Search
- Page Path
- HOME > Search
- Clinicopathologic characterization of cervical metastasis from an unknown primary tumor: a multicenter study in Korea
- Miseon Lee, Uiree Jo, Joon Seon Song, Youn Soo Lee, Chang Gok Woo, Dong-Hoon Kim, Jung Yeon Kim, Sun Och Yoon, Kyung-Ja Cho
- J Pathol Transl Med. 2023;57(3):166-177. Published online May 10, 2023
- DOI: https://doi.org/10.4132/jptm.2023.04.12
- 3,562 View
- 156 Download
- 4 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Research regarding cervical metastasis from an unknown primary tumor (CUP) according to human papillomavirus (HPV) and Epstein-Barr virus (EBV) status in Korea has been sporadic and small-scale. This study aims to analyze and understand the characteristics of CUP in Korea according to viral and p16 and p53 status through a multicenter study.
Methods
Ninety-five cases of CUP retrieved from six hospitals in Korea between January 2006 and December 2016 were subjected to high-risk HPV detection (DNA in situ hybridization [ISH] or real-time polymerase chain reaction), EBV detection (ISH), and immunohistochemistry for p16 and p53.
Results
CUP was HPV-related in 37 cases (38.9%), EBV-related in five cases (5.3%), and unrelated to HPV or EBV in 46 cases (48.4%). HPV-related CUP cases had the best overall survival (OS) (p = .004). According to the multivariate analysis, virus-unrelated disease (p = .023) and longer smoking duration (p < .005) were prognostic factors for poor OS. Cystic change (p = .016) and basaloid pattern (p < .001) were more frequent in HPV-related cases, and lymphoepithelial lesion was frequent in EBV-related cases (p = .010). There was no significant association between viral status and p53 positivity (p = .341), smoking status (p = .728), or smoking duration (p = .187). Korean data differ from Western data in the absence of an association among HPV, p53 positivity, and smoking history.
Conclusions
Virus-unrelated CUP in Korea had the highest frequency among all CUP cases. HPV-related CUP is similar to HPV-mediated oropharyngeal cancer and EBVrelated CUP is similar to nasopharyngeal cancer in terms of characteristics, respectively. -
Citations
Citations to this article as recorded by- Differenzierung von benignen und malignen Halszysten – eine diagnostische Herausforderung
Christina Sauter, Matthias Sand, Karim Plath, Michaela Maria Plath
Laryngo-Rhino-Otologie.2025; 104(05): 296. CrossRef - Unlocking the Hidden: Advancing Imaging Techniques in Diagnosing Cancers of Unknown Primary in the Head and Neck Region
Daniela Messineo, Filippo Valentini, Giovanni Francesco Niccolini, Federica Zoccali, Francesca Ripari, Enrico Marotta, Marcello Caratozzolo, Pasquale Frisina
Applied Sciences.2025; 15(4): 2194. CrossRef - Expansion of tumor-infiltrating lymphocytes from head and neck squamous cell carcinoma to assess the potential of adoptive cell therapy
Sangjoon Choi, Mofazzal Hossain, Hyun Lee, Jina Baek, Hye Seon Park, Chae-Lyul Lim, DoYeon Han, Taehyun Park, Jong Hyeok Kim, Gyungyub Gong, Mi-Na Kweon, Hee Jin Lee
Cancer Immunology, Immunotherapy.2024;[Epub] CrossRef
- Differenzierung von benignen und malignen Halszysten – eine diagnostische Herausforderung
- Evaluation of the characteristics of multiple human papillomavirus (HPV) infections identified using the BD Onclarity HPV assay and comparison with those of single HPV infection
- Jinhee Kim, Moonsik Kim, Ji Young Park
- J Pathol Transl Med. 2022;56(5):289-293. Published online September 13, 2022
- DOI: https://doi.org/10.4132/jptm.2022.08.02
- 5,112 View
- 126 Download
- 9 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background
Human papillomavirus (HPV) infection is a major cause of cervical cancer and associated precursor lesions. Multiple HPV genotype infections have been reported. However, their clinicopathological characteristics still remain elusive.
Methods
For this study, 814 consecutive patients who had undergone colposcopy and HPV genotyping test using BD Onclarity HPV assay were retrospectively selected. Clinicopathological parameters of multiple HPV infections were compared with those of single HPV infection.
Results
Multiple HPV infections were found in 110 out of 814 cases (13.5%). Multiple HPV infections were associated with a significantly higher incidence of high-grade intraepithelial lesions (HSILs) compared with single HPV infection. Other high-risk HPV genotypes, in addition to HPV 16, were found more frequently in the multiple HPV infections group; these included HPV 51, 52, 33/58, 56/59/66, and 35/39/68. No specific coinfection pattern was not identified. Additionally, the number of HPV genotypes in multiple HPV infections was not associated with the progression to HSIL or squamous cell carcinoma.
Conclusions
Multiple HPV infections have distinct clinicopathological characteristics (compared with single HPV infection). As their biological behavior is uncertain, close and frequent follow-up is warranted. -
Citations
Citations to this article as recorded by- The Prevalence of Multi-Type Infections Among Human Papillomavirus Types in Korean Women
Jang Mook Kim, Hee Seung Song, Jieun Hwang, Jae Kyung Kim
Pathogens.2025; 14(4): 369. CrossRef - The cervical cancer related distribution, coinfection and risk of 15 HPV types in Baoan, Shenzhen, in 2017–2023
Rukai Li, Weiwei Meng, Yunhai Zuo, Yanli Xu, Shaonan Wu
Virology Journal.2024;[Epub] CrossRef - Molecular findings and virological assessment of bladder papillomavirus infection in cattle
Francesca De Falco, Anna Cutarelli, Francesca Luisa Fedele, Cornel Catoi, Sante Roperto
Veterinary Quarterly.2024; 44(1): 1. CrossRef - Patterns of single and multiple HPV infections in female: A systematic review and meta-analysis
Dan Zhou, Jing Xue, Yaqiong Sun, Liling Zhu, Ming Zhao, Meimei Cui, Min Zhang, Jingjing Jia, Limei Luo
Heliyon.2024; 10(17): e35736. CrossRef - Age distribution of patients with multiple High-Risk Human Papilloma Virus (HR-HPV) genotypes and HPV vaccine recommendations by age
Gülçin Çetin Uysal, Nil Tekin
Family Practice and Palliative Care.2024; 9(3): 80. CrossRef - Relative distribution of HPV genotypes in histological cervical samples and associated grade lesion in a women population over the last 16 years in Burgundy, France
Christelle Auvray, Serge Douvier, Odile Caritey, Jean-Baptiste Bour, Catherine Manoha
Frontiers in Medicine.2023;[Epub] CrossRef - Epidemiologic characteristics of high-risk HPV and the correlation between multiple infections and cervical lesions
Qinli Luo, Xianghua Zeng, Hanyi Luo, Ling Pan, Ying Huang, Haiyan Zhang, Na Han
BMC Infectious Diseases.2023;[Epub] CrossRef
- The Prevalence of Multi-Type Infections Among Human Papillomavirus Types in Korean Women
- Evaluation of human papillomavirus (HPV) prediction using the International Endocervical Adenocarcinoma Criteria and Classification system, compared to p16 immunohistochemistry and HPV RNA in-situ hybridization
- Hezhen Ren, Jennifer Pors, Christine Chow, Monica Ta, Simona Stolnicu, Robert Soslow, David Huntsman, Lynn Hoang
- J Pathol Transl Med. 2020;54(6):480-488. Published online August 31, 2020
- DOI: https://doi.org/10.4132/jptm.2020.07.18
- 5,773 View
- 168 Download
- 8 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The International Endocervical Adenocarcinoma Criteria and Classification (IECC) separated endocervical adenocarcinomas into human papillomavirus (HPV) associated (HPVA) and non–HPV-associated (NHPVA) categories by morphology alone. Our primary objective was to assess the accuracy of HPV prediction by the IECC system compared to p16 immunohistochemistry and HPV RNA in-situ hybridization (RISH). Our secondary goal was to directly compare p16 and HPV RISH concordance.
Methods
Cases were classified by IECC and stained for p16 and HPV RISH on tissue microarray, with discordant p16/HPV RISH cases re-stained on whole tissue sections. Remaining discordant cases (p16/HPV, IECC/p16, IECC/HPV discordances) were re-reviewed by the original pathologists (n = 3) and external expert pathologists (n = 2) blinded to the p16 and HPV RISH results. Final IECC diagnosis was assigned upon independent agreement between all reviewers.
Results
One hundred and eleven endocervical adenocarcinomas were classified originally into 94 HPVA and 17 NHPVA cases. p16 and HPV RISH was concordant in 108/111 cases (97%) independent of the IECC. HPV RISH and p16 was concordant with IECC in 103/111 (93%) and 106/111 (95%), respectively. After expert review, concordance improved to 107/111 (96%) for HPV RISH. After review of the eight discordant cases, one remained as HPVA, four were reclassified to NHPVA from HPVA, two were unclassifiable, and one possibly represented a mixed usual and gastric-type adenocarcinoma.
