Search
- Page Path
- HOME > Search
- Proto-oncogene Pokemon in thyroid cancer: a potential promoter of tumorigenesis in papillary thyroid carcinoma
- Kyungseek Chang, Sung-Im Do, Kyungeun Kim, Seoung Wan Chae, In-gu Do, Hyun Joo Lee, Dong Hoon Kim, Jin Hee Sohn
- J Pathol Transl Med. 2021;55(5):317-323. Published online August 9, 2021
- DOI: https://doi.org/10.4132/jptm.2021.06.28
- 4,447 View
- 125 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Pokemon is an oncogenic transcription regulator that plays a critical role in cellular differentiation. Although it has been found to be overexpressed in several types of cancer involving different organs, its role in thyroid gland has yet to be reported. The objective of this study was to evaluate the expression of Pokemon in papillary thyroid carcinoma (PTC) based on clinicopathological parameters.
Methods
Tissue microarray samples derived from patients with PTC or benign thyroid disease were used to evaluate Pokemon expression based on immunohistochemical analysis. Correlations of its expression with various clinicopathological parameters were then analyzed.
Results
Pokemon expression was observed in 22.0% of thyroid follicular cells from the normal group, 44.0% from the group with benign thyroid diseases, and 92.1% from the group with PTC (p < .001). The intensity of Pokemon expression was markedly higher in the PTC group. Pokemon expression level and PTC tumor size showed an inverse correlation. T1a tumors showed strong expression levels of Pokemon. However, larger tumors showed weak expression (p = .006).
Conclusions
Pokemon expression is associated with tumorigenesis of PTC, with expression showing an inverse correlation with PTC tumor size. This might be related to the negative regulation of aerobic glycolysis by Pokemon. -
Citations
Citations to this article as recorded by- Systems biology approach delineates critical pathways associated with papillary thyroid cancer: a multi-omics data analysis
Febby Payva, Santhy K. S., Remya James, Amrisa Pavithra E, Venketesh Sivaramakrishnan
Thyroid Research.2025;[Epub] CrossRef - ZBTB7A as a therapeutic target for cancer
Ying Zhou, Xisha Chen, Xuyu Zu
Biochemical and Biophysical Research Communications.2024; 736: 150888. CrossRef - Knockdown of FBI-1 Inhibits the Warburg Effect and Enhances the Sensitivity of Hepatocellular Carcinoma Cells to Molecular Targeted Agents via miR-3692/HIF-1α
Juan Liu, Chao Yang, Xiao-Mei Huang, Pan-Pan Lv, Ya-Kun Yang, Jin-Na Zhao, Si-Yuan Zhao, Wan-Jun Sun
Frontiers in Oncology.2021;[Epub] CrossRef
- Systems biology approach delineates critical pathways associated with papillary thyroid cancer: a multi-omics data analysis
- A scoring system for the diagnosis of non-alcoholic steatohepatitis from liver biopsy
- Kyoungbun Lee, Eun Sun Jung, Eunsil Yu, Yun Kyung Kang, Mee-Yon Cho, Joon Mee Kim, Woo Sung Moon, Jin Sook Jeong, Cheol Keun Park, Jae-Bok Park, Dae Young Kang, Jin Hee Sohn, So-Young Jin
- J Pathol Transl Med. 2020;54(3):228-236. Published online April 15, 2020
- DOI: https://doi.org/10.4132/jptm.2020.03.07
- 7,661 View
- 260 Download
- 9 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Liver biopsy is the essential method to diagnose non-alcoholic steatohepatitis (NASH), but histological features of NASH are too subjective to achieve reproducible diagnoses in early stages of disease. We aimed to identify the key histological features of NASH and devise a scoring model for diagnosis.
Methods
Thirteen pathologists blindly assessed 12 histological factors and final histological diagnoses (‘not-NASH,’ ‘borderline,’ and ‘NASH’) of 31 liver biopsies that were diagnosed as non-alcoholic fatty liver disease (NAFLD) or NASH before and after consensus. The main histological parameters to diagnose NASH were selected based on histological diagnoses and the diagnostic accuracy and agreement of 12 scoring models were compared for final diagnosis and the NAFLD Activity Score (NAS) system.
Results
Inter-observer agreement of final diagnosis was fair (κ = 0.25) before consensus and slightly improved after consensus (κ = 0.33). Steatosis at more than 5% was the essential parameter for diagnosis. Major diagnostic factors for diagnosis were fibrosis except 1C grade and presence of ballooned cells. Minor diagnostic factors were lobular inflammation ( ≥ 2 foci/ × 200 field), microgranuloma, and glycogenated nuclei. All 12 models showed higher inter-observer agreement rates than NAS and post-consensus diagnosis (κ = 0.52–0.69 vs. 0.33). Considering the reproducibility of factors and practicability of the model, summation of the scores of major (× 2) and minor factors may be used for the practical diagnosis of NASH.
Conclusions
A scoring system for the diagnosis of NAFLD would be helpful as guidelines for pathologists and clinicians by improving the reproducibility of histological diagnosis of NAFLD. -
Citations
Citations to this article as recorded by- Preclinical liver toxicity models: Advantages, limitations and recommendations
Devaraj Ezhilarasan, Sivanesan Karthikeyan, Mustapha Najimi, Paramasivan Vijayalakshmi, Ganapathy Bhavani, Muthukrishnan Jansi Rani
Toxicology.2025; 511: 154020. CrossRef - Hepatic miR-93 promotes the pathogenesis of metabolic dysfunction-associated steatotic liver disease by suppressing SIRT1
Yo Han Lee, Jinyoung Lee, Joonho Jeong, Kieun Park, Bukyung Baik, Yuseong Kwon, Kimyeong Kim, Keon Woo Khim, Haneul Ji, Ji Young Lee, Kwangho Kim, Ji Won Kim, Tam Dao, Misung Kim, Tae Young Lee, Yong Ryoul Yang, Haejin Yoon, Dongryeol Ryu, Seonghwan Hwang
Metabolism.2025; 169: 156266. CrossRef - Presurgery health influences outcomes following vertical sleeve gastrectomy in adolescents
Debi Swertfeger, Ahlee Kim, Hannah Sexmith, Maria E. Moreno‐Fernandez, W. Sean Davidson, Michael Helmrath, Todd Jenkins, Tsuyoshi Okura, Esmond Geh, Stavra A. Xanthakos, Sara Szabo, Takahisa Nakamura, Senad Divanovic, Amy Sanghavi Shah
Obesity.2024; 32(6): 1187. CrossRef - Immunobiotic Bacteria Attenuate Hepatic Fibrosis through the Modulation of Gut Microbiota and the Activation of Aryl‐Hydrocarbon Receptors Pathway in Non‐Alcoholic Steatohepatitis Mice
Paulraj Kanmani, Julio Villena, Soo‐kyoung Lim, Eun‐Ji Song, Young‐Do Nam, Hojun Kim
Molecular Nutrition & Food Research.2024;[Epub] CrossRef - Lipid nanoparticle-mediated hepatocyte delivery of siRNA and silibinin in metabolic dysfunction-associated steatotic liver disease
Yifu Lyu, Xiuyi Yang, Lei Yang, Jinyu Dai, Huanyu Qin, Yunuo Zhou, Yunan Huang, Yanmei Wang, Di Wu, Qindai Shuai, Qilong Li, Xiaofei Xin, Lifang Yin
Journal of Controlled Release.2024; 373: 385. CrossRef - Enhanced hepatoprotective effects of empagliflozin and vitamin D dual therapy against metabolic dysfunction‐associated steatohepatitis in mice by boosted modulation of metabolic, oxidative stress, and inflammatory pathways
Wesam F. Farrash, Shakir Idris, Mohamed E. Elzubier, Elshiekh B. A. Khidir, Akhmed Aslam, Abdulrahman Mujalli, Riyad A. Almaimani, Ahmad A. Obaid, Mahmoud Z. El‐Readi, Mohammad A. Alobaidy, Afnan Salaka, Afnan M. Shakoori, Alaa M. Saleh, Faisal Minshawi,
International Journal of Experimental Pathology.2024; 105(6): 219. CrossRef - Bilirubin, a hepatoprotective agent that activates SIRT1, PGC-1α, and PPAR-α, while inhibiting NF-κB in rats with metabolic-associated fatty liver disease
Motahareh Taghizadeh, Mohammad Hasan Maleki, Omid Vakili, Ramin Tavakoli, Parvin Zarei, Amirreza Dehghanian, Hossein Bordbar, Sayed Mohammad Shafiee
Scientific Reports.2024;[Epub] CrossRef - Changes in indications for outpatient percutaneous liver biopsy over 5 years: from hepatitis C to fatty liver disease
Marlone Cunha-Silva, Luíza D. Torres, Mariana F. Fernandes, Tirzah de M. Lopes Secundo, Marina C.G. Moreira, Ademar Yamanaka, Leonardo T. Monici, Larissa B. Eloy da Costa, Daniel F. Mazo, Tiago Sevá-Pereira
Gastroenterología y Hepatología.2022; 45(8): 579. CrossRef - Changes in indications for outpatient percutaneous liver biopsy over 5 years: from hepatitis C to fatty liver disease
Marlone Cunha-Silva, Luíza D. Torres, Mariana F. Fernandes, Tirzah de M. Lopes Secundo, Marina C.G. Moreira, Ademar Yamanaka, Leonardo T. Monici, Larissa B. Eloy da Costa, Daniel F. Mazo, Tiago Sevá-Pereira
Gastroenterología y Hepatología (English Edition).2022; 45(8): 579. CrossRef
- Preclinical liver toxicity models: Advantages, limitations and recommendations
- Standardized Pathology Report for Colorectal Cancer, 2nd Edition
- Baek-hui Kim, Joon Mee Kim, Gyeong Hoon Kang, Hee Jin Chang, Dong Wook Kang, Jung Ho Kim, Jeong Mo Bae, An Na Seo, Ho Sung Park, Yun Kyung Kang, Kyung-Hwa Lee, Mee Yon Cho, In-Gu Do, Hye Seung Lee, Hee Kyung Chang, Do Youn Park, Hyo Jeong Kang, Jin Hee Sohn, Mee Soo Chang, Eun Sun Jung, So-Young Jin, Eunsil Yu, Hye Seung Han, Youn Wha Kim
- J Pathol Transl Med. 2020;54(1):1-19. Published online November 13, 2019
- DOI: https://doi.org/10.4132/jptm.2019.09.28
- 22,594 View
- 1,251 Download
- 43 Web of Science
- 35 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - The first edition of the ‘Standardized Pathology Report for Colorectal Cancer,’ which was developed by the Gastrointestinal Pathology Study Group (GIP) of the Korean Society of Pathologists, was published 13 years ago. Meanwhile, there have been many changes in the pathologic diagnosis of colorectal cancer (CRC), pathologic findings included in the pathology report, and immunohistochemical and molecular pathology required for the diagnosis and treatment of colorectal cancer. In order to reflect these changes, we (GIP) decided to make the second edition of the report. The purpose of this standardized pathology report is to provide a practical protocol for Korean pathologists, which could help diagnose and treat CRC patients. This report consists of “standard data elements” and “conditional data elements.” Basic pathologic findings and parts necessary for prognostication of CRC patients are classified as “standard data elements,” while other prognostic factors and factors related to adjuvant therapy are classified as “conditional data elements” so that each institution could select the contents according to the characteristics of the institution. The Korean version is also provided separately so that Korean pathologists can easily understand and use this report. We hope that this report will be helpful in the daily practice of CRC diagnosis.
