Articles
- Page Path
- HOME > J Pathol Transl Med > Volume 48(3); 2014 > Article
-
Brief Case Report
Dedifferentiated Solitary Fibrous Tumor of Thoracic Cavity - Jung Wook Yang1, Dae Hyun Song1, In Seok Jang2,3, Gyung Hyuck Ko1,3
-
Korean Journal of Pathology 2014;48(3):250-253.
DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.3.250
Published online: June 26, 2014
1Department of Pathology, Gyeongsang National University School of Medicine, Jinju, Korea.
2Department of Thoracic and Cardiovascular Surgery, Gyeongsang National University School of Medicine, Jinju, Korea.
3Institute of Health Sciences, Gyeongsang National University, Jinju, Korea.
- Corresponding Author: Gyung Hyuck Ko, M.D. Department of Pathology, Gyeongsang National University School of Medicine, 15 Jinju-daero 816beon-gil, Jinju 660-751, Korea. Tel: +82-55-772-8061, Fax: +82-55-759-7952, gyunghko@gnu.ac.kr
© 2014 The Korean Society of Pathologists/The Korean Society for Cytopathology
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Figure & Data
References
Citations

- Dedifferentiated Solitary Fibrous Tumor
Adrian Georg Simon, Adrian Mariño-Enríquez, Jason L. Hornick, Christopher D. M. Fletcher, William J. Anderson
American Journal of Surgical Pathology.2025; 49(10): 1015. CrossRef - A case of slow-growing dedifferentiated solitary fibrous tumor of the pleura over a 7-year period
Madoka Goto, Rio Takada, Yasuhisa Ichikawa, Hideki Tsubouchi, Yuta Kawasumi, Shoichi Mori
The Journal of the Japanese Association for Chest Surgery.2022; 36(7): 821. CrossRef - A Comprehensive Review on Solitary Fibrous Tumor: New Insights for New Horizons
Javier Martin-Broto, Jose L. Mondaza-Hernandez, David S. Moura, Nadia Hindi
Cancers.2021; 13(12): 2913. CrossRef - An intrathoracic giant tumour and vanishing lung cyst after tumour resection
Masashi Nishimura, Shinichiro Ota, Sumitaka Yamanaka, Kanako Shinada, Masaharu Shinkai
Respirology Case Reports.2021;[Epub] CrossRef - Molecular changes in solitary fibrous tumor progression
Hyung Kyu Park, Dan Bi Yu, Minjung Sung, Ensel Oh, Mingi Kim, Ji-Young Song, Mi-Sook Lee, Kyungsoo Jung, Ka-Won Noh, Sungbin An, Kyoung Song, Do-Hyun Nam, Yu Jin Kim, Yoon-La Choi
Journal of Molecular Medicine.2019; 97(10): 1413. CrossRef - A Case Report of Solitary Fibrous Tumor in the Axilla of a 4-year-old Girl with Additional Marker Chromosome
Ji Hye Park, Eun Jeong Kim, O Kyu Noh, Hyun Ju Jung, Jun Eun Park
Clinical Pediatric Hematology-Oncology.2015; 22(2): 171. CrossRef


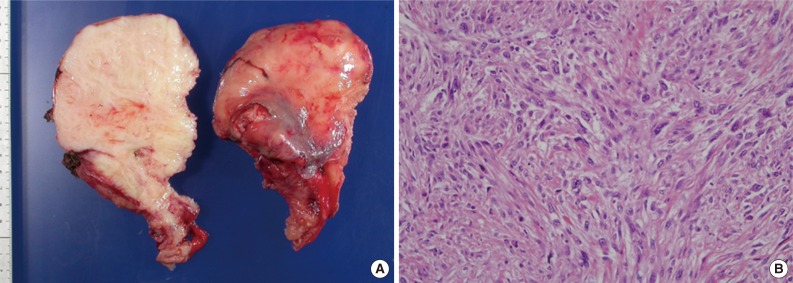
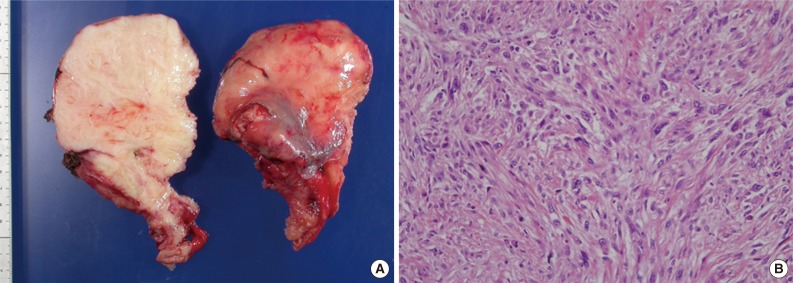
Fig. 1
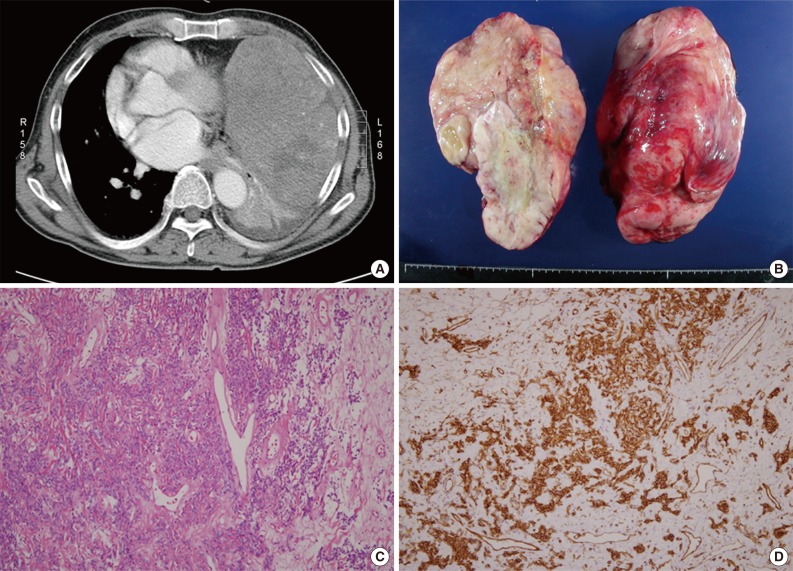
Fig. 2
| All SFT |
Benign SFT |
Malignant SFT |
Dedifferentiated SFT |
|
|---|---|---|---|---|
| Age (median, yr) | 53 | 51 | 61 | 51 |
| Sex (male:female) | 1:1 | - | - | 2:3 |
| Site | Abdomen, pelvis; 33/101 (32%) | - | - | Retroperitoneum, pelvic cavity; 7/10 (70%) |
| Size (cm) | 10.3 | 8.7 | 16.2 | 13.2 |
| 5YSR (%) | 89 | - | 60-93 |
50-60 |
5YSR, 5-year survival rate. Data extracted from Demicco Data extracted from Collini 93% for moderate-risk group, 60% for high-risk group.

 E-submission
E-submission
 PubReader
PubReader Cite this Article
Cite this Article