Conclusions
p16 and HPV RISH have excellent concordance in endocervical adenocarcinomas, and IECC can predict HPV status in most cases. Focal apical mitoses and apoptotic debris on original review led to the misclassification of several NHPVA as HPVA. -
Citations
Citations to this article as recorded by- Joint detection of multiple HPV-testing technologies and evaluation of clinicopathological characteristics discriminate between HPV-independent and low-copy HPV-associated cervical squamous cell carcinoma (CSCC) -an analysis of 3869 cases
Linghui Lu, Tianqi Liu, Shunni Wang, Jing Li, Feiran Zhang, Yan Ning, Yiqin Wang
Gynecologic Oncology.2023; 170: 59. CrossRef - Incidence and Clinicopathologic Characteristics of Human Papillomavirus–independent Invasive Squamous Cell Carcinomas of the Cervix
Simona Stolnicu, Douglas Allison, Aaron M. Praiss, Basile Tessier-Cloutier, Amir Momeni Boroujeni, Jessica Flynn, Alexia Iasonos, Rene Serrette, Lien Hoang, Andrei Patrichi, Cristina Terinte, Anna Pesci, Claudia Mateoiu, Ricardo R. Lastra, Takako Kiyokawa
American Journal of Surgical Pathology.2023; 47(12): 1376. CrossRef - Testing Algorithms for the Diagnosis of Malignant Glandular Tumors of the Uterine Cervix Histotyped per the International Endocervical Adenocarcinoma Criteria and Classification (IECC) System
Máire A. Duggan, Qiuli Duan, Ruth M. Pfeiffer, Mary Anne Brett, Sandra Lee, Mustapha Abubakar, Martin Köbel, Monica Rodriguez, Aylin Sar
Applied Immunohistochemistry & Molecular Morphology.2022; 30(2): 91. CrossRef - Local and Metastatic Relapses in a Young Woman with Papillary Squamous Cell Carcinoma of the Uterine Cervix
Ha Young Woo, Hyun-Soo Kim
Diagnostics.2022; 12(3): 599. CrossRef - Clinical correlation of lymphovascular invasion and Silva pattern of invasion in early-stage endocervical adenocarcinoma: proposed binary Silva classification system
Simona Stolnicu, Lien Hoang, Noorah Almadani, Louise De Brot, Glauco Baiocchi, Graziele Bovolim, Maria Jose Brito, Georgia Karpathiou, Antonio Ieni, Esther Guerra, Takako Kiyokawa, Pavel Dundr, Carlos Parra-Herran, Sofia Lérias, Ana Felix, Andres Roma, An
Pathology.2022; 54(5): 548. CrossRef - Reproducibility of Morphologic Parameters of the International Endocervical Adenocarcinoma Criteria and Classification System and Correlation With Clinicopathologic Parameters: A Multi-Institutional Study
Pinar Bulutay, Nihan Haberal, Özlem Özen, Özlem Erdem, Emine H. Zeren, İbrahim Kulac, Çagatay Taskiran, Dogan Vatansever, Ali Ayhan, Nilgün Kapucuoğlu
International Journal of Gynecological Pathology.2022; 41(5): 447. CrossRef - HPV-Negative Cervical Cancer: A Narrative Review
Francesca Arezzo, Gennaro Cormio, Vera Loizzi, Gerardo Cazzato, Viviana Cataldo, Claudio Lombardi, Giuseppe Ingravallo, Leonardo Resta, Ettore Cicinelli
Diagnostics.2021; 11(6): 952. CrossRef - International Endocervical Adenocarcinoma Criteria and Classification (IECC): An Independent Cohort With Clinical and Molecular Findings
Hezhen Ren, Noorah Almadani, Jennifer Pors, Samuel Leung, Julie Ho, Christine Chow, Monica Ta, Kay J. Park, Simona Stolnicu, Robert Soslow, David Huntsman, Blake C. Gilks, Lynn Hoang
International Journal of Gynecological Pathology.2021; 40(6): 533. CrossRef
- Joint detection of multiple HPV-testing technologies and evaluation of clinicopathological characteristics discriminate between HPV-independent and low-copy HPV-associated cervical squamous cell carcinoma (CSCC) -an analysis of 3869 cases
- Prevalence of high-risk human papillomavirus and its genotype distribution in head and neck squamous cell carcinomas
- Yuil Kim, Young-Hoon Joo, Min-Sik Kim, Youn Soo Lee
- J Pathol Transl Med. 2020;54(5):411-418. Published online July 21, 2020
- DOI: https://doi.org/10.4132/jptm.2020.06.22
- 8,406 View
- 181 Download
- 21 Web of Science
- 24 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
High-risk (HR) human papillomavirus (HPV) is found in a subset of head and neck (HN) squamous cell carcinomas (SCCs). For oropharyngeal SCCs, HR HPV positivity is known to be associated with good prognosis, and a separate staging system for HPV-associated carcinomas using p16 immunohistochemistry (IHC) as a surrogate test has been adopted in the 8th American Joint Committee on Cancer staging system. We examined the HR HPV status and the genotype distribution in five HN subsites.
Methods
Formalin-fixed paraffin-embedded tissue sections were used for p16 IHC and DNA extraction. HPV DNA detection and genotyping were done employing either a DNA chip-based or real-time polymerase chain reaction–based method.
Results
During 2011–2019, a total of 466 SCCs were tested for HPV DNA with 34.1% positivity for HR HPV. Among HN subsites, the oropharynx showed the highest HR HPV prevalence (149/205, 75.1%), followed by the sinonasal tract (3/14, 21.4%), larynx (5/43, 11.6%), hypopharynx (1/38, 2.6%), and oral cavity (1/166, 0.6%). The most common HPV genotype was HPV16 (84.3%) followed by HPV35 (6.9%) and HPV33 (4.4%). Compared with HR HPV status, the sensitivity and specificity of p16 IHC were 98.6% and 94.3% for the oropharynx, and 99.2% and 93.8% for the tonsil, respectively.
Conclusions
Using a Korean dataset, we confirmed that HR HPV is most frequently detected in oropharyngeal SCCs. p16 positivity showed a good concordance with HR HPV DNA for oropharyngeal and especially tonsillar carcinomas. The use of p16 IHC may further be extended to predict HR HPV positivity in sinonasal tract SCCs. -
Citations
Citations to this article as recorded by- Impact of histopathological parameters in prognosis of oral squamous cell carcinoma
R. P. Ekanayaka, W. M. Tilakaratne
Oral Diseases.2025; 31(5): 1420. CrossRef - Risk factors for cervical lymph node metastasis in oropharyngeal cancer and its impact on prognosis
Li Zhang, Zhilin Li, Jing Wang, Chen Wang, Shuxin Wen
Brazilian Journal of Otorhinolaryngology.2025; 91(2): 101520. CrossRef - Co-infection of human papillomavirus genotypes and Epstein-Barr virus in tumors of the oral cavity and oropharynx: a retrospective study in Northeastern Mexico
Gerardo del Carmen Palacios-Saucedo, Jose Manuel Vazquez-Guillen, Alondra Yamileth Alanis-Valdez, Leticia Lizeth Valdez-Treviño, Luis Roberto Galindo-Mendez, Angel Zavala-Pompa, Lydia Guadalupe Rivera-Morales, Ana Carolina Martinez-Torres, Roberto Lopez-V
IJID Regions.2025; 14: 100555. CrossRef - Rates of p16 and p53 expression in head and neck cutaneous squamous cell carcinoma vary according to human papillomavirus status
Rachid Ait Addi
World Journal of Clinical Cases.2025;[Epub] CrossRef - The epidemiological trends and survival of HPV-related oropharyngeal cancer other than tonsils and base of tongue − a systematic review and meta-analysis
Anas Mohammad Al Fadel, Kathrine Kronberg Jakobsen, Lasse Holmgaard Jensen, Amanda-Louise Fenger Carlander, Christian Grønhøj, Christian von Buchwald
Oral Oncology.2025; 165: 107311. CrossRef - Characteristics of human papillomavirus infection among oropharyngeal cancer patients: A systematic review and meta-analysis
Meimei Cui, Jinling Cheng, Huijuan Cheng, Ming Zhao, Dan Zhou, Min Zhang, Jingjing Jia, Limei Luo
Archives of Oral Biology.2024; 157: 105830. CrossRef - Longitudinal Screening for Oral High-Risk Non-HPV16 and Non-HPV18 Strains of Human Papillomavirus Reveals Increasing Prevalence among Adult and Pediatric Biorepository Samples: A Pilot Study
Jordan Jacobs, Eugene Chon, Karl Kingsley
Vaccines.2024; 12(8): 895. CrossRef - Position Statement about Gender-Neutral HPV Vaccination in Korea
Kyung-Jin Min, Yung-Taek Ouh, Sangrak Bae, Yong-Bae Ji, Jae-Kwan Lee, Jae-Weon Kim, Kwang-Jae Cho, Dong-Hun Im
Vaccines.2024; 12(10): 1110. CrossRef - Prevalence of human papilloma virus in head and neck mucous squamous cell carcinoma and genotypes by location: an observational study
Emilie Uhlrich, Jerzy Klijanienko, Joey Martin, Emmanuelle Jeannot, Anne Vincent-Salomon, Paul Freneaux, Christophe Le Tourneau, Olivier Choussy, Antoine Dubray-Vautrin
European Journal of Cancer Prevention.2024;[Epub] CrossRef - High-risk HPV Does not Appear to be an Important Risk Factor for Sinonasal Carcinomas in Turkish Population: A Tertiary Center Experience
Evsen Apaydin Arikan, Levent Aydemir, Murat Ulusan, Dilek Yilmazbayhan, Yasemin Ozluk
International Journal of Surgical Pathology.2023; 31(2): 124. CrossRef - Practical Application of Circulating Tumor-Related DNA of Human Papillomavirus in Liquid Biopsy to Evaluate the Molecular Response in Patients with Oropharyngeal Cancer