-
Citations
Citations to this article as recorded by- Diagnostic accuracy and pitfalls of MRI for restaging locally advanced rectal cancer in patients following anti-PD1 therapy plus neoadjuvant chemoradiotherapy: a multicenter study
Lixue Xu, Liting Sun, Yuhuan Fu, Guangyong Chen, Hongwei Yao, Zhenchang Wang, Zhenghan Yang, Jie Zhang
Abdominal Radiology.2025;[Epub] CrossRef - Additional staining for lymphovascular invasion is associated with increased estimation of lymph node metastasis in patients with T1 colorectal cancer: Systematic review and meta‐analysis
Jun Watanabe, Katsuro Ichimasa, Yuki Kataoka, Atsushi Miki, Hidehiro Someko, Munenori Honda, Makiko Tahara, Takeshi Yamashina, Khay Guan Yeoh, Shigeo Kawai, Kazuhiko Kotani, Naohiro Sata
Digestive Endoscopy.2024; 36(5): 533. CrossRef - The use of core descriptors from the ENiGMA code study in recent literature: a systematic review
Saher‐Zahra Khan, Andrea Arline, Kate M. Williams, Matthew J. Lee, Emily Steinhagen, Sharon L. Stein
Colorectal Disease.2024; 26(3): 428. CrossRef - Efficacy and safety of PD-1 blockade plus long-course chemoradiotherapy in locally advanced rectal cancer (NECTAR): a multi-center phase 2 study
Zhengyang Yang, Jiale Gao, Jianyong Zheng, Jiagang Han, Ang Li, Gang Liu, Yi Sun, Jie Zhang, Guangyong Chen, Rui Xu, Xiao Zhang, Yishan Liu, Zhigang Bai, Wei Deng, Wei He, Hongwei Yao, Zhongtao Zhang
Signal Transduction and Targeted Therapy.2024;[Epub] CrossRef - Diagnostic Accuracy of Highest-Grade or Predominant Histological Differentiation of T1 Colorectal Cancer in Predicting Lymph Node Metastasis: A Systematic Review and Meta-Analysis
Jun Watanabe, Katsuro Ichimasa, Yuki Kataoka, Shoko Miyahara, Atsushi Miki, Khay Guan Yeoh, Shigeo Kawai, Fernando Martínez de Juan, Isidro Machado, Kazuhiko Kotani, Naohiro Sata
Clinical and Translational Gastroenterology.2024; 15(3): e00673. CrossRef - Comparative evaluation of CT and MRI in the preoperative staging of colon cancer
Effrosyni Bompou, Aikaterini Vassiou, Ioannis Baloyiannis, Konstantinos Perivoliotis, Ioannis Fezoulidis, George Tzovaras
Scientific Reports.2024;[Epub] CrossRef - Pathologic Implications of Magnetic Resonance Imaging-detected Extramural Venous Invasion of Rectal Cancer
Hyun Gu Lee, Chan Wook Kim, Jong Keon Jang, Seong Ho Park, Young Il Kim, Jong Lyul Lee, Yong Sik Yoon, In Ja Park, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Clinical Colorectal Cancer.2023; 22(1): 129. CrossRef - A standardized pathology report for gastric cancer: 2nd edition
Young Soo Park, Myeong-Cherl Kook, Baek-hui Kim, Hye Seung Lee, Dong-Wook Kang, Mi-Jin Gu, Ok Ran Shin, Younghee Choi, Wonae Lee, Hyunki Kim, In Hye Song, Kyoung-Mee Kim, Hee Sung Kim, Guhyun Kang, Do Youn Park, So-Young Jin, Joon Mee Kim, Yoon Jung Choi,
Journal of Pathology and Translational Medicine.2023; 57(1): 1. CrossRef - IGFL2-AS1, a Long Non-Coding RNA, Is Associated with Radioresistance in Colorectal Cancer
Jeeyong Lee, Da Yeon Kim, Younjoo Kim, Ui Sup Shin, Kwang Seok Kim, Eun Ju Kim
International Journal of Molecular Sciences.2023; 24(2): 978. CrossRef - A Standardized Pathology Report for Gastric Cancer: 2nd Edition
Young Soo Park, Myeong-Cherl Kook, Baek-hui Kim, Hye Seung Lee, Dong-Wook Kang, Mi-Jin Gu, Ok Ran Shin, Younghee Choi, Wonae Lee, Hyunki Kim, In Hye Song, Kyoung-Mee Kim, Hee Sung Kim, Guhyun Kang, Do Youn Park, So-Young Jin, Joon Mee Kim, Yoon Jung Choi,
Journal of Gastric Cancer.2023; 23(1): 107. CrossRef - Incremental Detection Rate of Dysplasia and Sessile Serrated Polyps/Adenomas Using Narrow-Band Imaging and Dye Spray Chromoendoscopy in Addition to High-Definition Endoscopy in Patients with Long-Standing Extensive Ulcerative Colitis: Segmental Tandem End
Ji Eun Kim, Chang Wan Choi, Sung Noh Hong, Joo Hye Song, Eun Ran Kim, Dong Kyung Chang, Young-Ho Kim
Diagnostics.2023; 13(3): 516. CrossRef - Prognostic Impact of Extramural Lymphatic, Vascular, and Perineural Invasion in Stage II Colon Cancer: A Comparison With Intramural Invasion
Sang Sik Cho, Ji Won Park, Gyeong Hoon Kang, Jung Ho Kim, Jeong Mo Bae, Sae-Won Han, Tae-You Kim, Min Jung Kim, Seung-Bum Ryoo, Seung-Yong Jeong, Kyu Joo Park
Diseases of the Colon & Rectum.2023; 66(3): 366. CrossRef - Towards targeted colorectal cancer biopsy based on tissue morphology assessment by compression optical coherence elastography
Anton A. Plekhanov, Marina A. Sirotkina, Ekaterina V. Gubarkova, Elena B. Kiseleva, Alexander A. Sovetsky, Maria M. Karabut, Vladimir E. Zagainov, Sergey S. Kuznetsov, Anna V. Maslennikova, Elena V. Zagaynova, Vladimir Y. Zaitsev, Natalia D. Gladkova
Frontiers in Oncology.2023;[Epub] CrossRef - Is High-Grade Tumor Budding an Independent Prognostic Factor in Stage II Colon Cancer?
Jung Kyong Shin, Yoon Ah Park, Jung Wook Huh, Seong Hyeon Yun, Hee Cheol Kim, Woo Yong Lee, Seok Hyung Kim, Sang Yun Ha, Yong Beom Cho
Diseases of the Colon & Rectum.2023; 66(8): e801. CrossRef - Detection of Human cytomegalovirus UL55 Gene and IE/E Protein Expression in Colorectal Cancer Patients in Egypt
May Raouf, Ahmed A. Sabry, Mahinour A. Ragab, Samar El Achy, Amira Amer
BMC Cancer.2023;[Epub] CrossRef - Polo-like kinase 4 as a potential predictive biomarker of chemoradioresistance in locally advanced rectal cancer
Hyunseung Oh, Soon Gu Kim, Sung Uk Bae, Sang Jun Byun, Shin Kim, Jae-Ho Lee, Ilseon Hwang, Sun Young Kwon, Hye Won Lee
Journal of Pathology and Translational Medicine.2022; 56(1): 40. CrossRef - A Prediction Model for Tumor Recurrence in Stage II–III Colorectal Cancer Patients: From a Machine Learning Model to Genomic Profiling
Po-Chuan Chen, Yu-Min Yeh, Bo-Wen Lin, Ren-Hao Chan, Pei-Fang Su, Yi-Chia Liu, Chung-Ta Lee, Shang-Hung Chen, Peng-Chan Lin
Biomedicines.2022; 10(2): 340. CrossRef - Rationale and design of a prospective, multicenter, phase II clinical trial of safety and efficacy evaluation of long course neoadjuvant chemoradiotherapy plus tislelizumab followed by total mesorectal excision for locally advanced rectal cancer (NCRT-PD1
Zhengyang Yang, Xiao Zhang, Jie Zhang, Jiale Gao, Zhigang Bai, Wei Deng, Guangyong Chen, Yongbo An, Yishan Liu, Qi Wei, Jiagang Han, Ang Li, Gang Liu, Yi Sun, Dalu Kong, Hongwei Yao, Zhongtao Zhang
BMC Cancer.2022;[Epub] CrossRef - Potential of DEK proto‑oncogene as a prognostic biomarker for colorectal cancer: An evidence‑based review
Muhammad Habiburrahman, Muhammad Wardoyo, Stefanus Sutopo, Nur Rahadiani
Molecular and Clinical Oncology.2022;[Epub] CrossRef - Reproducibility and Feasibility of Classification and National Guidelines for Histological Diagnosis of Canine Mammary Gland Tumours: A Multi-Institutional Ring Study
Serenella Papparella, Maria Crescio, Valeria Baldassarre, Barbara Brunetti, Giovanni Burrai, Cristiano Cocumelli, Valeria Grieco, Selina Iussich, Lorella Maniscalco, Francesca Mariotti, Francesca Millanta, Orlando Paciello, Roberta Rasotto, Mariarita Roma
Veterinary Sciences.2022; 9(7): 357. CrossRef - Composite scoring system and optimal tumor budding cut-off number for estimating lymph node metastasis in submucosal colorectal cancer
Jeong-ki Kim, Ye-Young Rhee, Jeong Mo Bae, Jung Ho Kim, Seong-Joon Koh, Hyun Jung Lee, Jong Pil Im, Min Jung Kim, Seung-Bum Ryoo, Seung-Yong Jeong, Kyu Joo Park, Ji Won Park, Gyeong Hoon Kang
BMC Cancer.2022;[Epub] CrossRef - Automated Hybrid Model for Detecting Perineural Invasion in the Histology of Colorectal Cancer
Jiyoon Jung, Eunsu Kim, Hyeseong Lee, Sung Hak Lee, Sangjeong Ahn
Applied Sciences.2022; 12(18): 9159. CrossRef - Clinical Implication of Perineural and Lymphovascular Invasion in Rectal Cancer Patients Who Underwent Surgery After Preoperative Chemoradiotherapy
Young Il Kim, Chan Wook Kim, Jong Hoon Kim, Jihun Kim, Jun-Soo Ro, Jong Lyul Lee, Yong Sik Yoon, In Ja Park, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Diseases of the Colon & Rectum.2022; 65(11): 1325. CrossRef - Molecular Pathology of Gastric Cancer
Moonsik Kim, An Na Seo
Journal of Gastric Cancer.2022; 22(4): 264. CrossRef - Selective approach to arterial ligation in radical sigmoid colon cancer surgery with D3 lymph node dissection: A multicenter comparative study
Sergey Efetov, Albina Zubayraeva, Cüneyt Kayaalp, Alisa Minenkova, Yusuf Bağ, Aftandil Alekberzade, Petr Tsarkov
Turkish Journal of Surgery.2022; 38(4): 382. CrossRef - Evaluation of lncRNA FOXD2-AS1 Expression as a Diagnostic Biomarker in Colorectal Cancer
Hooman Shalmashi, Sahar Safaei, Dariush Shanehbandi, Milad Asadi, Soghra Bornehdeli, Abdolreza Mehdi Navaz
Reports of Biochemistry and Molecular Biology.2022; 11(3): 471. CrossRef - Improvement in the Assessment of Response to Preoperative Chemoradiotherapy for Rectal Cancer Using Magnetic Resonance Imaging and a Multigene Biomarker
Eunhae Cho, Sung Woo Jung, In Ja Park, Jong Keon Jang, Seong Ho Park, Seung-Mo Hong, Jong Lyul Lee, Chan Wook Kim, Yong Sik Yoon, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Cancers.2021; 13(14): 3480. CrossRef - Addition of V-Stage to Conventional TNM Staging to Create the TNVM Staging System for Accurate Prediction of Prognosis in Colon Cancer: A Multi-Institutional Retrospective Cohort Study
Jung Hoon Bae, Ji Hoon Kim, Jaeim Lee, Bong-Hyeon Kye, Sang Chul Lee, In Kyu Lee, Won Kyung Kang, Hyeon-Min Cho, Yoon Suk Lee
Biomedicines.2021; 9(8): 888. CrossRef - Gene Expression Profiles Associated with Radio-Responsiveness in Locally Advanced Rectal Cancer
Jeeyong Lee, Junhye Kwon, DaYeon Kim, Misun Park, KwangSeok Kim, InHwa Bae, Hyunkyung Kim, JoonSeog Kong, Younjoo Kim, UiSup Shin, EunJu Kim
Biology.2021; 10(6): 500. CrossRef - A Patient-Derived Organoid-Based Radiosensitivity Model for the Prediction of Radiation Responses in Patients with Rectal Cancer
Misun Park, Junhye Kwon, Joonseog Kong, Sun Mi Moon, Sangsik Cho, Ki Young Yang, Won Il Jang, Mi Sook Kim, Younjoo Kim, Ui Sup Shin
Cancers.2021; 13(15): 3760. CrossRef - Comparison between Local Excision and Radical Resection for the Treatment of Rectal Cancer in ypT0-1 Patients: An Analysis of the Clinicopathological Factors and Survival Rates
Soo Young Oh, In Ja Park, Young IL Kim, Jong-Lyul Lee, Chan Wook Kim, Yong Sik Yoon, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Cancers.2021; 13(19): 4823. CrossRef - Comparison of Vascular Invasion With Lymph Node Metastasis as a Prognostic Factor in Stage I-III Colon Cancer: An Observational Cohort Study
Jung Hoon Bae, Ji Hoon Kim, Bong-Hyeon Kye, Abdullah Al-Sawat, Chul Seung Lee, Seung-Rim Han, In Kyu Lee, Sung Hak Lee, Yoon Suk Lee
Frontiers in Surgery.2021;[Epub] CrossRef - Clinicopathological significance of Ki67 expression in colorectal cancer
Jing Li, Zhi-ye Liu, Hai-bo Yu, Qing Xue, Wen-jie He, Hai-tao Yu
Medicine.2020; 99(20): e20136. CrossRef - Lateral lymph node and its association with distant recurrence in rectal cancer: A clue of systemic disease
Young Il Kim, Jong Keon Jang, In Ja Park, Seong Ho Park, Jong Beom Kim, Jin-Hong Park, Tae Won Kim, Jun-Soo Ro, Seok-Byung Lim, Chang Sik Yu, Jin Cheon Kim
Surgical Oncology.2020; 35: 174. CrossRef - Transformation of Pathology Reports Into the Common Data Model With Oncology Module: Use Case for Colon Cancer
Borim Ryu, Eunsil Yoon, Seok Kim, Sejoon Lee, Hyunyoung Baek, Soyoung Yi, Hee Young Na, Ji-Won Kim, Rong-Min Baek, Hee Hwang, Sooyoung Yoo
Journal of Medical Internet Research.2020; 22(12): e18526. CrossRef
- Diagnostic accuracy and pitfalls of MRI for restaging locally advanced rectal cancer in patients following anti-PD1 therapy plus neoadjuvant chemoradiotherapy: a multicenter study
- Prognostic Role of Metastatic Lymph Node Ratio in Papillary Thyroid Carcinoma
- Jung-Soo Pyo, Jin Hee Sohn, Kyungseek Chang
- J Pathol Transl Med. 2018;52(5):331-338. Published online August 30, 2018
- DOI: https://doi.org/10.4132/jptm.2018.08.07
- 7,686 View
- 130 Download
- 16 Web of Science
- 14 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The aim of this study is to elucidate the clinicopathological significances, including the prognostic role, of metastatic lymph node ratio (mLNR) and tumor deposit diameter in papillary thyroid carcinoma (PTC) through a retrospective review and meta-analysis.
