):442-444. Published online December 31, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.6.442
- 13,718 View
- 89 Download
- 5 Crossref
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Genetic Profiling of Mammary Periductal Stromal Tumors With Histologic Correlation Highlights High-Grade and Low-Grade Groups and Similarities to Phyllodes Tumors
Gregor Krings, Gregory R. Bean, Elizabeth M. Hosfield, J Jordi Rowe, Joseph Geradts, Yunn-Yi Chen
Modern Pathology.2026; 39(3): 100961. CrossRef - Survey of recurrent diagnostic challenges in breast phyllodes tumours
Benjamin Yongcheng Tan, Stephen B Fox, Sunil R Lakhani, Puay Hoon Tan
Histopathology.2023; 82(1): 95. CrossRef - Management of a periductal stromal tumor in a young woman: Our breast unit experience
Irene Valente, Adela Ristani, Cristina Mancini, Eugenia Martella, Leonardo Quartieri, Cecilia D'Aloia
The Breast Journal.2020; 26(7): 1375. CrossRef - A Diagnostic Approach to Fibroepithelial Breast Lesions
Benjamin Yongcheng Tan, Puay Hoon Tan
Surgical Pathology Clinics.2018; 11(1): 17. CrossRef - A case of local recurrence of periductal stromal sarcoma of the breast
Kana TERAMOTO, Yasuro DOI, Kayo YAMAMOTO, Kaname MATSUKAWA, Hisaka IWAIHARA, Rumi MOTOSHIMA, Noboru TAKATA, Ichiro YOSHINAKA, Kazunori HARADA
Choonpa Igaku.2018; 45(1): 61. CrossRef
- Genetic Profiling of Mammary Periductal Stromal Tumors With Histologic Correlation Highlights High-Grade and Low-Grade Groups and Similarities to Phyllodes Tumors
- Solid Form of Epithelioid Hemangioma: A Case Report
- Jin Roh, Min Jeong Song, Mi Woo Lee, Chan-Sik Park
- Korean J Pathol. 2014;48(5):394-397. Published online October 27, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.5.394
- 11,380 View
- 88 Download
- 4 Crossref
-
 PDF
PDF -
Citations
Citations to this article as recorded by- Clinicopathologic and radio-genomic insights into hepatic epithelioid hemangioma: An illustrated review
Elijah Brown, Karen Schoedel, Adarsh Barwad, Alessandro Furlan, Paul J.L. Zhang, Nigar Anjuman Khurram
Human Pathology.2026; 170: 105955. CrossRef - Epithelioid Haemangioma of Bone: A Case Series and Comprehensive Literature Review Reappraising the Diagnostic Classification of All Epithelioid Vascular Neoplasms of Bone
Subramaniam Ramkumar
Cureus.2021;[Epub] CrossRef - Update on cutaneous epithelioid vascular tumours
Boštjan Luzar, Eduardo Calonje
Diagnostic Histopathology.2018; 24(8): 273. CrossRef - Epithelioid Hemangioma (Angiolymphoid Hyperplasia With Eosinophilia) of the Heart With Peripheral Eosinophilia and Nephrotic Syndrome
Isidro Machado, Agustín Chong, Anisia Serrano, Alfredo Mario Naranjo Ugalde, Damian Pineda, Laynes Savón, Ever Olivera, Antonio Llombart-Bosch
International Journal of Surgical Pathology.2016; 24(1): 59. CrossRef
- Clinicopathologic and radio-genomic insights into hepatic epithelioid hemangioma: An illustrated review
- Histologic Disorderliness in the Arrangement of Tumor Cells as an Objective Measure of Tumor Differentiation
- Sungwook Suh, Gyeongsin Park, Young Sub Lee, Yosep Chong, Youn Soo Lee, Yeong Jin Choi
- Korean J Pathol. 2014;48(5):339-345. Published online October 27, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.5.339
- 7,743 View
- 66 Download
-
 Abstract
Abstract
 PDF
PDF - Background: Inter-observer and intra-observer variation in histologic tumor grading are well documented. To determine whether histologic disorderliness in the arrangement of tumor cells may serve as an objective criterion for grading, we tested the hypothesis the degree of disorderliness is related to the degree of tumor differentiation on which tumor grading is primarily based. Methods: Borrowing from the statistical thermodynamic definition of entropy, we defined a novel mathematical formula to compute the relative degree of histologic disorderliness of tumor cells. We then analyzed a total of 51 photomicrographs of normal colorectal mucosa and colorectal adenocarcinoma with varying degrees of differentiation using our formula. Results: A one-way analysis of variance followed by post hoc pairwise comparisons using Bonferroni correction indicated that the mean disorderliness score was the lowest for the normal colorectal mucosa and increased with decreasing tumor differentiation. Conclusions: Disorderliness, a pathologic feature of malignant tumors that originate from highly organized structures is useful as an objective tumor grading proxy in the field of digital pathology.
- Prognostic Significance of BCL9 Expression in Hepatocellular Carcinoma
- Jiyeon Hyeon, Soomin Ahn, Jae Jun Lee, Dae Hyun Song, Cheol-Keun Park
- Korean J Pathol. 2013;47(2):130-136. Published online April 24, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.2.130
- 9,733 View
- 71 Download
- 19 Crossref
-
 Abstract
Abstract
 PDF
PDF Background BCL9 enhances β-catenin-mediated transcriptional activity regardless of the mutational status of the Wnt signaling components and increases the cell proliferation, migration, invasion, and metastatic potential of tumor cells. The goal of this study was to elucidate the prognostic significance of BCL9 protein expression in hepatocellular carcinoma (HCC) patients.
Methods We evaluated BCL9 protein expression by immunohistochemistry in tumor tissue from 288 primary HCC patients who underwent curative hepatectomy. The impact of BCL9 expression on the survival of the patients was analyzed. The median follow-up period was 97.1 months.
Results Nuclear BCL9 protein expression was observed in 74 (25.7%) of the 288 HCCs. BCL9 expression was significantly associated with younger age (p=0.038), higher Edmondson grade (p=0.001), microvascular invasion (p=0.013), and intrahepatic metastasis (p=0.017). Based on univariate analyses, BCL9 expression showed an unfavorable influence on both disease-free survival (DFS, p=0.012) and disease-specific survival (DSS, p=0.032). Multivariate analyses revealed that higher Barcelona Clinic Liver Cancer stage was an independent predictor of both shorter DFS (p<0.001) and shorter DSS (p<0.001). BCL9 expression tended to be an independent predictor of shorter DFS (p=0.078).
Conclusions BCL9 protein expression might be a marker of shorter DFS in HCC patients after curative hepatectomy.
-
Citations
Citations to this article as recorded by- BCL9 as a Key Player in Wnt/β-catenin Signaling: Implications for Osteogenesis, Tissue Repair, and Oncology
Yupeng Nie, Rixu Liu, Haoyang Sun, Yongchang Yao
Applied Biochemistry and Biotechnology.2026; 198(1): 63. CrossRef - The Wnt-dependent and Wnt-independent functions of BCL9 in development, tumorigenesis, and immunity: Implications in therapeutic opportunities
Minjie Wu, Heng Dong, Chao Xu, Mengqing Sun, Haojin Gao, Fangtian Bu, Jianxiang Chen
Genes & Diseases.2024; 11(2): 701. CrossRef - The role of BCL9 genetic variation as a biomarker for hepatitis C-related hepatocellular carcinoma in Egyptian patients
Eman Abd El Razek Abbas, Ahmed Barakat Barakat, Mohamed Hassany, Samar Samir Youssef
Journal of Genetic Engineering and Biotechnology.2022; 20(1): 4. CrossRef - Molecular Targets and Signaling Pathways of microRNA-122 in Hepatocellular Carcinoma
Kwang-Hoon Chun
Pharmaceutics.2022; 14(7): 1380. CrossRef - Wnt/β-Catenin Signalling and Its Cofactor BCL9L Have an Oncogenic Effect in Bladder Cancer Cells
Roland Kotolloshi, Mieczyslaw Gajda, Marc-Oliver Grimm, Daniel Steinbach
International Journal of Molecular Sciences.2022; 23(10): 5319. CrossRef - Bcl9 Depletion Modulates Endothelial Cell in Tumor Immune Microenvironment in Colorectal Cancer Tumor
Zhuang Wei, Mei Feng, Zhongen Wu, Shuru Shen, Di Zhu
Frontiers in Oncology.2021;[Epub] CrossRef - Wnt Signaling Pathway Is among the Drivers of Liver Metastasis
Ivana Samaržija
Livers.2021; 1(4): 180. CrossRef - Nuclear Expression of Pygo2 Correlates with Poorly Differentiated State Involving c-Myc, PCNA and Bcl9 in Myanmar Hepatocellular Carcinoma
Myo Win Htun, Yasuaki Shibata, Kyaw Soe, Takehiko Koji
ACTA HISTOCHEMICA ET CYTOCHEMICA.2021; 54(6): 195. CrossRef - Wnt status-dependent oncogenic role of BCL9 and BCL9L in hepatocellular carcinoma
Nicole Huge, Maria Sandbothe, Anna K. Schröder, Amelie Stalke, Marlies Eilers, Vera Schäffer, Brigitte Schlegelberger, Thomas Illig, Beate Vajen, Britta Skawran
Hepatology International.2020; 14(3): 373. CrossRef - Structure and function of Pygo in organ development dependent and independent Wnt signalling
Yan Shi, Xiushan Wu, Shuoji Zhu, Huanlei Huang, Jian Zhuang, Haiyun Yuan, Wuzhou Yuan, Ping Zhu
Biochemical Society Transactions.2020; 48(4): 1781. CrossRef - BCL9/BCL9L in hepatocellular carcinoma: will it or Wnt it be the next therapeutic target?