Agnieszka M. Mazurek, Tomasz W. Rutkowski
Cancers.2023; 15(4): 1047. CrossRef - The Prevalence of HPV in Oral Cavity Squamous Cell Carcinoma
Seyed Keybud Katirachi, Mathias Peter Grønlund, Kathrine Kronberg Jakobsen, Christian Grønhøj, Christian von Buchwald
Viruses.2023; 15(2): 451. CrossRef - The Protective Role of Cranberries and Blueberries in Oral Cancer
César Esquivel-Chirino, Mario Augusto Bolaños-Carrillo, Daniela Carmona-Ruiz, Ambar Lopéz-Macay, Fernando Hernández-Sánchez, Delina Montés-Sánchez, Montserrat Escuadra-Landeros, Luis Alberto Gaitán-Cepeda, Silvia Maldonado-Frías, Beatriz Raquel Yáñez-Ocam
Plants.2023; 12(12): 2330. CrossRef - Unusual cases of sinonasal malignancies: a letter to the editor on HPV-positive sinonasal squamous cell carcinomas
Benedicte Bitsch Lauritzen, Sannia Sjöstedt, Jakob Myllerup Jensen, Katalin Kiss, Christian von Buchwald
Acta Oncologica.2023; 62(6): 608. CrossRef - Prevalence of human Papillomavirus associated oropharyngeal and oral squamous cell carcinoma in Asian countries: A systematic review and large-scale meta-analysis
Yy Jean Tan, Ken Wong Siong Hou, Galvin Sim Siang Lin, Jasmine Lim Suk Wun, Wan Nor Amira Wan Ahmad Abdul Nasir, Lynn Wei Linn Ko
Acta Marisiensis - Seria Medica.2023; 69(2): 77. CrossRef - Top 100 most cited articles on human papillomavirus-induced head and neck squamous cell carcinoma: A bibliographic review
Rahul Mohandas, Subhashree Mohapatra, Mary Oshin, ShubhangiSambhaji Hajare
Journal of International Oral Health.2023; 15(3): 219. CrossRef - Intracellular Toll-Like Receptors Modulate Adaptive Immune Responses in Head and Neck Cancer
Sangeetha K. Nayanar, Deepak Roshan V.G., Shruthi Surendran, Göran Kjeller, Bengt Hasséus, Daniel Giglio
Viral Immunology.2023; 36(10): 659. CrossRef - Positive Rate of Human Papillomavirus and Its Trend in Head and Neck Cancer in South Korea
Hyun Woong Jun, Yong Bae Ji, Chang Myeon Song, Jae Kyung Myung, Hae Jin Park, Kyung Tae
Frontiers in Surgery.2022;[Epub] CrossRef - Transcriptionally active HPV in OPMD and OSCC: A systematic review following the CAP/ASCO guidelines
Laura Borges Kirschnick, Lauren Frenzel Schuch, Maria Eduarda Pérez‐de‐Oliveira, Ana Gabriela Costa Normando, Bruno Augusto Linhares Almeida Mariz, Eliete Neves Silva Guerra, Felipe Martins Silveira, Ana Carolina Uchoa Vasconcelos, Luciana Estevam Simonat
Oral Diseases.2022; 28(8): 2309. CrossRef - Effect of National Oral Health Screening Program on the Risk of Head and Neck Cancer: A Korean National Population-Based
Chan Woo Wee, Hyo-Jung Lee, Jae-Ryun Lee, Hyejin Lee, Min-Jeong Kwoen, Woo-Jin Jeong, Keun-Yong Eom
Cancer Research and Treatment.2022; 54(3): 709. CrossRef - Expression of p16, p53, and TLR9 in HPV-Associated Head and Neck Squamous Cell Carcinoma: Clinicopathological Correlations and Potential Prognostic Significance
Shu Wang, Xibing Zhuang, Caixia Gao, Tiankui Qiao
OncoTargets and Therapy.2021; Volume 14: 867. CrossRef - The Role of Human Papilloma Virus in Dictating Outcomes in Head and Neck Squamous Cell Carcinoma
Shane Brennan, Anne-Marie Baird, Esther O’Regan, Orla Sheils
Frontiers in Molecular Biosciences.2021;[Epub] CrossRef - A Contemporary Systematic Review on Repartition of HPV-Positivity in Oropharyngeal Cancer Worldwide
Amanda F. Carlander, Kathrine K. Jakobsen, Simone K. Bendtsen, Martin Garset-Zamani, Charlotte D. Lynggaard, Jakob Schmidt Jensen, Christian Grønhøj, Christian von Buchwald
Viruses.2021; 13(7): 1326. CrossRef - The Prevalence of High- and Low-Risk Types of HPV in Patients with Squamous Cell Carcinoma of the Head and Neck, Patients with Chronic Tonsillitis, and Healthy Individuals Living in Poland
Joanna Katarzyna Strzelczyk, Krzysztof Biernacki, Jadwiga Gaździcka, Elżbieta Chełmecka, Katarzyna Miśkiewicz-Orczyk, Natalia Zięba, Janusz Strzelczyk, Maciej Misiołek
Diagnostics.2021; 11(12): 2180. CrossRef
- Impact of histopathological parameters in prognosis of oral squamous cell carcinoma
- Comparison of papanicolaou smear and human papillomavirus (HPV) test as cervical screening tools: can we rely on HPV test alone as a screening method? An 11-year retrospective experience at a single institution
- Myunghee Kang, Seung Yeon Ha, Hyun Yee Cho, Dong Hae Chung, Na Rae Kim, Jungsuk An, Sangho Lee, Jae Yeon Seok, Juhyeon Jeong
- J Pathol Transl Med. 2020;54(1):112-118. Published online January 15, 2020
- DOI: https://doi.org/10.4132/jptm.2019.11.29
- 10,471 View
- 251 Download
- 19 Web of Science
- 20 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
The decrease in incidence of cervical dysplasia and carcinoma has not been as dramatic as expected with the development of improved research tools and test methods. The human papillomavirus (HPV) test alone has been suggested for screening in some countries. The National Cancer Screening Project in Korea has applied Papanicolaou smears (Pap smears) as the screening method for cervical dysplasia and carcinoma. We evaluated the value of Pap smear and HPV testing as diagnostic screening tools in a single institution.
Methods
Patients co-tested with HPV test and Pap smear simultaneously or within one month of each other were included in this study. Patients with only punch biopsy results were excluded because of sampling errors. A total of 999 cases were included, and the collected reports encompassed results of smear cytology, HPV subtypes, and histologic examinations.
Results
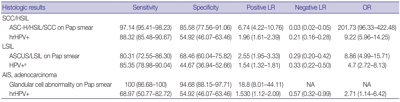
Sensitivity and specificity of detecting high-grade squamous intraepithelial lesion (HSIL) and squamous cell carcinoma (SCC) were higher for Pap smears than for HPV tests (sensitivity, 97.14%; specificity, 85.58% for Pap smears; sensitivity, 88.32%; specificity, 54.92% for HPV tests). HPV tests and Pap smears did not differ greatly in detection of low-grade squamous intraepithelial lesion (85.35% for HPV test, 80.31% for Pap smears). When atypical glandular cells were noted on Pap smears, the likelihood for histologic diagnosis of adenocarcinoma following Pap smear was higher than that of high-risk HPV test results (18.8 and 1.53, respectively).
Conclusions
Pap smears were more useful than HPV tests in the diagnosis of HSIL, SCC, and glandular lesions. -
Citations
Citations to this article as recorded by- Detection of cervical precancerous lesions and cancer by small-scale RT-qPCR analysis of oppositely deregulated mRNAs pairs in cytological smears
Anastasia A. Artyukh, Mikhail K. Ivanov, Sergei E. Titov, Victoria V. Dzyubenko, Sergey E. Krasilnikov, Anastasia O. Shumeikina, Nikita A. Afanasev, Anastasia V. Malek, Sergei A. Glushkov, Eduard F. Agletdinov
Frontiers in Oncology.2025;[Epub] CrossRef - High burden of abnormal cervical smears in South African primary health care: health programmes implications
Olufemi B Omole, Joel M Francis, John M Musonda, Pumla P Sodo, Elizabeth Reji, Nyundu S J Phukuta, Honey L M Mabuza, Joyce S Musonda, Jimmy Akii, John V Ndimande, Olalekan A Ayo-Yusuf
Health Promotion International.2025;[Epub] CrossRef - Bibliometric analysis: a study of the microenvironment in cervical cancer (2000-2024)
Yun-Tao Zhang, Yan-Ni Wei, Chen-Chen Liu, Mai-Qing Yang
Frontiers in Oncology.2025;[Epub] CrossRef - Challenges in the diagmosis of cervical pathologies
D. Y. Chernov, O. A. Tikhonovskaya, S. V. Logvinov, I. A. Petrov, Y. S. Yuriev, A. A. Zhdankina, A. V. Gerasimov, I. V. Zingalyuk, G. A. Mikheenko
Bulletin of Siberian Medicine.2024; 22(4): 201. CrossRef - “Barriers and Advantages of Self-Sampling Tests, for HPV Diagnosis: A Qualitative Field Experience Before Implementation in a Rural Community in Ecuador”
Bernardo Vega-Crespo, Vivian Alejandra Neira, Ruth Maldonado - Rengel, Diana López, Dayanara Delgado-López, Gabriela Guerra Astudillo, Veronique Verhoeven
International Journal of Women's Health.2024; Volume 16: 947. CrossRef - Cervical Human Papillomavirus Testing
Carol N. Rizkalla, Eric C. Huang
Surgical Pathology Clinics.2024; 17(3): 431. CrossRef - Segmentation of Overlapping Cells in Cervical Cytology Images: A Survey
E Chen, Hua-Nong Ting, Joon Huang Chuah, Jun Zhao
IEEE Access.2024; 12: 114170. CrossRef - Knowledge and awareness regarding pap test and HPV typing for cervical cancer screening in Edo North, Nigeria
Amina Momodu, Johnsolomon Eghosa Ohenhen, Godfrey Innocent Iyare, Musa Abidemi Muhibi, Godwin Avwioro
Discover Public Health.2024;[Epub] CrossRef - Colposcopy Value in Young Child-bearing Women: Is New Recommendations Necessary?