Methods
We categorized the cases into high (≥ 0.44) and low mLNR (< 0.44) and investigated the correlations with clinicopathological parameters in 64 PTCs with neck level VI lymph node (LN) metastasis. In addition, meta-analysis of seven eligible studies was used to investigate the correlation between mLNR and survival.
Results
Among 64 PTCs with neck level VI LN metastasis, high mLNR was found in 34 PTCs (53.1%). High mLNR was significantly correlated with macrometastasis (tumor deposit diameter ≥ 0.2 cm), extracapsular spread, and number of metastatic LNs. Based on linear regression test, mLNR was significantly increased by the largest LN size but not the largest metastatic LN (mLN) size. High mLNR was not correlated with nuclear factor κB or cyclin D1 immunohistochemical expression, Ki-67 labeling index, or other pathological parameters of primary tumor. Based on meta-analysis, high mLNR significantly correlated with worse disease-free survival at the 5-year and 10-year follow-up (hazard ratio [HR], 4.866; 95% confidence interval [CI], 3.527 to 6.714 and HR, 5.769; 95% CI, 2.951 to 11.275, respectively).
Conclusions
Our data showed that high mLNR significantly correlated with worse survival, macrometastasis, and extracapsular spread of mLNs. Further cumulative studies for more detailed criteria of mLNR are needed before application in daily practice. -
Citations
Citations to this article as recorded by- The application of a clinical-multimodal ultrasound radiomics model for predicting cervical lymph node metastasis of thyroid papillary carcinoma
Chang Liu, Shangjie Yang, Tian Xue, Qian Zhang, Yanjing Zhang, Yufang Zhao, Guolin Yin, Xiaohui Yan, Ping Liang, Liping Liu
Frontiers in Oncology.2025;[Epub] CrossRef - The Predictive Value of a Nomogram Based on Ultrasound Radiomics, Clinical Factors, and Enhanced Ultrasound Features for Central Lymph Node Metastasis in Papillary Thyroid Microcarcinoma
Lei Gao, Xiuli Wen, Guanghui Yue, Hui Wang, Ziqing Lu, Beibei Wu, Zhihong Liu, Yuming Wu, Dongmei Lin, Shijian Yi, Wei Jiang, Yi Hao
Ultrasonic Imaging.2025; 47(2): 93. CrossRef - Lymph Node Metastasis Ratio: Prognostic Significance in Papillary Thyroid Cancer
Ana Rita Ferreira, Diogo Ramalho, Daniela Martins, Andreia Amado, Susana Graça, Carlos Soares, Bela Pereira, Maria João Oliveira, Manuel Oliveira, Antónia Póvoa
Indian Journal of Surgery.2025;[Epub] CrossRef - Application and subgroup analysis of competing risks model based on different lymph node staging systems in differentiated thyroid cancer
Zhe Xu Cao, Jiang Sheng Huang, Ming Ming Wang
Updates in Surgery.2024; 76(5): 1927. CrossRef - Цитологічне прогнозування агресії раку щитоподібної залози як новий перспективний напрямок у клінічній тиреоїдології
H.V. Zelinska
Endokrynologia.2024; 29(4): 363. CrossRef - Thyroglobulin expression, Ki-67 index, and lymph node ratio in the prognostic assessment of papillary thyroid cancer
Helene Lindfors, Marie Karlsen, Ellinor Karlton, Jan Zedenius, Catharina Larsson, Catharina Ihre Lundgren, C. Christofer Juhlin, Ivan Shabo
Scientific Reports.2023;[Epub] CrossRef - Incidental Node Metastasis as an Independent Factor of Worse Disease-Free Survival in Patients with Papillary Thyroid Carcinoma
Renan Aguera Pinheiro, Ana Kober Leite, Beatriz Godoi Cavalheiro, Evandro Sobroza de Mello, Luiz Paulo Kowalski, Leandro Luongo Matos
Cancers.2023; 15(3): 943. CrossRef - A High-Quality Nomogram for Predicting Lung Metastasis in Newly Diagnosed Stage IV Thyroid Cancer: A Population-Based Study
WenYi Wang, JiaJing Liu, XiaoFan Xu, LiQun Huo, XuLin Wang, Jun Gu
Technology in Cancer Research & Treatment.2023;[Epub] CrossRef - Lymph Node Ratio Predicts Recurrence in Patients with Papillary Thyroid Carcinoma with Low Lymph Node Yield
Il Ku Kang, Joonseon Park, Ja Seong Bae, Jeong Soo Kim, Kwangsoon Kim
Cancers.2023; 15(11): 2947. CrossRef - Superiority of metastatic lymph node ratio over number of node metastases and TNM/AJCC N classification in predicting cancer‐specific survival in medullary thyroid cancer
Andreas Machens, Kerstin Lorenz, Frank Weber, Henning Dralle
Head & Neck.2022; 44(12): 2717. CrossRef - Value of Combining Clinical Factors, Conventional Ultrasound, and Contrast-Enhanced Ultrasound Features in Preoperative Prediction of Central Lymph Node Metastases of Different Sized Papillary Thyroid Carcinomas
Yanfang Wang, Fang Nie, Guojuan Wang, Ting Liu, Tiantian Dong, Yamin Sun
Cancer Management and Research.2021; Volume 13: 3403. CrossRef - Atypical Histiocytoid Cells and Multinucleated Giant Cells in Fine-Needle Aspiration Cytology of the Thyroid Predict Lymph Node Metastasis of Papillary Thyroid Carcinoma
Ji Eun Choi, Ja Seong Bae, Dong-Jun Lim, So Lyung Jung, Chan Kwon Jung
Cancers.2019; 11(6): 816. CrossRef - Patients Aged ≥55 Years With Stage T1-2N1M1 Differentiated Thyroid Cancer Should Be Downstaged in the Eighth Edition AJCC/TNM Cancer Staging System
Zeming Liu, Sichao Chen, Yihui Huang, Di Hu, Min Wang, Wei Wei, Chao Zhang, Wen Zeng, Liang Guo
Frontiers in Oncology.2019;[Epub] CrossRef - Prognostic Implication of Metastatic Lymph Node Ratio in Colorectal Cancers: Comparison Depending on Tumor Location
Jung-Soo Pyo, Young-Min Shin, Dong-Wook Kang
Journal of Clinical Medicine.2019; 8(11): 1812. CrossRef
- The application of a clinical-multimodal ultrasound radiomics model for predicting cervical lymph node metastasis of thyroid papillary carcinoma
- Detection of Tumor Multifocality Is Important for Prediction of Tumor Recurrence in Papillary Thyroid Microcarcinoma: A Retrospective Study and Meta-Analysis
- Jung-Soo Pyo, Jin Hee Sohn, Guhyun Kang
- J Pathol Transl Med. 2016;50(4):278-286. Published online June 6, 2016
- DOI: https://doi.org/10.4132/jptm.2016.03.29
- 10,842 View
- 111 Download
- 21 Web of Science
- 24 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The clinicopathological characteristics and conclusive treatment modality for multifocal papillary thyroid microcarcinoma (mPTMC) have not been fully established.
Methods
A retrospective study, systematic review, and meta-analysis were conducted to elucidate the clinicopathological significance of mPTMC. We investigated the multiplicity of 383 classical papillary thyroid microcarcinomas (PTMCs) and the clinicopathological significance of incidental mPTMCs. Correlation between tumor recurrence and multifocality in PTMCs was evaluated through a systematic review and meta-analysis.
Results
Tumor multifocality was identified in 103 of 383 PTMCs (26.9%). On linear regression analysis, primary tumor diameter was significantly correlated with tumor number (R2=0.014, p=.021) and supplemental tumor diameter (R2=0.117, p=.023). Of 103 mPTMCs, 61 (59.2%) were non-incidental, with tumor detected on preoperative ultrasonography, and 42 (40.8%) were diagnosed (incidental mPTMCs) on pathological examination. Lymph node metastasis and higher tumor stage were significantly correlated with tumor multifocality. However, there was no difference in nodal metastasis or tumor stage between incidental and non-incidental mPTMCs. On meta-analysis, tumor multifocality was significantly correlated with tumor recurrence in PTMCs (odds ratio, 2.002; 95% confidence interval, 1.475 to 2.719, p<.001).