Akshata Moghe, Satdarshan P. Monga
Hepatology International.2020; 14(4): 460. CrossRef - Loss of BCL9/9l suppresses Wnt driven tumourigenesis in models that recapitulate human cancer
David M. Gay, Rachel A. Ridgway, Miryam Müller, Michael C. Hodder, Ann Hedley, William Clark, Joshua D. Leach, Rene Jackstadt, Colin Nixon, David J. Huels, Andrew D. Campbell, Thomas G. Bird, Owen J. Sansom
Nature Communications.2019;[Epub] CrossRef - Immunohistochemical Mapping of Bcl9 Using Two Antibodies that Recognize Different Epitopes Is Useful to Characterize Juvenile Development of Hepatocellular Carcinoma in Myanmar
Myat Thu Soe, Yasuaki Shibata, Myo Win Htun, Kuniko Abe, Kyaw Soe, Nay Win Than, Thann Lwin, Myat Phone Kyaw, Takehiko Koji
ACTA HISTOCHEMICA ET CYTOCHEMICA.2019; 52(1): 9. CrossRef - Low BCL9 expression inhibited ovarian epithelial malignant tumor progression by decreasing proliferation, migration, and increasing apoptosis to cancer cells
Jing Wang, Mingjun Zheng, Liancheng Zhu, Lu Deng, Xiao Li, Linging Gao, Caixia Wang, Huimin Wang, Juanjuan Liu, Bei Lin
Cancer Cell International.2019;[Epub] CrossRef - SOX7 Suppresses Wnt Signaling by Disrupting β-Catenin/BCL9 Interaction
Rong Fan, HaiYan He, Wang Yao, YanFeng Zhu, XunJie Zhou, MingTai Gui, Jing Lu, Hao Xi, ZhongLong Deng, Min Fan
DNA and Cell Biology.2018; 37(2): 126. CrossRef - Hypoxia activates Wnt/β-catenin signaling by regulating the expression of BCL9 in human hepatocellular carcinoma
Wei Xu, Wang Zhou, Mo Cheng, Jing Wang, Zhian Liu, Shaohui He, Xiangji Luo, Wending Huang, Tianrui Chen, Wangjun Yan, Jianru Xiao
Scientific Reports.2017;[Epub] CrossRef - Hepatocellular carcinoma biology predicts survival outcome after liver transplantation in the USA
Mohamed Abd El-Fattah
Indian Journal of Gastroenterology.2017; 36(2): 117. CrossRef - miR-30a acts as a tumor suppressor by double-targeting COX-2 and BCL9 in H. pylori gastric cancer models
Xuan Liu, Qing Ji, Chengcheng Zhang, Xiaowei Liu, Yanna Liu, Ningning Liu, Hua Sui, Lihong Zhou, Songpo Wang, Qi Li
Scientific Reports.2017;[Epub] CrossRef - BCL9, a coactivator for Wnt/β-catenin transcription, is targeted by miR-30c and is associated with prostate cancer progression
XIAO-HUI LING, ZHI-YUN CHEN, HONG-WEI LUO, ZE-ZHEN LIU, YING-KE LIANG, GUAN-XING CHEN, FU-NENG JIANG, WEI-DE ZHONG
Oncology Letters.2016; 11(3): 2001. CrossRef
- BCL9 as a Key Player in Wnt/β-catenin Signaling: Implications for Osteogenesis, Tissue Repair, and Oncology
- CHD1L Is a Marker for Poor Prognosis of Hepatocellular Carcinoma after Surgical Resection
- Jiyeon Hyeon, Soomin Ahn, Cheol-Keun Park
- Korean J Pathol. 2013;47(1):9-15. Published online February 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.1.9
- 9,574 View
- 71 Download
- 24 Crossref
-
 Abstract
Abstract
 PDF
PDF Background The gene for chromodomain helicase/ATPase DNA binding protein 1-like (
CHD1L ) was recently identified as a target oncogene within the 1q21 amplicon, which occurs in 46% to 86% of primary hepatocellular carcinoma (HCC) cases. However, the prognostic significance of CHD1L in HCC remains uncertain. In this study, we investigated the roles of CHD1L in the prognosis of HCC.Methods We investigated the expressions of CHD1L in tumor tissue microarrays of 281 primary HCC patients who underwent surgical resection using immunohistochemistry. Prognostic factors of HCC were examined by univariate and multivariate analyses. The median follow-up period was 75.6 months.
Results CHD1L expression was observed in 48 of the 281 HCCs (17.1%). CHD1L expression was associated with a younger age (p=0.033), higher Edmondson grade (p=0.019), microvascular invasion (p<0.001), major portal vein invasion (p=0.037), higher American Joint Committee on Cancer T stage (p=0.001), lower albumin level (p=0.047), and higher α-fetoprotein level (p=0.002). Multivariate analyses revealed that CHD1L expression (p=0.027), Edmondson grade III (p=0.034), and higher Barcelona Clinic Liver Cancer stage (p<0.001) were independent predictors of shorter disease-free survival.
Conclusions CHD1L expression might be a prognostic marker of shorter disease-free survival in HCC patients after surgical resection.
-
Citations
Citations to this article as recorded by- High Expression of CHD1L, a Potent Oncogene Is Associated With Aggressive Head and Neck Cancer and Poor Survival Outcome
Aishvarya Rukmani Panayappan, Chandra Pandi, Vijayashree Priyadharshini Jayaseelan, Paramasivam Arumugam
Journal of Oral Pathology & Medicine.2026;[Epub] CrossRef - Targeted Inhibition of CHD1L by OTI-611 Reprograms Chemotherapy and Targeted Therapy-Induced Cell Cycle Arrest and Suppresses Proliferation to Produce Synergistic Antitumor Effects in Breast and Colorectal Cancer
Hector Esquer, Qiong Zhou, Daniel V. LaBarbera
Cells.2025; 14(5): 318. CrossRef - CHD1L in cancer and beyond: structure, oncogenic functions, and therapeutic potential
Sophia Clune, Paul Awolade, Hector Esquer, Qiong Zhou, Daniel V. LaBarbera
Journal of Experimental & Clinical Cancer Research.2025;[Epub] CrossRef - The validation of new CHD1L inhibitors as a therapeutic strategy for cancer
Sophia Clune, Paul Awolade, Qiong Zhou, Hector Esquer, Brock Matter, Jeffrey T. Kearns, Timothy Kellett, Damilola Caleb Akintayo, Uday B. Kompella, Daniel V. LaBarbera
Biomedicine & Pharmacotherapy.2024; 170: 116037. CrossRef - Role of pelitinib in the regulation of migration and invasion of hepatocellular carcinoma cells via inhibition of Twist1
Sewoong Lee, Eunjeong Kang, Unju Lee, Sayeon Cho
BMC Cancer.2023;[Epub] CrossRef - Design, Synthesis, and Biological Evaluation of the First Inhibitors of Oncogenic CHD1L
Brett J. Prigaro, Hector Esquer, Qiong Zhou, Laura A. Pike, Paul Awolade, Xin-He Lai, Adedoyin D. Abraham, Joshua M. Abbott, Brock Matter, Uday B. Kompella, Wells A. Messersmith, Daniel L. Gustafson, Daniel V. LaBarbera
Journal of Medicinal Chemistry.2022; 65(5): 3943. CrossRef - Diversity roles of CHD1L in normal cell function and tumorigenesis
Xifeng Xiong, Xudong Lai, Aiguo Li, Zhihe Liu, Ningfang Ma
Biomarker Research.2021;[Epub] CrossRef - Elevated serum alpha-fetoprotein levels are associated with poor prognosis of hepatocellular carcinoma after surgical resection: A systematic review and meta-analysis
Hong-Lin Chen, Yu-Hua Chen, Lin Du, Yi-Ping Song, Bin Zhu
Arab Journal of Gastroenterology.2021; 22(1): 12. CrossRef - Genome-wide scanning for CHD1L gene in papillary thyroid carcinoma complicated with type 2 diabetes mellitus
Y. Y. Kang, J. J. Li, J. X. Sun, J. X. Wei, C. Ding, C. L. Shi, G. Wu, K. Li, Y. F. Ma, Y. Sun, H. Qiao
Clinical and Translational Oncology.2021; 23(12): 2536. CrossRef - The high expression of CHD1L and its clinical significance in human solid tumors
Long Zhang, Yufen Jiang, Panpan Jiao, Xiaohong Deng, Yuancai Xie
Medicine.2021; 100(10): e24851. CrossRef - Clinical Significance of Trk Receptor Expression as a New Therapeutic Target in Hepatocellular Carcinoma
Sangjoon Choi, Sujin Park, Yoon Ah Cho, Cheol-Keun Park, Sang Yun Ha
Pathology & Oncology Research.2020; 26(4): 2587. CrossRef - Hepatocyte ploidy and pathological mutations in hepatocellular carcinoma: impact on oncogenesis and therapeutics
Taiji Yamazoe, Taizo Mori, Sachiyo Yoshio, Tatsuya Kanto
Global Health & Medicine.2020; 2(5): 273. CrossRef - First-in-Class Inhibitors of Oncogenic CHD1L with Preclinical Activity against Colorectal Cancer
Joshua M. Abbott, Qiong Zhou, Hector Esquer, Laura Pike, Travis P. Broneske, Sébastien Rinaldetti, Adedoyin D. Abraham, Dominique A. Ramirez, Paul J. Lunghofer, Todd M. Pitts, Daniel P. Regan, Aik Choon Tan, Daniel L. Gustafson, Wells A. Messersmith, Dani