Fahimeh Sabet, Avishan Aminizad, Fariba Behnamfar, Tajossadat Allameh, Seyedeh Ghazal Shahrokh, Rostami Koushan, Amirmohammad Taravati, Leila Mousavi Seresht
Advanced Biomedical Research.2024;[Epub] CrossRef - Selection of endogenous control and identification of significant microRNA deregulations in cervical cancer
T. Stverakova, I. Baranova, P. Mikyskova, B. Gajdosova, H. Vosmikova, J. Laco, V. Palicka, H. Parova
Frontiers in Oncology.2023;[Epub] CrossRef - Cytology Versus Molecular Diagnosis of HPV for Cervical Cancer Screening. Comparison of the Diagnostic Properties of Four Tests in a Rural Community of Cuenca Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, Rocío Murillo, Cristina Ochoa Avilés
ESPOCH Congresses: The Ecuadorian Journal of S.T.E.A.M..2023; 3(1): 139. CrossRef - Attitudes towards prevention of cervical cancer and early diagnosis among female academicians
Nurhan Doğan, Gamze Fışkın
Journal of Obstetrics and Gynaecology Research.2022; 48(6): 1433. CrossRef - Role of Self-Sampling for Cervical Cancer Screening: Diagnostic Test Properties of Three Tests for the Diagnosis of HPV in Rural Communities of Cuenca, Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, José Ortíz Segarra, Ruth Maldonado Rengel, Diana López, María Paz Orellana, Andrea Gómez, María José Vicuña, Jorge Mejía, Ina Benoy, Tesifón Parrón Carreño, Veronique Verhoeven
International Journal of Environmental Research and Public Health.2022; 19(8): 4619. CrossRef - Utility of Scoring System for Screening and Early Warning of Cervical Cancer Based on Big Data Analysis
Dan Hou, Binjie Yang, Yangdan Li, Ming Sun
Frontiers in Public Health.2022;[Epub] CrossRef - Evaluation of Urine and Vaginal Self-Sampling versus Clinician-Based Sampling for Cervical Cancer Screening: A Field Comparison of the Acceptability of Three Sampling Tests in a Rural Community of Cuenca, Ecuador
Bernardo Vega Crespo, Vivian Alejandra Neira, José Ortíz S, Ruth Maldonado-Rengel, Diana López, Andrea Gómez, María José Vicuña, Jorge Mejía, Ina Benoy, Tesifón Parrón Carreño, Veronique Verhoeven
Healthcare.2022; 10(9): 1614. CrossRef - Diagnostic distribution and pitfalls of glandular abnormalities in cervical cytology: a 25-year single-center study
Jung-A Sung, Ilias P. Nikas, Haeryoung Kim, Han Suk Ryu, Cheol Lee
Journal of Pathology and Translational Medicine.2022; 56(6): 354. CrossRef - Primary screening of cervical cancer by Pap smear in women of reproductive age group
Ruchi Mishra, Dakshina Bisht, Manisha Gupta
Journal of Family Medicine and Primary Care.2022; 11(9): 5327. CrossRef - Comparison of Learning Transfer Using Simulation Problem-Based Learning and Demonstration: An Application of Papanicolaou Smear Nursing Education
Jeongim Lee, Hae Kyoung Son
International Journal of Environmental Research and Public Health.2021; 18(4): 1765. CrossRef - Investigating host-virus interaction mechanism and phylogenetic analysis of viral proteins involved in the pathogenesis
Ahmad Abu Turab Naqvi, Farah Anjum, Alaa Shafie, Sufian Badar, Abdelbaset Mohamed Elasbali, Dharmendra Kumar Yadav, Md. Imtaiyaz Hassan, Timir Tripathi
PLOS ONE.2021; 16(12): e0261497. CrossRef - Utility of Human Papillomavirus Testing for Cervical Cancer Screening in Korea
Mee-seon Kim, Eun Hee Lee, Moon-il Park, Jae Seok Lee, Kisu Kim, Mee Sook Roh, Hyoun Wook Lee
International Journal of Environmental Research and Public Health.2020; 17(5): 1726. CrossRef
- Detection of cervical precancerous lesions and cancer by small-scale RT-qPCR analysis of oppositely deregulated mRNAs pairs in cytological smears
- Current Status of and Perspectives on Cervical Cancer Screening in Korea
- Sung-Chul Lim, Chong Woo Yoo
- J Pathol Transl Med. 2019;53(4):210-216. Published online May 16, 2019
- DOI: https://doi.org/10.4132/jptm.2019.04.11
- 9,894 View
- 269 Download
- 8 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF - Since the introduction of the Papanicolaou (Pap) smear system in 1943, cervicovaginal cytology has been used as a standard screening test for cervical cancer. The dissemination of this test contributed to reductions of the incidence and mortality of cervical cancer worldwide. In Korea, regular health check-ups for industrial workers and their family members were introduced in 1988 and were performed as part of the National Cancer Screening Program in 1999. As a result, the incidence of cervical cancer in Korea has been steadily decreasing. However, about 800 cases of cervical cancer-related deaths are reported each year due to false-negative test results. Hence, new screening methods have been proposed. Liquid-based cytology (LBC) was introduced in 1996 to overcome the limitations of conventional Pap smears. Since then, other LBC methods have been developed and utilized, including the human papilloma virus test—a method with higher sensitivity that requires fewer screenings. In this study, we review current issues and future perspectives related to cervical cancer screening in Korea.
-
Citations
Citations to this article as recorded by- A questionnaire study on disparity of cervical cancer prevention programs in Asia‐Oceania
Ka Yu Tse, Kimio Ushijima, Ai Ling Tan, Perapong Intasorn, Jitendra Pariyar, Chih‐Long Chang, Efren J. Domingo, Hiralal Konar, Suresh Kumarasamy, Brahmana Askandar Tjokroprawiro, Sarikapan Wilailak
Journal of Obstetrics and Gynaecology Research.2023; 49(4): 1230. CrossRef - Current state of cytopathology residency training: a Korean national survey of pathologists
Uiju Cho, Tae Jung Kim, Wan Seop Kim, Kyo Young Lee, Hye Kyoung Yoon, Hyun Joo Choi
Journal of Pathology and Translational Medicine.2023; 57(2): 95. CrossRef - Meeting the challenges of cervical cancer screening and HPV vaccination in the UK
Roxanne Westwood, Joanna Lavery
Primary Health Care.2022; 32(01): 22. CrossRef - Local and Metastatic Relapses in a Young Woman with Papillary Squamous Cell Carcinoma of the Uterine Cervix
Ha Young Woo, Hyun-Soo Kim
Diagnostics.2022; 12(3): 599. CrossRef - Serum Human Epididymis Protein 4 as a Prognostic Marker in Cervical Cancer
Woo Yeon Hwang, Dong Hoon Suh, Kidong Kim, Yong Beom Kim, Jae Hong No
Cancer Control.2022;[Epub] CrossRef - HPV detection and/or cytological diagnostics
Sanja Milenković
Glasnik javnog zdravlja.2022; 96(3): 313. CrossRef - Clinical management of abnormal Pap tests: differences between US and Korean guidelines
Seyeon Won, Mi Kyoung Kim, Seok Ju Seong
Journal of Pathology and Translational Medicine.2020; 54(3): 213. CrossRef - Current status of cytopathology practices in Korea: annual report on the Continuous Quality Improvement program of the Korean Society for Cytopathology for 2018
Yosep Chong, Haeyoen Jung, Jung-Soo Pyo, Soon Won Hong, Hoon Kyu Oh
Journal of Pathology and Translational Medicine.2020; 54(4): 318. CrossRef - Cytomorphological Features of Hyperchromatic Crowded Groups in Liquid-Based Cervicovaginal Cytology: A Single Institutional Experience
Youngeun Lee, Cheol Lee, In Ae Park, Hyoung Jin An, Haeryoung Kim
Journal of Pathology and Translational Medicine.2019; 53(6): 393. CrossRef
- A questionnaire study on disparity of cervical cancer prevention programs in Asia‐Oceania
- Detection of Human Papillomavirus in Korean Breast Cancer Patients by Real-Time Polymerase Chain Reaction and Meta-Analysis of Human Papillomavirus and Breast Cancer
- Jinhyuk Choi, Chungyeul Kim, Hye Seung Lee, Yoo Jin Choi, Ha Yeon Kim, Jinhwan Lee, Hyeyoon Chang, Aeree Kim
- J Pathol Transl Med. 2016;50(6):442-450. Published online October 10, 2016
- DOI: https://doi.org/10.4132/jptm.2016.07.08
- 12,838 View
- 225 Download
- 15 Web of Science
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) is a well-established oncogenic virus of cervical, anogenital, and oropharyngeal cancer. Various subtypes of HPV have been detected in 0% to 60% of breast cancers. The roles of HPV in the carcinogenesis of breast cancer remain controversial. This study was performed to determine the prevalence of HPV-positive breast cancer in Korean patients and to evaluate the possibility of carcinogenic effect of HPV on breast.
Methods
Meta-analysis was performed in 22 case-control studies for HPV infection in breast cancer. A total of 123 breast cancers, nine intraductal papillomas and 13 nipple tissues of patients with proven cervical HPV infection were tested by real-time polymerase chain reaction to detect 28 subtypes of HPV. Breast cancers were composed of 106 formalin-fixed and paraffin embedded (FFPE) breast cancer samples and 17 touch imprint cytology samples of breast cancers.
Results
The overall odds ratio between breast cancer and HPV infection was 5.43 (95% confidence interval, 3.24 to 9.12) with I2 = 34.5% in meta-analysis of published studies with case-control setting and it was statistically significant. HPV was detected in 22 cases of breast cancers (17.9%) and two cases of intaductal papillomas (22.2%). However, these cases had weak positivity.
Conclusions
These results failed to serve as significant evidence to support the relationship between HPV and breast cancer. Further study with larger epidemiologic population is merited to determine the relationship between HPV and breast cancer. -
Citations
Citations to this article as recorded by- Advances in human papillomavirus detection for cervical cancer screening and diagnosis: challenges of conventional methods and opportunities for emergent tools
O. Fashedemi, Okoroike C. Ozoemena, Siwaphiwe Peteni, Aderemi B. Haruna, Leshweni J. Shai, Aicheng Chen, Frankie Rawson, Maggie E. Cruickshank, David Grant, Oluwafunmilola Ola, Kenneth I. Ozoemena
Analytical Methods.2025; 17(7): 1428. CrossRef - Bacterial-Viral Interactions in Human Orodigestive and Female Genital Tract Cancers: A Summary of Epidemiologic and Laboratory Evidence
Ikuko Kato, Jilei Zhang, Jun Sun
Cancers.2022; 14(2): 425. CrossRef - Breast cancer association with oncogenic papillomaviruses: papillomaviral DNA detection in breast cancer cells
G. M. Volgareva
Advances in Molecular Oncology.2022; 9(2): 10. CrossRef - Presence of Human Papillomavirus DNA in Malignant Neoplasia and Non-Malignant Breast Disease
Erika Maldonado-Rodríguez, Marisa Hernández-Barrales, Adrián Reyes-López, Susana Godina-González, Perla I. Gallegos-Flores, Edgar L. Esparza-Ibarra, Irma E. González-Curiel, Jesús Aguayo-Rojas, Adrián López-Saucedo, Gretel Mendoza-Almanza, Jorge L. Ayala-
Current Issues in Molecular Biology.2022; 44(8): 3648. CrossRef - Risk Role of Breast Cancer in Association with Human Papilloma Virus among Female Population in Taiwan: A Nationwide Population-Based Cohort Study
Chia-Hsin Liu, Chi-You Liao, Ming-Hsin Yeh, James Cheng-Chung Wei
Healthcare.2022; 10(11): 2235. CrossRef - HPV-Associated Breast Cancer: Myth or Fact?
Erik Kudela, Eva Kudelova, Erik Kozubík, Tomas Rokos, Terezia Pribulova, Veronika Holubekova, Kamil Biringer
Pathogens.2022; 11(12): 1510. CrossRef - Assessment of Human Papillomavirus Infection and Risk Factors in Egyptian Women With Breast Cancer
Nabila El-Sheikh, Nahla O Mousa, Amany M Tawfeik, Alaa M Saleh, Iman Elshikh, Mohamed Deyab, Faten Ragheb, Manar M Moneer, Ahmed Kawashti, Ahmed Osman, Mohamed Elrefaei
Breast Cancer: Basic and Clinical Research.2021;[Epub] CrossRef - Human Papillomavirus (HPV) Detection by Chromogenic In Situ Hybridization (CISH) and p16 Immunohistochemistry (IHC) in Breast Intraductal Papilloma and Breast Carcinoma
Hua Guo, Juan P. Idrovo, Jin Cao, Sudarshana Roychoudhury, Pooja Navale, Louis J. Auguste, Tawfiqul Bhuiya, Silvat Sheikh-Fayyaz
Clinical Breast Cancer.2021; 21(6): e638. CrossRef - Human Papillomavirus in Breast Carcinogenesis: A Passenger, a Cofactor, or a Causal Agent?