Conclusions
Our results show that tumor multifocality in PTMC, regardless of manner of detection, is significantly correlated with aggressive tumor behavior. -
Citations
Citations to this article as recorded by- A machine learning model utilizing Delphian lymph node characteristics to predict contralateral central lymph node metastasis in papillary thyroid carcinoma: a prospective multicenter study
Jia-ling He, Yu-zhao Yan, Yan Zhang, Jin-sui Li, Fei Wang, Yi You, Wei Liu, Ying Hu, Ming-Hao Wang, Qing-wen Pan, Yan Liang, Ming-shijing Ren, Zi-wei Wu, Kai You, Yi Zhang, Jun Jiang, Peng Tang
International Journal of Surgery.2025; 111(1): 360. CrossRef - Retrospective comparison of individual risk factors hemithyroidectomy and thyroidectomy in patients with papillary carcinoma of the thyroid gland in combination with autoimmune thyroiditis
E. V. Ryabchenko
Head and Neck Tumors (HNT).2023; 12(4): 71. CrossRef - Individual risk factors for recurrence after hemithyroidectomy and thyroidectomy in patients with papillary thyroid microcarcinoma in the presence of autoimmune thyroiditis
E.V. Ryabchenko
P.A. Herzen Journal of Oncology.2023; 12(3): 20. CrossRef - The value of total tumor diameter in unilateral multifocal papillary thyroid carcinoma: a propensity score matching analysis
Zhu-juan Wu, Bao-ying Xia, Zi-wei Chen, Hao Gong, Munire Abuduwaili, Zhi-chao Xing, An-ping Su
Frontiers in Endocrinology.2023;[Epub] CrossRef - Negative Histopathological Prognostic Factors Affecting Morbidity in T1 Differentiated Thyroid Carcinoma
Mine Araz, Elgin Özkan, Pınar Gunduz, Cigdem Soydal, N. Özlem Küçük, K. Metin Kır
Cancer Biotherapy and Radiopharmaceuticals.2022; 37(1): 56. CrossRef - Total tumor diameter is a better indicator of multifocal papillary thyroid microcarcinoma: A propensity score matching analysis
Ke-cheng Jiang, Bei Lin, Yu Zhang, Ling-qian Zhao, Ding-cun Luo
Frontiers in Endocrinology.2022;[Epub] CrossRef - The relationship between lipotoxicity and risk of extrathyroidal extension in papillary thyroid microcarcinoma
Changlin Li, Haixia Guan, Qiao He, Yishen Zhao, Nan liang, Jiao Zhang, Gianlorenzo Dionigi, Hui Sun
Endocrine.2021; 74(3): 646. CrossRef - Multifocality and Progression of Papillary Thyroid Microcarcinoma During Active Surveillance
Ryuta Nagaoka, Aya Ebina, Kazuhisa Toda, Tomoo Jikuzono, Marie Saitou, Masaomi Sen, Hiroko Kazusaka, Mami Matsui, Keiko Yamada, Hiroki Mitani, Iwao Sugitani
World Journal of Surgery.2021; 45(9): 2769. CrossRef - Correlation of ThyroSeq Results with Surgical Histopathology in Cytologically Indeterminate Thyroid Nodules
Patrick D. Chin, Catherine Y. Zhu, Dipti P. Sajed, Gregory A. Fishbein, Michael W. Yeh, Angela M. Leung, Masha J. Livhits
Endocrine Pathology.2020; 31(4): 377. CrossRef - Application of Ultrasonography in the Diagnosis and Management of Papillary Thyroid Microcarcinoma
Huang, MD Kun, Liu, MD Ji-Bin
ADVANCED ULTRASOUND IN DIAGNOSIS AND THERAPY.2020; 4(4): 284. CrossRef - Analysis of Malignant Thyroid Neoplasms with a Striking Rise of Papillary Microcarcinoma in an Endemic Goiter Region
Alka Mary Mathai, K. Preetha, S. Valsala Devi, Sam Vicliph, Raja Pradeep, Aqib Shaick
Indian Journal of Otolaryngology and Head & Neck Surgery.2019; 71(S1): 121. CrossRef - The first postoperative-stimulated serum thyroglobulin is a prognostic factor for thyroid microcarcinomas
Isabela de Oliveira Amui, José Vicente Tagliarini, Emanuel C. Castilho, Mariângela de Alencar Marques, Yoshio Kiy, José Eduardo Corrente, Gláucia M.F.S. Mazeto
Brazilian Journal of Otorhinolaryngology.2019; 85(1): 37. CrossRef - Surgical management of follicular thyroid carcinoma in children and adolescents: A study of 30 cases
Claudio Spinelli, Leonardo Rallo, Riccardo Morganti, Valentina Mazzotti, Alessandro Inserra, Giovanni Cecchetto, Maura Massimino, Paola Collini, Silvia Strambi
Journal of Pediatric Surgery.2019; 54(3): 521. CrossRef - The role of prophylactic central compartment lymph node dissection in elderly patients with differentiated thyroid cancer: a multicentric study
Claudio Gambardella, Renato Patrone, Francesco Di Capua, Chiara Offi, Claudio Mauriello, Guglielmo Clarizia, Claudia Andretta, Andrea Polistena, Alessandro Sanguinetti, Pietrogiorgio Calò, Giovanni Docimo, Nicola Avenia, Giovanni Conzo
BMC Surgery.2019;[Epub] CrossRef - Cervical Lymph Node Metastases of Papillary Thyroid Carcinoma, in the Central and Lateral Compartments, in Children and Adolescents: Predictive Factors
C. Spinelli, F. Tognetti, S. Strambi, R. Morganti, M. Massimino, P. Collini
World Journal of Surgery.2018; 42(8): 2444. CrossRef - Active Surveillance for Papillary Thyroid Microcarcinoma: Challenges and Prospects
Shuai Xue, Peisong Wang, Zachary A. Hurst, Yi Seok Chang, Guang Chen
Frontiers in Endocrinology.2018;[Epub] CrossRef - A comparison of lobectomy and total thyroidectomy in patients with papillary thyroid microcarcinoma: a retrospective individual risk factor-matched cohort study
Hyemi Kwon, Min Ji Jeon, Won Gu Kim, Suyeon Park, Mijin Kim, Dong Eun Song, Tae-Yon Sung, Jong Ho Yoon, Suck Joon Hong, Tae Yong Kim, Young Kee Shong, Won Bae Kim
European Journal of Endocrinology.2017; 176(4): 371. CrossRef - Total thyroidectomy may be more reasonable as initial surgery in unilateral multifocal papillary thyroid microcarcinoma: a single-center experience
Shuai Xue, Peisong Wang, Jia Liu, Guang Chen
World Journal of Surgical Oncology.2017;[Epub] CrossRef - Lack of Efficacy of Radioiodine Remnant Ablation for Papillary Thyroid Microcarcinoma: Verification Using Inverse Probability of Treatment Weighting
Hyemi Kwon, Min Ji Jeon, Won Gu Kim, Suyeon Park, Mijin Kim, Tae Yong Kim, Minkyu Han, Dong Eun Song, Tae-Yon Sung, Jong Ho Yoon, Suck Joon Hong, Jin-Sook Ryu, Young Kee Shong, Won Bae Kim
Annals of Surgical Oncology.2017; 24(9): 2596. CrossRef - Radioactive Iodine Ablation Decrease Recurrences in Papillary Thyroid Microcarcinoma with Lateral Lymph Node Metastasis in Chinese Patients
Shuai Xue, Peisong Wang, Jia Liu, Guang Chen
World Journal of Surgery.2017; 41(12): 3139. CrossRef - The Prognostic Value of Tumor Multifocality in Clinical Outcomes of Papillary Thyroid Cancer
Fei Wang, Xiaolong Yu, Xiaopei Shen, Guangwu Zhu, Yueye Huang, Rengyun Liu, David Viola, Rossella Elisei, Efisio Puxeddu, Laura Fugazzola, Carla Colombo, Barbara Jarzab, Agnieszka Czarniecka, Alfred K Lam, Caterina Mian, Federica Vianello, Linwah Yip, Gar
The Journal of Clinical Endocrinology & Metabolism.2017; 102(9): 3241. CrossRef - Evaluation of surgical results of micropapillary thyroid cancers according to tumor size and focality
Bekir Uçan, Muhammed Erkam Sencar, Muhammed Kızılgül, Mustafa Özbek, İlknur Öztürk Ünsal, Erman Çakal
Ortadoğu Tıp Dergisi.2017; 9(3): 123. CrossRef - Contrastive study of two screening criteria for active surveillance in patients with low-risk papillary thyroid microcarcinoma: a retrospective analysis of 1001 patients
Kai Qian, Kai Guo, Xiaoke Zheng, Tuanqi Sun, Duanshu Li, Yi Wu, Qinghai Ji, Zhuoying Wang
Oncotarget.2017; 8(39): 65836. CrossRef - 10.1016/j.bjorlp.2018.01.005
CrossRef Listing of Deleted DOIs.2000;[Epub] CrossRef
- A machine learning model utilizing Delphian lymph node characteristics to predict contralateral central lymph node metastasis in papillary thyroid carcinoma: a prospective multicenter study
- Interobserver Agreement on Pathologic Features of Liver Biopsy Tissue in Patients with Nonalcoholic Fatty Liver Disease
- Eun Sun Jung, Kyoungbun Lee, Eunsil Yu, Yun Kyung Kang, Mee-Yon Cho, Joon Mee Kim, Woo Sung Moon, Jin Sook Jeong, Cheol Keun Park, Jae-Bok Park, Dae Young Kang, Jin Hee Sohn, So-Young Jin
- J Pathol Transl Med. 2016;50(3):190-196. Published online April 18, 2016
- DOI: https://doi.org/10.4132/jptm.2016.03.01
- 12,260 View
- 261 Download
- 27 Web of Science
- 26 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The histomorphologic criteria for the pathological features of liver tissue from patients with non-alcoholic fatty liver disease (NAFLD) remain subjective, causing confusion among pathologists and clinicians. In this report, we studied interobserver agreement of NAFLD pathologic features and analyzed causes of disagreement.
Methods
Thirty-one cases of clinicopathologically diagnosed NAFLD from 10 hospitals were selected. One hematoxylin and eosin and one Masson’s trichrome-stained virtual slide from each case were blindly reviewed with regard to 12 histological parameters by 13 pathologists in a gastrointestinal study group of the Korean Society of Pathologists. After the first review, we analyzed the causes of disagreement and defined detailed morphological criteria. The glass slides from each case were reviewed a second time after a consensus meeting. The degree of interobserver agreement was determined by multi-rater kappa statistics.
Results
Kappa values of the first review ranged from 0.0091–0.7618. Acidophilic bodies (k = 0.7618) and portal inflammation (k = 0.5914) showed high levels of agreement, whereas microgranuloma (k = 0.0984) and microvesicular fatty change (k = 0.0091) showed low levels of agreement. After the second review, the kappa values of the four major pathological features increased from 0.3830 to 0.5638 for steatosis grade, from 0.1398 to 0.2815 for lobular inflammation, from 0.1923 to 0.3362 for ballooning degeneration, and from 0.3303 to 0.4664 for fibrosis.