Molecular Cancer Therapeutics.2020; 19(8): 1598. CrossRef - Prognostic role of chromodomain helicase DNA binding protein 1-like protein in human solid cancers
Wanwei Liu, Jiwei Xu, Caiyun Zhang
Medicine.2018; 97(29): e11522. CrossRef - CHD1L Expression Increases Tumor Progression and Acts as a Predictive Biomarker for Poor Prognosis in Pancreatic Cancer
Chuan Liu, Xiaowei Fu, Zhiwei Zhong, Jing Zhang, Haiyan Mou, Qiong Wu, Tianle Sheng, Bo Huang, Yeqing Zou
Digestive Diseases and Sciences.2017; 62(9): 2376. CrossRef - Overexpression of CHD1L is associated with poor survival and aggressive tumor biology in esophageal carcinoma
Ze-Han Liu, Qi Zhang, Yi-Jie Ding, Ying-Hui Ren, Hui-Peng Yang, Qing Xi, Ying-Nan Cheng, Guo-Lin Miao, Hong-Kun Liu, Cai-Xia Li, Wen-Qiang Yan, Yan Li, Zhenyi Xue, Lijuan Zhang, Xin-Ye Li, Chen-Long Zhao, Yurong Da, Xian-Zhong Wu, Jun-Qiang Chen, Rongxin
Oncotarget.2017; 8(43): 74178. CrossRef - CHD1L Regulates Cell Cycle, Apoptosis, and Migration in Glioma
Jie Sun, Li Zhang, Hongyu Zhao, Xiaojun Qiu, Wenjuan Chen, Donglin Wang, Na Ban, Shaochen Fan, Chaoyan Shen, Xiaojie Xia, Bin Ji, Yuchan Wang
Cellular and Molecular Neurobiology.2016; 36(4): 565. CrossRef - Expression of DBC1 is associated with poor prognosis in hepatitis virus-related hepatocellular carcinoma
Sang Yun Ha, Jeong Hoon Kim, Jung Wook Yang, Hyunsik Bae, Hae Yon Cho, Cheol-Keun Park
Pathology - Research and Practice.2016; 212(7): 616. CrossRef - The Overexpression of CCAR1 in Hepatocellular Carcinoma Associates with Poor Prognosis
Sang Yun Ha, Jeong Hoon Kim, Jung Wook Yang, Jimin Kim, Binnari Kim, Cheol-Keun Park
Cancer Research and Treatment.2016; 48(3): 1065. CrossRef - Genetic alterations in hepatocellular carcinoma: An update
Zhao-Shan Niu, Xiao-Jun Niu, Wen-Hong Wang
World Journal of Gastroenterology.2016; 22(41): 9069. CrossRef - CHD1L is a novel independent prognostic factor for gastric cancer
Z. Su, J. Zhao, G. Xian, W. Geng, Z. Rong, Y. Wu, C. Qin
Clinical and Translational Oncology.2014; 16(8): 702. CrossRef - Presence of CHD1L Over-Expression Is Associated with Aggressive Tumor Biology and Is a Novel Prognostic Biomarker for Patient Survival in Human Breast Cancer
Jiayi Wu, Yu Zong, Xiaochun Fei, Xiaosong Chen, Ou Huang, Jianrong He, Weiguo Chen, Yafen Li, Kunwei Shen, Li Zhu, Xin-Yuan Guan
PLoS ONE.2014; 9(8): e98673. CrossRef - CHD1L: a novel oncogene
Wen Cheng, Yun Su, Feng Xu
Molecular Cancer.2013; 12(1): 170. CrossRef - Expression of CHD1L in bladder cancer and its influence on prognosis and survival
Feng Tian, Feng Xu, Zheng-Yu Zhang, Jing-Ping Ge, Zhi-Feng Wei, Xiao-Feng Xu, Wen Cheng
Tumor Biology.2013; 34(6): 3687. CrossRef
- High Expression of CHD1L, a Potent Oncogene Is Associated With Aggressive Head and Neck Cancer and Poor Survival Outcome
- The Histologic Cut-off Point for Adjacent and Remote Non-neoplastic Liver Parenchyma of Hepatocellular Carcinoma in Chronic Hepatitis B Patients
- Hae Yoen Jung, Soo Hee Kim, Jin Jing, Jae Moon Gwak, Chul Ju Han, Ja-June Jang, Kyoung-Bun Lee
- Korean J Pathol. 2012;46(4):349-358. Published online August 23, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.4.349
- 9,227 View
- 56 Download
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Background The molecular profile of peritumoral non-neoplastic liver parenchyma (PNLP) has recently been suggested as predictive factor of early and late recurrence of hepatocellular carcinoma (HCC). However, there is no definite cut-off point for tumor-free PNLP in terms of either histological or molecular changes. Therefore, our aim is to determine the numerical cut-off point for separating adjacent PNLP and remote PNLP in histopathologic perspective.
Methods Peritumoral tissues from 20 resected HCC patients were sampled from 0 to 40 mm distance from the tumor border (divided into 5-mm columns). Histopathologic parameters such as necroinflammatory activity, fibrosis, bile ductular reaction, hepatic venulitis, peliosis, and steatosis were compared between each column.
Results The morphologic changes just adjacent to the tumor were notably severe and faded with distance. The parenchyma within 10 mm of the tumor showed significantly severe inflammation, fibrosis, peliosis and hepatic venulitis compared with those from farther areas. The histopathologic changes of the parenchyma became stable beyond 20 mm.
Conclusions Results of this study revealed that the parenchyma within 10 mm distance from the tumor, or adjacent PNLP, has histopathologic changes that are directly affected by the tumor, and the parenchyma beyond 20 mm as the remote PNLP without tumor effect.
-
Citations
Citations to this article as recorded by- Multi-omics profiling reveals cholic acid-mediated immunosuppression driven by peritumoral ductular reactions in hepatocellular carcinoma
Qianhui Xu, Hang Chen, Ganggang Wang, Xiaodong Wang, JieYi Shi, Yifei Cheng, Yanan Xu, Sainan Ma, Siqi Guo, Xiyang Liu, Qiang Gao, Guohe Song
Cancer Letters.2026; 646: 218393. CrossRef - Does very high alpha-fetoprotein affect very early hepatocellular carcinoma receiving hepatectomy?
Hong-Shiue Chou, Chen-Fang Lee, Hao-Chien Hung, Yin Lai, Jin-Chiao Lee, Yu-Chao Wang, Chih-Hsien Cheng, Tsung-Han Wu, Ting-Jung Wu, Kun-Ming Chan, Wei-Chen Lee
Langenbeck's Archives of Surgery.2025;[Epub] CrossRef - Evaluation of the effects of dimethyl fumarate on transforming growth factor beta levels in the liver of rats with bile duct ligation-induced cholestasis
Hannaneh Vossoughi, Pejman Mortazavi, Mahsa Ale-Ebrahim, Razieh Hosseini
Toxicology Reports.2025; 15: 102115. CrossRef - Peritumoral histopathologic findings in patients with chronic viral hepatitis‐associated hepatocellular carcinoma
Burcin Pehlivanoglu, Anil Aysal, Cihan Agalar, Tufan Egeli, Mucahit Ozbilgin, Tarkan Unek, Tugba Unek, Ilhan Oztop, Ozgul Sagol
APMIS.2022; 130(6): 346. CrossRef - Prognostic value of non-invasive fibrosis indices post-curative resection in hepatitis-B-associated hepatocellular carcinoma patients
Ting-Ting Zhang, Si-Si Ye, Jun Liang, Li Bai
Experimental Biology and Medicine.2020; 245(8): 703. CrossRef - Evaluation of Peritumoral Fibrosis in Metastatic Colorectal Adenocarcinoma to the Liver Using Digital Image Analysis
Kevin M Waters, Tricia R Cottrell, Sepideh Besharati, Qingfeng Zhu, Robert A Anders
American Journal of Clinical Pathology.2019; 151(2): 226. CrossRef - Fibrosis-4 Model Influences Results of Patients with Hepatocellular Carcinoma Undergoing Hepatectomy
Haiqing Wang, Aixiang Liu, Wentao Bo, Xielin Feng, Yong Hu, Lang Tian, Hui Zhang, Xiaoli Tang, Lixia Zhang
BioMed Research International.2018; 2018: 1. CrossRef - Forns index predicts recurrence and death in patients with hepatitis B‐related hepatocellular carcinoma after curative resection
Won‐Mook Choi, Jeong‐Hoon Lee, Hongkeun Ahn, Hyeki Cho, Young Youn Cho, Minjong Lee, Jeong‐ju Yoo, Yuri Cho, Dong Hyeon Lee, Yun Bin Lee, Eun Ju Cho, Su Jong Yu, Nam‐Joon Yi, Kwang‐Woong Lee, Yoon Jun Kim, Jung‐Hwan Yoon, Kyung‐Suk Suh, Chung Yong Kim, Hy
Liver International.2015; 35(8): 1992. CrossRef - Renal Histologic Parameters Influencing Postoperative Renal Function in Renal Cell Carcinoma Patients
Myoung Ju Koh, Beom Jin Lim, Kyu Hun Choi, Yon Hee Kim, Hyeon Joo Jeong
Korean Journal of Pathology.2013; 47(6): 557. CrossRef
- Multi-omics profiling reveals cholic acid-mediated immunosuppression driven by peritumoral ductular reactions in hepatocellular carcinoma
- Fine Needle Aspiration Cytology of hepatocellular Carcinoma: A Study on 247 Cases.