Rancés Blanco, Diego Carrillo-Beltrán, Juan P. Muñoz, Alejandro H. Corvalán, Gloria M. Calaf, Francisco Aguayo
Biology.2021; 10(8): 804. CrossRef - Systematic review and meta-analysis of the papillomavirus prevalence in breast cancer fresh tissues
Geilson Gomes de Oliveira, Ana Katherine Gonçalves, José Eleutério, Luiz Gonzaga Porto Pinheiro
Breast Disease.2021; 41(1): 123. CrossRef - Is human papillomavirus associated with breast cancer or papilloma presenting with pathologic nipple discharge?
Fatih Levent Balci, Cihan Uras, Sheldon Marc Feldman
Cancer Treatment and Research Communications.2019; 19: 100122. CrossRef - Is the HPV virus responsible for the development of breast cancer?
Erik Kudela, Marcela Nachajova, Jan Danko
The Breast Journal.2019; 25(5): 1053. CrossRef - Absence of Human Papillomavirus in Benign and Malignant Breast Tissue
Maryam Kazemi Aghdam, Seyed Alireza Nadji, Azadeh Alvandimanesh, Maliheh Khoddami, Yassaman Khademi
Iranian Journal of Pathology.2019; 14(4): 279. CrossRef - Oncogenic Viruses and Breast Cancer: Mouse Mammary Tumor Virus (MMTV), Bovine Leukemia Virus (BLV), Human Papilloma Virus (HPV), and Epstein–Barr Virus (EBV)
James S. Lawson, Brian Salmons, Wendy K. Glenn
Frontiers in Oncology.2018;[Epub] CrossRef - Viral infections and breast cancer – A current perspective
O.M. Gannon, A. Antonsson, I.C. Bennett, N.A. Saunders
Cancer Letters.2018; 420: 182. CrossRef - Prevalence of EBV, HPV and MMTV in Pakistani breast cancer patients: A possible etiological role of viruses in breast cancer
Wasifa Naushad, Orooj Surriya, Hajra Sadia
Infection, Genetics and Evolution.2017; 54: 230. CrossRef
- Advances in human papillomavirus detection for cervical cancer screening and diagnosis: challenges of conventional methods and opportunities for emergent tools
- Clinical Significance of an HPV DNA Chip Test with Emphasis on HPV-16 and/or HPV-18 Detection in Korean Gynecological Patients
- Min-Kyung Yeo, Ahwon Lee, Soo Young Hur, Jong Sup Park
- J Pathol Transl Med. 2016;50(4):294-299. Published online June 26, 2016
- DOI: https://doi.org/10.4132/jptm.2016.05.09
- 9,166 View
- 80 Download
- 3 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) is a major risk factor for cervical cancer.
Methods
We evaluated the clinical significance of the HPV DNA chip genotyping assay (MyHPV chip, Mygene Co.) compared with the Hybrid Capture 2 (HC2) chemiluminescent nucleic acid hybridization kit (Digene Corp.) in 867 patients.
Results
The concordance rate between the MyHPV chip and HC2 was 79.4% (kappa coefficient, κ = 0.55). The sensitivity and specificity of both HPV tests were very similar (approximately 85% and 50%, respectively). The addition of HPV result (either MyHPV chip or HC2) to cytology improved the sensitivity (95%, each) but reduced the specificity (approximately 30%, each) compared with the HPV test or cytology alone. Based on the MyHPV chip results, the odds ratio (OR) for ≥ high-grade squamous intraepithelial lesions (HSILs) was 9.9 in the HPV-16/18 (+) group and 3.7 in the non-16/18 high-risk (HR)-HPV (+) group. Based on the HC2 results, the OR for ≥ HSILs was 5.9 in the HR-HPV (+) group. When considering only patients with cytological diagnoses of “negative for intraepithelial lesion or malignancy” and “atypical squamous cell or atypical glandular cell,” based on the MyHPV chip results, the ORs for ≥ HSILs were 6.8 and 11.7, respectively, in the HPV-16/18 (+) group.
Conclusions
The sensitivity and specificity of the MyHPV chip test are similar to the HC2. Detecting HPV-16/18 with an HPV DNA chip test, which is commonly used in many Asian countries, is useful in assessing the risk of high-grade cervical lesions. -
Citations
Citations to this article as recorded by- Human papilloma virus identification in ocular surface squamous neoplasia by p16 immunohistochemistry and DNA chip test
Tina Shrestha, Won Choi, Ga Eon Kim, Jee Myung Yang, Kyung Chul Yoon
Medicine.2019; 98(2): e13944. CrossRef - Comparison of the PANArray HPV Genotyping Chip Test with the Cobas 4800 HPV and Hybrid Capture 2 Tests for Detection of HPV in ASCUS Women
Eun Young Ki, Yoon Kyung Lee, Ahwon Lee, Jong Sup Park
Yonsei Medical Journal.2018; 59(5): 662. CrossRef
- Human papilloma virus identification in ocular surface squamous neoplasia by p16 immunohistochemistry and DNA chip test
- Comparison of Analytical and Clinical Performance of HPV 9G DNA Chip, PANArray HPV Genotyping Chip, and Hybrid-Capture II Assay in Cervicovaginal Swabs
- Ho Young Jung, Hye Seung Han, Hyo Bin Kim, Seo Young Oh, Sun-Joo Lee, Wook Youn Kim
- J Pathol Transl Med. 2016;50(2):138-146. Published online January 13, 2016
- DOI: https://doi.org/10.4132/jptm.2015.10.21
- 8,975 View
- 68 Download
- 4 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF - Background
Human papillomavirus (HPV) infection can be detected by using several molecular methods, including Hybrid-Capture II (HC2) assay and variable HPV DNA chip tests, although each method has different sensitivities and specificities. Methods: We performed HPV 9G DNA Chip (9G) and PANArray HPV Genotyping Chip (PANArray) tests on 118 cervicovaginal swabs and compared the results with HC2, cytology, histology, and direct sequencing results. Results: The overall and high-risk HPV (HR-HPV) positivity rates were 62.7% and 44.9% using 9G, and 61.0% and 30.5% using PANArray, respectively. The positivity rates for HR-HPV with these two chips were significantly lower than 55.1% when HC2 was used. The sensitivity of overall HPV positivity in detecting histologically confirmed low-grade cervical squamous intraepithelial lesions or higher was 88.7% for all three tests. The specificity was 58.5% for 9G and 61.5% for PANArray, which was significantly lower than the 72.3% for HC2. With the HR-HPV+ genotype threshold, the sensitivity decreased to 75.5% for 9G and 52.8% for PANArray, which was significantly lower than the 88.7% for HC2. Comparison of the two chips showed concordant results in 55.1% of the samples, compatible results in 16.9%, and discordant results in 28.0%, exhibiting poor agreement in detecting certain HPV genotypes. Compared with direct sequencing, 9G yielded no discordant results, whereas PANArray yielded 31 discordant results (26.7%). Conclusions: Compared with HC2, the HPV genotyping tests showed lower sensitivity in histologic correlation. When the two chips were compared, the 9G was more sensitive and accurate for detecting HR-HPV than the PANArray. -
Citations
Citations to this article as recorded by- Concordance of Anyplex™ II HPV HR assays with reference HPV assays in cervical cancer screening: Systematic review
Habtamu Biazin
Journal of Virological Methods.2022; 301: 114435. CrossRef - The clinical performance of human papillomavirus genotyping using PANArray HPV chip: Comparison to ThinPrep cytology alone and co-testing
Jiyoung Kim, Sun-Young Jun, Lee-So Maeng
Pathology - Research and Practice.2020; 216(9): 153121. CrossRef - Analytic performance of PANArray HPV and HPV 9G DNA chip tests for genotyping of high-risk human papillomavirus in cervical ThinPrep PreservCyt samples
Jiyoung Kim, Sun-Young Jun, Magdalena Grce
PLOS ONE.2019; 14(10): e0224483. CrossRef
- Concordance of Anyplex™ II HPV HR assays with reference HPV assays in cervical cancer screening: Systematic review
- Uncommon and Rare Human Papillomavirus Genotypes Relating to Cervical Carcinomas
- Na Rae Kim, Myunghee Kang, Soon Pyo Lee, Hyunchul Kim, Jungsuk An, Dong Hae Chung, Seung Yeon Ha, Hyun Yee Cho
- Korean J Pathol. 2014;48(1):43-49. Published online February 25, 2014
- DOI: https://doi.org/10.4132/KoreanJPathol.2014.48.1.43
- 8,330 View
- 53 Download
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Human papillomavirus (HPV) is an oncogenic virus in cervical cancer and most invasive carcinomas (ICs) are caused by HPV16 and 18. However, the roles and contributions of other uncommon and rare genotypes remain uncertain.
Methods HPV genotypes were retrospectively assessed using an HPV DNA chip that can specify up to 32 HPV genotypes. We arbitrarily regarded genotypes accounting for less than 6% of the total as uncommon and rare genotypes.
Results A total of 3,164 HPV-positive cases were enrolled. In groups 2A, 2B, 3, and unclassified HPV genotypes, 2.4% of cases with uncommon HPV genotypes (68, 26, 34, 53, 66, 69, 70, 73, 40, 42, 43, 44, 54, 55, 61, 62, 6, and 11) showed high grade squamous intraepithelial lesions and ICs. There were no HPV32- and 57-infected cases.
Conclusions We found that the uncommon and rare HPV genotypes may provide incremental etiologic contributions in cervical carcinogenesis, especially HPV68, 70, and 53. Further studies on these uncommon and rare HPV genotypes will be of importance in establishing the significance of genotypes in different regions, especially in planning a strategy for further vaccine development as well as follow-up on the effectiveness of the currently used vaccines.