Conclusions
More detailed histomorphological criteria must be defined for correct diagnosis and high interobserver agreement of NAFLD. -
Citations
Citations to this article as recorded by- Chronic polypharmacy, monotherapy, and deprescribing: Understanding complex effects on the hepatic proteome of aging mice
Kevin Winardi, John Mach, Matthew J. McKay, Mark P. Molloy, Sarah J. Mitchell, Michael R. MacArthur, Catriona McKenzie, David G. Le Couteur, Sarah N. Hilmer
Aging Cell.2025;[Epub] CrossRef - Utility of AI digital pathology as an aid for pathologists scoring fibrosis in MASH
Desiree Abdurrachim, Serene Lek, Charlene Zhi Lin Ong, Chun Kit Wong, Yongqi Zhou, Aileen Wee, Gwyneth Soon, Timothy J. Kendall, Michael O. Idowu, Christopher Hendra, Ashmita Saigal, Radha Krishnan, Elaine Chng, Dean Tai, Gideon Ho, Thomas Forest, Annaswa
Journal of Hepatology.2025; 82(5): 898. CrossRef - Artificial intelligence scoring of liver biopsies in a phase II trial of semaglutide in nonalcoholic steatohepatitis
Vlad Ratziu, Sven Francque, Cynthia A. Behling, Vanja Cejvanovic, Helena Cortez-Pinto, Janani S. Iyer, Niels Krarup, Quang Le, Anne-Sophie Sejling, Dina Tiniakos, Stephen A. Harrison
Hepatology.2024; 80(1): 173. CrossRef - Classification of the Stages of Nonalcoholic Steatohepatitis via Federated General Visual Representation Learning
Mehmet Nergiz
International Journal of Imaging Systems and Technology.2024;[Epub] CrossRef - Outcome prediction in metabolic dysfunction‐associated steatotic liver disease using stain‐free digital pathological assessment
Timothy J. Kendall, Elaine Chng, Yayun Ren, Dean Tai, Gideon Ho, Jonathan A. Fallowfield
Liver International.2024; 44(10): 2511. CrossRef - Non-alcoholic fatty liver disease: the pathologist’s perspective
Wei-Qiang Leow, Anthony Wing-Hung Chan, Paulo Giovanni L. Mendoza, Regina Lo, Kihan Yap, Haeryoung Kim
Clinical and Molecular Hepatology.2023; 29(Suppl): S302. CrossRef - CT-based Hounsfield unit values reflect the degree of steatohepatitis in patients with low-grade fatty liver disease
Ha Neul Kim, Hong Jae Jeon, Hei Gwon Choi, In Sun Kwon, Woo Sun Rou, Jeong Eun Lee, Tae Hee Lee, Seok Hyun Kim, Byung Seok Lee, Kyung Sook Shin, Hyun Jung Lee, Hyuk Soo Eun
BMC Gastroenterology.2023;[Epub] CrossRef - Artificial intelligence and deep learning: New tools for histopathological diagnosis of nonalcoholic fatty liver disease/nonalcoholic steatohepatitis
Yoshihisa Takahashi, Erdenetsogt Dungubat, Hiroyuki Kusano, Toshio Fukusato
Computational and Structural Biotechnology Journal.2023; 21: 2495. CrossRef - An integrated gene-to-outcome multimodal database for metabolic dysfunction-associated steatotic liver disease
Timothy J. Kendall, Maria Jimenez-Ramos, Frances Turner, Prakash Ramachandran, Jessica Minnier, Michael D. McColgan, Masood Alam, Harriet Ellis, Donald R. Dunbar, Gabriele Kohnen, Prakash Konanahalli, Karin A. Oien, Lucia Bandiera, Filippo Menolascina, An
Nature Medicine.2023; 29(11): 2939. CrossRef - Improved pathology reporting in NAFLD/NASH for clinical trials
Caitlin Rose Langford, Marc H Goldinger, Darren Treanor, Clare McGenity, Jonathan R Dillman, Daniela S Allende, Robert Goldin, Elizabeth M Brunt, Kurt Zatloukal, Helmut Denk, Kenneth A Fleming
Journal of Clinical Pathology.2022; 75(2): 73. CrossRef - Standardizing the histological assessment of late posttransplantation biopsies from pediatric liver allograft recipients
Stefan G. Hübscher, Sandy Feng, Annette S. H. Gouw, Hironori Haga, Hyo Jeong Kang, Deirdre A. Kelly, Mina Komuta, Andrew Lesniak, Benjamin A. Popp, Henkjan J. Verkade, Eunsil Yu, Anthony J. Demetris
Liver Transplantation.2022; 28(9): 1475. CrossRef - Discordant pathological diagnosis of non‐alcoholic fatty liver disease: A prospective multicenter study
Takuya Kuwashiro, Hirokazu Takahashi, Hideyuki Hyogo, Yuji Ogawa, Kento Imajo, Masato Yoneda, Takashi Nakahara, Satoshi Oeda, Kenichi Tanaka, Yuichiro Amano, Shinji Ogawa, Atsushi Kawaguchi, Shinichi Aishima, Masayoshi Kage, Kazuaki Chayama, Atsushi Nakaj
JGH Open.2020; 4(3): 497. CrossRef - Obeticholic acid for the treatment of nonalcoholic steatohepatitis: Expectations and concerns
Stergios A. Polyzos, Jannis Kountouras, Christos S. Mantzoros
Metabolism.2020; 104: 154144. CrossRef - A scoring system for the diagnosis of non-alcoholic steatohepatitis from liver biopsy
Kyoungbun Lee, Eun Sun Jung, Eunsil Yu, Yun Kyung Kang, Mee-Yon Cho, Joon Mee Kim, Woo Sung Moon, Jin Sook Jeong, Cheol Keun Park, Jae-Bok Park, Dae Young Kang, Jin Hee Sohn, So-Young Jin
Journal of Pathology and Translational Medicine.2020; 54(3): 228. CrossRef - An Improved qFibrosis Algorithm for Precise Screening and Enrollment into Non-Alcoholic Steatohepatitis (NASH) Clinical Trials
Wei-Qiang Leow, Pierre Bedossa, Feng Liu, Lai Wei, Kiat-Hon Lim, Wei-Keat Wan, Yayun Ren, Jason Pik-Eu Chang, Chee-Kiat Tan, Aileen Wee, George Boon-Bee Goh
Diagnostics.2020; 10(9): 643. CrossRef - Deep learning quantification of percent steatosis in donor liver biopsy frozen sections
Lulu Sun, Jon N. Marsh, Matthew K. Matlock, Ling Chen, Joseph P. Gaut, Elizabeth M. Brunt, S. Joshua Swamidass, Ta-Chiang Liu
EBioMedicine.2020; 60: 103029. CrossRef - Magnetic resonance elastography SE-EPI vs GRE sequences at 3T in a pediatric population with liver disease
Juan S. Calle-Toro, Suraj D. Serai, Erum A. Hartung, David J. Goldberg, Bradley D. Bolster, Kassa Darge, Sudha A. Anupindi
Abdominal Radiology.2019; 44(3): 894. CrossRef - R2 relaxometry based MR imaging for estimation of liver iron content: A comparison between two methods
Juan S. Calle-Toro, Christian A. Barrera, Dmitry Khrichenko, Hansel J. Otero, Suraj D. Serai
Abdominal Radiology.2019; 44(9): 3058. CrossRef - Inhibition of mitochondrial fatty acid oxidation in drug-induced hepatic steatosis
Bernard Fromenty
Liver Research.2019; 3(3-4): 157. CrossRef - Standardising the interpretation of liver biopsies in non‐alcoholic fatty liver disease clinical trials
Rish K. Pai, David E. Kleiner, John Hart, Oyedele A. Adeyi, Andrew D. Clouston, Cynthia A. Behling, Dhanpat Jain, Sanjay Kakar, Mayur Brahmania, Lawrence Burgart, Kenneth P. Batts, Mark A. Valasek, Michael S. Torbenson, Maha Guindi, Hanlin L. Wang, Veeral
Alimentary Pharmacology & Therapeutics.2019; 50(10): 1100. CrossRef - NAFLD Histology: a Critical Review and Comparison of Scoring Systems
Rish K. Pai
Current Hepatology Reports.2019; 18(4): 473. CrossRef - Hepatic sonic hedgehog protein expression measured by computer assisted morphometry significantly correlates with features of non-alcoholic steatohepatitis
Michael Estep, Rohini Mehta, Gary Bratthauer, Lakshmi Alaparthi, Fanny Monge, Simon Ali, Dinan Abdelatif, Zahra Younoszai, Maria Stepanova, Zachary D. Goodman, Zobair M. Younossi
BMC Gastroenterology.2019;[Epub] CrossRef - Validation of intimate correlation between visceral fat and hepatic steatosis: Quantitative measurement techniques using CT for area of fat and MR for hepatic steatosis
Moon Hyung Choi, Joon-Il Choi, Michael Yong Park, Sung Eun Rha, Soon Nam Oh, Seung Eun Jung, Jae Young Byun, Stephan Kannengiesser, Yohan Son
Clinical Nutrition.2018; 37(1): 214. CrossRef - Ultrasound or MR elastography of liver: which one shall I use?
Meng Yin, Sudhakar K. Venkatesh
Abdominal Radiology.2018; 43(7): 1546. CrossRef - Feasibility and agreement of stiffness measurements using gradient-echo and spin-echo MR elastography sequences in unselected patients undergoing liver MRI
Guilherme Moura Cunha, Kevin J Glaser, Anke Bergman, Rodrigo P Luz, Eduardo H de Figueiredo, Flavia Paiva Proença Lobo Lopes
The British Journal of Radiology.2018; : 20180126. CrossRef - Second harmonic generation microscopy provides accurate automated staging of liver fibrosis in patients with non-alcoholic fatty liver disease
Pik Eu Chang, George Boon Bee Goh, Wei Qiang Leow, Liang Shen, Kiat Hon Lim, Chee Kiat Tan, Manlio Vinciguerra
PLOS ONE.2018; 13(6): e0199166. CrossRef
- Chronic polypharmacy, monotherapy, and deprescribing: Understanding complex effects on the hepatic proteome of aging mice
- Core Needle Biopsy Is a More Conclusive Follow-up Method Than Repeat Fine Needle Aspiration for Thyroid Nodules with Initially Inconclusive Results: A Systematic Review and Meta-Analysis
- Jung-Soo Pyo, Jin Hee Sohn, Guhyun Kang
- J Pathol Transl Med. 2016;50(3):217-224. Published online April 14, 2016
- DOI: https://doi.org/10.4132/jptm.2016.02.15
- 10,884 View
- 116 Download
- 18 Web of Science
- 18 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
This study investigated the appropriate management of thyroid nodules with prior non-diagnostic or atypia of undetermined significance/follicular lesion of undetermined significance (AUS/FLUS) through a systematic review and meta-analysis.
Methods
This study included 4,235 thyroid nodules from 26 eligible studies. We investigated the conclusive rate of follow-up core needle biopsy (CNB) or repeat fine needle aspiration (rFNA) after initial fine needle aspiration (FNA) with non-diagnostic or AUS/FLUS results. A diagnostic test accuracy (DTA) review was performed to determine the diagnostic role of the follow-up CNB and to calculate the area under the curve (AUC) on the summary receiver operating characteristic (SROC) curve.
Results
The conclusive rates of follow-up CNB and rFNA after initial FNA were 0.879 (95% confidence interval [CI], 0.801 to 0.929) and 0.684 (95% CI, 0.627 to 0.736), respectively. In comparison of the odds ratios of CNB and rFNA, CNB had more frequent conclusive results than rFNA (odds ratio, 5.707; 95% CI, 2.530 to 12.875). Upon subgroup analysis, follow-up CNB showed a higher conclusive rate than rFNA in both initial non-diagnostic and AUS/FLUS subgroups. In DTA review of followup CNB, the pooled sensitivity and specificity were 0.94 (95% CI, 0.88 to 0.97) and 0.88 (95% CI, 0.84 to 0.91), respectively. The AUC for the SROC curve was 0.981, nearing 1.