- Kwang Gil Lee, Jong Tae Lee, Soo Im Choi, Chan II Park
- J Pathol Transl Med. 1990;1(1):1-17.
- 42,763 View
- 91 Download
-
 Abstract
Abstract
 PDF
PDF - Hepatocellular carcinoma(HCC) is malignant tumor frequently occurring in Koreans. There have been few reports regarding the cytologic findings of fine needle aspiration(FNA) of HCC. Most have suggested a diagnostic problem in the cytology distinguishing HCC from some benign hepatic lesion-for example, a regeneration nodule in cirrhosis and liver cell adenoma. In spite of its high frequency in Korea, no cytologic study has been reported, concerning the FNA of HCC. In an attempt to achieve cytologic criteria for the diagnosis of HCC, the authors studied retrospectively cytopathologic findings of 247 cases of HCC. These cases were confirmed either by histologic examination including lobectomy, biopsy, or cell block material, or, when tissue diagnosis was unavailable, by a high serum alpha-fetoprotein level(over 400 I. U.). All aspiration smears were stained by the Papainicolaou method. In each case, the smears were analyzed for cell patterns and various cytomorphology of the tumor cells. The smear background was assessed for the presence of tumor cell necrosis and inflammatory components and compared to that of metastatic carcinomas. The cell patterns were classified as trabecular, acinar, dispersed, and irregular. The cytologic parameters analyzed included the degree of nuclear atypia and the presence of mitoses, intranuclear cytoplasmic inclusions, nucleolar prominency, endothelial lining, multinucleated giant cells, eosinophilc, globules bile and Mallory body. Most of the FNA of HCC showed markedly cellular smears. The tumor cells were most frequently arranged in a trabecular pattern(80.3%). The irregular(12.6%), the acinar(5.5%), and the dispersed patterns(1.7%) followed in decreasing frequency. Individual hepatoma cells were larger than normal liver cells. However, they had morphologic features characteristic of the hepatic cells : the cells were round or polygonal, their cytoplasm was abundant and granular with eosinophilic or amphophilic stainability, and their nuclei were round to oval, located centrally, and tended to have prominent nucleoli. Anaplasia and pleomorphism of tumor cells were generally mild to moderate. These findings existed even in very well differentiated cases. Mitotic figures were present in about 85% of the cases. Prominent nucleoli were observed only in about half the cases. The frequency of other cytologic features was as follows : intranuclear cytoplasmic inclusion in 86.8% ; endothelial lining in 56.1% ; bile in 19.8% ; and giant cells in 60.1%. Clear cells were often present in 11.7%, Most aspiration smears of HCC displayed clean background without necrosis or inflammatory material in contrast to the dirty, necrotic background of metastatic cancers and cholangiocarcinomas. Based on the above mentioned features, it is suqqested that the cytologic critieria most important for the diagnosis of HCC include a markedly cellular smear, trabecular pattern. hepatocytoid appearance of tumor cells, endothelial lining, the presence of bile, giant cells, intranuclear cytoplasmic inclusions, and prominent nucleoli, Among these, trabecular pattern, endothelial lining, giant cells and clean smear background are points to be considered in differentiating HCC from metastatic and cholangiocellular carcinoma.
- Fine Needle Aspiration Cytology of Hepatoblastoma: Report of Two Cases.
- Young Nyun Park, Kwang Gil Lee, Chan II Park
- J Pathol Transl Med. 1990;1(1):98-102.
- 2,204 View
- 35 Download
-
 Abstract
Abstract
 PDF
PDF - Hepatoblastoma(HB) is a rare embryonic malignant tumor of the liver. Most morphological studies on HB have limited to the histological characteristics and only 3 cases of HB have been described in the cytology literature. We present 2 cases of HB occurring in children aged 1 year and 3 years, respectively. The distinctive cytologic features of fine needle aspiration of HB were clusters of tumor cells showing acinar and trabecular pattern, smaller tumor cells with a high nuclear-cytoplasmic ratio and hyperchromatic nuclei having prominent nucleoli, and the presence of extramedullary hematopoiesis and osteoid material. These features were also found in the cell block and the biopsy specimen, and appeared very useful in the differentiation of HB from hepatocellular carcinoma.
- Expression of Multidrug Resistance Protein 1 in Human Hepatocellular Carcinoma.
- Yun Kyung Kang
- Korean J Pathol. 2011;45(3):281-289.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.3.281
- 4,566 View
- 28 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Multidrug resistance protein 1 (MDR1) encoded by ATP-binding cassette, sub-family B (Mdr/Tap), member 1 (ABCB1) mediates cross-resistance to antineoplastic drugs, and its expression is related to tumor aggressiveness.
METHODS
MDR1 expression was investigated in 100 hepatocellular carcinomas (HCCs) by immunohistochemical staining. The epigenetic mechanisms underlying ABCB1 transcriptional regulation were investigated in cell lines.
RESULTS
MDR1 was normally localized in the bile canalicular surface of the hepatocytes. Among 100 HCCs, 45 showed canalicular/luminal (CL) staining similar to the normal pattern, another 45 displayed membranous/cytoplasmic (MC) overexpression, and the remaining 10 revealed loss of expression. MC pattern or null staining of HCCs correlated with a higher histological grade and had a poorer prognosis than HCCs with a CL pattern (p<0.05). They also tended to have a poor prognosis by multivariate survival analysis. The ABCB1 promoter was hypomethylated regardless of MDR1 expression or ABCB1 mRNA levels in 10 HCC cell lines. Histone deacetylase inhibitor treatment induced ABCB1 upregulation in 4 cell lines with low or moderate ABCB1 levels.
CONCLUSIONS
Our findings suggest that either an increase or a loss of MDR1 expression may contribute to the poor outcome of HCCs; histone deacetylation may be one of the epigenetic mechanisms directing the ABCB1 expression in HCCs. -
Citations
Citations to this article as recorded by- Preferential expression of prostate specific membrane in CD34 labeled Neo-vasculature of Hepatocellular carcinoma: Prognostic and therapeutic potentials
Safaa MM Abd El Khalek, Mona QR Mohammed, Amira M Al Balakosy
Egyptian Journal of Pathology.2023; 43(1): 66. CrossRef
- Preferential expression of prostate specific membrane in CD34 labeled Neo-vasculature of Hepatocellular carcinoma: Prognostic and therapeutic potentials
- Adrenal Cortical Adenoma Developed in Adrenohepatic Fusion, a Mimicry of Hepatocellular Carcinoma: A Case Report.
- Sun A Kim, Young Joo Lee, Kyoung Won Kim, Gyungyub Gong
- Korean J Pathol. 2011;45(2):196-200.
- DOI: https://doi.org/10.4132/KoreanJPathol.2011.45.2.196
- 5,337 View
- 42 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF - Adrenohepatic fusion is the union of the liver and adrenal gland with close intermingling of their respective parenchymal cells. Adrenal cortical adenoma arising in adrenohepatic fusion tissue is extremely rare, although adrenohepatic fusion itself is relatively common. Here we report a case of a 59-year-old man with a mass in the right lobe of his liver. The mass showed slight hyperattenuation during arterial phase and hypoattenuation during portal phase on dynamic computed tomography with contrast enhancement. On pathology, the mass consisted of round to polygonal cells with clear microvesicular or eosinophilic cytoplasm, arranged in nests or in a trabecular pattern. The tumor cells were positive for inhibin and melan-A, but negative for Hep Par-1. In the periphery of the mass, adrenohepatic fusion was identified between the liver and adrenal gland, and was simultaneously resected with the mass. We report this rare case, and discuss its clinical implications, especially the differential diagnosis with hepatocellular carcinoma.
-
Citations
Citations to this article as recorded by- An intrahepatic adrenal adenoma mimicking hepatocellular carcinoma: A case report and literature review
Cheng-Ju Yang, Cheng-Ming Peng
Formosan Journal of Surgery.2025; 58(5): 222. CrossRef - Adrenal cortical adenoma arising in an adreno-hepatic fusion: Case report and literature review of a potential diagnostic pitfall
Adam Stenman, Ivan Shabo, Jan Zedenius, C. Christofer Juhlin
Human Pathology Reports.2022; 29: 300656. CrossRef - Intrahepatic adrenocortical adenoma arising from adrenohepatic fusion mimicking hepatic malignancy
Yong Soo Cho, Jin Woong Kim, Hyun Ju Seon, Ju-Yeon Cho, Jun-Hee Park, Hyung Joong Kim, Yoo Duk Choi, Young Hoe Hur
Medicine.2019; 98(23): e15901. CrossRef - Direct and indirect imaging features of adrenohepatic fusion
Jung Jae Park, Byung Kwan Park, Chan Kyo Kim
Abdominal Radiology.2016; 41(2): 377. CrossRef
- An intrahepatic adrenal adenoma mimicking hepatocellular carcinoma: A case report and literature review
- The Expression of Apolipoprotein D in Hepatocellular Carcinoma.