-
Citations
Citations to this article as recorded by- High-risk human papillomavirus diversity among indigenous women of western Botswana with normal cervical cytology and dysplasia
Patricia S. Rantshabeng, Billy M. Tsima, Andrew K. Ndlovu, Keneilwe Motlhatlhedi, Kirthana Sharma, Carol B. Masole, Natasha O. Moraka, Kesego Motsumi, Angela K. T. Maoto-Mokote, Alemayehu B. Eshetu, Leabaneng Tawe, Tendani Gaolathe, Sikhulile Moyo, Lynnet
BMC Infectious Diseases.2024;[Epub] CrossRef - Human Papillomavirus (HPV69/HPV73) Coinfection associated with Simultaneous Squamous Cell Carcinoma of the Anus and Presumed Lung Metastasis
Stephanie Shea, Marina Muñoz, Stephen C. Ward, Mary B. Beasley, Melissa R Gitman, Michael D Nowak, Jane Houldsworth, Emilia Mia Sordillo, Juan David Ramirez, Alberto E. Paniz Mondolfi
Viruses.2020; 12(3): 349. CrossRef - Human Papillomavirus Selected Properties and Related Cervical Cancer Prevention Issues
Saule Balmagambetova, Andrea Tinelli, Ospan A. Mynbaev, Arip Koyshybaev, Olzhas Urazayev, Nurgul Kereyeva, Elnara Ismagulova
Current Pharmaceutical Design.2020; 26(18): 2073. CrossRef - Periungual Bowen's disease with a narrow longitudinal melanonychia mimicking periungual warts
Taiyo HITAKA, Michiko HASEGAWA, Akira SHIMIZU, Yuko KURIYAMA, Atsushi TAMURA
Skin Cancer.2019; 33(3): 211. CrossRef - Detection of HPV RNA molecules in stratified mucin-producing intraepithelial lesion (SMILE) with concurrent cervical intraepithelial lesion: a case report
Shiho Fukui, Kazunori Nagasaka, Naoko Iimura, Ranka Kanda, Takayuki Ichinose, Takeru Sugihara, Haruko Hiraike, Shunsuke Nakagawa, Yuko Sasajima, Takuya Ayabe
Virology Journal.2019;[Epub] CrossRef - Pitfalls of commercially available HPV tests in HPV68a detection
Hana Jaworek, Katerina Kubanova, Vladimira Koudelakova, Rastislav Slavkovsky, Jiri Drabek, Marian Hajduch, Craig Meyers
PLOS ONE.2019; 14(8): e0220373. CrossRef - Overall accuracy of cervical cytology and clinicopathological significance of LSIL cells in ASC‐H cytology
S. H. Kim, J. M. Lee, H. G. Yun, U. S. Park, S. U. Hwang, J.‐S. Pyo, J. H. Sohn
Cytopathology.2017; 28(1): 16. CrossRef - Human papillomavirus genotyping by Linear Array and Next-Generation Sequencing in cervical samples from Western Mexico
María Guadalupe Flores-Miramontes, Luis Alberto Torres-Reyes, Liliana Alvarado-Ruíz, Salvador Angel Romero-Martínez, Verenice Ramírez-Rodríguez, Luz María Adriana Balderas-Peña, Verónica Vallejo-Ruíz, Patricia Piña-Sánchez, Elva Irene Cortés-Gutiérrez, Lu
Virology Journal.2015;[Epub] CrossRef - Impact of human papillomavirus coinfections on the risk of high-grade squamous intraepithelial lesion and cervical cancer
Adela Carrillo-García, Sergio Ponce-de-León-Rosales, David Cantú-de-León, Verónica Fragoso-Ontiveros, Imelda Martínez-Ramírez, Asunción Orozco-Colín, Alejandro Mohar, Marcela Lizano
Gynecologic Oncology.2014; 134(3): 534. CrossRef - Human papillomavirus 66‐associated subungual squamous cell carcinoma
Jin Hee Kang, Hwa young Ahn, Miri Kim, Shin Taek Oh, Baik Kee Cho, Hyun Jeong Park
The Journal of Dermatology.2014; 41(12): 1119. CrossRef
- High-risk human papillomavirus diversity among indigenous women of western Botswana with normal cervical cytology and dysplasia
- Cytological Evaluation and REBA HPV-ID HPV Testing of Newly Developed Liquid-Based Cytology, EASYPREP: Comparison with SurePath
- Youn Soo Lee, Gyungyub Gong, Jin Hee Sohn, Ki Sung Ryu, Jung Hun Lee, Shin Kwang Khang, Kyung-Ja Cho, Yong-Man Kim, Chang Suk Kang
- Korean J Pathol. 2013;47(3):265-274. Published online June 25, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.3.265
- 10,761 View
- 94 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF Background The objective of this study was to evaluate a newly-developed EASYPREP liquid-based cytology method in cervicovaginal specimens and compare it with SurePath.
Methods Cervicovaginal specimens were prospectively collected from 1,000 patients with EASYPREP and SurePath. The specimens were first collected by brushing for SurePath and second for EASYPREP. The specimens of both methods were diagnosed according to the Bethesda System. Additionally, we performed to REBA HPV-ID genotyping and sequencing analysis for human papillomavirus (HPV) on 249 specimens.
Results EASYPREP and SurePath showed even distribution of cells and were equal in cellularity and staining quality. The diagnostic agreement between the two methods was 96.5%. Based on the standard of SurePath, the sensitivity, specificity, positive predictive value, and negative predictive value of EASYPREP were 90.7%, 99.2%, 94.8%, and 98.5%, respectively. The positivity of REBA HPV-ID was 49.4% and 95.1% in normal and abnormal cytological samples, respectively. The result of REBA HPV-ID had high concordance with sequencing analysis.
Conclusions EASYPREP provided comparable results to SurePath in the diagnosis and staining quality of cytology examinations and in HPV testing with REBA HPV-ID. EASYPREP could be another LBC method choice for the cervicovaginal specimens. Additionally, REBA HPV-ID may be a useful method for HPV genotyping.
-
Citations
Citations to this article as recorded by- Virome capture sequencing for comprehensive HPV genotyping in cervical samples
Thanayod Sasivimolrattana, Sasiprapa Liewchalermwong, Wasun Chantratita, Insee Sensorn, Arkom Chaiwongkot, Parvapan Bhattarakosol
Science Progress.2025;[Epub] CrossRef - High-Risk Human Papillomavirus Detection via Cobas® 4800 and REBA HPV-ID® Assays
Sasiprapa Liewchalermwong, Shina Oranratanaphan, Wichai Termrungruanglert, Surang Triratanachat, Patou Tantbirojn, Nakarin Kitkumthorn, Parvapan Bhattarakosol, Arkom Chaiwongkot
Viruses.2022; 14(12): 2713. CrossRef - Evaluation of nuclear chromatin using grayscale intensity and thresholded percentage area in liquid‐based cervical cytology
Hyekyung Lee, Myungein Han, Taejo Yoo, Chanho Jung, Hyun‐Jin Son, Migyung Cho
Diagnostic Cytopathology.2018; 46(5): 384. CrossRef - Comparison of EASYPREP® and SurePath® in thyroid fine‐needle aspiration
Yosep Chong, Ki Hyun Baek, Jee Young Kim, Tae‐Jung Kim, Eun Jung Lee, Chang Suk Kang
Diagnostic Cytopathology.2016; 44(4): 283. CrossRef
- Virome capture sequencing for comprehensive HPV genotyping in cervical samples
- Human Papillomavirus Prevalence and Cell Cycle Related Protein Expression in Tonsillar Squamous Cell Carcinomas of Korean Patients with Clinicopathologic Analysis
- Miji Lee, Sung Bae Kim, Sang-wook Lee, Jong-Lyel Roh, Seung-Ho Choi, Soon Yuhl Nam, Sang Yoon Kim, Kyung-Ja Cho
- Korean J Pathol. 2013;47(2):148-157. Published online April 24, 2013
- DOI: https://doi.org/10.4132/KoreanJPathol.2013.47.2.148
- 8,080 View
- 52 Download
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Human papillomavirus (HPV)-related tonsillar squamous cell carcinoma (TSCC) has recently been characterized as a distinct subset with a favorable prognosis. The prevalence and clinicopathologic significance of HPV-related TSCC in Koreans are not well known.
Methods HPV
in situ hybridization (ISH) accompanied by p53, p16, pRb, and cyclin D1 immunohistochemical staining were performed on 89 resection cases of TSCC from 2000 through 2010.Results HPV was detected by ISH in 59 of 89 cases (66.3%). HPV-positive TSCCs were more common in younger ages (p=0.005), and tumor sizes were smaller in the HPV-positive compared to the HPV-negative group (p=0.040). Positive HPV staining was significantly correlated with p16 expression (p<0.001), pRb inactivation (p=0.003), and cyclin D1 down-regulation (p<0.001) but not with p53 expression (p=0.334). Seventeen cases that showed p16-immunopositivity with HPV-negativity by ISH were retested by HPV typing; HPV DNA was not detected in all cases. There was no significant difference between HPV-positive and HPV-negative patients either in the disease-specific survival (DSS, p=0.857) or overall survival (p=0.910). Furthermore, pRb-inactivated cases showed better DSS (p=0.023), and p53-positive cases showed worse DSS (p=0.001).
Conclusions Although high HPV prevalence was noted, it was not correlated with histopathologic findings or survival benefit. In addition to p53 expression, pRb inactivation along with p16 overexpression and down-regulation of cyclin D1 are thought to be important pathogenetic steps for developing TSCCs.