Conclusions
Our results show that CNB has a higher conclusive rate than rFNA when the initial FNA produced inconclusive results. Further prospective studies with more detailed criteria are necessary before follow-up CNB can be applied in daily practice. -
Citations
Citations to this article as recorded by- Diagnostic yield of fine needle aspiration with simultaneous core needle biopsy for thyroid nodules
Mohammad Ali Hasannia, Ramin Pourghorban, Hoda Asefi, Amir Aria, Elham Nazar, Hojat Ebrahiminik, Alireza Mohamadian
Journal of Pathology and Translational Medicine.2025; 59(3): 180. CrossRef - Fine Needle Aspiration Cytology vs. Core Needle Biopsy for Thyroid Nodules: A Prospective, Experimental Study Using Surgical Specimen
Hyuk Kwon, Jandee Lee, Soon Won Hong, Hyeong Ju Kwon, Jin Young Kwak, Jung Hyun Yoon
Journal of the Korean Society of Radiology.2022; 83(3): 645. CrossRef - Comparison of Core Needle Biopsy and Repeat Fine-Needle Aspiration in Avoiding Diagnostic Surgery for Thyroid Nodules Initially Diagnosed as Atypia/Follicular Lesion of Undetermined Significance
Leehi Joo, Dong Gyu Na, Ji-hoon Kim, Hyobin Seo
Korean Journal of Radiology.2022; 23(2): 280. CrossRef - Diagnostic performance of core needle biopsy as a first‐line diagnostic tool for thyroid nodules according to ultrasound patterns: Comparison with fine needle aspiration using propensity score matching analysis
Hye Shin Ahn, Inyoung Youn, Dong Gyu Na, Soo Jin Kim, Mi Yeon Lee
Clinical Endocrinology.2021; 94(3): 494. CrossRef - Usage and Diagnostic Yield of Fine-Needle Aspiration Cytology and Core Needle Biopsy in Thyroid Nodules: A Systematic Review and Meta-Analysis of Literature Published by Korean Authors
Soon-Hyun Ahn
Clinical and Experimental Otorhinolaryngology.2021; 14(1): 116. CrossRef - 2021 Korean Thyroid Imaging Reporting and Data System and Imaging-Based Management of Thyroid Nodules: Korean Society of Thyroid Radiology Consensus Statement and Recommendations
Eun Ju Ha, Sae Rom Chung, Dong Gyu Na, Hye Shin Ahn, Jin Chung, Ji Ye Lee, Jeong Seon Park, Roh-Eul Yoo, Jung Hwan Baek, Sun Mi Baek, Seong Whi Cho, Yoon Jung Choi, Soo Yeon Hahn, So Lyung Jung, Ji-hoon Kim, Seul Kee Kim, Soo Jin Kim, Chang Yoon Lee, Ho K
Korean Journal of Radiology.2021; 22(12): 2094. CrossRef - Malignancy rate of Bethesda category III thyroid nodules according to ultrasound risk stratification system and cytological subtype
Won Sang Yoo, Hwa Young Ahn, Hye Shin Ahn, Yun Jae Chung, Hee Sung Kim, Bo Youn Cho, Mirinae Seo, Jae Hoon Moon, Young Joo Park
Medicine.2020; 99(2): e18780. CrossRef - 2019 Practice guidelines for thyroid core needle biopsy: a report of the Clinical Practice Guidelines Development Committee of the Korean Thyroid Association
Chan Kwon Jung, Jung Hwan Baek, Dong Gyu Na, Young Lyun Oh, Ka Hee Yi, Ho-Cheol Kang
Journal of Pathology and Translational Medicine.2020; 54(1): 64. CrossRef - Laser Ablation Versus Radiofrequency Ablation for Benign Non-Functioning Thyroid Nodules: Six-Month Results of a Randomized, Parallel, Open-Label, Trial (LARA Trial)
Roberto Cesareo, Claudio Maurizio Pacella, Valerio Pasqualini, Giuseppe Campagna, Mario Iozzino, Andrea Gallo, Angelo Lauria Pantano, Roberto Cianni, Claudio Pedone, Paolo Pozzilli, Chiara Taffon, Anna Crescenzi, Silvia Manfrini, Andrea Palermo
Thyroid.2020; 30(6): 847. CrossRef - Diagnostic Efficacy and Safety of Core Needle Biopsy as a First-Line Diagnostic Method for Thyroid Nodules: A Prospective Cohort Study
Min Ji Hong, Dong Gyu Na, Hunkyung Lee
Thyroid.2020; 30(8): 1141. CrossRef - Is thyroid core needle biopsy a valid compliment to fine-needle aspiration?
Liron Pantanowitz, Lester D.R. Thompson, Xin Jing, Esther Diana Rossi
Journal of the American Society of Cytopathology.2020; 9(5): 383. CrossRef - A Monocentric Retrospective Study about the Correlation between Histology and Cytology of Thyroid Indeterminate Nodules Classified as TIR 3A and TIR 3B, according to 2014 Italian Consensus for Classification and Reporting of Thyroid Cytology
Francesco Quaglino, Giulia Arnulfo, Sergio Sandrucci, Claudio Rossi, Valentina Marchese, Roberto Saracco, Stefano Guzzetti, Stefano Taraglio, Enrico Mazza
Advances in Medicine.2019; 2019: 1. CrossRef - Nuclear features of papillary thyroid carcinoma: Comparison of Core needle biopsy and thyroidectomy specimens
Jae Yeon Seok, Jungsuk An, Hyun Yee Cho, Younghye Kim, Seung Yeon Ha
Annals of Diagnostic Pathology.2018; 32: 35. CrossRef - Statement and Recommendations on Interventional Ultrasound as a Thyroid Diagnostic and Treatment Procedure
Christoph F. Dietrich, Thomas Müller, Jörg Bojunga, Yi Dong, Giovanni Mauri, Maija Radzina, Manjiri Dighe, Xin-Wu Cui, Frank Grünwald, Andreas Schuler, Andre Ignee, Huedayi Korkusuz
Ultrasound in Medicine & Biology.2018; 44(1): 14. CrossRef - Role of core needle biopsy as a first-line diagnostic tool for thyroid nodules: a retrospective cohort study
Min Ji Hong, Dong Gyu Na, Soo Jin Kim, Dae Sik Kim
Ultrasonography.2018; 37(3): 244. CrossRef - Core Needle Biopsy of the Thyroid: 2016 Consensus Statement and Recommendations from Korean Society of Thyroid Radiology
Dong Gyu Na, Jung Hwan Baek, So Lyung Jung, Ji-hoon Kim, Jin Yong Sung, Kyu Sun Kim, Jeong Hyun Lee, Jung Hee Shin, Yoon Jung Choi, Eun Ju Ha, Hyun Kyung Lim, Soo Jin Kim, Soo Yeon Hahn, Kwang Hwi Lee, Young Jun Choi, Inyoung Youn, Young Joong Kim, Hye Sh
Korean Journal of Radiology.2017; 18(1): 217. CrossRef - Ultrasound-guided fine needle aspiration versus core needle biopsy: comparison of post-biopsy hematoma rates and risk factors
In Hye Chae, Eun-Kyung Kim, Hee Jung Moon, Jung Hyun Yoon, Vivian Y. Park, Jin Young Kwak
Endocrine.2017; 57(1): 108. CrossRef - The Role of Core Needle Biopsy for Thyroid Nodules with Initially Indeterminate Results on Previous Fine-Needle Aspiration: A Systematic Review and Meta-Analysis
C.H. Suh, J.H. Baek, C. Park, Y.J. Choi, J.H. Lee
American Journal of Neuroradiology.2017; 38(7): 1421. CrossRef
- Diagnostic yield of fine needle aspiration with simultaneous core needle biopsy for thyroid nodules
- MUC2 Expression Is Correlated with Tumor Differentiation and Inhibits Tumor Invasion in Gastric Carcinomas: A Systematic Review and Meta-analysis
- Jung-Soo Pyo, Jin Hee Sohn, Guhyun Kang, Dong-Hoon Kim, Kyungeun Kim, In-Gu Do, Dong Hyun Kim
- J Pathol Transl Med. 2015;49(3):249-256. Published online May 15, 2015
- DOI: https://doi.org/10.4132/jptm.2015.03.27
- 8,810 View
- 70 Download
- 6 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
While MUC2 is expressed in intestinal metaplasia and malignant lesions, the clinico-pathological significance of MUC2 expression is not fully elucidated in gastric carcinoma (GC). Methods: The present study investigated the correlation between MUC2 expression and clinico-pathological parameters in 167 human GCs. In addition, to confirm the clinicopathological significance of MUC2 expression, we performed a systematic review and meta-analysis in 1,832 GCs. Results: MUC2 expression was found in 58 of 167 GCs (34.7%). MUC2-expressing GC showed lower primary tumor (T), regional lymph node (N), and tumor node metastasis (TNM) stages compared with GCs without MUC2 expression (p=.001, p=.001, and p=.011, respectively). However, MUC2 expression was not correlated with Lauren’s classification and tumor differentiation. In meta-analysis, MUC2 expression was significantly correlated with differentiation and lower tumor stage (odds ratio [OR], 1.303; 95% confidence interval [CI], 1.020 to 1.664; p = .034 and OR, 1.352; 95% CI, 1.055 to 1.734; p = .017, respectively) but not with Lauren’s classification, pN stage, or pTNM stage. Conclusions: MUC2 expression was correlated with a lower tumor depth and lower lymph node metastasis in our study; the meta-analysis showed a correlation of MUC2 expression with tumor differentiation and lower tumor depth. -
Citations
Citations to this article as recorded by- Prognostic and clinicopathological significance of mucin family members expression in gastric cancer: a meta-analysis
Shunda Wang, Yongrun Mu, Jianwei Zhang, Chengfeng Wang
Frontiers in Oncology.2025;[Epub] CrossRef - Diagnostic gastrointestinal markers in primary lung cancer and pulmonary metastases
Karina Malmros, Andreas Lindholm, Halla Vidarsdottir, Karin Jirström, Björn Nodin, Johan Botling, Johanna S. M. Mattsson, Patrick Micke, Maria Planck, Mats Jönsson, Johan Staaf, Hans Brunnström
Virchows Archiv.2024; 485(2): 347. CrossRef - Gastric epithelial histology and precancerous conditions
Hang Yang, Wen-Juan Yang, Bing Hu
World Journal of Gastrointestinal Oncology.2022; 14(2): 396. CrossRef - COX-2 strengthens the effects of acid and bile salts on human esophageal cells and Barrett esophageal cells
Shen Jiangang, Kang Nayoung, Wang Hongfang, Li Junda, Chen Li, Bai Xuefeng, Li Mingsong
BMC Molecular and Cell Biology.2022;[Epub] CrossRef - Comparative genomic analysis of primary tumors and paired brain metastases in lung cancer patients by whole exome sequencing: a pilot study
Pascale Tomasini, Fabrice Barlesi, Sophie Gilles, Isabelle Nanni-Metellus, Riccardo Soffietti, Emilie Denicolai, Eric Pellegrino, Emilie Bialecki, L’Houcine Ouafik, Philippe Metellus
Oncotarget.2020; 11(50): 4648. CrossRef - A High Ki67/BCL2 Index Could Predict Lower Disease-Free and Overall Survival in Intestinal-Type Gastric Cancer
Kyueng-Whan Min, Dong-Hoon Kim, Byoung Kwan Son, Dong Hyun Kim, Eun-Kyung Kim, Jinwon Seo, Sang Bong Ahn, Yun Ju Jo, Young Sook Park, Junghoon Ha
European Surgical Research.2017; 58(3-4): 158. CrossRef
- Prognostic and clinicopathological significance of mucin family members expression in gastric cancer: a meta-analysis
- Traumatic Bowel Perforation and Inguinal Hernia Masking a Mesenteric Calcifying Fibrous Tumor
- Dong Hyun Kim, Kyueng-Whan Min, Dong-Hoon Kim, Seoung Wan Chae, Jin Hee Sohn, Jung-Soo Pyo, Sung-Im Do, Kyungeun Kim, Hyun Joo Lee
- J Pathol Transl Med. 2015;49(3):267-269. Published online May 15, 2015
- DOI: https://doi.org/10.4132/jptm.2015.03.20
- 8,356 View
- 50 Download
- 1 Web of Science
- 1 Crossref
- Cytological Evaluation and REBA HPV-ID HPV Testing of Newly Developed Liquid-Based Cytology, EASYPREP: Comparison with SurePath
- Youn Soo Lee, Gyungyub Gong, Jin Hee Sohn, Ki Sung Ryu, Jung Hun Lee, Shin Kwang Khang, Kyung-Ja Cho, Yong-Man Kim, Chang Suk Kang
- Korean J Pathol. 2013;47(3):265-274. Published online June 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.3.265
- 10,768 View
- 94 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF Background The objective of this study was to evaluate a newly-developed EASYPREP liquid-based cytology method in cervicovaginal specimens and compare it with SurePath.
Methods Cervicovaginal specimens were prospectively collected from 1,000 patients with EASYPREP and SurePath. The specimens were first collected by brushing for SurePath and second for EASYPREP. The specimens of both methods were diagnosed according to the Bethesda System. Additionally, we performed to REBA HPV-ID genotyping and sequencing analysis for human papillomavirus (HPV) on 249 specimens.
Results EASYPREP and SurePath showed even distribution of cells and were equal in cellularity and staining quality. The diagnostic agreement between the two methods was 96.5%. Based on the standard of SurePath, the sensitivity, specificity, positive predictive value, and negative predictive value of EASYPREP were 90.7%, 99.2%, 94.8%, and 98.5%, respectively. The positivity of REBA HPV-ID was 49.4% and 95.1% in normal and abnormal cytological samples, respectively. The result of REBA HPV-ID had high concordance with sequencing analysis.
Conclusions EASYPREP provided comparable results to SurePath in the diagnosis and staining quality of cytology examinations and in HPV testing with REBA HPV-ID. EASYPREP could be another LBC method choice for the cervicovaginal specimens. Additionally, REBA HPV-ID may be a useful method for HPV genotyping.