- Hongxiu Han, Chan Kum Park
- Korean J Pathol. 2010;44(2):187-190.
- DOI: https://doi.org/10.4132/KoreanJPathol.2010.44.2.187
- 3,811 View
- 27 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Apolipoprotein D (Apo D) has recently been identified as a novel tumor suppressor gene. Apo D may have a profound effect on the carcinogenesis and progression of hepatocellular carcinoma. This study was designed to evaluate the expression of Apo D in hepatocellular carcinoma and to investigate the relationship between the expression of Apo D and the clinicopathological characteristics and the patients' survival.
METHODS
An immunohistochemical study was performed on the tumors and tissues from 43 hepatocellular carcinoma (HCC) patients with controls to determine the expression of Apo D protein.
RESULTS
Our data showed that a higher expression of Apo D was seen in 10 of 43 cases (23.3%), while a lower and no expression of Apo D was observed in 28 of 43 cases (65.1%) and 5 of 43 cases (11.6%), respectively. A reduced expression of Apo D was correlated with the tumor stage (p = 0.037) and tumor size (p = 0.017). However, the patients' 5-year survival was not associated with the expression of Apo D (p = 0.903).
CONCLUSIONS
The results suggest that a reduced Apo D protein expression may play an important role in HCC progression as associated with the tumor stage and size, but it does not affect the survival of HCC patients.
- Hepatoid Thymic Carcinoma: A Case Report.
- Jeong Hyeon Lee, Hyunchul Kim, Yang Seok Chae, Nam Hee Won, Jong Sang Choi, Chul Hwan Kim
- Korean J Pathol. 2009;43(6):562-565.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.6.562
- 4,439 View
- 32 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - We report here on a rare case of hepatoid thymic carcinoma in a 34-year-old man. The patient complained of a high fever and headache, and a 6.6cm-sized anterior mediastinal mass was found on chest computed tomography (CT). There was no hepatic mass seen on abdominal CT. The resected mass consisted of epithelioid cells with abundant eosinophilic cytoplasm, pleomorphic vesicular nuclei and prominent nucleoli, and the mass was surrounded by thymic tissue. The tumor cells were immunopositive for cytokeratin 7, alpha-1-antitrypsin, hepatocyte staining, and epithelial membrane antigen, but they were negative for CD5, alpha-fetoprotein (AFP) and placental alkaline phosphatase, and this all led to a diagnosis of hepatoid thymic carcinoma rather than hepatoid yolk sac tumor. This entity should be included in the differential diagnosis of epithelioid thymic tumors.
-
Citations
Citations to this article as recorded by- Hepatoid thymic carcinoma in a polycythemia vera patient treated with ropeginterferon Alfa-2b: Clinical, histopathological and molecular correlates
Giuseppe G. Loscocco, Margherita Vannucchi, Raffaella Santi, Andrea Amorosi, Stefania Scarpino, Maria Chiara Siciliano, Paola Guglielmelli, Claudio Tripodo, Arianna Di Napoli, Alessandro M. Vannucchi
Pathology - Research and Practice.2024; 263: 155648. CrossRef
- Hepatoid thymic carcinoma in a polycythemia vera patient treated with ropeginterferon Alfa-2b: Clinical, histopathological and molecular correlates
- Enhanced Protein Expression of Signal Transducer and Activator of Transcription 3 and Protein Kinase Substrate p36 in Hepatocellular Carcinoma.
- Hongxiu Han, Si Hyong Jang, Chan Kum Park
- Korean J Pathol. 2009;43(5):393-399.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.5.393
- 3,596 View
- 28 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Signal transducers and activators of transcription 3 (STAT3) and protein kinase substrate p36 may be involved in cell proliferation, differentiation and growth.
METHODS
Immunohistochemistry for STAT3 and p36 was performed in 46 patients with hepatocellular carcinoma (HCC).
RESULTS
STAT3 staining was present in the cytoplasm and/or nucleus, while p36 staining was present in the nucleus. STAT3 and p36 expression occurred in 78.3% (36/46) and 47.8% (22/46) of HCC patients, respectively. However, no correlation was found between STAT3 and p36 protein expression (p>0.05). Enhanced expression of STAT3 was negatively correlated with portal vein invasion (p=0.033). Expression of STAT3 in the nucleus was correlated with tumor grade (p=0.004). Enhanced expression of p36 was correlated with tumor grade (p=0.031). HCC was correlated with HBV infection (p=0.032). The patients'5-year survival was related to expression of p36 (p=0.044), but not to total STAT3 or nuclear STAT3 (p>0.05).
CONCLUSIONS
The enhanced expression of STAT3 in the nucleus and the enhanced expression of p36 are associated with the aggressive phenotype of HCC. Enhanced p36 expression may contribute to poor survival of patients with HCC.
- The Expressions of Nerve Growth Factor and Its Receptor p75NGFR in Hepatocellular Carcinoma: Their Relation with the Clinicopathologic Factors.
- Woo Sung Moon, Kyu Yun Jang, Myoung Ja Chung, Myoung Jae Kang, Dong Geun Lee, Ho Lee, Ho Sung Park
- Korean J Pathol. 2009;43(2):145-151.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.2.145
- 4,929 View
- 24 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Nerve growth factor (NGF) has been suggested to participate in tumor progression and it can interact with its receptor p75NGFR. In the present study, we investigated the expressions of NGF and p75NGFR in hepatocellular carcinoma (HCC).
METHODS
We performed immunohistochemistry for NGF, p75NGFR and PCNA in 45 cases of HCCs, and examined the relationships between the clinicopathologic factors and the immunohistochemical results.
RESULTS
NGF was detected in 84.4% (38/45) of the tumor cells and in 64.4% (29/45) of the non-tumorous hepatocytes. Furthermore, a NGF expression was present in 28.9% (13/45) of the endothelial cells in the HCCs, but in 80% (36/45) of the endothelial cells in the non-tumor liver tissue. The tumor cells were negative for p75NGFR in all the HCCs. Although a p75NGFR expression was present in all the nerve fibers in the non-tumor liver tissues, it was markedly reduced (42.2%; 19/45) in the HCCs and a p75NGFR expression was observed at the sinusoids or around the large vessels. The HCCs expressing NGF, either in the tumor cells or the endothelial cells, showed a larger size than those HCCs that didn't express NGF. The NGF positive tumors showed a tendency toward a higher PCNA-labeling index than did the negative tumors.
CONCLUSIONS
The changed localization of the NGF expression and the decreased expression of p75NGFR are associated with hepatic carcinogenesis. We suggest that a NGF expression may contribute to the progression of HCC. -
Citations
Citations to this article as recorded by- Expression of nerve growth factor and heme oxygenase-1 predict poor survival of breast carcinoma patients
Sang Jae Noh, Jun Sang Bae, Urangoo Jamiyandorj, Ho Sung Park, Keun Sang Kwon, Sung Hoo Jung, Hyun Jo Youn, Ho Lee, Byung-Hyun Park, Myoung Ja Chung, Woo Sung Moon, Myoung Jae Kang, Kyu Yun Jang
BMC Cancer.2013;[Epub] CrossRef
- Expression of nerve growth factor and heme oxygenase-1 predict poor survival of breast carcinoma patients
- Gastric Adenocarcinoma with Coexistent Hepatoid Adenocarcinoma and Neuroendocrine Carcinoma: A Case Report.
- Aeri Kim, Sang Woon Kim, Sun Kyo Song, Young Kyung Bae
- Korean J Pathol. 2009;43(1):79-82.
- DOI: https://doi.org/10.4132/KoreanJPathol.2009.43.1.79
- 4,316 View
- 34 Download
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - This report represents a very rare case of a gastric adenocarcinoma that was coexistent with hepatoid adenocarcinoma and neuroendocrine carcinoma. A 77-year-old man was admitted to our hospital due to a huge ulcerofungating mass identified at the proximal body of the stomach. After a pathological diagnosis of the tumor as a poorly differentiated adenocarcinoma was made, the patient underwent a total gastrectomy with lymph node dissection. Microscopically, the tumor consisted of three morphologically distinct components-tubular adenocarcinoma, hepatoid adenocarcinoma and neuroendocrine carcinoma. The hepatoid adenocarcinoma component resembled a hepatocellular carcinoma and produced alpha-fetoprotein. The neuroendocrine carcinoma component was positive for chromogranin and synaptophysin immunostains. This is an example of the diverse morphological and immunophenotypical differentiation of gastric carcinomas.
-
Citations
Citations to this article as recorded by- An Intestinal Type Gastric Neuroendocrine Tumor: A Case Report
Mohammad Abu-Jeyyab, Renata Kakish, Malak Alkatib, Leen Alshawabkeh, Rawan Bani Hamad, Mary Almadani, Ma'wia Santarisi, Mohammad Al-Jafari, Abdulqadir J. Nashwan
Case Reports in Oncology.2023; 16(1): 1113. CrossRef - Gastric adenocarcinoma is concurrent with metastatic neuroendocrine cancer treated with nivolumab and chemotherapy: A case report
Bing Yan, Meiqi Cui, Junhao You, Fang Li, Hui Liu
Molecular and Clinical Oncology.2018;[Epub] CrossRef
- An Intestinal Type Gastric Neuroendocrine Tumor: A Case Report
- The Effects of Transforming Growth Factor beta1 on Apoptosis in Rat Hepatocellular Carcinoma.