-
Citations
Citations to this article as recorded by- Assessment of the Mutation Profile of Tonsillar Squamous Cell Carcinomas Using Targeted Next-Generation Sequencing
Ha Young Park, Joong Seob Lee, Jee Hye Wee, Jeong Wook Kang, Eun Soo Kim, Taeryool Koo, Hee Sung Hwang, Hyo Jung Kim, Ho Suk Kang, Hyun Lim, Nan Young Kim, Eun Sook Nam, Seong Jin Cho, Mi Jung Kwon
Biomedicines.2023; 11(3): 851. CrossRef - Clinicopathologic characterization of cervical metastasis from an unknown primary tumor: a multicenter study in Korea
Miseon Lee, Uiree Jo, Joon Seon Song, Youn Soo Lee, Chang Gok Woo, Dong-Hoon Kim, Jung Yeon Kim, Sun Och Yoon, Kyung-Ja Cho
Journal of Pathology and Translational Medicine.2023; 57(3): 166. CrossRef - Negative Prognostic Implication of TERT Promoter Mutations in Human Papillomavirus–Negative Tonsillar Squamous Cell Carcinoma Under the New 8th AJCC Staging System
Hyunchul Kim, Mi Jung Kwon, Bumjung Park, Hyo Geun Choi, Eun Sook Nam, Seong Jin Cho, Kyueng-Whan Min, Eun Soo Kim, Hee Sung Hwang, Mineui Hong, Taeryool Koo, Hyo Jung Kim
Indian Journal of Surgical Oncology.2021; 12(S1): 134. CrossRef - Prevalence of high-risk human papillomavirus and its genotype distribution in head and neck squamous cell carcinomas
Yuil Kim, Young-Hoon Joo, Min-Sik Kim, Youn Soo Lee
Journal of Pathology and Translational Medicine.2020; 54(5): 411. CrossRef - Frequent hepatocyte growth factor overexpression and low frequency of c-Met gene amplification in human papillomavirus–negative tonsillar squamous cell carcinoma and their prognostic significances
Mi Jung Kwon, Dong Hoon Kim, Hye-Rim Park, Hyung Sik Shin, Ji Hyun Kwon, Dong Jin Lee, Jin Hwan Kim, Seong Jin Cho, Eun Sook Nam
Human Pathology.2014; 45(7): 1327. CrossRef
- Assessment of the Mutation Profile of Tonsillar Squamous Cell Carcinomas Using Targeted Next-Generation Sequencing
- Expression of c-Met Is Different along the Location and Associated with Lymph Node Metastasis of Head and Neck Carcinoma
- Ji-Young Choe, Ji Yun Yun, Soo-Jeong Nam, Ji Eun Kim
- Korean J Pathol. 2012;46(6):515-522. Published online December 26, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.6.515
- 7,670 View
- 51 Download
- 18 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Activation of the c-Met pathway is involved in cancer progression and the prognosis. We aimed to identify any association of c-Met protein expression with a number of clinicopathologic variables including infection of human papillomavirus and Epstein-Barr virus (EBV) in head and neck carcinomas (HNCa).
Methods Eighty-two cases were enrolled in this study. Expression of c-Met and p16 was investigated immunohistochemically. EBV was detected by
in situ hybridization and amplification of thec-Met gene by fluorescencein situ hybridization.Results The c-Met protein was expressed in 41.5% (34/82), and gene amplification was found in 1.4% (1/71). High expression of c-Met was associated with the primary location of the tumor; the hypopharynx showed the highest expression, followed by the oral cavity, larynx, and nasal cavity. Squamous cell carcinoma expressed c-Met more frequently than undifferentiated carcinoma. Also, p16 immunoreactivity or EBV infection was associated with the tumor location and well-differentiated histologic type, but were not linked to c-Met expression. The patients with positive c-Met expression showed frequent lymph node metastasis.
Conclusions Activation of the c-Met pathway might be involved in a subset of HNCa. Cases showing positive c-Met expression should be carefully monitored because of the high probability of lymph node metastasis.
-
Citations
Citations to this article as recorded by- c-MET pathway in human malignancies and its targeting by natural compounds for cancer therapy
Chakrabhavi Dhananjaya Mohan, Muthu K Shanmugam, Siddegowda Gopalapura Shivanne Gowda, Arunachalam Chinnathambi, Kanchugarakoppal S. Rangappa, Gautam Sethi
Phytomedicine.2024; 128: 155379. CrossRef - Nadir paranazal sinüs kanserlerinde yeni tanımlanan reseptör tirozin kinaz mutasyonları ve potansiyel fonksiyonel etkileri
Bakiye GÖKER BAGCA, Sercan GÖDE, Göksel TURHAL, Neslihan Pınar ÖZATEŞ, Ali VERAL, Cumhur GÜNDÜZ, Çığır Biray AVCI
Ege Tıp Dergisi.2023; 62(1): 139. CrossRef - The Emerging Role of c-Met in Carcinogenesis and Clinical Implications as a Possible Therapeutic Target
Antonio Faiella, Ferdinando Riccardi, Giacomo Cartenì, Martina Chiurazzi, Livia Onofrio, Rengyun Liu
Journal of Oncology.2022; 2022: 1. CrossRef - NK4 Regulates Laryngeal Squamous Cell Carcinoma Cell Properties and Inhibits Tumorigenicity by Modulating the DKK1/Wnt/β-Catenin Axis
Shoukai Zhang, Hulai Wei, Xiaoqin Ha, Yueyu Zhang, Yufen Guo
Frontiers in Oncology.2021;[Epub] CrossRef - Epstein-Barr Virus-Associated Carcinoma of the Larynx: A Systematic Review with Meta-Analysis
Marcos Antonio Pereira de Lima, Álife Diêgo Lima Silva, Antônio Carlos Silva do Nascimento Filho, Thiago Lima Cordeiro, João Pedro de Souza Bezerra, Maria Aline Barroso Rocha, Sally de França Lacerda Pinheiro, Roberto Flávio Fontenelle Pinheiro Junior, Ma
Pathogens.2021; 10(11): 1429. CrossRef - The roles of PTEN, cMET, and p16 in resistance to cetuximab in head and neck squamous cell carcinoma
Alexandre A. B. A. da Costa, Felipe D’Almeida Costa, Daniel Vilarim Araújo, Marcos Pedro Guedes Camandaroba, Victor Hugo Fonseca de Jesus, Audrey Oliveira, Ana Caroline Fonseca Alves, Carlos Stecca, Larissa Machado, Andrea Cruz Feraz de Oliveira, Thiago B
Medical Oncology.2019;[Epub] CrossRef - Role of c‐Met expression on prognosis of head and neck cancer: A literature review and meta‐analysis
Lei Li, Zhijun Sun, Xin Huang, Xiao Li, Lihua Sun, Lei Zhang, Xiaodan Zhang, Longwei Ye, Jie Yuan, Limin Mao, Guolin Li
Head & Neck.2019; 41(6): 1999. CrossRef - MET Genomic Alterations in Head and Neck Squamous Cell Carcinoma (HNSCC): Rapid Response to Crizotinib in a Patient with HNSCC with a Novel MET R1004G Mutation
Lisa Pei Chu, Debra Franck, Christine A. Parachoniak, Jeffrey P. Gregg, Michael G. Moore, D. Gregory Farwell, Shyam Rao, Andreas M. Heilmann, Rachel L. Erlich, Jeffrey S. Ross, Vincent A. Miller, Siraj Ali, Jonathan W. Riess
The Oncologist.2019; 24(10): 1305. CrossRef - Understanding c-MET signalling in squamous cell carcinoma of the head & neck
P. Szturz, E. Raymond, C. Abitbol, S. Albert, A. de Gramont, S. Faivre
Critical Reviews in Oncology/Hematology.2017; 111: 39. CrossRef - Prognostic value of c-MET in head and neck cancer: A systematic review and meta-analysis of aggregate data
Petr Szturz, Marie Budíková, Jan B. Vermorken, Ivana Horová, Břetislav Gál, Eric Raymond, Armand de Gramont, Sandrine Faivre
Oral Oncology.2017; 74: 68. CrossRef - Activated HGF-c-Met Axis in Head and Neck Cancer
Levi Arnold, Jonathan Enders, Sufi Thomas
Cancers.2017; 9(12): 169. CrossRef - Clinicopathological impacts of high c-Met expression in head and neck squamous cell carcinoma: a meta-analysis and review
Jung Han Kim, Bum Jun Kim, Hyeong Su Kim
Oncotarget.2017; 8(68): 113120. CrossRef - High expression of c‑Met and EGFR is associated with poor survival of patients with glottic laryngeal squamous cell carcinoma
Mei Jiang, Hui Zhang, He Xiao, Zhimin Zhang, Dan Que, Jia Luo, Jian Li, Bijing Mao, Yuanyuan Chen, Meilin Lan, Ge Wang, Hualiang Xiao
Oncology Letters.2017;[Epub] CrossRef - Profiling of cMET and HER Family Receptor Expression in Pancreatic Ductal Adenocarcinomas and Corresponding Lymph Node Metastasis to Assess Relevant Pathways for Targeted Therapies
Alexander Muckenhuber, Galina Babitzki, Marlene Thomas, Gabriele Hölzlwimmer, Magdalena Zajac, Moritz Jesinghaus, Frank Bergmann, Jens Werner, Albrecht Stenzinger, Wilko Weichert
Pancreas.2016; 45(8): 1167. CrossRef - Absent and abundant MET immunoreactivity is associated with poor prognosis of patients with oral and oropharyngeal squamous cell carcinoma
Maria J. De Herdt, Stefan M. Willems, Berdine van der Steen, Rob Noorlag, Esther I. Verhoef, Geert J.L.H. van Leenders, Robert J.J. van Es, Senada Koljenović, Robert J. Baatenburg de Jong, Leendert H.J. Looijenga
Oncotarget.2016; 7(11): 13167. CrossRef - Biological, diagnostic and therapeutic relevance of the MET receptor signaling in head and neck cancer
Lluís Nisa, Daniel Matthias Aebersold, Roland Giger, Yitzhak Zimmer, Michaela Medová
Pharmacology & Therapeutics.2014; 143(3): 337. CrossRef - Frequent hepatocyte growth factor overexpression and low frequency of c-Met gene amplification in human papillomavirus–negative tonsillar squamous cell carcinoma and their prognostic significances
Mi Jung Kwon, Dong Hoon Kim, Hye-Rim Park, Hyung Sik Shin, Ji Hyun Kwon, Dong Jin Lee, Jin Hwan Kim, Seong Jin Cho, Eun Sook Nam
Human Pathology.2014; 45(7): 1327. CrossRef - Distinct c-Met activation mechanisms induce cell rounding or invasion through pathways involving integrins, RhoA and HIP1
Anja Mai, Ghaffar Muharram, Rachel Barrow-McGee, Habib Baghirov, Juha Rantala, Stéphanie Kermorgant, Johanna Ivaska
Journal of Cell Science.2014; 127(9): 1938. CrossRef
- c-MET pathway in human malignancies and its targeting by natural compounds for cancer therapy
- Primary Endometrial Squamous Cell Carcinoma: A Case Report and Review of Relevant Literature on Korean Women