-
Citations
Citations to this article as recorded by- Virome capture sequencing for comprehensive HPV genotyping in cervical samples
Thanayod Sasivimolrattana, Sasiprapa Liewchalermwong, Wasun Chantratita, Insee Sensorn, Arkom Chaiwongkot, Parvapan Bhattarakosol
Science Progress.2025;[Epub] CrossRef - High-Risk Human Papillomavirus Detection via Cobas® 4800 and REBA HPV-ID® Assays
Sasiprapa Liewchalermwong, Shina Oranratanaphan, Wichai Termrungruanglert, Surang Triratanachat, Patou Tantbirojn, Nakarin Kitkumthorn, Parvapan Bhattarakosol, Arkom Chaiwongkot
Viruses.2022; 14(12): 2713. CrossRef - Evaluation of nuclear chromatin using grayscale intensity and thresholded percentage area in liquid‐based cervical cytology
Hyekyung Lee, Myungein Han, Taejo Yoo, Chanho Jung, Hyun‐Jin Son, Migyung Cho
Diagnostic Cytopathology.2018; 46(5): 384. CrossRef - Comparison of EASYPREP® and SurePath® in thyroid fine‐needle aspiration
Yosep Chong, Ki Hyun Baek, Jee Young Kim, Tae‐Jung Kim, Eun Jung Lee, Chang Suk Kang
Diagnostic Cytopathology.2016; 44(4): 283. CrossRef
- Virome capture sequencing for comprehensive HPV genotyping in cervical samples
- Early Colorectal Epithelial Neoplasm in Korea: A Multicenter Survey of Pathologic Diagnosis
- Yun Kyung Kang, So-Young Jin, Mee Soo Chang, Jung Yeon Kim, Gyeong Hoon Kang, Hye Seung Lee, Jin Hee Sohn, Ho Sung Park, Kye Won Kwon, Mi Jin Gu, Young Hee Maeng, Jong Eun Joo, Haeng Ji Kang, Hee Kyung Kim, Kee-Taek Jang, Mi Ja Lee, Hee Kyung Chang, Joon Mee Kim, Hye Seung Han, Won Ae Lee, Yoon Jung Choi, Dong Wook Kang, Sunhoo Park, Jae Hyuk Lee, Mee-Yon Cho
- Korean J Pathol. 2013;47(3):245-251. Published online June 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.3.245
- 10,463 View
- 56 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF Background The incidence of early colorectal epithelial neoplasm (ECEN) is increasing, and its pathologic diagnosis is important for patient care. We investigated the incidence of ECEN and the current status of its pathologic diagnosis.
Methods We collected datasheets from 25 institutes in Korea for the incidence of colorectal adenoma with high grade dysplasia (HGD) and low grade dysplasia in years 2005, 2007, and 2009; and early colorectal carcinoma in the year 2009. We also surveyed the diagnostic terminology of ECEN currently used by the participating pathologists.
Results The average percentage of diagnoses of adenoma HGD was 7.0%, 5.0%, and 3.4% in years 2005, 2007, and 2009, respectively. The range of incidence rates of adenoma HGD across the participating institutes has gradually narrowed over the years 2005 to 2009. The incidence rate of early colorectal carcinoma in the year 2009 was 21.2%. The participants did not share a single criterion or terminology for the diagnosis of adenoma HGD. The majority accepted the diagnostic terms that distinguished noninvasive, mucosal confined, and submucosal invasive carcinoma.
Conclusions Further research requirements suggested are a diagnostic consensus for the histopathologic diagnosis of ECEN; and standardization of diagnostic terminology critical for determining the disease code.
-
Citations
Citations to this article as recorded by- Diminutive and Small Colorectal Polyps: The Pathologist's Perspective
Yun Kyung Kang
Clinical Endoscopy.2014; 47(5): 404. CrossRef
- Diminutive and Small Colorectal Polyps: The Pathologist's Perspective
- Proposal for a Standardized Pathology Report of Gastroenteropancreatic Neuroendocrine Tumors: Prognostic Significance of Pathological Parameters
- Mee-Yon Cho, Jin Hee Sohn, So Young Jin, Hyunki Kim, Eun Sun Jung, Mi-Jung Kim, Kyoung-Mee Kim, Woo Ho Kim, Joon Mee Kim, Yun Kyung Kang, Joon Hyuk Choi, Dae Young Kang, Youn Wha Kim, Eun Hee Choi
- Korean J Pathol. 2013;47(3):227-237. Published online June 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.3.227
- 14,277 View
- 145 Download
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF Background There is confusion in the diagnosis and biological behaviors of gastroenteropancreatic neuroendocrine tumors (GEP-NETs), because of independently proposed nomenclatures and classifications. A standardized form of pathology report is required for the proper management of patients.
Methods We discussed the proper pathological evaluation of GEP-NET at the consensus conference of the subcommittee meeting for the Gastrointestinal Pathology Study Group of the Korean Society of Pathologists. We then verified the prognostic significance of pathological parameters from our previous nationwide collection of pathological data from 28 hospitals in Korea to determine the essential data set for a pathology report.
Results Histological classification, grading (mitosis and/or Ki-67 labeling index), T staging (extent, size), lymph node metastasis, and lymphovascular and perineural invasion were significant prognostic factors and essential for the pathology report of GEP-NET, while immunostaining such as synaptophysin and chromogranin may be optional. Furthermore, the staging system, either that of the 2010 American Joint Cancer Committee (AJCC) or the European Neuroendocrine Tumor Society (ENETS), should be specified, especially for pancreatic neuroendocrine neoplasms.
Conclusions A standardized pathology report is crucial for the proper management and prediction of prognosis of patients with GEP-NET.
-
Citations
Citations to this article as recorded by- Analysis of Prognostic Risk Factors of Endoscopic Submucosal Dissection (ESD) and Curative Resection of Gastrointestinal Neuroendocrine Neoplasms
Yuan Si, ChaoKang Huang, JingBin Yuan, XianHui Zhang, QingQiang He, ZhiJin Lin, Ling He, ZhongXin Liu, Yuvaraja Teekaraman
Contrast Media & Molecular Imaging.2022;[Epub] CrossRef - Standardization of the pathologic diagnosis of appendiceal mucinous neoplasms
Dong-Wook Kang, Baek-hui Kim, Joon Mee Kim, Jihun Kim, Hee Jin Chang, Mee Soo Chang, Jin-Hee Sohn, Mee-Yon Cho, So-Young Jin, Hee Kyung Chang, Hye Seung Han, Jung Yeon Kim, Hee Sung Kim, Do Youn Park, Ha Young Park, So Jeong Lee, Wonae Lee, Hye Seung Lee,
Journal of Pathology and Translational Medicine.2021; 55(4): 247. CrossRef - Preoperative diagnosis of well‐differentiated neuroendocrine tumor in common hepatic duct by brush cytology: A case report
Jiwoon Choi, Kyong Joo Lee, Sung Hoon Kim, Mee‐Yon Cho
Diagnostic Cytopathology.2019; 47(7): 720. CrossRef - Primary renal well-differentiated neuroendocrine tumors: report of six cases with an emphasis on the Ki-67 index and mitosis
Bohyun Kim, Han-Seong Kim, Kyung Chul Moon
Diagnostic Pathology.2019;[Epub] CrossRef - Primary low‐grade neuroendocrine carcinoma of the skin: An exceedingly rare entity
Tiffany Y. Chen, Annie O. Morrison, Joe Susa, Clay J. Cockerell
Journal of Cutaneous Pathology.2017; 44(11): 978. CrossRef - Prognostic Validity of the American Joint Committee on Cancer and the European Neuroendocrine Tumors Staging Classifications for Pancreatic Neuroendocrine Tumors
Jae Hee Cho, Ji Kon Ryu, Si Young Song, Jin-Hyeok Hwang, Dong Ki Lee, Sang Myung Woo, Young-Eun Joo, Seok Jeong, Seung-Ok Lee, Byung Kyu Park, Young Koog Cheon, Jimin Han, Tae Nyeun Kim, Jun Kyu Lee, Sung-Hoon Moon, Hyunjin Kim, Eun Taek Park, Jae Chul Hw
Pancreas.2016; 45(7): 941. CrossRef - Early diagnosis and treatment of gastrointestinal neuroendocrine tumors
Hong Shen, Zhuo Yu, Jing Zhao, Xiu-Zhen Li, Wen-Sheng Pan
Oncology Letters.2016; 12(5): 3385. CrossRef - Recent Updates on Neuroendocrine Tumors From the Gastrointestinal and Pancreatobiliary Tracts
Joo Young Kim, Seung-Mo Hong
Archives of Pathology & Laboratory Medicine.2016; 140(5): 437. CrossRef - Pancreatic neuroendocrine tumors: Correlation between the contrast-enhanced computed tomography features and the pathological tumor grade
Koji Takumi, Yoshihiko Fukukura, Michiyo Higashi, Junnichi Ideue, Tomokazu Umanodan, Hiroto Hakamada, Ichiro Kanetsuki, Takashi Yoshiura
European Journal of Radiology.2015; 84(8): 1436. CrossRef - Tumeurs neuroendocrines du tube digestif et du pancréas : ce que le pathologiste doit savoir et doit faire en 2014
Jean-Yves Scoazec, Anne Couvelard
Annales de Pathologie.2014; 34(1): 40. CrossRef - Spectrum of Gastroenteropancreatic NENs in Routine Histological Examinations of Bioptic and Surgical Specimen: A Study of 161 Cases Collected from 17 Departments of Pathology in the Czech Republic
Václav Mandys, Tomáš Jirásek
Gastroenterology Research and Practice.2014; 2014: 1. CrossRef - p27 Loss Is Associated with Poor Prognosis in Gastroenteropancreatic Neuroendocrine Tumors
Hee Sung Kim, Hye Seung Lee, Kyung Han Nam, Jiwoon Choi, Woo Ho Kim
Cancer Research and Treatment.2014; 46(4): 383. CrossRef
- Analysis of Prognostic Risk Factors of Endoscopic Submucosal Dissection (ESD) and Curative Resection of Gastrointestinal Neuroendocrine Neoplasms
- Update on the Proposal for Creating a Guideline for Cancer Registration of the Gastrointestinal Tumors (I-2)
- Eun Sun Jung, Yun Kyung Kang, Mee-Yon Cho, Joon Mee Kim, Won Ae Lee, Hee Eun Lee, Sunhoo Park, Jin Hee Sohn, So-Young Jin
- Korean J Pathol. 2012;46(5):443-453. Published online October 25, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.5.443
- 10,663 View
- 181 Download
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Cancer registries play a fundamental role in cancer control and multicenter collaborative research. Recently, the need for reassessment of cancer registry criteria has arisen due to the newly released 2010 World Health Organization (WHO) classification. Accordingly, development of new coding guidelines for cancer is necessary to improve the quality of cancer registries, as well as to prevent conflicts that may arise when seeking medical insurance compensation.
Methods With funding from the Management Center for Health Promotion, 35 members of the Gastrointestinal Pathology Study Group and the Cancer Registration Committee of the Korean Society of Pathologists (KSP) participated in a second workshop for gastrointestinal tumor registration in Korea.
Results The topics of gastric epithelial tumor, colonic intramucosal carcinoma, neuroendocrine tumor (NET), gastrointestinal stromal tumor (GIST) and appendiceal mucinous tumor were discussed for new coding guidelines. A survey was then conducted among 208 members of the KSP for a consensus of the guidelines proposed in the workshop.
Conclusions Although a few issues were set aside for further discussion, such as coding for non-gastric GIST and some types of NET, the members agreed upon most of the proposed guidelines. Therefore, we suggest using the newly revised International Classification of Diseases for Oncology, 3rd edition (ICD-O-3) coding guidelines for registering gastrointestinal tumors in Korea.