- Young Euy Park, Young Hee Choi, Won Yo Lee, Jin Ja Park, Kyung Chan Choi, Hyung Shik Shin
- Korean J Pathol. 1999;33(2):71-79.
- 1,947 View
- 10 Download
-
 Abstract
Abstract
- Based upon the concept that carcinogenesis is associated with apoptosis, specific therapies designed to enhance the susceptibility of cancer cells to undergo apoptosis could be developed. Thus, in this paper, it was designed to investigate whether, using rat animal model with chemical-induced hepatocellular carcinoma, TGF-1 in vivo could induce apoptosis in cancer. The chemical hepatocarcinogenic procedure of Solt-Farber method was used on Sprague-Dawley rats. Experimental groups were divided into group A treated with the standard Solt-Farber regimen of diethylnitrosamine (DEN) and 2-Acetaminofluorene (AAF), group B TGF-, group C TGF-1, and group D adriamycin after hepatocellular carcinoma developed. For detection of apoptotic cells, apoptotic indices were examined by the in situ end DNA labelling method. The expression of proliferating cell nuclear antigen was examined by immunohistochemical staining. Apoptosis of rat hepatocellular carcinoma cells increased significantly to 4.92+/-2.32/HPF in the group C compared with the control group (A) (2.54+/-1.13/HPF; P<0.05). Two distinctly different populations of proliferating hepatocellular carcinoma cells were identified. The cells at G1/S boundary (weak granular staining) increased to 15.75+/-6.19/HPF and 6.45+/-2.93/HPF in the groups C and D, respectively, but decreased to 2.42+/-2.06/HPF in the group B compared with the control group (A) (6.38+/-2.18/HPF; p<0.05). The cells at S phase (strong granular staining) increased to 3.37+/-2.69/HPF in the group B but decreased to 0.32+/-0.47/HPF in the group D (p<0.05). In conclusion, these results indicate that the TGF-1 may be used as an effective anticancer agent.
- Kupffer Cells in Hepatocellular Carcinoma.
- Young Nyun Park, Soon Hee Jung, Chan Il Park
- Korean J Pathol. 1989;23(3):305-310.
- 3,210 View
- 91 Download
-
 Abstract
Abstract
 PDF
PDF - Kupffer cells are tissue macrophages (histiocytes) fixed in hepatie sinusoids. Since malignant hepatocytes are the only tumor parencymal cells of the hepatocellular carcinoma, theoretically there are no Kupffer cells within the hepatocellular carcinoma. To clarify whether it is true or not, 12 cases of hepatocellular carcinoma of the trabecular type with some extents of the non-neoplastic surrounding liver were subjected to immunoperoxidase staining for lysozyme and S-100 protein and the results are as follows. 1) Kupffer cells were stained positively by the immunoperoxidase staining for lysozyme but not for S-100 protein, indicating that they are monocyte derived macrophages. 2) Kupffer cells were also present within the hepatocellular carcinoma, but were 2-7 times fewer within the hepatocellular carcinoma than in the non-neoplastic areas (p<0.05). 3) The non-neoplastic hepatic tissue of patients with serum HBsAg shows a tendency to have more kupffer cells than those without HBsAg.
- Clinicopathologic Features of Early Hepatocellular Carcinoma.
- Chang Ohk Sung, Suk Jin Choi, Cheol Keun Park
- Korean J Pathol. 2004;38(3):138-144.
- 2,509 View
- 23 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Early hepatocellular carcinoma (HCC) is an early stage HCC, and it is sometimes difficult to identify the margins of the cancer nodules in the resected specimens.
METHODS
We studied 22 cases of early HCC to investigate the clinicopathologic features of early stage HCC.
RESULTS
Seven of 22 cases were single HCC, and 15 were multicentric HCC. The average tumor size was 1.34 cm (0.4-2.7 cm). Early HCCs didn't destroy the basic architecture of the liver lobules or pseudolobules and the lesions had an indistinct margin. Most tumors were uniformly composed of well-differentiated cancer tissue that was characterized by an increased cell density and an irregular thin-trabecular pattern. The tumor retained a varying number of portal tracts. There was a replacing growth pattern at the tumor-nontumor boundary without tumor capsule. Three of 22 cases had a "nodule-in-nodule" lesion, and the inner nodules consisted of moderately differentiated HCC without portal tracts. All 22 cases showed no vascular invasion. All 7 patients with single early HCC have survived for the past 11-54 months without any local recurrence. But in one patient with single early HCC, multicentric HCC developed 20 months after surgery.
CONCLUSION
The clinicopathologic features of early HCCs are quite different from those of advanced HCCs. The increased recognition of early HCC during routine clinical practice will contribute to improved patient survival.
- A Study on the Expression of Proliferating Cell Nuclear Antigen and Apoptosis of the Hepatocellular Carcinoma in Human and Hepatitis B Virus X Transgenic Mice.
- Hyung Bae Moon, Dae Yeul Yu, Hyung Ryun Yoo, Byung Joon So, Kwon Mook Chae, Haak Cheol Kim, Ki Jung Yun, Won Cheol Han, Hyang Jeong Jo, Bo Yong Kim
- Korean J Pathol. 2001;35(2):129-136.
- 2,094 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
This experiment was designed to study the cell kinetics of hepatocellular carcinoma (HCC) in both hepatitis B virus X (HBx) transgenic mice and humans.
METHODS
The immunohistochemical stain of proliferating cell nuclear antigen (PCNA) and TdT-mediated dUTP-biotin nick end labeling (TUNEL) assay of apoptosis were used on formalin fixed-paraffin embedded tissues.
RESULTS
PCNA labeling indices (PCNA-LI) in the liver of HBx transgenic mice were markedly increased in HCC (11.3%) compare to the dysplastic areas (1.3%) and in the liver of non-transgenic littermates (0.1%). There was no significant difference of PCNA-LI in the dysplastic areas between HCC developed mice and non-HCC developed mice. Apoptosis labeling indices (Apoptosis-LI) in both the dysplastic areas and HCC of HBx transgenic mice were similar to those of non-transgenic littermates. PCNA-LI was markedly increased in human HCC (28.9%) compare to the background of HCC (2.9%) and the control liver (2.9%). Apoptosis-LI was decreased in human HCC (0.3%) compare to the background of HCC (0.4%) and the control liver (1.0%). Conclusion : There is a marked increase of cell proliferating activity in human HCC and in HCC of HBx transgenic mice, and there is a decrease of apoptosis in human HCC, but not in HCC of HBx transgenic mice.
- Cytologic Diagnosis of Metastatic Hepatocellular Carcinoma by Aspiration Cytology of Sacrum.
- Jungweon Shim, Illhyang Ko
- J Pathol Transl Med. 1990;1(2):179-184.
- 2,205 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - Bone metastasis of hepatocellular carcinoma appears to be peculiar when clinical manifestation of liver disease is not apparent, and initial diagnosis of metastatic hepatocellular carcinoma by fine needle aspiration cytology is rarely obtained. We experienced a case of 45-year-old man with metastatic hepatocellular carcinoma in the sacrum, which was diagnosed by fine needle aspiration cytology. The intrahepatic mass, measuring 1.2 cm in diameter and kept unchanged in size for two years, was never proved to be hepatocellular carcinoma histopathologically. The aspirated neoplastic cells were mostly in sheets, showing abundant acidophilic cytoplasm and large, round. centrally located nuclei with single, prominent acidophilic mucleoti. In the cell block section, diagnosis of metastatic well-differentiated hepatocellular carcinoma was made without difficulty, and definite trabecular fashion with sinusoidal endothelial cell lining was found.
- Rarity of EGFR and c-ErbB-2 Overexpressions in Hepatocellular Carcinoma: An Immunohistochemical Study.
- Woo Sung Moon, Hyun Jin Son, Ho Sung Park, Min Young Park
- Korean J Pathol. 2004;38(4):244-248.
- 2,358 View
- 13 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The overexpression of epidermal growth factor receptor (EGFR) and c-erbB-2 oncogenes has been implicated in the development of many types of cancer. However, the role of EGFR and c-erbB-2 overexpression in hepatocellular carcinoma (HCC) has not been fully elucidated.
METHODS
The aim of this study was to evaluate the immunohistochemical expression of EGFR and c-erbB-2 oncoprotein in a series of 52 HCCs.
RESULTS
All but one of the HCC tumor tissues were negative for EGFR monoclonal antibody, clone H11. All of the HCC tumor tissue samples were negative for EGFR monoclonal antibody, clone 29.1.1. However, strong EGFR immunoreactivity was detected in sinusoidal endothelial cells of HCC in 25 tumors (48%) using EGFR 29.1.1 antibody. The expression of c-erbB-2 was observed in 6% (3/52) of the HCCs. No significant correlation was found between p53 mutation and the expression of c-erbB-2.
CONCLUSION
Our results suggest that both EGFR and c-erbB-2 oncoprotein overexpressions in tumor cells are rare and do not seem to predominantly contribute to the malignant phenotype in HCC.
- Immunohistochemical Localization of Extracellular Matrix Components in Diabetic Nephropathy.
- Seung Sam Paik, Moon Hyang Park
- Korean J Pathol. 1997;31(5):427-435.