- Sung Jong Lee, Hyun Joo Choi
- Korean J Pathol. 2012;46(4):395-398. Published online August 23, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.4.395
- 8,037 View
- 76 Download
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF Primary endometrial squamous cell carcinoma (PESCC) is an extremely rare tumor with unclear pathogenesis. A 54-year-old postmenopausal woman presented with a 6-month history of vaginal bleeding. The patient was provisionally diagnosed with uterine submucosal leiomyoma. This was followed by total hysterectomy with a bilateral salpingo-oophorectomy under the laparoscopic guidance. Histopathologically, the tumor was PESCC which was accompanied by a lack of the tumor in the uterine cervix. The tumor showed positive immunoreactivity for p16INK4a. But there was no evidence of human papillomavirus (HPV) on
in situ hybridization and HPV DNA chip analysis. We also present a review of the relevant literature on Korean women.-
Citations
Citations to this article as recorded by- Primary endometrial squamous cell carcinoma (PESCC): Review of the literature and case report
Kuang-Han Liu, Chia-Chin Tsai, Krystal Baysan Lin, Pei-Shen Huang
Taiwanese Journal of Obstetrics and Gynecology.2025; 64(1): 159. CrossRef - p16 Block Type Overexpression, p53 Wild Type Reactivity, and Cervical Involvement do not Always Exclude the Diagnosis of Primary Endometrial Squamous Cell Carcinoma (PESCC)
Daniela Fanni, Clara Gerosa, Michele Peiretti, Valerio Mais, Elena Massa, Stefano Angioni, Gavino Faa
International Journal of Gynecological Pathology.2024; 43(2): 200. CrossRef - Pathogenetic characteristics of endometrioid adenocarcinoma of uterus at present stage
T. I. Moiseenko, S. V. Shatalova, E. M. Nepomnyashchaya, V. A. Bandovkina, M. L. Adamyan
Medical alphabet.2024; (36): 35. CrossRef - Case report: Clinicopathological characteristic of two cases of primary endometrial squamous cell carcinoma and review of the literature
Hui-Bin Zhang, Li-Hua Lin, Qiu-Ping Lin, Yuan-Qing Lin, Dan Luo, Shu-Xia Xu
Frontiers in Oncology.2024;[Epub] CrossRef - Treatment of primary squamous cell carcinoma of the endometrium and review of previous literature: A case report
Liyun Song, Qi Wu, Suning Bai, Ren Xu, Xiaona Wang, Yanyan Yang
Medicine.2023; 102(17): e33667. CrossRef -
Prevalence of
human papilloma virus
and
Chlamydia trachomatis
in endometrial and cervical carcinoma: a comparative study in North Indian women
Heena Gautam, Sumita Mehta, Nidhi Nayar, Neha Kumar, Syed Akhtar Husain, Mausumi Bharadwaj
Systems Biology in Reproductive Medicine.2023; 69(6): 399. CrossRef - PAX8 Positivity, Abnormal p53 Expression, and p16 Negativity in a Primary Endometrial Squamous Cell Carcinoma: A Case Report and Review of the Literature
Daniela Fanni, Michele Peiretti, Valerio Mais, Elena Massa, Clara Gerosa, Francesca Ledda, Maria Luisa Fais, Gavino Faa, Stefano Angioni
International Journal of Gynecological Pathology.2022; 41(4): 431. CrossRef - Molecular Analysis of HPV-independent Primary Endometrial Squamous Cell Carcinoma Reveals TP53 and CDKN2A Comutations
Mark R. Hopkins, Doreen N. Palsgrove, Brigitte M. Ronnett, Russell Vang, Jeffrey Lin, Tricia A. Murdock
American Journal of Surgical Pathology.2022; 46(12): 1611. CrossRef - Primary squamous cell carcinoma of the endometrium—Case report with cytological characteristics in direct and indirect endometrial samples
Sanda Rajhvajn, Ana Barišić, Lada Škopljanac‐Mačina, Danijela Jurič, Vesna Mahovlić
Cytopathology.2021; 32(6): 823. CrossRef - Primary squamous cell carcinoma of the endometrium associated with human papilloma virus in a young woman: a case report
Tchin Darré, Abdoul-Samadou Aboubakari, Lantam Sonhaye, Baguilane Douaguibe, Akila Bassowa, Gado Napo-Koura
Journal of Medical Case Reports.2019;[Epub] CrossRef - Primary squamous cell carcinoma of the endometrium in a woman of perimenopausal age
Chao Zhang, Hongyan Zhang, Linqing Yang, Yunfei Wang, Xiaoyu Li, Jinfeng Guo, Jing Xu
Medicine.2018; 97(48): e13418. CrossRef - S100P is Overexpressed in Squamous Cell and Adenosquamous Carcinoma Subtypes of Endometrial Cancer and Promotes Cancer Cell Proliferation and Invasion
Hongfei Jiang, Hang Hu, Fan Lin, Yoon Pin Lim, Yunfen Hua, Xiaomei Tong, Songying Zhang
Cancer Investigation.2016; 34(10): 477. CrossRef - Überraschung in der Abradatdiagnostik
U. Kellner, A. Kellner, U. Cirkel
Der Pathologe.2015; 36(3): 317. CrossRef
- Primary endometrial squamous cell carcinoma (PESCC): Review of the literature and case report
- Expression of Human Papillomavirus-Related Proteins and Its Clinical Implication in Tonsillar Squamous Cell Carcinoma
- Joon Seon Song, Min-Sik Kim, Joon Wook Park, Youn Soo Lee, Chang Suk Kang
- Korean J Pathol. 2012;46(2):177-186. Published online April 25, 2012
- DOI: https://doi.org/10.4132/KoreanJPathol.2012.46.2.177
- 9,711 View
- 41 Download
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Background Human papillomavirus (HPV) is known to cause of oropharyngeal squamous cell carcinoma (SqCC). HPV positive SqCCs overexpress p16 and are associated with better survival. Several markers of cell cycles and apoptosis have been reported as a prognostic value. We examined the prognostic value of HPV status, p16, cyclin D1, and Bcl-2 in patients with tonsillar SqCC.
Methods Tissue microarrays were constructed in 56 cases of tonsillar SqCC for which we performed an immunohistochemistry and an
in situ hybridization (ISH) of the HPV.Results Of the 56 cases, 31 (55.3%) were positive for p16 and 20 (35.7%) were positive for HPV ISH. The expressions of p16, cyclin D1, and Bcl-2 were not correlated with the clinicopathologic variables including smoking status, differentiation and pT- and pN-stages. The HPV ISH positive group showed a better overall survival than the HPV negative group (p=0.04), and the p16 positive group showed a better disease free survival (DFS) than the negative group (p=0.016). Cox regression analysis showed that only p16 positivity was an independent prognostic factor for DFS (p=0.03; hazard ratio, 10.1).
Conclusions Our results indicate that both p16 expression and HPV status are useful indicators for risk stratification in patients with tonsillar SqCC.
-
Citations
Citations to this article as recorded by- Positive Rate of Human Papillomavirus and Its Trend in Head and Neck Cancer in South Korea
Hyun Woong Jun, Yong Bae Ji, Chang Myeon Song, Jae Kyung Myung, Hae Jin Park, Kyung Tae
Frontiers in Surgery.2022;[Epub] CrossRef - Negative Prognostic Implication of TERT Promoter Mutations in Human Papillomavirus–Negative Tonsillar Squamous Cell Carcinoma Under the New 8th AJCC Staging System
Hyunchul Kim, Mi Jung Kwon, Bumjung Park, Hyo Geun Choi, Eun Sook Nam, Seong Jin Cho, Kyueng-Whan Min, Eun Soo Kim, Hee Sung Hwang, Mineui Hong, Taeryool Koo, Hyo Jung Kim
Indian Journal of Surgical Oncology.2021; 12(S1): 134. CrossRef - In situ hybridization for high risk HPV E6/E7 mRNA in oropharyngeal squamous cell carcinoma
Krish Suresh, Parth V. Shah, Sydney Coates, Borislav A. Alexiev, Sandeep Samant
American Journal of Otolaryngology.2021; 42(1): 102782. CrossRef - Prevalence of high-risk human papillomavirus and its genotype distribution in head and neck squamous cell carcinomas
Yuil Kim, Young-Hoon Joo, Min-Sik Kim, Youn Soo Lee
Journal of Pathology and Translational Medicine.2020; 54(5): 411. CrossRef - Human Papillomavirus Testing in Head and Neck Carcinomas: Guideline From the College of American Pathologists
James S. Lewis, Beth Beadle, Justin A. Bishop, Rebecca D. Chernock, Carol Colasacco, Christina Lacchetti, Joel Todd Moncur, James W. Rocco, Mary R. Schwartz, Raja R. Seethala, Nicole E. Thomas, William H. Westra, William C. Faquin
Archives of Pathology & Laboratory Medicine.2018; 142(5): 559. CrossRef - Detection of HPV infection in head and neck cancers: Promise and pitfalls in the last ten years: A meta-analysis
Carolin G�tz, Clara Bischof, Klaus-Dietrich Wolff, Andreas Kolk
Molecular and Clinical Oncology.2018;[Epub] CrossRef - Frequent hepatocyte growth factor overexpression and low frequency of c-Met gene amplification in human papillomavirus–negative tonsillar squamous cell carcinoma and their prognostic significances
Mi Jung Kwon, Dong Hoon Kim, Hye-Rim Park, Hyung Sik Shin, Ji Hyun Kwon, Dong Jin Lee, Jin Hwan Kim, Seong Jin Cho, Eun Sook Nam
Human Pathology.2014; 45(7): 1327. CrossRef - Human papillomavirus‐stratified analysis of the prognostic role of miR‐21 in oral cavity and oropharyngeal squamous cell carcinoma
Yoon Ho Ko, Hye Sung Won, Der Sheng Sun, Ho Jung An, Eun Kyoung Jeon, Min Sik Kim, Han Hong Lee, Jin Hyoung Kang, Chan Kwon Jung
Pathology International.2014; 64(10): 499. CrossRef - Human Papillomavirus Prevalence and Cell Cycle Related Protein Expression in Tonsillar Squamous Cell Carcinomas of Korean Patients with Clinicopathologic Analysis
Miji Lee, Sung Bae Kim, Sang-wook Lee, Jong-Lyel Roh, Seung-Ho Choi, Soon Yuhl Nam, Sang Yoon Kim, Kyung-Ja Cho
Korean Journal of Pathology.2013; 47(2): 148. CrossRef
- Positive Rate of Human Papillomavirus and Its Trend in Head and Neck Cancer in South Korea

 E-submission
E-submission





 First
First Prev
Prev