-
Citations
Citations to this article as recorded by- Different miRNAs Related to FBXW7 Mutations or High Mitotic Indices Contribute to Rectal Neuroendocrine Tumors: A Pilot Study
Ho Suk Kang, Ha Young Park, Hyun Lim, Il Tae Son, Min-Jeong Kim, Nan Young Kim, Min Jeong Kim, Eun Sook Nam, Seong Jin Cho, Mi Jung Kwon
International Journal of Molecular Sciences.2023; 24(7): 6329. CrossRef - Clinicopathologic Impact of Peptide Hormonal Expression in Rectal Neuroendocrine Tumors
Jisup Kim, Dong-Hoon Yang, HaeSung Jung, HyungJun Cho, Hyeung-Jin Jang, Changhoon Yoo, In Ja Park, Baek-Yeol Ryoo, Jin-Sook Ryu, Seung-Mo Hong
Archives of Pathology & Laboratory Medicine.2023; 147(7): 797. CrossRef - Prognostic nomogram and novel risk-scoring system for small cell lung cancer with different patterns of metastases
Hongli Ruan, Huali Sun, Yu Guo, Yan Ding, Yanmei Liu, Shenpeng Ying, Peipei Lin
General Thoracic and Cardiovascular Surgery.2022; 70(12): 1022. CrossRef - Development of a nomogram model to predict survival outcomes in patients with primary hepatic neuroendocrine tumors based on SEER database
Ziteng Zhang, Xin Zhao, Zhiyan Li, Youchun Wu, Yao Liu, Zhiwei Li, Guobao Li
BMC Cancer.2021;[Epub] CrossRef - Standardization of the pathologic diagnosis of appendiceal mucinous neoplasms
Dong-Wook Kang, Baek-hui Kim, Joon Mee Kim, Jihun Kim, Hee Jin Chang, Mee Soo Chang, Jin-Hee Sohn, Mee-Yon Cho, So-Young Jin, Hee Kyung Chang, Hye Seung Han, Jung Yeon Kim, Hee Sung Kim, Do Youn Park, Ha Young Park, So Jeong Lee, Wonae Lee, Hye Seung Lee,
Journal of Pathology and Translational Medicine.2021; 55(4): 247. CrossRef - Analysis of the Incidence and Clinical Features of Colorectal Nonadenocarcinoma in Korea: A National Cancer Registry-Based Study
Soomin Nam, Dongwook Kim, Kyuwon Jung, Yoon Jung Choi, Jung Gu Kang
Annals of Coloproctology.2020; 36(6): 390. CrossRef - Novel Finding of Paired Box 5 (PAX5) Cytoplasmic Staining in Well-differentiated Rectal Neuroendocrine Tumors (Carcinoids) and Its Diagnostic and Potentially Prognostic Utility
Zhiyan Fu, Chunlai Zuo, Christine E. Sheehan, Deepa T. Patil, Jingmei Lin, Zhaohai Yang, Hwajeong Lee
Applied Immunohistochemistry & Molecular Morphology.2019; 27(6): 454. CrossRef - Lymphovascular invasion as a prognostic value in small rectal neuroendocrine tumor treated by local excision: A systematic review and meta-analysis
Ho Suk Kang, Mi Jung Kwon, Tae-Hwan Kim, Junhee Han, Young-Su Ju
Pathology - Research and Practice.2019; 215(11): 152642. CrossRef - Management Colorectal Gastrointestinal Stromal Tumors (Gists) in Surabaya
Yuda Handaya, Sutamto Wibowo, Iwan Kristian
Open Journal of Gastroenterology.2016; 06(04): 97. CrossRef - Non-L-cell Immunophenotype and Large Tumor Size in Rectal Neuroendocrine Tumors Are Associated With Aggressive Clinical Behavior and Worse Prognosis
Joo Young Kim, Ki-Suk Kim, Kyung-Jo Kim, In Ja Park, Jong Lyul Lee, Seung-Jae Myung, Yangsoon Park, Young Soo Park, Chang Sik Yu, Jin Cheon Kim, Eunsil Yu, Hyeung-Jin Jang, Seung-Mo Hong
American Journal of Surgical Pathology.2015; 39(5): 632. CrossRef - Diagnostic Coding for Intramucosal Carcinoma and Neuroendocrine Tumor in the Colorectum: Proposal for Avoiding Confusing Coding in Korea
Dong Soo Han, Jin Hee Sohn, Jeong-Sik Byeon, Hwang Choi, Joon Mee Kim
Clinical Endoscopy.2015; 48(3): 216. CrossRef - Prognostic Significance of Defining L-Cell Type on the Biologic Behavior of Rectal Neuroendocrine Tumors in Relation with Pathological Parameters
Jin Hee Sohn, Mee-Yon Cho, Yangsoon Park, Hyunki Kim, Woo Ho Kim, Joon Mee Kim, Eun Sun Jung, Kyoung-Mee Kim, Jae Hyuk Lee, Hee Kyung Chan, Do Youn Park, Mee Joo, Sujin Kim, Woo Sung Moon, Mi Seon Kang, So-Young Jin, Yun Kyung Kang, Sun Och Yoon, HyeSeung
Cancer Research and Treatment.2015; 47(4): 813. CrossRef - Diminutive and Small Colorectal Polyps: The Pathologist's Perspective
Yun Kyung Kang
Clinical Endoscopy.2014; 47(5): 404. CrossRef - Highlights from the 50th Seminar of the Korean Society of Gastrointestinal Endoscopy
Eun Young Kim, Il Ju Choi, Kwang An Kwon, Ji Kon Ryu, Seok Ho Dong, Ki Baik Hahm
Clinical Endoscopy.2014; 47(4): 285. CrossRef - Early Colorectal Epithelial Neoplasm in Korea: A Multicenter Survey of Pathologic Diagnosis
Yun Kyung Kang, So-Young Jin, Mee Soo Chang, Jung Yeon Kim, Gyeong Hoon Kang, Hye Seung Lee, Jin Hee Sohn, Ho Sung Park, Kye Won Kwon, Mi Jin Gu, Young Hee Maeng, Jong Eun Joo, Haeng Ji Kang, Hee Kyung Kim, Kee-Taek Jang, Mi Ja Lee, Hee Kyung Chang, Joon
Korean Journal of Pathology.2013; 47(3): 245. CrossRef - Expression of metallothionein‐1 and metallothionein‐2 as a prognostic marker in hepatocellular carcinoma
Yangsoon Park, Eunsil Yu
Journal of Gastroenterology and Hepatology.2013; 28(9): 1565. CrossRef
- Different miRNAs Related to FBXW7 Mutations or High Mitotic Indices Contribute to Rectal Neuroendocrine Tumors: A Pilot Study
- A Proposal for Creating a Guideline for Cancer Registration of the Fibromatosis, PEComa Group, Malignant Lymphoma
In Situ and Dendritic Cell Tumors (III) - Changyoung Yoo, Chang Suk Kang, Yoon La Choi, Hye Yoon Kang, Jin Man Kim, Young Hye Koh, Joo Hee Lee, Seung Sook Lee, In Sun Kim, Dong Hoon Kim, Yong Ku Park, Jin Hee Sohn
- Korean J Pathol. 2012;46(5):436-442. Published online October 25, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.5.436
- 8,937 View
- 54 Download
-
 Abstract
Abstract
 PDF
PDF Background Understanding the biologic behavior of a tumor is a prerequisite for tumor registration code assignment. The aim of this report was to propose appropriate behavior codes of the International Classification of Disease Oncology 3 (ICD-O3) to rare, yet pathologically interesting hematopoietic and soft tissue tumors.
Methods The Study Group for Hematopathology, the Bone and Soft Tissue Pathology Study Group, and the Cancer Registration Committee prepared the questionnaire containing provisional behavior codes of selected diseases.
Results In situ lesions of mantle cell and follicular lymphomas, dendritic cell tumors, and neoplasms with perivascular epithelioid cell differentiation (PEComa), not otherwise specified were classified as malignant (-/3). The fibromatosis group, with the exception of lipofibromatosis, was proposed as benign (-/0). Lipofibromatosis and several diseases that belong to the PEComa group were proposed as uncertain malignant potential (-/1). For the hematologic and soft tissue tumors, 274 and 288 members of the Korean Society of Pathologists, respectively, provided opinions through questionnaire, and most responders showed agreement with the provisional behavior code proposed.Conclusions The determination of behavior codes for the rare diseases described in this study, especially those of the PEComa group or malignant lymphoma, could be viewed as impractical and premature, but this study provides the basis for future research on this topic.
- Extranodal Follicular Dendritic Cell Sarcoma with Rapid Growth in Parapharynx: A Case Report
- Jung-Soo Pyo, Guhyun Kang, Sung-Im Do, Seoung Wan Chae, Kyungeun Kim, Sang Hyuk Lee, Yoon-La Choi, Joon Hyuk Choi, Jin Hee Sohn, Dong-Hoon Kim
- Korean J Pathol. 2012;46(3):306-310. Published online June 22, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.3.306
- 7,391 View
- 54 Download
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Follicular dendritic cell sarcoma (FDCS) is a rare malignancy arising from the antigen-presenting cells in the lymph node and extranodal tissue. We describe a 31-year-old male patient who presented with a swelling of the left parapharynx. The radiologic findings showed a 4.7×4.5×1.9 cm-sized, ill-defined mass in the left parapharyngeal space. A fine-needle aspiration cytology was performed and it showed scattered, irregular, cohesive clusters of tumor cells with a spindle-to-ovoid shape with irregular contours in a background of lymphocytes. Based on these findings, a diagnosis of spindle cell neoplasm was made. The surgically resected tumor was composed of elongated, ovoid or polygonal cells showing positive immunohistochemistry for CD21, CD23, and CD35. Postoperatively, the residual tumor was observed to undergo a rapidly growth. There is an overlap in the cytologic and histologic findings between FDCS of the parapharynx and other tumors. Pathologists should therefore be aware of its characteristics not only to provide an accurate diagnosis but also to recommend the appropriate clinical management.
-
Citations
Citations to this article as recorded by- Extranodal Follicular Dendritic Cell Sarcoma of the Head and Neck Region: A Clinicopathological Study of 7 Cases
Nasir Ud Din, Zubair Ahmad, Shabina Rahim, Karen Fritchie, Muhammad Usman Tariq, Arsalan Ahmed
International Journal of Surgical Pathology.2023; 31(6): 1067. CrossRef - Cytomorphology of follicular dendritic cell sarcoma: a report of 7 cases with an emphasis on the diagnostic challenges
Cody Weimholt, Jalal B. Jalaly, Cedric Bailey
Journal of the American Society of Cytopathology.2023; 12(3): 229. CrossRef - Follicular dendritic cells
Seham A. Abd El‐Aleem, Entesar Ali Saber, Neven M. Aziz, Hani El‐Sherif, Asmaa M. Abdelraof, Laiche Djouhri
Journal of Cellular Physiology.2022; 237(4): 2019. CrossRef - Clinicopathological characteristics of extranodal follicular dendritic cell sarcoma: A report of two cases
Xing Zhao, Dayong Sun, Gang Zhang
Oncology Letters.2021;[Epub] CrossRef - Cytological diagnosis of follicular dendritic cell sarcoma: A case report and review of literature
A. Dutta, P. Arun, P. Roy, I. Arun
Cytopathology.2018; 29(5): 461. CrossRef - Follicular dendritic cells and related sarcoma
Fabio Facchetti, Luisa Lorenzi
Seminars in Diagnostic Pathology.2016; 33(5): 262. CrossRef - Extranodal follicular dendritic cell sarcoma: A clinicopathological report of four cases and a literature review
RUI-FEN WANG, WEI HAN, LEI QI, LI-HUI SHAN, ZHENG-CAI WANG, LI-FENG WANG
Oncology Letters.2015; 9(1): 391. CrossRef - Follicular Dendritic Cell Sarcoma of Parapharyngeal Space: A Case Report and Review of the Literature
Turki Al-Hussain, Muhammad Saleem, Suresh Babu Velagapudi, Mohammad Anas Dababo
Head and Neck Pathology.2015; 9(1): 135. CrossRef - Clinical and pathological features of head and neck follicular dendritic cell sarcoma
Ji Li, Min-Li Zhou, Shui-Hong Zhou
Hematology.2015; 20(10): 571. CrossRef
- Extranodal Follicular Dendritic Cell Sarcoma of the Head and Neck Region: A Clinicopathological Study of 7 Cases

 E-submission
E-submission



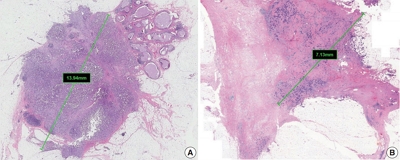
 First
First Prev
Prev