- 2,007 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - Normal human glomerular basement membrane (GBM) and mesangial matrix (MM) contain several different basement membrane components in varying degrees. The characteristic morphological and ultrastructural changes in patients with diabetic nephropathy are the thickening of the GBM and the expansion of the MM. In order to investigate the changes of extracellular matrix components in diabetes, the immunohistochemical localization was performed in 17 cases with different degrees using antisera to human collagen types I, III, IV, VI, fibronectin, and laminin. The following results were obtained: 1. The reactivity for collagen IV was increased in expanded MM in the diffuse glomerulosclerosis (GS). With the progression to the nodule formation, collagen IV was prominently decreased in the peripheral area of the nodules. 2. Collagen VI was increased in GBM and MM in the diffuse GS, it was especially prominent in the expanded MM. With the progression to nodule formation, collagen VI was prominently increased in the periphery of the nodules. 3. Interstitial collagen I and III were not stained in many of the cases with the diffuse GS. With the progression to nodule formation, these were slightly expressed. A lamellar pattern of positive reaction was noted at the periphery of the late nodular lesions. 4. Fibronectin was increased in GBM & MM in the diffuse GS, it was especially intense in the MM. With the progression to the nodule formation, the reactivity of antibody to the fibronectin was decreased. 5. Laminin was weakly stained along the GBM & trace in the MM, but was not changed in the nodular GS. In summary, the expanded mesangial matrix in the diffuse GS showed a markedly increased staining for collagen IV, fibronectin and collagen VI. Less intense linear staining for collagen VI, fibronectin, laminin, collagen IV and collagen III was noted along the GBM. In the nodular GS, the composition of the early nodules resembled that of the diffuse GS. However, the late nodular lesion of the nodular GS revealed decreased reactivity for collagen IV and fibronectin at the periphery of the nodule, where collagen VI and interstitial collagen I and III were increased in laminated pattern.
- Analysis of DNA Ploidy Patterns and Nuclear Morphometry in Diethylnitrosamine Induced Hepatocyte Nodules and Hepatocellular Carcinoma of Rats.
- Chan Choi, Myung Kwan Kim, Kwan Mook Chae, Eun Cheol Kim, Hyung Bae Moon
- Korean J Pathol. 1993;27(3):226-234.
- 2,343 View
- 24 Download
-
 Abstract
Abstract
 PDF
PDF - This study was designed to answer the question; (1) How does the DNA ploidy pattern change in hepatocarcinogenesis? (2) How does the nuclear morphology change in hepatocarcinogenesis? Diethylnitrosamine(DEN) (16.5 mg per kg) was subcutaneously injected to female Sprague-Dawley rats(150~200g) by weekly interval for 30 weeks. DNA ploidy and parameters of nuclear morphology were measured by image analyser(IBAS 200, Kontron, FRG). The DNA ploidy pattern was divided into three basic patterns(diploid, polyploid, and aneuploid modes). In 8 cases of saline-injected control rats, the DNA histograms showed all polyploid pattern. Inhepatocyte nodules(hyperplastic nodules), DNA diploidy was the most frequent pattern, being followed by polyploid and aneuploid DNA patterns, contrast to hepatocelular carcinomas in which polyploid DNA pattern was most frequently noted being followed by diploid and aneuploid DNA pattern. Although the nuclei of hepatocytes in hepatocyte nodules and hepatocellular carcinomas were larger and more pleomorphic than those of normal hepatocytes, they were as same as those of normal hepatocytes in regard to nuclear hyperchromasia. DNA content, which was increased in hepatocarcinogenesis, was significantly related to the nuclear area.
- Expression of Fas/Fas Ligand and Its Relationship with Apoptosis in Chemically Induced Preneoplastic Lesions in Rat Liver.
- Hye Jin Lee, Do Youn Park, Kyung Un Choi, Jee Yeon Kim, Chang Hun Lee, Mee Young Sol, Kang Suek Suh
- Korean J Pathol. 2001;35(5):383-390.
- 2,143 View
- 15 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Apoptosis of hepatocytes plays a major role in experimental hepatocarcinogenesis of rats. But sequential change and localization of Fas and Fas ligand (FasL) in preneoplastic lesions and the relationship with apoptosis are not clearly elucidated.
METHODS
We investigated sequential change and localization of Fas/FasL and its relationship to apoptosis in preneoplastic lesions of chemical hepatocarcinogenesis in rats using northern blot analysis, immunohistochemistry and terminal deoxynucleotidyl transferase end labeling (TUNEL) assay.
RESULTS
We found that mRNA of Fas and Fas ligand increased for up to 42 days and 14 days after partial hepatectomy, respectively, and thereafter decreased with time. Fas protein was localized on the cytoplasm of hepatocytes of preneoplastic lesions, as well as on the cytoplasmic membrane of the adjacent liver parenchyme. Fas negative preneoplastic lesions were evident at 42 days after partial hepatectomy. FasL protein was found only in the cytoplasm of hepatocytes of preneoplastic lesions, instead of in the adjacent liver parenchyme. FasL-positive hepatocytes increased with time for up to 14 days after partial hepatectomy and therafter decreased. Also, TUNEL-positive apoptotic cells increased with time and were more numerous in the adjacent liver parenchyme than in the preneoplastic lesions.
CONCLUSIONS
It was suggested that Fas/FasL-mediated apoptosis might be one of the major mechanisms for controlling apoptotic cell death in the promotion stage of chemical hepatocarcinogenesis.
- Immunohistochemical Study of the Expression of p53, Pan-ras, c-erbB-2 and PCNA in N-Nitrosomorpholine(NNM)-Induced Hepatocellular Carcinoma of Rats.
- Ok Kyung Kim, Ryun Jo Shin
- Korean J Pathol. 1995;29(6):727-739.
- 1,818 View
- 14 Download
-
 Abstract
Abstract
 PDF
PDF - The focus of this study was o aialyze the morphologic expression of p53, Pan-ras, c-erbB-2, and PCNA in preneoplastic and neoplastic liver lesions induced with NNM of rats. The development of hepatocellular tumors was investigated by histology and electron microscope in 65 Splague-Dawley rats administered with NNM in drinking water at low dose(5 mg/100 ml) and high dose(20 mg/100 ml). Three types of hepatocytic degeneration glycogenotic, eosinophilic and basophilic changes were followed by the appearance of hepatocellullar carcinoma. Hepatocellular carcinoma was increased in number and size according to NNM dosage and to duration of exposure. The histological classifications of hepatocelular carcinoma wer trabecular type, which was which was the most common, large eosinophilic, small cell, adenocarcinomatous and clear cell type. The expression of p53, Pan-ras, c-erbB-2 PCNA was examined by immunohistochemical stains. Eosinophilic degeneration revealed mild positivity at 18-26 weeks for expression of all oncogenic proteins studied and PCNA, whereas precancerous lesions showed variable expression from negative to moderate positivity on PCNA. Hepatocellular carcinoma lesions showed strong positivity for all stains and increased intensity during experimental period. These may indicate that chemical carcinogen produce hepatic eosinophilic degeneration and preCancerOus lesions by genetic mutation, resulting in hepatocellular carcinoma.
- The Tissue Expression of HBsAg and HBcAg in Hepatocellular Carcinoma and Peritumoral Liver.
- Jee Young Han, Woo Hee Jung, Chae Yoon Chon, Chan Il Park
- Korean J Pathol. 1993;27(4):371-378.
- 2,457 View
- 24 Download
-
 Abstract
Abstract
 PDF
PDF - To evaluate the tissue expression rate and pattenr of HBsAg and HBcAg in tumors and peritumoral livers, an immunohistochemical study was undertaken on 47 surgically resected hepatocellular carcinomas(HCCs). The results are as follows. 1. Patient's sera were positive for HBsAg in 40 cases(85.1%). In the remaining 7 cases, the tumor and peritumoral liver expressed neither HBcAg nor HbSaG, suggesting that they were caused by other etiologies than hepatitis B virus. 2. The peritumoral liver had HBsAg and HBcAg in 95.0% and 27.5% among the 40 cases, respectively. But the tumor expressed HBsAg in 50.0% and HBcAg in none. 3. The expression of HBsAg within the tumor and both HBsAg and HBcAg in the peritumoral liver tended to be more frequent in the pretreated cases before surgery. 4. Edmondson-Steiner grade IV tumors revealed a lower expression rate of HBsAg than the low grade tumors(p<0.05). Incases with cirrhosis at peritumoral tissues, HBcAg was less frequently found than in those without cirrhosis. The majority of tissue HBsAg and HBcAg was represented as groups of positive cells. These results suggest that, during the development and progression of HCCs, the HBcAg containing cells are repeatedly removed and the HBcAg negative cells are selected, because cellular expression of HBcAg is the target of host immune response.
- Expression of ICAM-1 on Short-Term Cultured Human Keratinocytes: Modulation by IFN-gamma, UVB and retinoic acid.
- Bang Hur, Duck Ha Kim, Man Ha Hur
- Korean J Pathol. 1995;29(6):746-755.
- 1,972 View
- 14 Download
-
 Abstract
Abstract
 PDF
PDF - Intercellular adhesion molecule I(ICAM-1; CD 54), a 90 kD glycoprotein, counter-receptor for lymphocyte function-associated antigen-I(LFA-1) on T-cells, is critically important to a wide variety of adhesion-dependent leukocyte functions, including antigen presentation and target cell lysis. Induction of ICAM-1 on the keratinocytes(KCs) is an important regulator in initiation, maintenance, and resolution of cutaneous inflammation, which is modulated with cytokines produced by activated T-lymphocytes. This study was designed to further our understanding on modulation effects of ultraviolet B(UVB), gamma interferon(IFN-;v), and retinoic acid(all trans) upon expression of ICAM-1 on cultured human KCs, with emphasis on their correlation. Cell surface expression of ICAM-1 in cultured human KCs was analyzed with the use of indirect immunofluorescence and fluorescence activating cell sorting(FACS) by flow cytometry. The results of this study were as follows: 1) Expression of ICAM-1 was significantly induced with IFN-,-(20 U/ml)(p<0.005). 2) UVB irradiation of 30mJ/cm2 significantly suppressed ICAM-1 expression of KCs 24 hours after irradiation(p<0.05). However, at 72 hours after irradiation, ICAM-1 expression of KCs was considerably increased in comparison to that of initial phase (24 hours after irradiation). 3) High concentrations(10(-5)M) of retinoic acid reduced UVB-induced expression of ICAM-1 in late phase(72 hours after irradiation), although retinoic acid showed induction effect of ICAM- I expression of KCs. In summary, these results indicate that ICAM- I may contribute to the biphasic effect of UVB on delayed hypersensitivity in vivo. Also, retinoic acid, a vitamin A derivative, may have a cutaneous photoprotective effect through a regulation of UVB-induced ICAM-1 expression on the KCs.
- Cellular Schwannoma Arising in a Facial Nerve.
- Mee Joo, Hye Sung Kim, Yun Kyung Kang, Hye Kyung Lee, Jae Young Park
- Korean J Pathol. 1997;31(7):688-691.
- 2,095 View
- 19 Download
-
 Abstract
Abstract
 PDF
PDF - Cellular schwaninoma is a variant of schwannoma, which is characterized by predominance of cellular Antoni A area, presence of mitotic activity, nuclear hyperchromasia, pleomorphism, and absence of Verocay body. These pathologic features often prompted a misdiagnosis of malignancy. However, the clinical outcome has indicated the benignity of the tumor. We have experienced a case of cellular schwannoma arising from right facial nerve with right hemifacial weakness and erosion of mastoid process. Grossly, it was a 3.5 x 3 cm sized and relatively well encapsulated mass with yellowish, friable cut surface. Microscopically, cellular growth with moderate cellular pleomorphism and some mitotic activity (5/40 HPFS, up to 2/HPF) were noted. Immunostaining for S-100 protein showed diffuse strong positive reaction.
- Relationship between Proliferative Activity and Expression of HBcAg and p53 Protein in Hepatocellular Carcinoma and Surrounding Nontumorous Liver.
- So Ya Paik, Ho Guen Kim, Chan Il Park
- Korean J Pathol. 1997;31(8):773-781.
- 1,902 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - In an attempt to discover the factors contributing to the increased proliferative activity in hepatocytes and subsequent development of HCC, the proliferative activity of hepatocytes was compared with the size of regenerative nodules and HBcAg expression status in the surrounding nontumorous liver of 45 surgically resected hepatocellular carcinomas, including 34 HBV related ones. In the tumor, the difference in proliferative activity and the histological grade was analyzed in terms of p53 gene alteration. The proliferative activity was assessed by immunohistochemical methods using Ki-67 monoclonal antibody. HBcAg expression in the surrounding nontumorous liver correlated with both the inflammatory and proliferative activity of hepatocytes (p<0.05). p53 overexpression was associated with high proliferative activity and aggressive phenotype of tumor. No correlation was observed between the proliferative activity of hepatocytes and the size of regenerative nodules in cirrhosis (p>0.05). p53 overexpression was not evident in surrounding nontumorous liver including cirrhosis. In conclusion, the above results are in line with the view that hepatic carcinogenesis is a mutistep, progressive process. In the initial stage, chronic cellular injury incurred by immumologic reaction against HBcAg seems to play a pivotal role in increased cellular regeneration. However, once transformation of hepatocytes occur the major contributor to tumor growth seems to be alteration in p53 tumor suppresor gene.
- A Case of Combined Hepatocellular and Cholangiocarcinoma with Neuroendocrine Differentiation and Sarcomatoid Transformation: A Case Report.
- Mi Jung Kim, Hyun Lyoung Koo, Seung Kyu Lee, Jae Y Ro, Eunsil Yu
- Korean J Pathol. 2005;39(2):125-129.
- 2,045 View
- 15 Download
-
 Abstract
Abstract
 PDF
PDF - We report here on a case of combined hepatocellular and cholangiocarcinoma (CHC) with neuroendocrine differentiation and sarcomatoid transformation. A 59-year-old male who had had HBV-associated chronic liver disease presented with hepatic masses. The explanted liver showed three small masses, two in the right lobe and one in the left lobe. The largest one in the right lobe was a 2.0 cm sized binodular mass,consisting of a yellowish tan nodule and an abutting reddish brown nodule. Microscopically, the reddish brown nodule was a cholangiocarcinoma (CC) showing neuroendocrine differentiation and sarcomatoid tranformation. The yellowish tan nodule and the remaining two masses were hepatocellular carcinoma (HCC)s. On immunohistochemistry, both the adenocarcinoma and spindle sarcomatoid cells were positive for pancytokeratin, but only the adenocarcinoma cells were positive for chromogranin and carcinoembryonic antigen (CEA). Mitotic and Ki67 labeling indices as well as p53 immunopositivity were significantly increased only in the CC component. We report here on the first case of CHC in which the CC displayed neuroendocrine differentiation and sarcomatoid transformation with high mitotic and Ki67-labeling indices, as well as having p53 overexpression.

 E-submission
E-submission
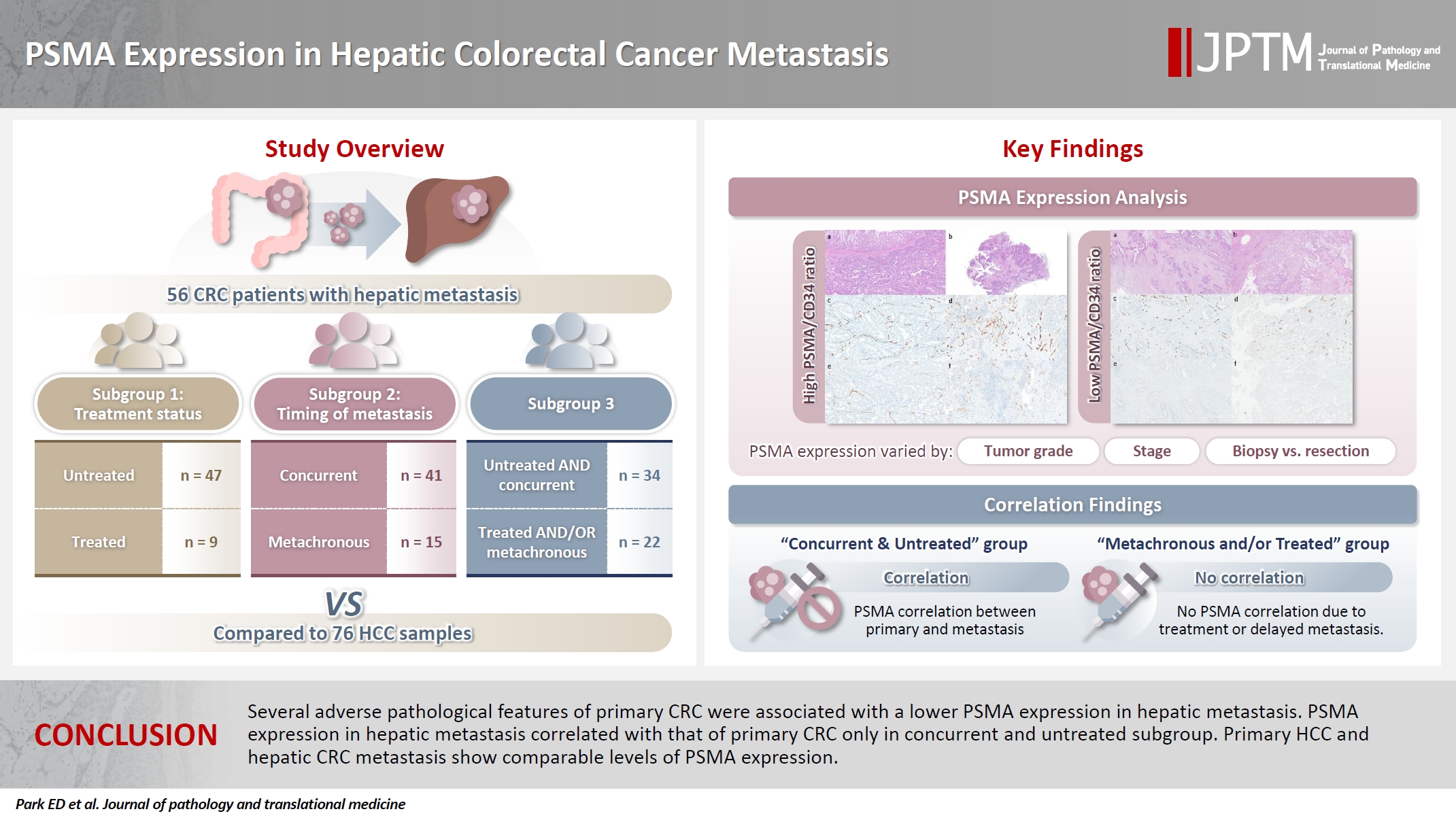








 First
First Prev
Prev



